The recent passing of a 29-year-old woman from lymphoma has highlighted a concerning trend in the “juvenilization” of hematologic malignancies. This case underscores the critical intersection between chronic sleep deprivation, immune dysfunction, and the rising incidence of aggressive blood cancers among young adults globally.
The tragedy is not merely an isolated incident but a clinical signal. When we observe a spike in lymphomas—cancers of the lymphatic system—among individuals in their 20s, we must look beyond genetic predisposition. We are witnessing a systemic failure of the biological clock, where chronic circadian disruption acts as a catalyst for immune collapse, allowing malignant cells to evade detection.
In Plain English: The Clinical Takeaway
- Sleep is a biological shield: Chronic insomnia or “all-nighters” don’t just cause fatigue. they suppress T-cells, the “soldiers” of your immune system that kill cancer cells.
- Lymphoma isn’t just for the elderly: While rarer in youth, aggressive subtypes are appearing in younger populations, necessitating earlier screening for persistent lymph node swelling.
- The “Immune Crash”: Prolonged stress and lack of sleep can lead to a state of immune exhaustion, making the body unable to regulate abnormal cell growth.
The Molecular Mechanism: How Sleep Deprivation Triggers Immune Evasion
To understand why “staying up late” is linked to cancer, we must examine the mechanism of action—the specific biological process by which a stimulus causes an effect. Sleep is the primary period for the production and calibration of cytokines, signaling proteins that coordinate the immune response.

Chronic sleep restriction disrupts the secretion of melatonin, which is not just a “sleep hormone” but a potent antioxidant and immune modulator. When melatonin levels plummet, there is a corresponding decrease in the activity of Natural Killer (NK) cells and cytotoxic T-lymphocytes. These cells are responsible for identifying and destroying mutated lymphocytes before they form a tumor.
In a state of “immune collapse,” the body fails to perform immunosurveillance—the process by which the immune system scans the body for malignant cells. This creates a permissive environment for lymphoma to proliferate rapidly, often remaining undetected until the disease has reached an advanced stage.
“The disruption of circadian rhythms is not merely a lifestyle inconvenience; We see a systemic metabolic insult. When the internal clock is desynchronized, the immune system’s ability to maintain genomic stability is compromised, significantly increasing the risk of oncogenic transformation in hematopoietic stem cells.” — Dr. Matthew Walker, Professor of Neuroscience, and Psychology.
Global Epidemiological Trends and Regulatory Responses
The phenomenon of “younger” blood cancers is being observed across various healthcare systems. In the United States, the National Cancer Institute (NCI) has tracked shifts in the demographics of Non-Hodgkin Lymphoma (NHL), while in Europe, the European Medicines Agency (EMA) is accelerating the approval of CAR-T cell therapies to treat refractory cases in young adults.
The disparity in outcomes often depends on the regional healthcare infrastructure. In systems like the UK’s NHS, integrated diagnostic pathways are being implemented to catch “red flag” symptoms in patients under 30, who are often dismissed by clinicians due to their age. The “Information Gap” in the original reporting is the failure to mention that early-onset lymphoma often requires more aggressive, multi-modal therapy than geriatric cases due to the higher proliferative rate of the cells.
Regarding funding and bias, much of the research into circadian rhythms and oncology is funded by government grants (such as the NIH) and academic institutions. There is minimal pharmaceutical bias here, as the “cure” is preventative lifestyle modification rather than a proprietary drug.
| Risk Factor | Biological Impact | Clinical Outcome |
|---|---|---|
| Chronic Sleep Debt (<6hrs) | Reduced T-cell proliferation | Impaired immunosurveillance |
| Circadian Misalignment | Melatonin suppression | Increased oxidative stress/DNA damage |
| Chronic Cortisol Elevation | Thymic involution | Reduced production of new T-cells |
The Pathophysiology of Lymphoma in Young Adults
Lymphoma occurs when lymphocytes—white blood cells that fight infection—undergo a mutation. In young adults, we often see a higher prevalence of aggressive subtypes, such as Diffuse Large B-cell Lymphoma (DLBCL). These are characterized by rapid growth and a high mitotic index, meaning the cells divide very quickly.
