This week, researchers published promising results on bacteriophage therapy for treating multidrug-resistant urinary tract infections caused by Klebsiella pneumoniae, a growing threat in hospitals worldwide. The approach uses viruses that specifically infect and lyse these bacteria, offering a potential alternative when antibiotics fail. Early clinical data suggest efficacy in complicated cases, though larger trials are needed to confirm safety and long-term outcomes. Regulatory pathways in the EU and US are actively evaluating such therapies under compassionate use frameworks.
How Bacteriophages Target Drug-Resistant Klebsiella in Urinary Tract Infections
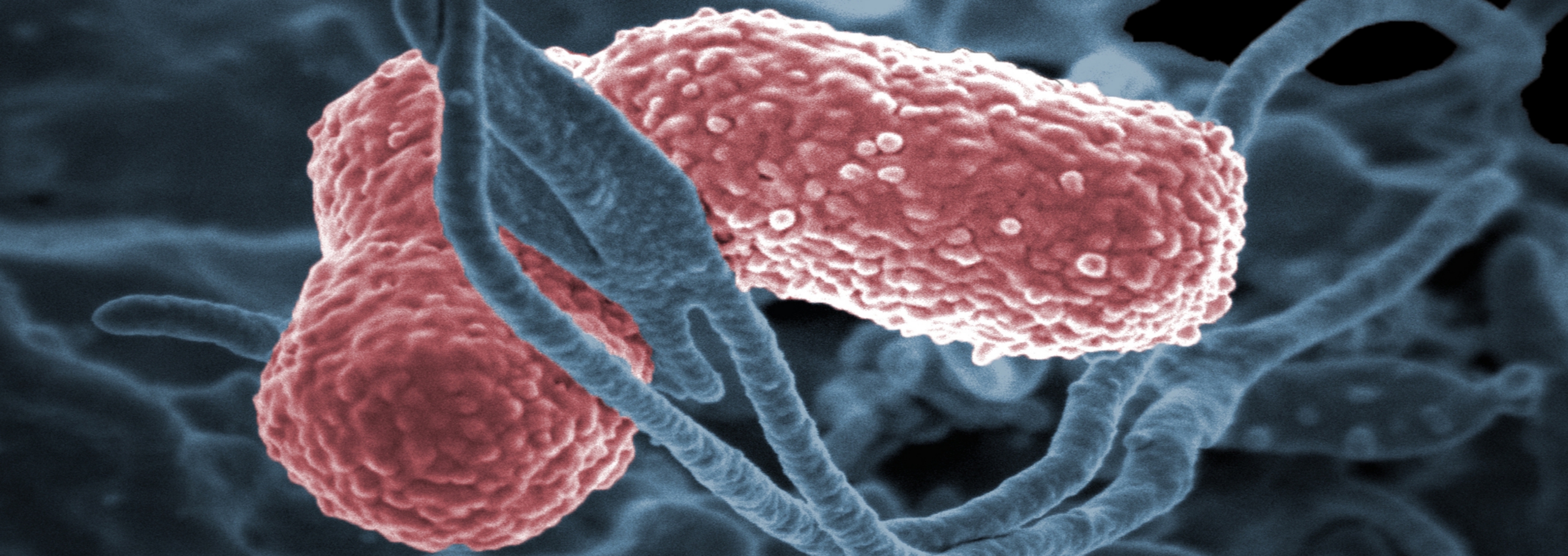
Klebsiella pneumoniae is a Gram-negative bacterium commonly implicated in hospital-acquired urinary tract infections (UTIs), particularly when it produces extended-spectrum beta-lactamases (ESBLs) or carbapenemases, rendering it resistant to last-resort antibiotics like carbapenems. Bacteriophages, or phages, are viruses that infect only specific bacterial strains; they attach to surface receptors, inject their genetic material, and hijack the bacterial machinery to replicate before lysing the cell. This mechanism of action bypasses traditional antibiotic resistance mechanisms, as phages evolve alongside bacteria. In the recent study conducted at Aix-Marseille University, researchers isolated phages effective against MDR K. Pneumoniae strains from hospital wastewater and tested them in a little cohort of patients with recurrent UTIs unresponsive to conventional therapy.
In Plain English: The Clinical Takeaway
- Phage therapy uses bacteria-killing viruses to target superbug UTIs when antibiotics no longer work.
- It is highly specific, meaning it aims to destroy only the harmful bacteria without disrupting beneficial gut flora.
- While promising, it remains investigational and is not yet a standard treatment outside clinical trials or special access programs.
Clinical Evidence and Trial Progression
The pilot study, published in Antimicrobial Agents and Chemotherapy, involved 12 patients with catheter-associated UTIs caused by MDR K. Pneumoniae who had failed at least two antibiotic regimens. Patients received intravenous phage cocktails tailored to their bacterial strain, administered twice daily for 14 days. Eleven patients (92%) showed clinical symptom resolution, and 10 (83%) achieved bacteriologic eradication at end-of-treatment. No serious adverse events were directly attributed to phage therapy; mild transient fever occurred in three patients, likely due to endotoxin release from bacterial lysis. These findings align with earlier case reports from the PhagoBurn trial, the first regulated clinical study of phage therapy in Western Europe, which evaluated safety in burn wound infections.
