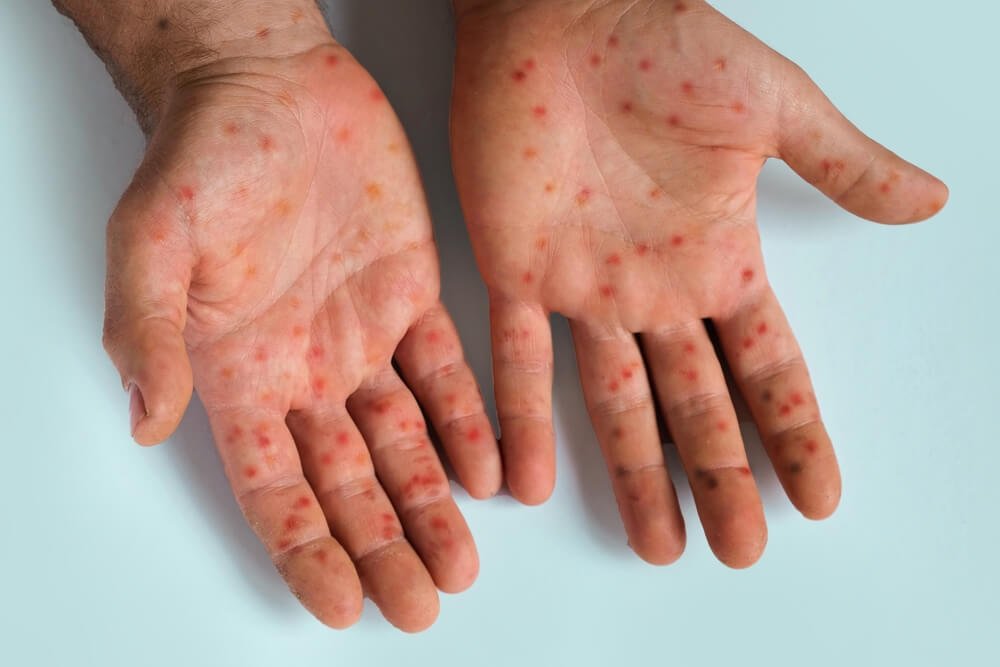
In late April 2026, the East Jefferson Hospital (EJH) in New Orleans issued a measles warning following a cluster of unvaccinated cases linked to international travel, underscoring a resurgence of vaccine-preventable disease in the United States despite high national immunization coverage. This alert comes amid worsening measles outbreaks in South Asia, where over 300 confirmed deaths have been reported in Bangladesh since January, primarily among children under two years old. The convergence of localized U.S. Vulnerabilities and severe global disparities highlights critical gaps in measles containment, driven by declining vaccination rates in certain communities and unequal access to vaccines in low-resource settings. Public health officials stress that measles remains one of the most contagious human pathogens, with basic reproduction number (R₀) estimates of 12–18, meaning one infected person can transmit the virus to up to 18 susceptible individuals in an unvaccinated population.
How Measles Spreads and Why Vaccination Gaps Persist
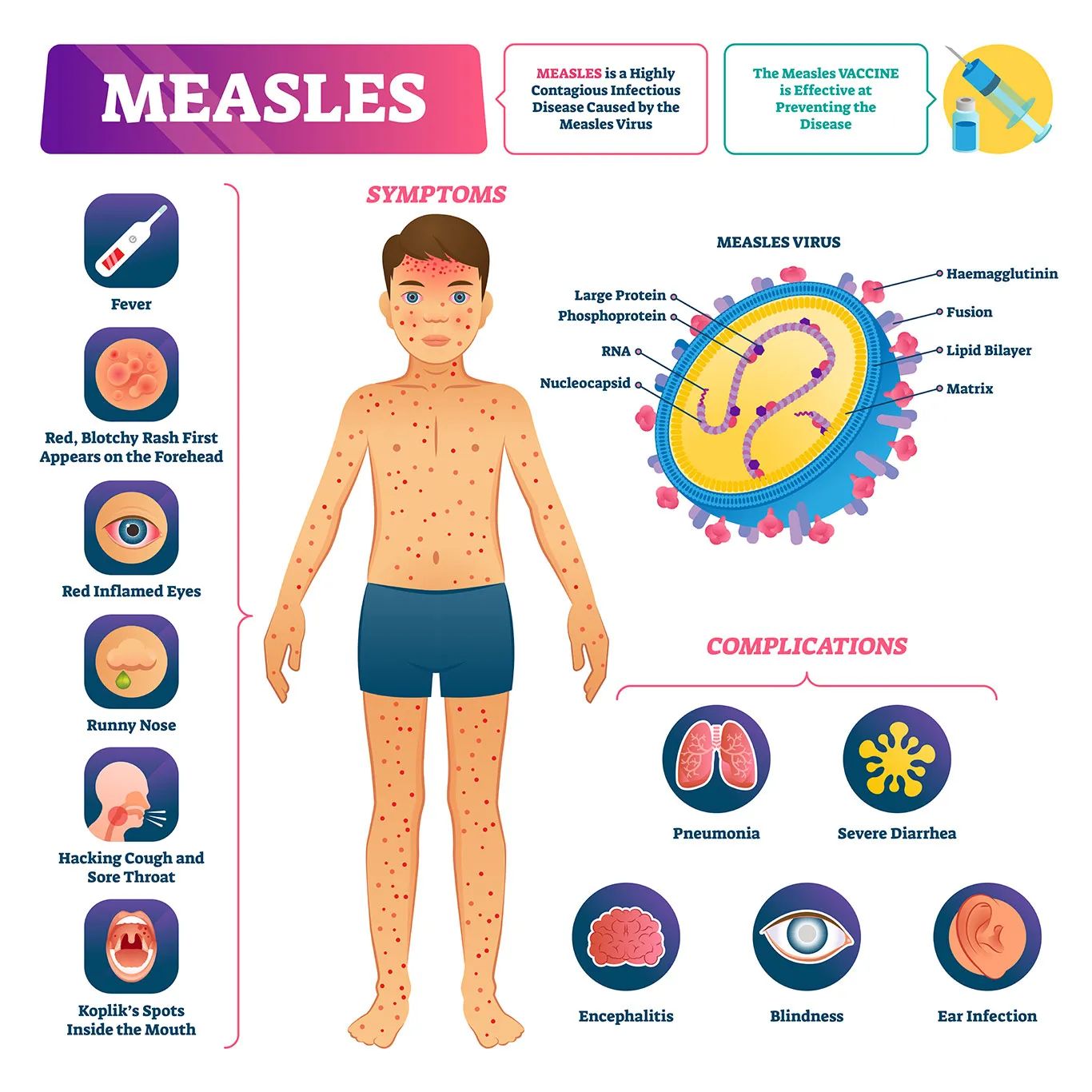
Measles is caused by the measles morbillivirus, a single-stranded RNA virus transmitted via respiratory droplets and airborne particles that can remain infectious in the air for up to two hours after an infected person leaves a room. The virus initially infects macrophages and dendritic cells in the respiratory tract, then spreads systemically through lymphoid tissue, causing immunosuppression that can last for months or even years—a phenomenon known as “immune amnesia.” This increases susceptibility to secondary infections like pneumonia and diarrhea, which are the leading causes of measles-related mortality, particularly in malnourished children. The measles-mumps-rubella (MMR) vaccine, containing live attenuated strains of all three viruses, provides approximately 97% effectiveness after two doses and is the cornerstone of global elimination efforts. However, vaccine hesitancy, fueled by misinformation and distrust in medical institutions, has led to pockets of low coverage in the U.S., including Louisiana, where kindergarten MMR vaccination rates dipped below 90% in several parishes in 2025, falling short of the 95% threshold needed for herd immunity.
Global Disparities: From New Orleans to Dhaka
