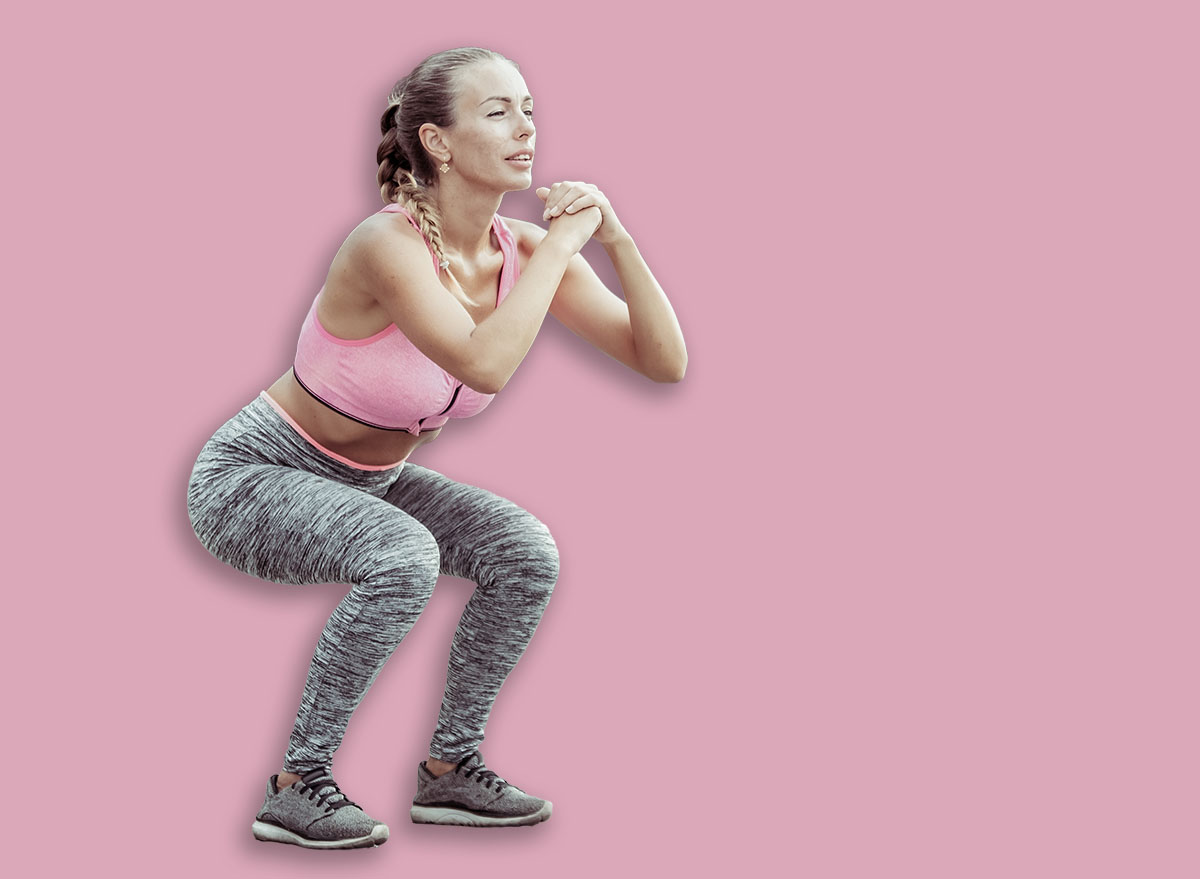Maintaining lower-body strength after age 60 is a primary predictor of functional independence and reduced fall-related morbidity. A 60-second timed squat test serves as a valid, equipment-free diagnostic tool to assess neuromuscular control, cardiorespiratory endurance, and musculoskeletal integrity, helping clinicians identify patients at risk for sarcopenia and mobility decline.
In Plain English: The Clinical Takeaway
- Sarcopenia Screening: This test identifies age-related muscle mass loss, which can lead to frailty.
- Neuromuscular Efficiency: Performing controlled squats requires your brain to communicate effectively with your motor neurons, improving balance and coordination.
- Metabolic Demand: Because the squat engages the body’s largest muscle groups (quadriceps and gluteals), it forces the cardiovascular system to work harder, improving oxygen utilization over time.
