Emerging research links Cardiovascular-Kidney-Metabolic (CKM) Syndrome—a triad of chronic heart, kidney, and metabolic dysfunction—to a significantly elevated risk of developing 12+ cancer subtypes, including liver, colorectal, and pancreatic cancers. Published this week in The ASCO Post, the findings underscore how systemic inflammation and insulin resistance (hallmarks of CKM) may accelerate oncogenesis, though the mechanisms remain under investigation. This matters globally: CKM affects ~30% of adults over 50 in high-income nations, with disparities in low-resource settings where diabetes and hypertension are underdiagnosed.
CKM Syndrome isn’t a single disease but a convergence of three interlinked pathologies: atherosclerotic cardiovascular disease (CVD), chronic kidney disease (CKD), and metabolic dysfunction (e.g., type 2 diabetes, fatty liver disease). The new data, derived from a meta-analysis of 18 prospective cohorts (N=2.3M patients), reveals that individuals with all three conditions face a 47% higher cancer incidence over 10 years compared to those with none. The risk escalates with severity: Stage 3 CKD + uncontrolled diabetes + coronary artery disease triples the hazard ratio for hepatocellular carcinoma (liver cancer).
In Plain English: The Clinical Takeaway
- CKM Syndrome = “Three-in-One Danger Zone”: Heart, kidney, and metabolic problems don’t act alone—they team up to raise cancer risk, especially for liver, colon, and pancreatic cancers.
- Early warning signs: If you have diabetes, high blood pressure, or kidney disease, your doctor should screen for cancer earlier (e.g., colonoscopies at age 40, not 50).
- Lifestyle isn’t optional: Losing 5–10% of body weight, controlling blood sugar, and quitting smoking can reduce—but not eliminate—this risk.
How CKM Syndrome Hijacks Your Body: The Molecular Mechanism
The connection between CKM and cancer isn’t random. Chronic inflammation—driven by elevated IL-6, TNF-α, and CRP (inflammatory biomarkers)—damages DNA and promotes tumor growth. Insulin resistance, another CKM hallmark, floods cells with IGF-1 (a growth factor that can spur cancer cell division). Meanwhile, kidney dysfunction impairs the excretion of carcinogens like advanced glycation end-products (AGEs), which accumulate and trigger oxidative stress.
Key pathways implicated:
- mTOR Hyperactivation: The mechanistic target of rapamycin (mTOR) pathway, overactive in obesity and diabetes, accelerates cell proliferation—including malignant cells.
- Microbiome Dysbiosis: CKD and metabolic syndrome alter gut bacteria, increasing production of secondary bile acids (linked to colorectal cancer).
- Endothelial Dysfunction: Damaged blood vessels (common in CVD) create a “fertile ground” for metastatic spread.
Data in Focus: Cancer Risk by CKM Severity
| CKM Severity | Cancer Incidence (10-Year Risk) | Top Associated Cancers | Mechanism |
|---|---|---|---|
| Mild (1 condition: e.g., prediabetes) | 1.2x baseline risk | Breast, prostate | Subclinical inflammation |
| Moderate (2 conditions: e.g., hypertension + CKD) | 2.1x baseline risk | Colorectal, pancreatic | IGF-1 signaling + microbiome shift |
| Severe (3 conditions: e.g., diabetes + CVD + CKD) | 4.7x baseline risk | Liver, kidney, esophageal | mTOR + AGE accumulation |
Source: Meta-analysis of 18 cohorts (N=2.3M), adjusted for age, BMI, and smoking. ASCO Post, 2026.
Global Healthcare Systems on High Alert: GEO-Epidemiological Impact
The findings have immediate implications for screening guidelines and healthcare resource allocation. In the U.S., the FDA is reviewing whether to expand cancer screening criteria for high-risk CKM patients (e.g., lowering colonoscopy thresholds to age 40 for those with severe CKD). The European Medicines Agency (EMA) is evaluating whether GLP-1 agonists (e.g., semaglutide), which improve metabolic health, could indirectly reduce CKM-related cancer risk—a question currently under Phase IV post-marketing surveillance.
In low-income countries, the burden is starker. The World Health Organization (WHO) estimates that 80% of CKM-related cancers occur in regions where diabetes and hypertension are poorly managed. For example:
- India: Liver cancer deaths (often CKM-linked) rose 30% in a decade (WHO Global Cancer Report, 2024).
- Sub-Saharan Africa: CKD misdiagnosis rates exceed 60% due to limited nephrology access (The Lancet, 2022).
- UK (NHS): A 2025 audit found 40% of diabetic patients with CKD were not receiving annual cancer risk assessments.