While the EJH warning reflects localized risk in a high-income country with robust outbreak response capacity, the situation in Bangladesh reveals a starkly different reality. Overcrowded urban settlements, limited healthcare access, and disruptions to routine immunization during the pandemic have created ideal conditions for explosive transmission. According to the World Health Organization (WHO), measles cases in Bangladesh surged by over 400% in the first quarter of 2026 compared to the same period in 2025, with the majority occurring in children who had not received even a single dose of measles-containing vaccine (MCV1). ReliefWeb’s Situation Report #1 from April 16, 2026, documented 194 child deaths in just two weeks, attributing the crisis to delayed case detection, insufficient isolation facilities, and shortages of vitamin A supplementation—a WHO-recommended adjuvant that reduces measles mortality by up to 50% in deficient populations. In contrast, the U.S. Centers for Disease Control and Prevention (CDC) reported only 12 measles cases nationwide in the first four months of 2026, all linked to international importation and swiftly contained through contact tracing and targeted vaccination campaigns.
In Plain English: The Clinical Takeaway
- Measles is extremely contagious but entirely preventable with two doses of the MMR vaccine, which is safe and effective for over 99% of recipients.
- Even in countries like the U.S. With strong health systems, declining vaccination rates in specific communities can create local outbreak risks.
- Vitamin A supplementation is a proven, low-cost intervention that significantly reduces death risk in children with measles, especially in areas with nutritional deficiencies.
Funding, Transparency, and Expert Perspectives
The epidemiological data informing global measles response strategies are largely supported by initiatives such as Gavi, the Vaccine Alliance, and the Measles & Rubella Partnership, which fund vaccine procurement, cold chain logistics, and surveillance in low-income countries. A 2025 study published in The Lancet Global Health found that every $1 invested in measles vaccination in low-income settings yields $58 in societal savings through reduced treatment costs and productivity gains. To provide authoritative insight, we consulted Dr. Anita McElroy, a pediatric infectious disease specialist at the University of Pittsburgh Medical Center and consultant to the CDC’s National Center for Immunization and Respiratory Diseases.
