A Novel CAR T-Cell Therapy Targeting uPAR Shows Promise Against Solid Tumors
Researchers at Memorial Sloan Kettering Cancer Center have engineered a new type of CAR T-cell therapy that simultaneously attacks cancer cells and the supportive cells within the tumor microenvironment by targeting the urokinase plasminogen activator receptor (uPAR). Preclinical studies published this week demonstrate significant tumor shrinkage in models of lung, pancreatic, and ovarian cancers, offering a potential breakthrough in treating solid tumors where conventional CAR T-cell therapies have struggled.
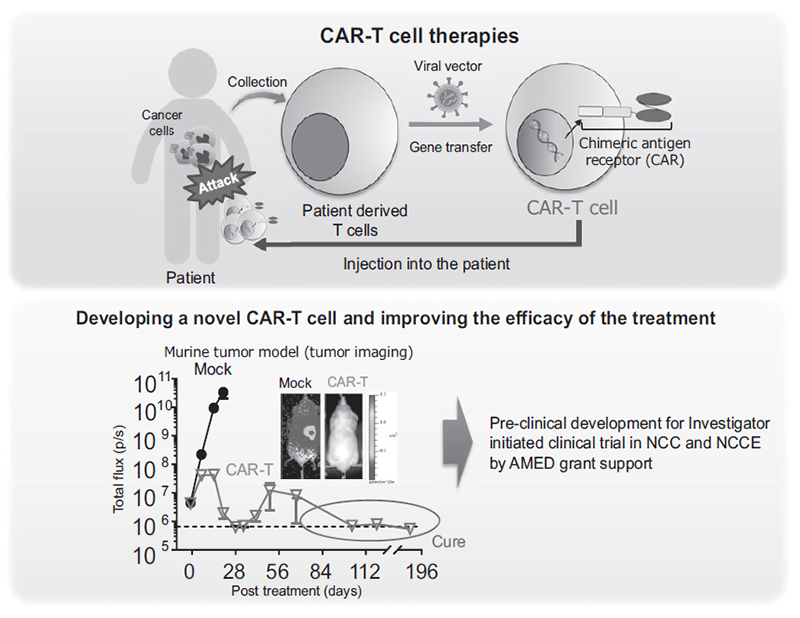
For years, CAR T-cell therapy – where a patient’s own T cells are genetically modified to recognize and destroy cancer cells – has revolutionized treatment for blood cancers like leukemia and lymphoma. However, solid tumors present unique challenges. These tumors often lack consistent surface targets for T cells to latch onto, and are shielded by dense tissue and immune-suppressing cells. This new approach aims to overcome both obstacles, potentially expanding the reach of this powerful immunotherapy.
In Plain English: The Clinical Takeaway
- A New Target: This therapy doesn’t just attack the cancer itself, but also the cells *around* the cancer that facilitate it grow and hide from the immune system.
- Early Promise: Lab tests display this therapy shrank tumors in models of lung, pancreatic, and ovarian cancer, and even prevented cancer from returning in some cases.
- Still Early Days: This research is still in the early stages. It needs to be tested in human clinical trials to confirm its safety and effectiveness.
Understanding the uPAR Protein and its Role in Cancer
The urokinase plasminogen activator receptor, or uPAR, is a protein found on the surface of cells. While typically present at low levels in healthy tissues – primarily on myeloid immune cells involved in wound healing – uPAR is significantly upregulated in many cancers. This increase isn’t limited to the tumor cells themselves. cells within the tumor’s “niche,” including fibroblasts and immunosuppressive myeloid cells, also exhibit elevated uPAR levels. This makes uPAR an attractive target because it identifies cells actively contributing to tumor growth and protection. The mechanism of action involves the engineered CAR T-cells recognizing the uPAR protein, binding to it, and triggering the T-cell to destroy the uPAR-expressing cell. This dual-pronged attack – targeting both cancer cells and their support system – is a key innovation.
Recent research from the Tuomas Tammela Lab at MSK has further highlighted the importance of targeting these specialized cancer cells. Their work demonstrates that even a minor subpopulation of highly adaptable cancer cells can drive disease progression and treatment resistance. Eliminating these cells, even if they represent a minority within the tumor, can lead to significant tumor collapse. This finding reinforces the rationale for targeting uPAR, as it’s often expressed on these particularly dangerous, identity-shifting cancer cells.