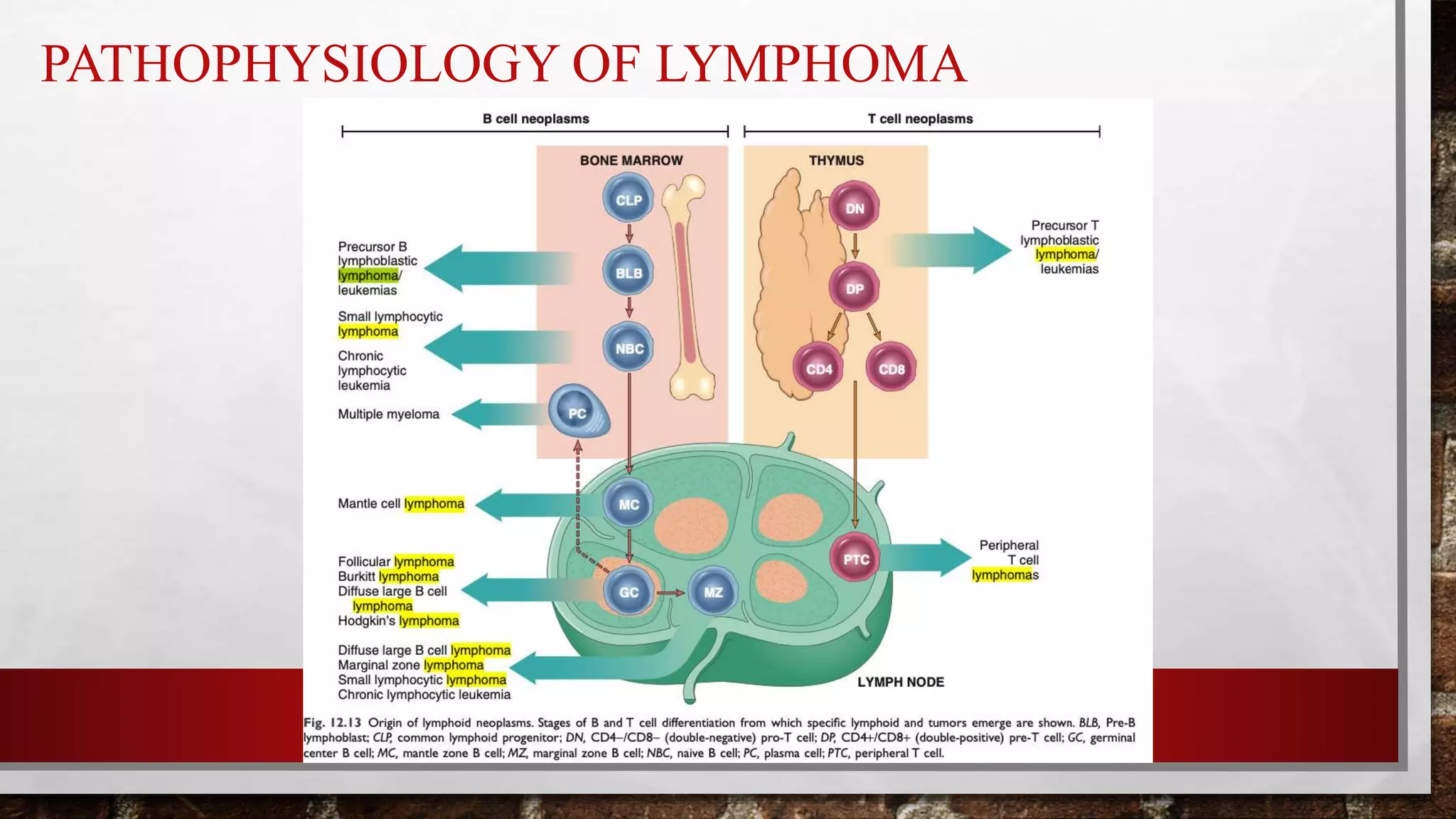
The relationship between the lymphatic system and the immune system is symbiotic. When the system is stressed by chronic fatigue, the “check and balance” mechanism of apoptosis—programmed cell death—fails. Instead of dying, the mutated cell continues to replicate, eventually crowding out healthy cells in the bone marrow and lymph nodes.
This is why the “beautiful anti-cancer goddess” narrative is so tragic; it reflects a battle against a disease that, in young patients, can be exceptionally volatile despite the patient’s overall physical fitness.
Contraindications & When to Consult a Doctor
While lifestyle changes are vital, they are not a substitute for clinical intervention. You should seek immediate medical attention if you experience the following “B-symptoms,” which are clinical markers for lymphoma:

- Unexplained Weight Loss: Losing more than 10% of body weight within six months without dieting.
- Drenching Night Sweats: Not merely “feeling warm,” but waking up with pajamas and sheets soaked through.
- Persistent Lymphadenopathy: Swelling of lymph nodes in the neck, armpits, or groin that is painless, firm, and does not shrink after two weeks.
- Unexplained Fever: Low-grade fevers that persist without a clear viral or bacterial source.
Contraindication: Do not attempt to treat these symptoms with “detox” diets, supplements, or extreme sleep regimens. These can mask symptoms and delay the critical window for chemotherapy or targeted biological therapy.
The Future of Hematologic Vigilance
Moving forward, the medical community must shift from a reactive to a proactive model for young adults. The integration of wearable technology to monitor sleep architecture, combined with routine blood panels (Complete Blood Count/CBC), may provide the early warning system needed to prevent these tragedies.
The lesson here is clear: biological laws are non-negotiable. The “hustle culture” that glorifies sleep deprivation is not just a productivity issue; it is a public health crisis. By protecting our circadian rhythms, we are not just improving our mood—we are maintaining the very cellular machinery that keeps cancer at bay.
References
- PubMed Central (National Library of Medicine) – Research on Circadian Rhythm and Immune Function.
- World Health Organization (WHO) – Global Cancer Fact Sheets.
- The Lancet – Longitudinal studies on hematologic malignancies in young adults.
- Centers for Disease Control and Prevention (CDC) – Guidelines on sleep and chronic disease prevention.