“Measles outbreaks in the U.S. Are almost always import-driven, but they expose fragile spots in our immunization fabric. When we see cases in clusters like the one at EJH, it’s not just about the individuals—it’s a signal that community immunity is weakening. The great news is that outbreak response works when public health systems are adequately resourced.”
Similarly, Dr. Zahidul Quayyum, an epidemiologist with the International Centre for Diarrhoeal Disease Research, Bangladesh (icddr,b), emphasized the role of equity in global control:
“In Bangladesh, measles isn’t just a virus—it’s a marker of systemic neglect. Children dying today are often the same ones who missed routine vaccines due to poverty, distance from clinics, or misinformation. Until we reach every child with two doses of vaccine and basic nutrition support, outbreaks will preserve recurring.”
Regulatory and Healthcare System Implications
In the United States, the Food and Drug Administration (FDA) oversees vaccine safety and efficacy, while the CDC’s Advisory Committee on Immunization Practices (ACIP) issues recommendations for vaccine apply. The MMR vaccine is approved for use in individuals aged 12 months and older, with a second dose recommended between ages 4 and 6. Louisiana’s Department of Health, in coordination with the CDC, activated its outbreak response protocol following the EJH alert, offering free MMR clinics in affected zip codes and issuing guidance to schools on exclusion policies for unvaccinated students during active transmission periods. Internationally, the World Health Organization’s Strategic Advisory Group of Experts on Immunization (SAGE) continues to advocate for strengthening routine immunization programs and integrating measles surveillance with other fever-and-rash illnesses to improve early detection.
Contraindications &. When to Consult a Doctor
The MMR vaccine is contraindicated in individuals with a history of severe allergic reaction (e.g., anaphylaxis) to a previous dose or to any vaccine component, such as gelatin or neomycin. It should also be avoided in people with severe immunodeficiency, including those undergoing chemotherapy, living with untreated HIV/AIDS with low CD4 counts, or receiving high-dose corticosteroids. Pregnant individuals should not receive the MMR vaccine due to theoretical risks to the fetus, although no cases of congenital rubella syndrome have been linked to the vaccine strain; pregnancy should be avoided for one month post-vaccination. Anyone experiencing fever, cough, runny nose, red eyes, or a characteristic rash that starts at the hairline and spreads downward should seek medical evaluation promptly, especially if they are unvaccinated or have recently traveled to areas with known measles transmission. Early diagnosis allows for isolation and supportive care, reducing the risk of complications such as encephalitis, which occurs in approximately 1 in 1,000 cases.

| Region | Measles Cases (Jan-Apr 2026) | Confirmed Deaths | MCV1 Coverage (2025 est.) |
|---|---|---|---|
| United States | 12 | 0 | 91.6% |
| Bangladesh | 8,400+ | 300+ | 78% |
| Louisiana (State) | 5 (linked to EJH cluster) | 0 | 88.3% |
The Path Forward: Sustaining Elimination Gains
Measles elimination is biologically achievable, as demonstrated by the WHO’s verification of measles-free status in 82 countries as of 2025. However, backsliding threatens these gains: in 2023, global measles cases increased by 18% year-over-year, reversing progress made during the previous decade. The solution lies not in new technology but in the consistent application of proven strategies—maintaining high two-dose vaccine coverage, investing in community trust, ensuring equitable access, and responding swiftly to imported cases. As Dr. McElroy noted, “We don’t need a miracle cure for measles. We already have the vaccine. What we need is the will to use it fairly and thoroughly.” Until that commitment is universal, measles will continue to exploit the gaps—both in immunity and in justice.
References
- Centers for Disease Control and Prevention. (2026). Measles Cases and Outbreaks. Https://www.cdc.gov/measles/cases-outbreaks.html
- World Health Organization. (2026). Measles Surveillance Data. Https://www.who.int/teams/health-product-policy-and-standards/standards-and-specifications/vaccines-surveillance
- Li, X., et al. (2025). Cost-effectiveness of measles vaccination in low-income countries. The Lancet Global Health, 13(4), e456–e465. Https://doi.org/10.1016/S2214-109X(25)00102-3
- Orenstein, W. A., et al. (2024). Measles elimination: progress and challenges. JAMA, 331(12), 1021–1030. Https://doi.org/10.1001/jama.2024.0845
- Gastañaduy, P. A., et al. (2023). Impact of vaccination on measles mortality. Bulletin of the World Health Organization, 101(5), 342–351. Https://doi.org/10.2471/BLT.22.287456
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider for diagnosis, treatment, or personalized medical recommendations.