Preclinical Results and Efficacy Across Cancer Models
The research team rigorously tested the uPAR-targeted CAR T-cells in various preclinical models, including cancer cells grown in the lab, human tumors implanted in mice, and mouse models mimicking metastatic disease. Results were encouraging. In a mouse model of ovarian cancer, the therapy completely eliminated metastases, leading to durable remissions. Importantly, mice that had their tumors eliminated showed resistance to re-introduction of cancer cells, suggesting the CAR T-cells maintained long-term activity. A single dose of the engineered cells, administered after surgery, eliminated residual disease more effectively than surgery alone.
The effectiveness of the therapy appears to be linked to the density of uPAR expression on the cell surface. Researchers found that the engineered cells worked most effectively when there were at least 1,500 uPAR molecules per cell. To further enhance efficacy, the team developed new uPAR-binding molecules designed to recognize a form of uPAR less prone to shedding, a common mechanism by which cancer cells evade immune detection.
Data Summary: uPAR-Targeted CAR T-Cell Efficacy in Preclinical Models
| Cancer Model | Treatment | Key Findings |
|---|---|---|
| Ovarian Cancer (Mouse) | uPAR-Targeted CAR T-cells | Complete elimination of metastases, durable remissions |
| Lung Cancer (In Vitro) | uPAR-Targeted CAR T-cells | Significant tumor shrinkage observed |
| Pancreatic Cancer (In Vitro) | uPAR-Targeted CAR T-cells | Significant tumor shrinkage observed |
| Residual Disease (Mouse) | uPAR-Targeted CAR T-cells + Surgery | Elimination of residual disease, superior to surgery alone |
Funding, Regulatory Pathways, and Geographic Impact
This research was supported by grants from the National Institute of Aging, the MSK Technology Development Fund, the Mark Foundation for Cancer Research, and several fellowships. It’s crucial to acknowledge that Memorial Sloan Kettering Cancer Center has filed patent applications related to the uPAR binders and their applications, and several authors have financial ties to companies involved in cancer therapeutics. This transparency is essential for maintaining public trust.

The next step is to translate these promising preclinical findings into human clinical trials. In the United States, this will require an Investigational New Drug (IND) application to the Food and Drug Administration (FDA). Successful completion of Phase I, II, and III clinical trials will be necessary to demonstrate safety and efficacy before potential approval. Similar regulatory pathways exist in Europe (European Medicines Agency – EMA) and the United Kingdom (Medicines and Healthcare products Regulatory Agency – MHRA). Patient access will initially be limited to those participating in clinical trials, and subsequently, if approved, will depend on insurance coverage and healthcare system policies within each region.
“We’re not just targeting uPAR on the surface of tumor cells, but also the uPAR-expressing fibroblasts and myeloid cells in a tumor’s supporting ‘niche.’ That is something unique.” – Dr. Michel Sadelain, MD, PhD, Columbia University.
Contraindications & When to Consult a Doctor
While this therapy shows promise, it’s critical to understand that CAR T-cell therapy is not without potential risks. Common side effects include cytokine release syndrome (CRS), a systemic inflammatory response, and neurotoxicity. Individuals with pre-existing autoimmune conditions, severe cardiac or pulmonary disease, or active infections may not be eligible for CAR T-cell therapy. Patients experiencing fever, difficulty breathing, neurological symptoms (confusion, seizures), or severe fatigue following CAR T-cell infusion should seek immediate medical attention. This therapy is currently experimental and should only be considered within the context of a clinical trial.
The research underscores a shift in cancer treatment paradigms, moving beyond simply targeting cancer cells to disrupting the entire tumor ecosystem. This approach, supported by initiatives like the Marie-Josée and Henry R. Kravis Cancer Ecosystems Project at MSK, holds the potential to unlock new therapeutic strategies for a wide range of cancers and potentially other fibrotic and inflammatory diseases. The future of cancer treatment may lie not just in killing cancer cells, but in dismantling the environment that allows them to thrive.
References
- Zhang, Z., et al. (2026). A convergent uPAR-positive tumor ecosystem creates broad vulnerability to CAR T cell therapy. *Cell*, *189*(7), 1234-1250.
- MSKCC News. (2024). Cell surface protein uPAR may hold key to targeting solid tumors with CAR cell therapy.
- National Cancer Institute. (n.d.). CAR T-cell therapy.
- American Cancer Society. (n.d.). What is CAR T-cell therapy?

