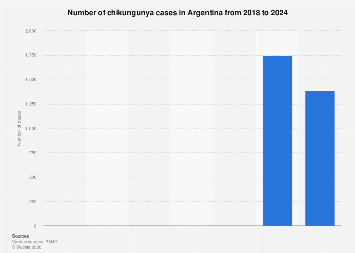
Argentina has recorded over 1,500 confirmed cases of chikungunya in early 2026. This surge, driven by the Aedes mosquito vector, signals an intensifying public health challenge in South America, requiring urgent vector control and clinical vigilance to prevent chronic joint morbidity in the affected population.
The current spike in cases is not merely a regional statistical anomaly; it represents a broader epidemiological shift. For the global community, this outbreak underscores the volatility of arboviruses—viruses transmitted by arthropods—and the ease with which they can establish endemicity in novel territories. When a virus like chikungunya (CHIKV) takes hold, the primary concern for clinicians is not the acute febrile phase, but the potential for chronic inflammatory rheumatism that can disable patients for years.
In Plain English: The Clinical Takeaway
- Transmission: You cannot catch chikungunya from another person; This proves spread exclusively through the bite of an infected mosquito.
- The Main Symptom: While fever is common, the “signature” of this virus is severe joint pain (arthralgia) that can be debilitating.
- Prevention: There is no cure once infected; the best defense is eliminating standing water where mosquitoes breed and using EPA-approved repellents.
The Viral Mechanism: From Vector Inoculation to Chronic Arthralgia
The pathogenesis of chikungunya begins when an infected Aedes aegypti or Aedes albopictus mosquito inoculates the human dermis with the virus. The mechanism of action—the specific way the virus produces an effect in the body—involves the virus targeting fibroblasts (connective tissue cells) and macrophages (immune cells). This triggers a massive release of pro-inflammatory cytokines, which are signaling proteins that coordinate the immune response.

While the initial fever usually subsides within a week, the virus often induces a persistent inflammatory state in the synovial membrane—the lining of the joints. This leads to chronic arthralgia, or severe joint pain. In a significant percentage of patients, this transition from acute to chronic phase mimics rheumatoid arthritis, causing long-term stiffness and reduced mobility. This cellular infiltration of the joints is what makes chikungunya particularly devastating compared to other seasonal viruses.
“The challenge with the 2026 surge in the Southern Cone is the increasing frequency of chronic cases. We are seeing patients who, months after the initial infection, still present with debilitating joint inflammation that requires long-term rheumatological management,” states Dr. Elena Rossi, an epidemiologist specializing in tropical medicine.
Climate Shifts and the Expansion of the Aedes Vector
The expansion of chikungunya into wider regions of Argentina is inextricably linked to geo-epidemiological shifts. Warming average temperatures and altered precipitation patterns have expanded the habitable zone for the Aedes mosquito. Previously, the cooler climates of southern Argentina acted as a natural barrier; however, current data suggests a northward-to-southward migration of the vector.

This shift creates a “surveillance gap” where healthcare providers in non-endemic areas may not initially recognize the symptoms, leading to misdiagnosis as dengue or Zika. This represents critical because the clinical management differs. For instance, the use of certain medications is contraindicated (advised against) until dengue is ruled out, as dengue can cause hemorrhage, which certain painkillers exacerbate.
From a global regulatory perspective, this puts pressure on the World Health Organization (WHO) and the Pan American Health Organization (PAHO) to accelerate the distribution of diagnostic kits and vector-control funding. Most of the current funding for these initiatives is provided by member states through the WHO’s Programme for Mosquito-borne Diseases, though critics argue that funding often arrives after an outbreak has already peaked.
Comparing the Tropical Triple Threat: CHIKV, DENV, and ZIKV
To understand the clinical urgency, it is essential to differentiate chikungunya from its “cousins,” Dengue and Zika, which are often co-circulating in the same regions.
| Clinical Feature | Chikungunya (CHIKV) | Dengue (DENV) | Zika (ZIKV) |
|---|---|---|---|
| Primary Symptom | Severe Joint Pain | High Fever / Muscle Pain | Rash / Conjunctivitis |
| Joint Involvement | High (Often Chronic) | Moderate (Acute) | Mild |
| Hemorrhagic Risk | Low | High (Severe Dengue) | Low |
| Neurological Risk | Rare | Low | High (Microcephaly/GBS) |
| Incubation Period | 3–7 Days | 4–10 Days | 3–14 Days |
The Global Vaccine Landscape and Regulatory Hurdles
The arrival of the first approved chikungunya vaccines, such as the live-attenuated options approved by the FDA and EMA, represents a pivotal shift in public health. However, the “last mile” delivery—getting the vaccine from the warehouse to the patient in rural Argentina—remains a hurdle. The efficacy of these vaccines is high, but their deployment is often hampered by cold-chain requirements (the need to preserve vaccines at specific low temperatures).
Current Phase III trial data indicates that these vaccines significantly reduce the incidence of severe arthralgia. However, the cost-benefit analysis for government procurement often lags behind the actual rate of infection. For patients in the US or Europe who have traveled to Argentina, the focus remains on post-exposure monitoring and ensuring that any joint pain is treated with evidence-based anti-inflammatories rather than unverified “natural” cures.
Contraindications & When to Consult a Doctor
Medical intervention is critical if you suspect a chikungunya infection. Do not self-medicate with aspirin or non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen until a healthcare provider has ruled out Dengue fever, as these can increase the risk of bleeding in Dengue patients.
Seek immediate emergency care if you experience any of the following “red flag” symptoms:
- Neurological Changes: Sudden confusion, seizures, or severe disorientation.
- Hemodynamic Instability: Extreme lethargy, cold extremities, or a significant drop in blood pressure.
- Respiratory Distress: Difficulty breathing or shortness of breath.
- Severe Dehydration: Inability to keep fluids down due to persistent vomiting.
Patients with pre-existing autoimmune conditions, such as rheumatoid arthritis, should consult their specialist immediately upon infection, as the virus can trigger a severe exacerbation of their underlying condition.
While the 1,500 cases in Argentina are a sobering reminder of the persistence of arboviruses, they also serve as a catalyst for better regional cooperation. The path forward requires a synthesis of aggressive vector control, rapid molecular diagnostics, and a global commitment to vaccine equity. By treating this not as a localized “outbreak” but as a symptom of a changing global climate, we can move from reactive treatment to proactive prevention.