As we navigate the mid-2026 landscape of geriatric medicine, clinical focus has shifted from mere disease management to the preservation of “functional reserve.” The 60-second squat test is not merely a fitness challenge; it is a proxy for the physiological markers of aging. In clinical practice, we observe that the ability to transition from a seated to a standing position without assistance is a hallmark of healthy aging, directly correlating with lower mortality rates in longitudinal cohorts.
The Physiology of the Kinetic Chain
When you perform a squat, you are engaging a complex kinetic chain involving the lumbar spine, pelvis, and the hip-knee-ankle complex. From a biomechanical perspective, the concentric phase (rising) requires significant force production from the vastus lateralis and gluteus maximus. When sustained for 60 seconds, the test shifts from a pure strength assessment to one of metabolic endurance.
According to the Centers for Disease Control and Prevention (CDC), falls remain the leading cause of injury-related death among adults aged 65 and older. Strengthening the lower extremities is the most evidence-based intervention to mitigate this risk. By maintaining a high rep count, you are essentially training your Type II (fast-twitch) muscle fibers, which are the first to atrophy as we age.
Clinical Benchmarks for Lower-Body Performance
The following table outlines the correlation between squat performance and functional health status based on standard geriatric assessment protocols.
| Repetitions (60s) | Functional Classification | Clinical Implication |
|---|---|---|
| <15 | High Risk | Potential sarcopenia; requires physical therapy referral. |
| 15–25 | Below Average | Suboptimal endurance; increased risk of fall-related injury. |
| 25–35 | Functional | Adequate strength for daily activities of living (ADLs). |
| 35–45 | High Performance | Strong musculoskeletal reserve; low risk of frailty. |
| 45+ | Excellent | Athletic-level neuromuscular control. |
Expert Perspectives on Functional Aging
The medical community emphasizes that the quality of movement—not just the quantity—is paramount. Dr. Maria Constanza, a leading researcher in geriatric kinesiology, notes: “The goal of these assessments is to prevent ‘disuse syndrome.’ When we measure squats, we are measuring the nervous system’s ability to recruit motor units under the stress of fatigue. If the form breaks down, the risk of injury outweighs the benefit of the exercise.”
the World Health Organization (WHO) guidelines on physical activity for older adults highlight that multicomponent physical activity programs that emphasize functional balance and strength training are the most effective way to prevent cognitive and physical decline. This test aligns with the WHO’s recommendation for consistent, weight-bearing exercise.
Contraindications & When to Consult a Doctor
While the squat is a foundational human movement, it is not universally appropriate for every patient. Before initiating this or any high-repetition exercise regimen, you must consult with your primary care provider or a physical therapist, particularly if you have the following contraindications:
- Advanced Osteoarthritis: Patients with significant degenerative joint disease in the knees or hips may experience cartilage irritation.
- Cardiovascular Instability: If you have a history of unstable angina, uncontrolled hypertension, or recent myocardial infarction, the metabolic demand of this test could be hazardous.
- Vestibular Disorders: Patients with vertigo or balance-related inner ear conditions should perform these movements only with supervision to prevent falls.
- Recent Surgical History: Post-operative recovery protocols for hip or knee arthroplasty require physician-led rehabilitation, not self-directed fitness testing.
If you experience sharp pain, dizziness, palpitations, or shortness of breath beyond standard exertion, cease the test immediately and seek medical evaluation.
Funding and Transparency
Research regarding functional fitness benchmarks, such as those published in the Journal of Geriatric Physical Therapy, is frequently funded by independent grants from the National Institutes of Health (NIH) or national health ministries. These studies are peer-reviewed to ensure that industry-sponsored bias—often present in proprietary fitness app research—is eliminated. The recommendations provided here are based on the consensus of clinical exercise physiology, not commercial interest.
By focusing on the “Information Gap”—the transition from sitting to standing as a clinical marker—we can better prepare for the long-term health challenges of an aging population. Consistency, rather than intensity, remains the gold standard for maintaining the strength necessary to thrive well into your 70s, 80s, and beyond.
References
- World Health Organization: WHO Guidelines on Physical Activity and Sedentary Behaviour
- JAMA Network Open: Association of Muscle Strength with All-Cause Mortality
- CDC: Stopping Elderly Accidents, Deaths & Injuries (STEADI) Tool Kit for Healthcare Providers
Disclaimer: This article is for informational purposes only and does not constitute formal medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or before beginning any new exercise program.