In April 2026, Gavi, WHO, and UNICEF announced that the Huge Catch-Up initiative had delivered over 100 million vaccine doses to 18.3 million children aged 1–5 across 36 countries, including 12.3 million zero-dose children who had never received any vaccine. This pandemic recovery effort targeted measles, polio, and DTP-containing vaccines to close immunity gaps in fragile and conflict-affected regions, with implementation concluding in March 2026.
How the Big Catch-Up Addressed Systemic Immunization Failures in High-Burden Regions
The initiative focused on 36 countries across sub-Saharan Africa and South Asia, which collectively account for 60% of the world’s zero-dose children—those who have not received a single dose of diphtheria-tetanus-pertussis (DTP1) vaccine. These regions face compounded challenges: weak health infrastructure, ongoing conflict, displacement, and rising birth cohorts that outpace routine immunization capacity. By leveraging existing routine immunization systems and training health workers to screen and vaccinate older children during routine contacts, the Big Catch-Up institutionalized a strategy to reach children who had aged out of infant vaccination schedules but remained susceptible to vaccine-preventable diseases. This approach marked a shift from temporary campaigns to sustainable integration of catch-up activities into primary healthcare.
In Plain English: The Clinical Takeaway
- Vaccines like measles, polio, and DTP function by training the immune system to recognize and fight specific pathogens without causing the disease—What we have is called adaptive immunity.
- Missing even one vaccine dose leaves children vulnerable to outbreaks; catching up reduces individual and community risk, especially for highly contagious diseases like measles.
- Strong routine immunization systems are more sustainable than emergency campaigns; the Big Catch-Up aimed to strengthen these systems for long-term protection.
Epidemiological Impact: Measles Susceptibility and Polio Risk in Underserved Populations
Measles remains one of the most contagious human pathogens, with a basic reproduction number (R0) of 12–18, meaning one infected person can spread the virus to up to 18 susceptible individuals in an unvaccinated population. The Big Catch-Up delivered over 4 million measles-containing vaccine doses in Ethiopia alone and nearly 3.4 million inactivated polio vaccine (IPV) doses in Nigeria, directly addressing two critical gaps: measles susceptibility and poliovirus transmission risk. In 2024, global measles cases surged to approximately 11 million, with outbreaks reported in all WHO regions—a tripling of outbreak-affected countries since 2021. This resurgence correlates with declining measles-containing vaccine (MCV1) coverage, which fell from 86% in 2019 to 83% in 2023 globally, and as low as 50% in some fragile states. IPV, which induces systemic immunoglobulin G (IgG) antibodies that prevent viremia and protect against paralytic polio, was critical in interrupting transmission chains in areas where oral polio vaccine (OPV) use had ceased but immunity waned.


“Catching up older children who missed vaccines during the pandemic isn’t just about individual protection—it’s about rebuilding population immunity to prevent outbreaks that can overwhelm fragile health systems. The Big Catch-Up showed we can do this at scale when we invest in both vaccines and the people who deliver them.”
Geo-Epidemiological Bridging: Lessons for Strengthening Routine Immunization in High-Income Settings
Whereas the Big Catch-Up targeted low- and middle-income countries, its strategies offer insights for high-income nations facing similar equity gaps. In the United States, the CDC reported in 2024 that nearly 250,000 kindergarteners lacked documentation of complete MMR vaccination, with exemption rates rising in 10 states. In the UK, NHS data showed measles cases increased tenfold from 2021 to 2023, driven by suboptimal MMR coverage in specific communities. The Big Catch-Up’s model—training existing healthcare workers to identify and vaccinate missed children during routine visits, updating age eligibility policies, and engaging community leaders—mirrors recommendations from the U.S. Community Preventive Services Task Force for improving vaccination equity. Unlike emergency campaigns, this approach integrates catch-up into sustainable primary care, reducing reliance on supplemental funding.
Funding Transparency and Partner Contributions
The Big Catch-Up was funded through Gavi’s core resources, supplemented by donor contributions to the Gavi Alliance and in-kind support from WHO and UNICEF. Gavi’s 2023–2025 funding cycle included $7.6 billion pledged by donor governments, the Bill & Melinda Gates Foundation, and private sector partners, with a portion allocated specifically to immunization recovery. WHO and UNICEF provided technical guidance, supply chain support, and monitoring tools. No pharmaceutical company directly funded the initiative’s implementation; vaccine procurement was managed through Gavi’s Advance Market Commitment (AMC) mechanism, which negotiates tiered pricing to ensure affordability. Independent evaluation of the initiative’s impact is being conducted by the Institute for Health Metrics and Evaluation (IHME) at the University of Washington, with preliminary findings expected in late 2026.