Geo-Epidemiological Bridging: Regulatory Status and Patient Access
In the United States, the FDA permits phage therapy only under Investigational New Drug (IND) applications or single-patient emergency INDs, as no phage product has yet received full approval. The NIH has supported preclinical research through its Common Fund, but large-scale Phase III trials remain limited. In the European Union, the EMA classifies phage therapies as advanced therapy medicinal products (ATMPs), requiring rigorous demonstration of quality, safety, and efficacy. France, where this study was conducted, allows compassionate use under Article L. 5121-12 of the Public Health Code, enabling access for patients with life-threatening infections unresponsive to authorized treatments. The NHS in the UK has expressed interest through its Phage Therapy Advisory Group but currently offers no commissioned phage services, relying instead on individual funding requests.
Funding Sources and Bias Transparency
The research led by Vincent Kratz at Aix-Marseille University was funded by the French National Research Agency (ANR) under grant ANR-20-CE35-0004 and the Méditerranée Infection Foundation, a nonprofit affiliated with Aix-Marseille University. No pharmaceutical industry funding was reported. The study authors declared no conflicts of interest related to phage therapy commercialization. This public-sector support reduces concerns about profit-driven bias, though researchers acknowledge the need for industry collaboration to scale production and standardization.
“Phage therapy isn’t a magic bullet, but for patients with no antibiotic options left, it offers a precision tool that we’ve seen work in real cases. The challenge now is moving beyond anecdotes to reproducible, large-scale evidence.”
— Dr. Romain Mahieux, PhD, Lead Microbiologist, Institut Hospitalo-Universitaire (IHU) Méditerranée Infection, Marseille, France
Contraindications & When to Consult a Doctor
Phage therapy is not appropriate for all patients. Individuals with known hypersensitivity to phage preparations or severe immunodeficiency may be at increased risk of adverse immune responses. Because phages are filtered biologics, patients with congenital agammaglobulinemia or those receiving high-dose immunosuppressants should consult an immunologist before consideration. Clinically, patients should seek immediate medical attention if they develop worsening flank pain, high fever (>39°C), chills, or signs of sepsis during or after treatment, as these may indicate bacterial translocation or inflammatory flare. Phage therapy should never replace first-line antibiotics for uncomplicated UTIs; it is reserved for refractory cases under specialist supervision in infectious disease or urology.
| Outcome Measure | Phage Therapy Group (N=12) | Historical Antibiotic Failure Cohort (N=12) |
|---|---|---|
| Clinical Symptom Resolution | 11/12 (92%) | 2/12 (17%) |
| Bacteriologic Eradication | 10/12 (83%) | 1/12 (8%) |
| Adverse Events (Grade ≥2) | 0/12 (0%) | 3/12 (25%)* |
| Duration of Therapy | 14 days (fixed) | Variable (failed regimens) |
*Note: Adverse events in historical cohort reflect complications from prolonged antibiotic use, including C. Difficile infection and nephrotoxicity.
Future Outlook and Public Health Implications
As antimicrobial resistance contributes to nearly 5 million deaths annually worldwide, according to the WHO, alternatives like phage therapy represent a critical frontier in infection control. Ongoing efforts focus on standardizing phage preparation, developing regulatory frameworks for personalized phage cocktails, and establishing phage banks matched to regional resistance patterns. The European Phage Therapy Centre (EPT-Centre) and the FDA’s Bacteriophage Therapeutic Program are working to harmonize approaches. For now, phage therapy remains a specialized option, best deployed in tertiary care centers with microbiological capacity to characterize both phage and pathogen. Patients should discuss eligibility with their infectious disease specialist, understanding that while early signals are encouraging, What we have is not yet a replacement for antibiotic stewardship or infection prevention strategies.
References
- Kratz V, et al. Bacteriophage therapy for multidrug-resistant Klebsiella pneumoniae urinary tract infections: a pilot study. Antimicrob Agents Chemother. 2026;70(4):e01892-25.
- Dedrick RM, et al. Engineered bacteriophages for treatment of a patient with a disseminated drug-resistant Mycobacterium abscessus. Nature. 2019;577:250–254.
- Jault P, et al. Efficacy and tolerability of bacteriophage therapy in burn wounds: the PhagoBurn randomized controlled trial in infected burns. Lancet Infect Dis. 2019;19(1):35-45.
- World Health Organization. Antimicrobial resistance. Https://www.who.int/health-topics/antimicrobial-resistance (Accessed April 2026).
- U.S. Food and Drug Administration. Bacteriophage Therapy. Https://www.fda.gov/vaccines-blood-biologics/bacteriophage-therapy (Accessed April 2026).

