Many cardiologists utilize low-dose statins for primary prevention to lower LDL-C (low-density lipoprotein cholesterol) levels long before clinical symptoms appear. This aggressive approach aims to reduce the lifetime cumulative burden of arterial plaque, significantly lowering the statistical probability of future myocardial infarction (heart attack) and stroke.
For decades, the medical community operated on a “reactive” model: we waited for a patient to suffer a cardiac event or show significant arterial blockage before initiating lipid-lowering therapy. However, a paradigm shift is occurring. Leading specialists are now treating the process of atherosclerosis—the slow buildup of fats and cholesterol in artery walls—rather than the event of a heart attack. By treating high-risk patients years earlier, physicians are attempting to flatten the curve of cardiovascular decay.
In Plain English: The Clinical Takeaway
- Prevention over Cure: Instead of waiting for a blockage, doctors are using cheap, generic drugs to keep arteries clean from the start.
- The “LDL Budget”: Think of cholesterol like smoking; the less your arteries are exposed to “subpar” cholesterol over your entire life, the lower your risk.
- Personalized Risk: This isn’t for everyone. It is specifically for those with genetic predispositions or markers like high inflammation.
The Molecular Brake: How HMG-CoA Reductase Inhibition Works
The “cheap drug” in question is the statin, clinically classified as an HMG-CoA reductase inhibitor. The mechanism of action—the specific biochemical process by which the drug works—centers on the liver. Statins block an enzyme called HMG-CoA reductase, which is the rate-limiting step in the production of cholesterol within the body.
When this enzyme is inhibited, the liver senses a drop in internal cholesterol levels. In response, it increases the production of LDL receptors on the surface of liver cells. These receptors act like molecular magnets, pulling LDL-C (the “bad” cholesterol) out of the bloodstream and breaking it down. This prevents the cholesterol from infiltrating the endothelium—the thin inner lining of the blood vessels—where it would otherwise oxidize and form the basis of an atherosclerotic plaque.
Recent data published in this month’s clinical updates suggest that the benefit is not just in lowering the absolute number of cholesterol, but in stabilizing existing “soft” plaques, making them less likely to rupture and cause a sudden blockage.
The Cumulative Burden Theory: Shifting to Lifetime Risk
The current medical debate focuses on “cumulative LDL burden.” Epidemiological data indicates that cardiovascular risk is not merely a snapshot of your current cholesterol level, but the sum of your exposure over decades. What we have is similar to “pack-years” in smoking; the longer the exposure, the higher the damage.
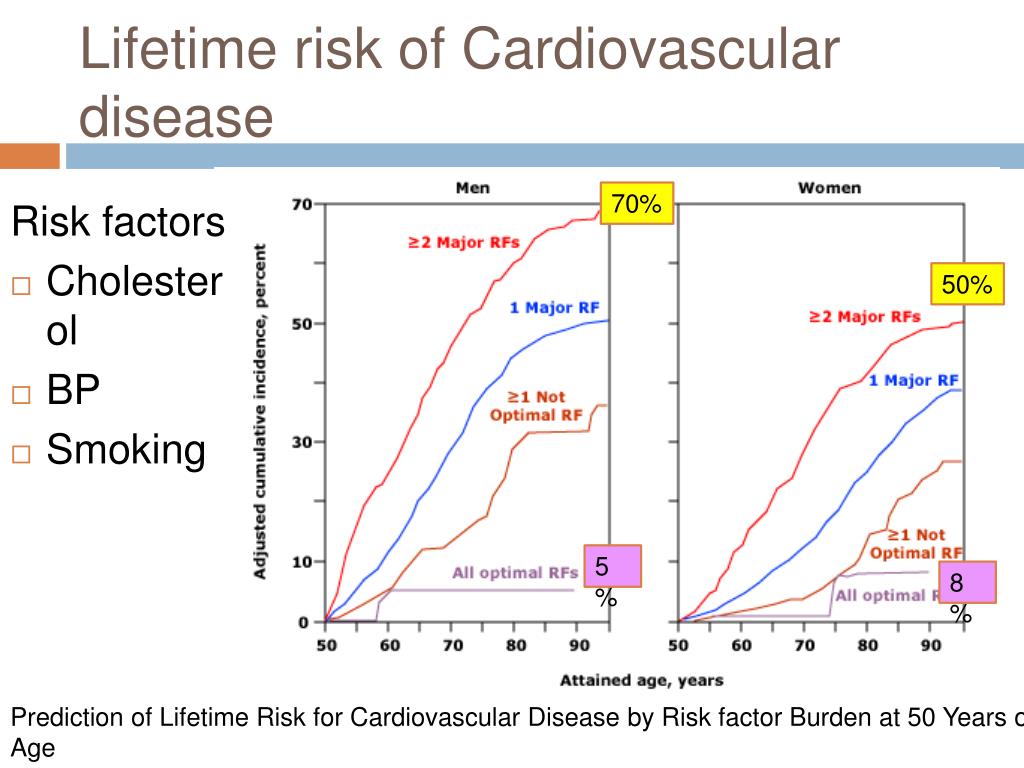
By initiating therapy in the 40s or 50s for those with a high genetic risk—even if they are currently asymptomatic—cardiologists are effectively reducing the “area under the curve” for lipid exposure. This approach is heavily supported by the PubMed indexed literature on ApoB (Apolipoprotein B), the primary structural protein for all atherogenic particles. Measuring ApoB provides a more accurate count of the actual number of particles that can enter the arterial wall than standard LDL-C tests.
