As of 2026, cesarean section (C-section) delivery remains the most frequently performed surgical procedure in the United States, accounting for approximately 32% of all births according to the latest CDC National Vital Statistics Report. This high rate reflects a complex interplay of clinical indications, maternal request, systemic healthcare factors, and evolving obstetric guidelines, with significant variation across states, hospital types, and demographic groups. Understanding the risks, benefits, and appropriate indications for C-section is critical for informed maternal decision-making and reducing preventable morbidity.
Why C-Section Rates Remain High Despite Clinical Guidelines
The World Health Organization (WHO) recommends an ideal C-section rate between 10% and 15% to optimize maternal and neonatal outcomes, yet the U.S. Rate has more than doubled this threshold. Contributing factors include rising maternal age, increased prevalence of obesity and gestational diabetes, fear of litigation leading to defensive medicine, and hospital scheduling efficiencies. A 2024 study in Obstetrics & Gynecology found that non-medically indicated early-term deliveries (37–38 weeks) scheduled for physician convenience still occur in nearly 10% of low-risk pregnancies, despite clear evidence linking such interventions to increased neonatal respiratory morbidity.
Mechanistically, C-section involves surgical incision through the abdominal wall and uterus to deliver the fetus, bypassing vaginal birth. While life-saving in cases of placenta previa, fetal distress, or cephalopelvic disproportion, the procedure carries inherent risks including hemorrhage, infection, thromboembolism, and potential complications in future pregnancies such as uterine rupture or placenta accreta spectrum disorder. These risks are dose-dependent, with each subsequent C-section increasing the likelihood of placental implantation abnormalities.
In Plain English: The Clinical Takeaway
- For most low-risk pregnancies, vaginal birth after cesarean (VBAC) is a safe option, with success rates of 60–80% when attempted in appropriate candidates.
- Planned C-sections without medical indication increase the risk of breathing problems in newborns and longer maternal recovery compared to vaginal birth.
- Hospitals with midwife-led care models and doula support show consistently lower C-section rates without compromising safety.
Geographic and Systemic Disparities in Access and Outcomes
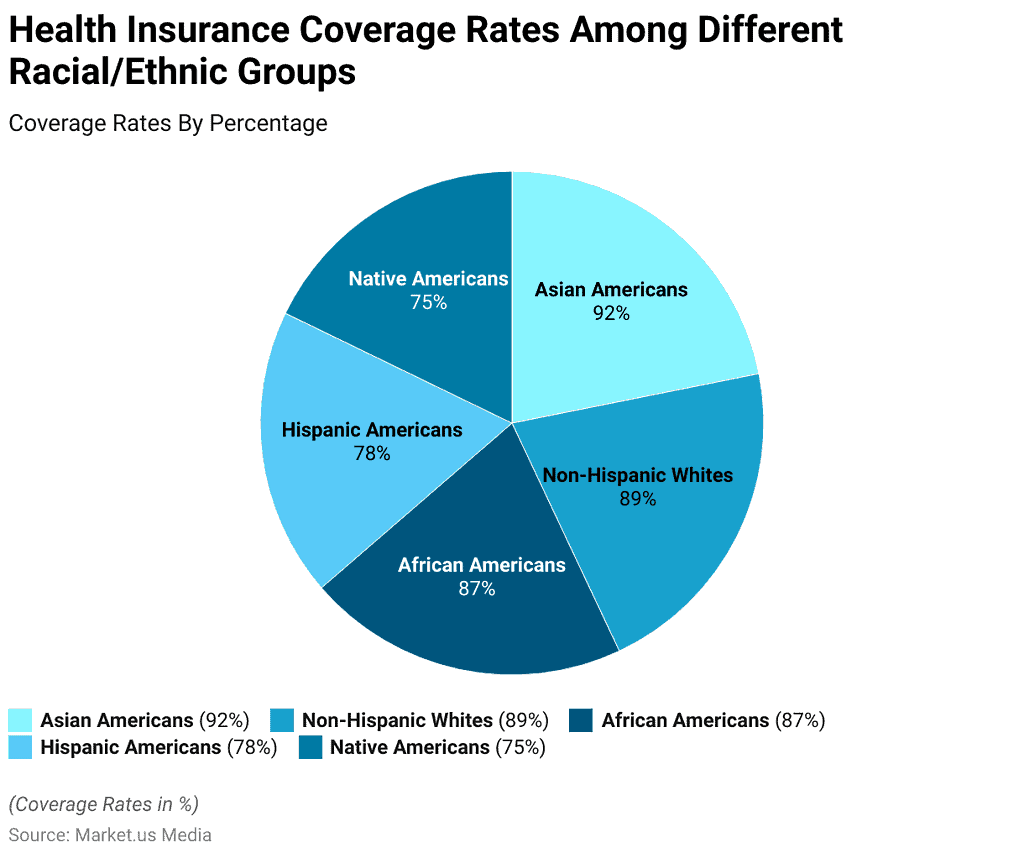
C-section rates vary significantly by region and facility type. Data from the Agency for Healthcare Research and Quality (AHRQ) show that rates exceed 40% in some Southern states, while integrated systems like Kaiser Permanente in California maintain rates below 25% through standardized labor management protocols and shared decision-making tools. These disparities correlate with insurance type, race, and socioeconomic status: Black women are 20% more likely to undergo unscheduled C-section and 50% more likely to experience severe maternal morbidity compared to White women, even after adjusting for comorbidities.
