US Health Secretary Robert F. Kennedy Jr.’s “Make America Healthy Again” guidelines highlight the tension between populist health claims and rigorous statistical evidence. This conflict underscores the difficulty patients face in distinguishing clinical causation from correlation, necessitating a return to evidence-based, peer-reviewed nutritional science to protect public health.
The current friction surrounding national dietary guidelines is not merely a political debate; This proves a crisis of scientific literacy. When public health directives shift rapidly, the “information gap” often leaves patients caught between legacy medical advice and new, sometimes unverified, nutritional trends. For the global patient, the danger lies in the misinterpretation of epidemiological data—the study of how often diseases occur in different groups of people—which can lead to the adoption of restrictive diets that may be contraindicated for specific medical conditions.
In Plain English: The Clinical Takeaway
- Correlation is not Causation: Just because two things happen together (e.g., eating a certain food and feeling better) does not mean one caused the other.
- Evidence Hierarchy: A large-scale, peer-reviewed clinical trial carries significantly more weight than a personal anecdote or a single observational study.
- Personalized Medicine: No single dietary guideline fits every biology; metabolic needs vary based on genetics, current medications, and pre-existing organ function.
The Statistical Mirage: Distinguishing Signal from Noise in Nutrition
At the heart of the debate over the new dietary guidelines is the challenge of “p-hacking”—the practice of manipulating data until a statistically significant result is found. In nutritional science, Here’s a pervasive issue because it is nearly impossible to conduct a lifelong, double-blind placebo-controlled trial (a study where neither the participant nor the researcher knows who is receiving the treatment) on a specific diet.
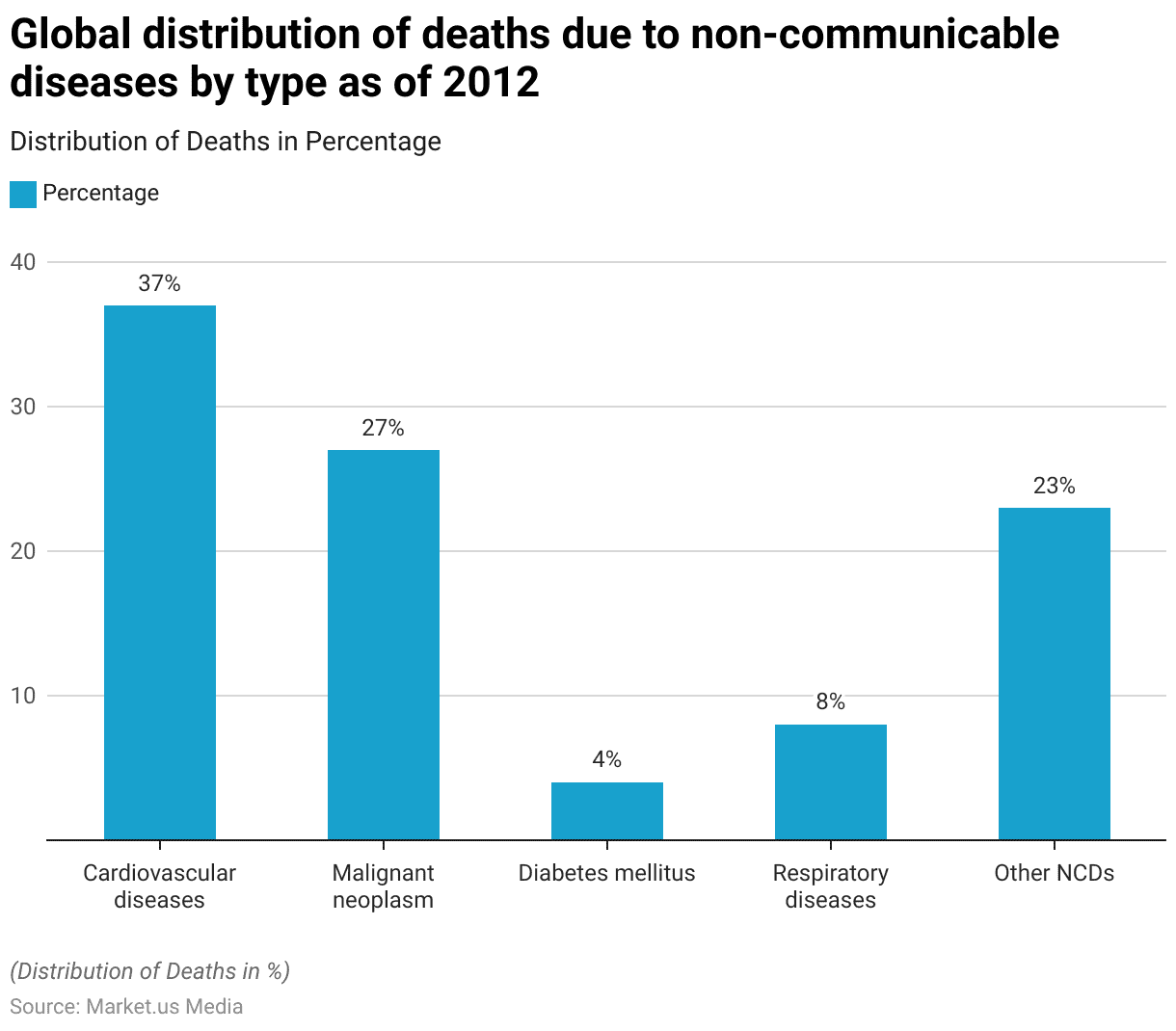
Instead, researchers rely on observational cohorts. While these provide valuable signals, they are prone to confounding variables. For example, people who eat more organic produce may likewise exercise more and smoke less. If a study finds they have lower rates of cardiovascular disease, it is a mistake to attribute the result solely to the organic produce without adjusting for those other lifestyle factors.