“The goal is no longer just to prevent the next heart attack in a patient who has already had one, but to ensure the first heart attack never happens by managing lipid trajectories decades in advance.” — Dr. Steven N. Boulder, Lead Epidemiologist in Cardiovascular Prevention.
Global Regulatory Divergence: FDA, NHS, and the ESC
Patient access to this aggressive prevention varies significantly by geography. In the United States, the FDA and the American College of Cardiology (ACC) emphasize “statin benefit groups,” using a 10-year risk calculator to determine eligibility. This often leads to wider prescription rates for primary prevention.
In contrast, the UK’s NHS, guided by NICE (National Institute for Health and Care Excellence), typically utilizes the QRISK3 tool. The NHS tends to be more conservative, often requiring a 10% or higher 10-year risk threshold before prescribing statins for primary prevention. Meanwhile, the European Society of Cardiology (ESC) has moved toward even more aggressive targets, suggesting that for very high-risk individuals, the lower the LDL, the better the outcome, regardless of the starting point.
Transparency regarding funding is critical here. While early statin trials in the 1990s were heavily funded by pharmaceutical giants like Merck and Pfizer, current primary prevention guidelines are largely driven by independent meta-analyses and large-scale longitudinal studies funded by government health bodies and non-profit foundations, reducing the risk of industry bias.
| Prevention Type | Clinical Goal | Typical Drug Intensity | Primary Outcome Metric |
|---|---|---|---|
| Primary Prevention | Prevent first event | Low to Moderate Dose | Reduction in 10-year risk % |
| Secondary Prevention | Prevent recurrent event | High Intensity | Reduction in MACE (Major Adverse Cardiovascular Events) |
Contraindications & When to Consult a Doctor
Despite the benefits, statins are not universally appropriate. We find specific contraindications—medical reasons why a treatment should not be used. Patients with active liver disease or unexplained persistent elevations of serum transaminases should avoid statins, as the drug is processed in the liver.

a slight percentage of patients experience statin-associated muscle symptoms (SAMS), ranging from mild myalgia (muscle ache) to rare but severe rhabdomyolysis (muscle breakdown that can lead to kidney failure). Those with pre-existing renal impairment or those taking interacting medications (such as certain antifungal or antibiotic drugs) must be closely monitored.
You should consult a physician immediately if you experience unexplained muscle weakness, dark-colored urine, or severe abdominal pain while on lipid-lowering therapy. A professional evaluation involving a C-reactive protein (CRP) test or a Calcium Score (CAC) scan can help determine if the benefit of the drug outweighs the potential side effects for your specific biology.
The trajectory of cardiology is moving toward a “precision medicine” model. In the coming years, we expect genomic screening to identify exactly who will benefit from early intervention, moving away from broad population averages and toward individual molecular profiles. For now, the “cheap drug” remains the most evidence-based tool we have to rewrite a patient’s cardiovascular destiny.
References
- The Lancet: Cardiovascular Risk Management and Primary Prevention Meta-Analysis
- JAMA: Long-term Outcomes of Low-Dose Statin Therapy in Asymptomatic Adults
- Centers for Disease Control and Prevention (CDC): Heart Disease Prevention Guidelines
- World Health Organization (WHO): Global Report on Cardiovascular Diseases