The financial burden is substantial. A 2023 analysis in Health Affairs estimated that reducing the national C-section rate to the WHO-recommended range could save over $5 billion annually in direct medical costs. Conversely, unnecessary procedures contribute to avoidable harm. the CDC estimates that over 20,000 severe maternal morbidity events each year are potentially preventable through improved obstetric care.
Evidence-Based Guidelines and Clinical Trial Evidence
Major obstetric societies, including the American College of Obstetricians and Gynecologists (ACOG) and the Society for Maternal-Fetal Medicine (SMFM), emphasize that C-section should be performed only when maternal or fetal benefits outweigh risks. This is informed by decades of clinical research, including the Term Breech Trial (2000), which demonstrated improved perinatal outcomes with planned C-section for breech presentation at term, and the ARRIVE Trial (2018), which found no significant reduction in composite perinatal morbidity with elective induction at 39 weeks compared to expectant management, though it did show a slight reduction in C-section rates in the induction group.
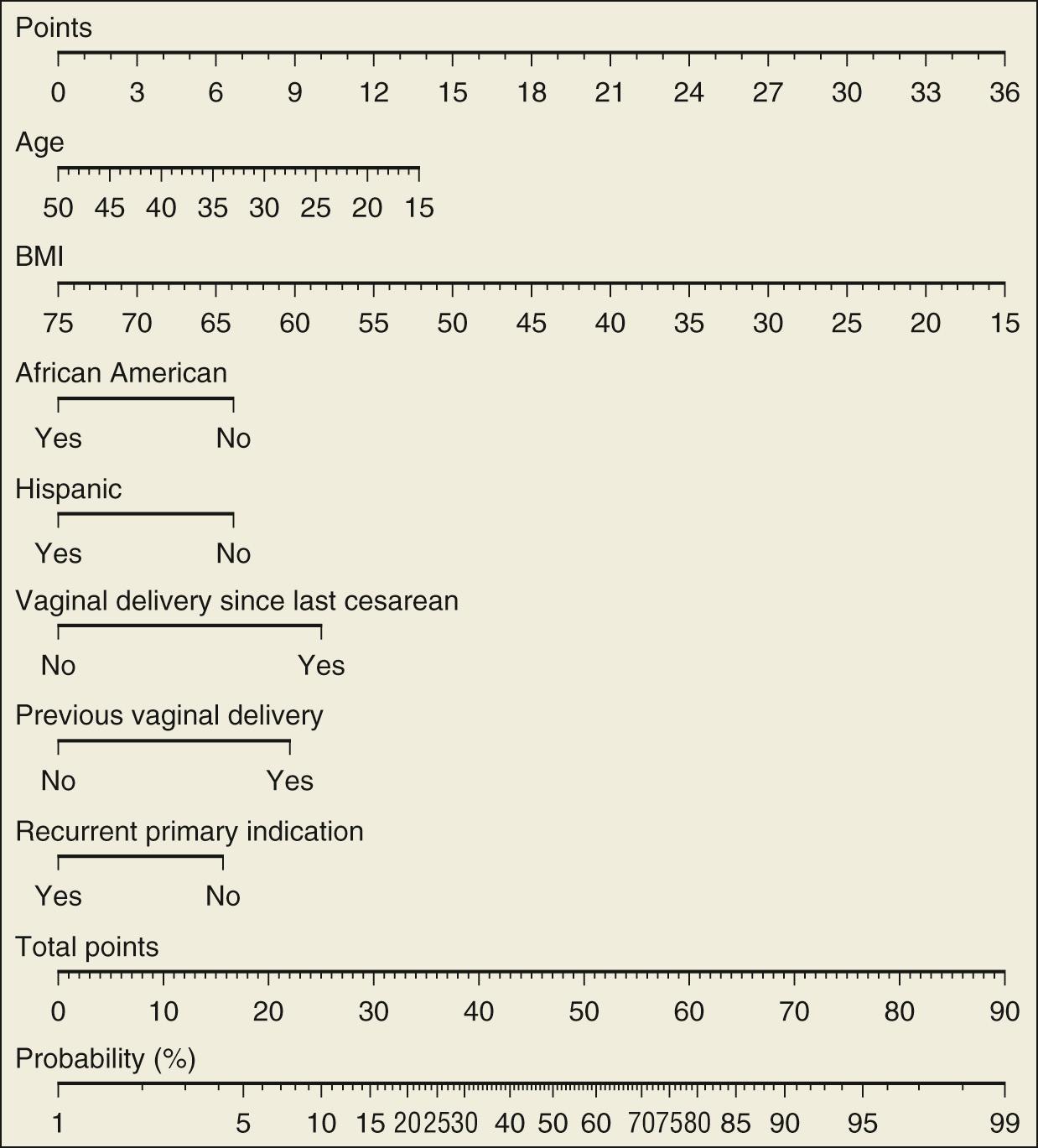
More recently, the PROPECT Study (2022), a multicenter randomized controlled trial funded by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), demonstrated that a standardized labor support protocol—including continuous epidural analgesia, delayed pushing in nulliparous women, and oxytocin protocols—reduced primary C-section rates by 18% without increasing adverse outcomes. The study enrolled 4,600 nulliparous women across 12 U.S. Hospitals and was published in JAMA.
“We have the tools to safely reduce primary C-section rates through systematic labor management. What’s needed is consistent implementation across diverse healthcare settings, not just academic medical centers.”
— Dr. Alison Gemmill, PhD, MPH, Assistant Professor, Department of Population, Family and Reproductive Health, Johns Hopkins Bloomberg School of Public Health
Funding, Conflicts of Interest, and Policy Implications
Research driving obstetric guideline updates is primarily funded by public institutions such as the NIH, CDC, and AHRQ, minimizing industry bias. However, implementation gaps persist due to fragmented reimbursement models: fee-for-service structures may inadvertently incentivize surgical delivery over prolonged labor management, whereas bundled payments and global maternity care models—like those used in the UK’s NHS—align financial incentives with physiologic birth and reduced intervention rates.