The mechanism of action—the specific biochemical process through which a substance produces its effect—for many of the “MAHA” suggestions involves the reduction of ultra-processed foods (UPFs). From a clinical perspective, UPFs often trigger hyperinsulinemia, a condition where the body produces excess insulin to manage rapid glucose spikes. Over time, this leads to insulin resistance, the primary driver of Type 2 Diabetes and metabolic syndrome.
“The challenge we face is not a lack of data, but an abundance of low-quality data. When we translate nutritional epidemiology into public policy, we must demand a higher threshold of evidence to avoid the ‘pendulum swing’ of dietary advice that confuses the public.” — Dr. Vikram Patel, Epidemiologist and Global Health Researcher.
Global Regulatory Divergence: FDA, EMA, and the WHO
The shift in US guidelines creates a geopolitical ripple effect. While the US FDA (Food and Drug Administration) focuses heavily on additive safety and labeling, the European Medicines Agency (EMA) and the European Food Safety Authority (EFSA) often apply the “precautionary principle,” banning substances more proactively if there is a plausible risk, even if definitive proof is lacking.
In the United Kingdom, the NHS (National Health Service) integrates dietary guidance into a centralized care model, which allows for more controlled implementation of nutritional interventions. The discrepancy between these systems creates “health tourism,” where patients seek specific dietary protocols based on the regulatory environment of another country, often ignoring the local clinical contraindications—conditions or factors that serve as a reason to withhold a certain treatment.
Transparency regarding funding is critical here. A significant portion of early nutritional research was funded by industry giants (sugar, seed oils, and grains), creating a systemic bias. Modern, gold-standard research is increasingly funded by independent bodies like the National Institutes of Health (NIH) or the World Health Organization (WHO), though funding gaps still exist for long-term longitudinal studies—research that follows the same individuals over decades.
| Evidence Type | Reliability Level | Primary Limitation | Clinical Application |
|---|---|---|---|
| Meta-Analysis of RCTs | Highest | Publication bias (negative results often ignored) | Establishing gold-standard treatment protocols |
| Cohort Studies | Moderate | Confounding variables; correlation vs. Causation | Identifying risk factors and population trends |
| Case-Control Studies | Low to Moderate | Recall bias (patients forgetting past habits) | Investigating rare diseases or outbreaks |
| Expert Opinion/Anecdote | Lowest | Subjective bias; lack of control groups | Hypothesis generation only |
The Metabolic Pathway: Why ‘One Size Fits All’ Fails
The push for a “healthier America” often overlooks the complexity of the glycemic index—a system that ranks carbohydrates by how quickly they raise blood glucose levels. For a healthy athlete, a high-glycemic load may be acceptable. However, for a patient with chronic kidney disease (CKD), certain “healthy” high-protein or high-potassium diets can lead to hyperkalemia, a dangerous buildup of potassium in the blood that can cause cardiac arrest.
the interaction between diet and pharmacokinetics—how the body processes medication—is often ignored in broad public health slogans. For instance, sudden increases in leafy green vegetable intake (high in Vitamin K) can interfere with the mechanism of action of warfarin, a common blood thinner, potentially leading to life-threatening clots.
Contraindications & When to Consult a Doctor
While improving diet is generally beneficial, drastic changes can be dangerous for specific populations. You must consult a licensed physician before implementing the new guidelines if you fall into these categories:
- Type 1 or Type 2 Diabetics: Rapidly reducing carbohydrate intake while on insulin or sulfonylureas can trigger severe hypoglycemia (dangerously low blood sugar).
- Chronic Kidney Disease (CKD) Patients: High-protein diets or specific mineral-rich “superfoods” can overwhelm impaired renal filtration.
- Pregnant or Lactating Women: Restrictive diets can lead to critical micronutrient deficiencies (e.g., folate, B12) essential for fetal neurological development.
- Individuals on Anticoagulants: Significant changes in the intake of Vitamin K-rich foods can destabilize blood clotting times.
If you experience sudden fatigue, unexplained weight loss, or cardiac palpitations after starting a new dietary regimen, seek immediate medical evaluation to rule out electrolyte imbalances or metabolic distress.
The Path Forward: Evidence-Based Wellness
The goal of “Making America Healthy Again” is a noble one, but the execution must be tethered to the rigors of clinical science. Public health intelligence should not be a matter of opinion or political willpower, but a reflection of the most robust data available. As we move further into 2026, the focus must shift from broad mandates to precision nutrition—using biomarkers and genetic profiling to determine what is “healthy” for the individual, rather than the average.
True health literacy involves questioning the source, understanding the sample size (N-value), and recognizing the difference between a “breakthrough” and a statistically insignificant trend. By demanding transparency in funding and adherence to the hierarchy of evidence, People can move past the noise of misinformation and toward a sustainable, scientifically sound future for public health.
References
- PubMed Central (National Library of Medicine) – Analysis of Ultra-Processed Foods and Metabolic Syndrome.
- The Lancet – Global Burden of Disease Study: Nutritional Risk Factors.
- World Health Organization (WHO) – Guidelines on Sugars and Non-Sugar Sweeteners.
- JAMA (Journal of the American Medical Association) – Randomized Controlled Trials in Nutritional Epidemiology.
- Centers for Disease Control and Prevention (CDC) – National Health and Nutrition Examination Survey (NHANES) Data.

