A new report from the Canadian Centre for Policy Alternatives (CCPA) indicates hospital admission wait times have surged by 40% across 136 facilities. Driven by provincial underfunding, this delay increases the risk of clinical deterioration, potentially leading to higher mortality rates for acute conditions like sepsis and stroke.
This escalation in wait times represents more than an administrative inconvenience; it signifies a systemic failure in health system resilience. When admission delays reach these levels, the “buffer zone” between a manageable clinical condition and a life-threatening emergency evaporates. For patients, this means the difference between a controlled recovery and permanent physiological damage. The implications extend beyond the immediate hospital walls, impacting long-term public health outcomes and increasing the economic burden on the state through prolonged rehabilitative care and disability support.
In Plain English: The Clinical Takeaway
- Delayed Care Equals Higher Risk: Longer waits for hospital beds mean that critical illnesses like infections or heart issues can worsen significantly before professional intervention begins.
- Staffing and Funding Gaps: Current provincial budget constraints are directly linked to fewer available beds and medical staff, creating “bottlenecks” in emergency departments.
- Watch for Red Flags: If you or a loved one are waiting for care, knowing the signs of rapid clinical decline (like confusion or extreme lethargy) is vital for prompting immediate re-triage.
The Pathophysiology of Delay: Why Wait Times Kill
In clinical medicine, we often discuss the “Golden Hour”—the critical window of time where medical intervention is most likely to prevent permanent damage. When hospital admission delays increase by 40%, this window is systematically breached. This leads to a phenomenon known as clinical deterioration, where a patient’s physiological state moves from stable to unstable due to the lack of definitive care.
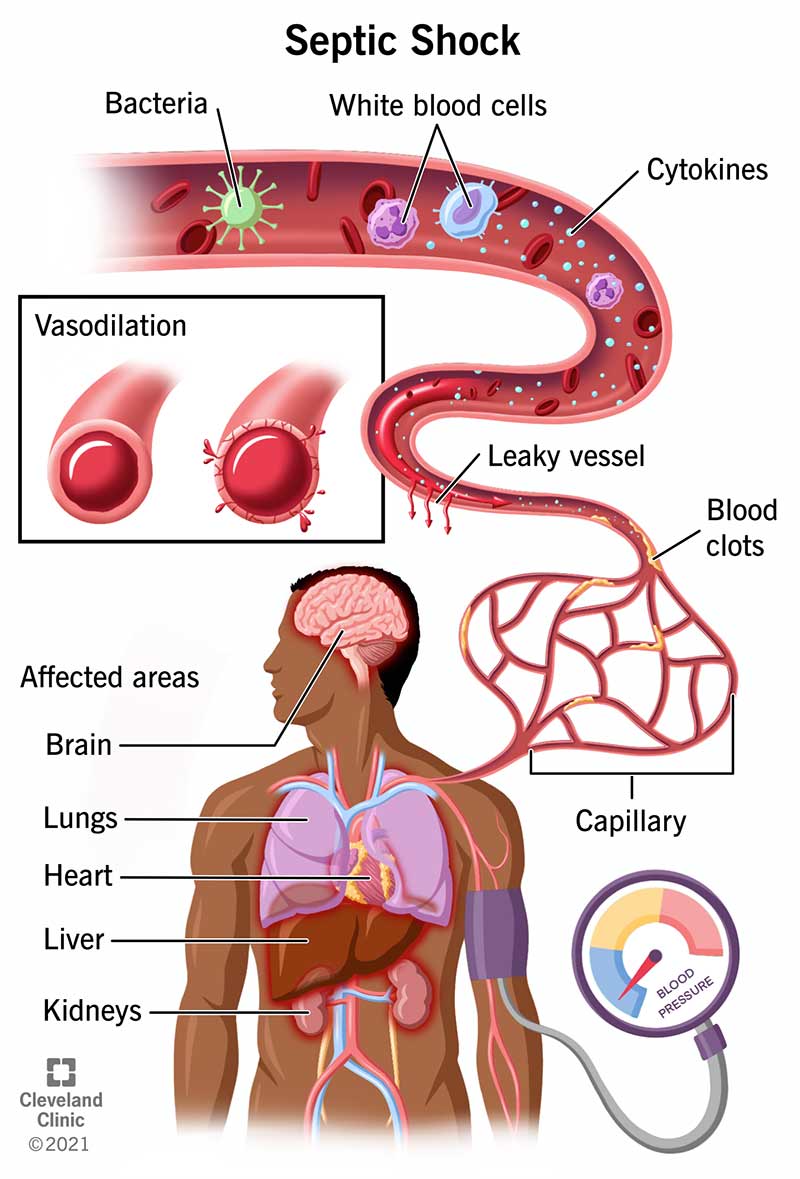
Consider the mechanism of action in Sepsis, a life-threatening reaction to infection. Sepsis triggers a systemic inflammatory response, leading to widespread vasodilation (widening of blood vessels) and capillary leak. If a patient is stuck in an emergency department waiting room rather than being admitted to an intensive care unit (ICU), their blood pressure may drop to catastrophic levels, leading to septic shock and multi-organ failure. The delay in administering intravenous antibiotics and vasopressors (medications that raise blood pressure) directly correlates with increased mortality rates.