In 2025, the Centers for Medicare & Medicaid Services (CMS) introduced a maternal health bonus payment for hospitals that meet benchmark C-section rates and severe morbidity reduction targets under the Birthing-Friendly Hospital designation. Early adopters report a 12% average decline in low-risk first-time C-section rates within the first year, according to a CMS interim evaluation.
Contraindications & When to Consult a Doctor
While C-section is essential in many clinical scenarios, it should be avoided when risks outweigh benefits. Absolute indications include placenta previa, transverse lie, and certain fetal anomalies incompatible with vaginal delivery. Relative indications—such as suspected macrosomia, prior C-section, or maternal request—require individualized counseling.
Patients should consult their obstetrician or midwife if they experience: persistent abdominal pain, vaginal bleeding, decreased fetal movement, or signs of preterm labor. Those with a prior C-section considering VBAC should be evaluated for uterine scar integrity and counseled on the 0.5–1% risk of uterine rupture during labor.
Red flags requiring immediate emergency care include sudden severe hypotension, tachycardia, or abdominal distension postpartum, which may indicate hemorrhage or uterine rupture.
Takeaway: Toward Safer, More Equitable Birth Outcomes
The persistence of high C-section rates in the U.S. Reflects not just clinical complexity but systemic opportunities for improvement. By aligning financial incentives with physiologic birth, expanding access to doula and midwifery care, and standardizing labor management protocols grounded in robust clinical evidence, healthcare systems can reduce unnecessary surgery while preserving access to life-saving intervention when needed. The goal is not to eliminate C-section—a vital tool in modern obstetrics—but to ensure it is used judiciously, equitably, and always in the service of maternal and neonatal well-being.
References
- Martin JA, et al. Births: Final Data for 2023. National Vital Statistics Reports. CDC; 2024.
- American College of Obstetricians and Gynecologists. Practice Bulletin No. 205: Vaginal Birth After Cesarean Delivery. Obstet Gynecol. 2019.
- Grobman WA, et al. Labor Induction versus Expectant Management in Low-Risk Nulliparous Women. NEJM. 2018;379:513-523.
- Reddy UM, et al. Impact of Continuous Labor Support on Cesarean Delivery Rates. JAMA. 2022;328(10):945-954.
- World Health Organization. WHO Statement on Cesarean Section Rates. 2015.