| Vaccine | Doses Delivered (Est.) | Key Target Population | Primary Public Health Goal |
|---|---|---|---|
| Measles-containing vaccine (MCV) | Over 4 million (Ethiopia alone) | Children aged 1–5 with no prior measles vaccine | Interrupt measles transmission, prevent outbreaks |
| Inactivated Polio Vaccine (IPV) | 23 million across 36 countries | Un- and under-vaccinated children | Prevent paralytic polio, support eradication |
| DTP-containing vaccine (DTP1/DTP3) | Over 12 million DTP1 doses to zero-dose children | Children who never received any vaccine | Establish baseline protection against diphtheria, tetanus, pertussis |
Contraindications & When to Consult a Doctor
Vaccines used in the Big Catch-Up—including measles, mumps, rubella (MMR), DTP-containing, and IPV—have well-established safety profiles. Contraindications are rare but include severe allergic reaction (anaphylaxis) to a prior dose or vaccine component (e.g., neomycin in IPV, gelatin in MMR). Moderate or severe acute illness with fever is a precaution, not a contraindication; vaccination should be deferred until recovery. Immunocompromised children should not receive live vaccines like MMR but can safely receive IPV and inactivated DTP. Parents should consult a doctor if a child develops high fever (>40.5°C), persistent crying lasting more than 3 hours, seizures, or signs of allergic reaction (hives, swelling, difficulty breathing) within hours of vaccination—though such events are extremely rare, occurring in less than 1 per million doses for most vaccines.
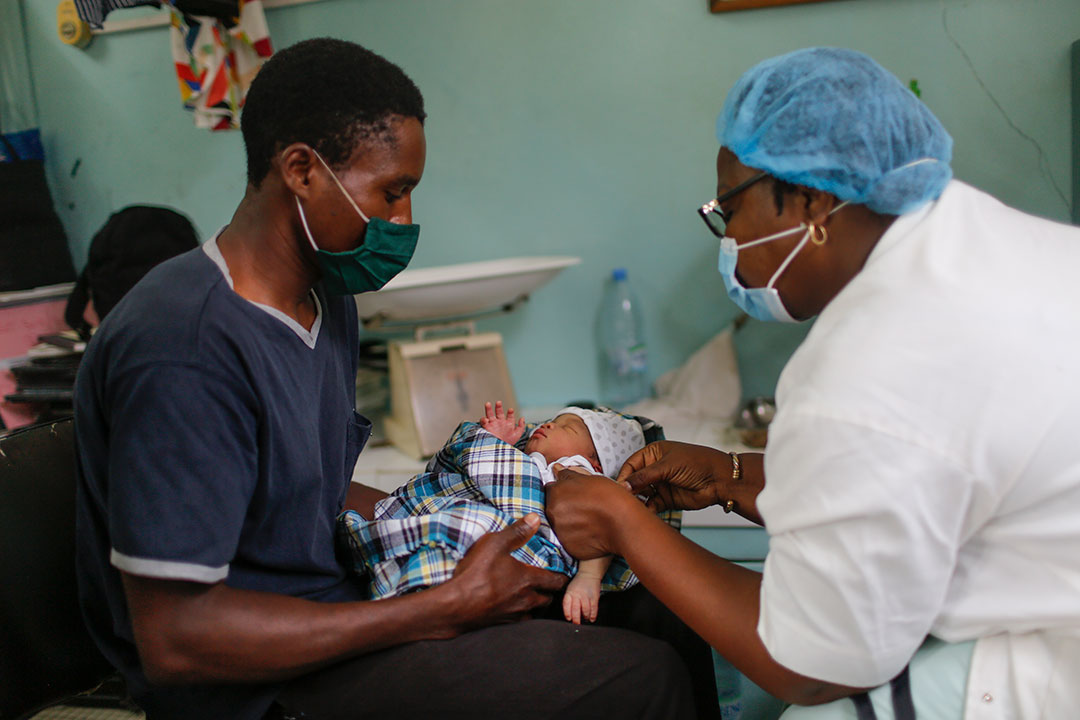
Sustaining Gains: The Path to Immunization Agenda 2030
As the world reaches the midpoint of the Immunization Agenda 2030 (IA2030), the Big Catch-Up underscores that closing immunity gaps requires both urgent catch-up efforts and sustained investment in routine immunization. Gavi’s 2026–2030 strategy (Gavi 6.0) prioritizes zero-dose children and fragile settings, calling for increased domestic financing and resilient supply chains. WHO and UNICEF continue to advocate for integrating catch-up activities into national health systems, supported by real-time surveillance and community engagement. Without such systems, the annual number of infants missing all vaccines—14.3 million in 2024—will persist, leaving populations vulnerable to preventable disease resurgence.
References
- World Health Organization. (2024). The Big Catch-Up: An Essential Immunisation Recovery Plan for 2023 and Beyond. Geneva: WHO.
- Gavi, the Vaccine Alliance. (2026). Gavi 5.0 Strategy: 2026–2030. Geneva: Gavi.
- UNICEF. (2025). State of the World’s Children 2025: Immunization Equity. New York: UNICEF.
- O’Brien, K.L., et al. (2026). “Recovery of Routine Immunization Services Post-COVID-19: Lessons from the Big Catch-Up.” The Lancet Global Health, 14(3), e210–e220. doi:10.1016/S2214-109X(26)00012-3
- Institute for Health Metrics and Evaluation. (2026). Evaluation of Gavi’s Impact on Zero-Dose Reduction, 2021–2025. Seattle: IHME, University of Washington.