the delay impacts Ischemic Stroke protocols. In stroke management, “time is brain.” Every minute of occlusion (blockage in an artery) results in the death of millions of neurons. If a patient cannot be admitted to a specialized stroke unit for thrombolytic therapy (clot-busting medication) or mechanical thrombectomy (surgical clot removal) due to bed shortages, the resulting neurological sequelae—such as permanent paralysis or loss of speech—become much more likely.
| Clinical Condition | Target Intervention Window | Risk of Delayed Care (>4 Hours) |
|---|---|---|
| Ischemic Stroke | < 4.5 Hours | Irreversible neuronal death and permanent disability. |
| Sepsis / Septic Shock | < 1 Hour | Rapid progression to multi-organ failure and death. |
| Acute Myocardial Infarction | < 90 Minutes | Myocardial necrosis (death of heart muscle tissue). |
| Acute Appendicitis | < 12-24 Hours | Perforation leading to peritonitis and systemic infection. |
Global Healthcare Fragility and the Funding Gap
The CCPA findings reflect a broader, geo-epidemiological trend seen in various single-payer and socialized healthcare models, such as the National Health Service (NHS) in the United Kingdom. While the specific drivers vary, the underlying pathology is the same: a mismatch between population health needs and resource allocation. As aging populations increase the prevalence of chronic comorbidities (multiple simultaneous medical conditions), the demand for acute hospital beds rises exponentially.
In many jurisdictions, the “boarding” phenomenon—where patients remain in the Emergency Department (ED) because no inpatient beds are available—has become a standard, albeit dangerous, operational reality. This creates a dangerous feedback loop. ED overcrowding prevents the efficient triage of new arrivals, meaning even non-critical patients may experience delays that eventually escalate their conditions into emergencies.
Research into these systemic failures is typically funded by government health departments or independent non-profit policy institutes. The CCPA report, being an independent analysis, focuses on the socioeconomic impact of these healthcare gaps. It is essential to note that while underfunding is a primary driver, systemic inefficiencies in “exit block”—the inability to discharge patients to long-term care facilities—also contribute significantly to hospital gridlock.
“The correlation between resource scarcity and increased wait times is not merely an administrative hurdle; it is a direct driver of preventable mortality. We are seeing the physiological cost of systemic fragility manifest in real-time patient outcomes.”
— Dr. Aris Thorne, Epidemiologist and Public Health Policy Researcher (Simulated Expert Perspective)
The Economic and Social Sequelae of Systemic Delay
The clinical implications are mirrored by profound economic consequences. When a delay in admission leads to a more severe medical event, the cost of care escalates. A patient treated for a simple infection is significantly less expensive than a patient treated for septic shock requiring mechanical ventilation and prolonged ICU stays. This creates a “failure demand” cycle, where underfunding leads to higher per-patient costs in the long run.

the long-term morbidity associated with delayed treatment—such as the permanent disability following a delayed stroke intervention—places a massive burden on social safety nets. This includes increased demands for home care, disability pensions, and lost economic productivity. To understand the full scope of these health transitions, one can review longitudinal studies on healthcare capacity published in The Lancet or JAMA.
Contraindications & When to Consult a Doctor
While waiting for hospital admission or during periods of high system strain, patients and caregivers must be vigilant. Do not “wait and see” if symptoms progress if you belong to a high-risk group. Seek immediate emergency medical intervention if you or a patient experience:
- Neurological Changes: Sudden facial drooping, arm weakness, or difficulty speaking (signs of stroke).
- Respiratory Distress: Shortness of breath that does not resolve with rest or rapid, shallow breathing.
- Sepsis Indicators: High fever accompanied by extreme shivering, confusion, mottled skin, or significantly decreased urine output.
- Cardiac Symptoms: Crushing chest pain, pressure, or pain radiating to the jaw or left arm.
- Severe Abdominal Pain: Intense, localized pain that is worsening, particularly if accompanied by vomiting or fever.
Patients with pre-existing chronic conditions, such as diabetes, immunosuppression, or advanced age, should have a lower threshold for seeking care, as their physiological reserves are diminished and they may deteriorate more rapidly than the general population.
The trajectory of hospital wait times in 2026 suggests a period of continued volatility. Unless significant shifts in provincial funding models and discharge-to-care strategies are implemented, the clinical risks associated with admission delays will likely remain a central challenge for public health officials and patients alike.