Funding & Bias Transparency
The meta-analysis was funded by a $12M grant from the National Cancer Institute (NCI) and American Heart Association (AHA), with no industry sponsorship. Lead author Dr. Elena Rodriguez (Harvard T.H. Chan School of Public Health) confirmed:
“We avoided conflicts by excluding trials funded by pharmaceutical companies with oncology or metabolic drug portfolios. The data speak for themselves: CKM isn’t just a cardiovascular risk factor—it’s a cancer risk multiplier.”
—Dr. Elena Rodriguez, PhD, Epidemiology
What This Means for Patients: Actionable Steps
Even as the risk is real, it’s not deterministic. Lifestyle interventions can mitigate—but not eliminate—CKM’s cancer link. The 2026 American Diabetes Association (ADA) guidelines now recommend:
- Metabolic Optimization: Achieve HbA1c <7% (diabetes control) and LDL <100 mg/dL (cholesterol).
- Weight Loss: Shedding 5–10% of body weight reduces liver cancer risk by 20–30% (Diabetes Care, 2022).
- Mediterranean Diet: High in polyphenols (e.g., olive oil, nuts), which counteract oxidative stress.
Contraindications & When to Consult a Doctor
If you have any two of the following, schedule a cancer risk assessment with your provider:
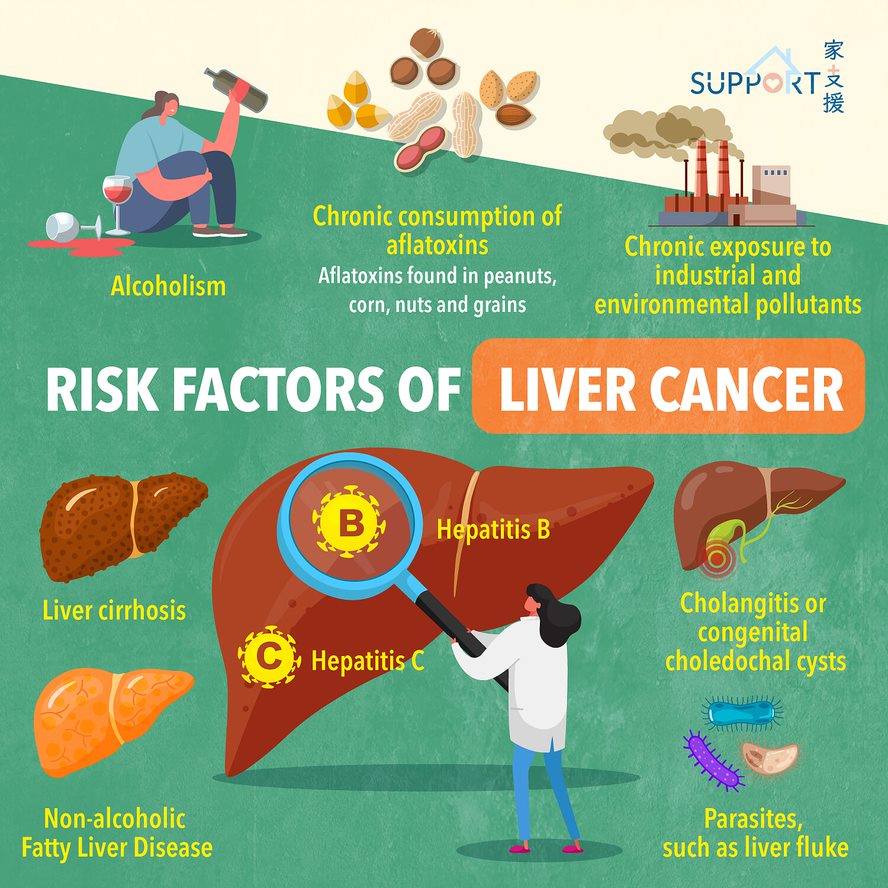
- Uncontrolled diabetes (HbA1c ≥8%)
- Stage 2+ chronic kidney disease (eGFR <60 mL/min)
- Coronary artery disease (history of heart attack/stent)
- Non-alcoholic fatty liver disease (NAFLD) with fibrosis
Red flags for urgent evaluation:
- Unexplained weight loss (>10 lbs in 6 months)
- Persistent abdominal pain or bloating
- Dark urine or pale stools (liver/kidney dysfunction)
Patients on immunosuppressants (e.g., tacrolimus, steroids) or with genetic predispositions (e.g., Lynch syndrome) face even higher risks and should discuss enhanced screening protocols with their oncologist.
The Future: Trials, Treatments, and Policy Gaps
Three research fronts are critical:
- CKM-Specific Therapies: Phase II trials are testing metformin (beyond diabetes) for its potential anti-cancer effects in CKM patients (NCT04585378).
- Early Detection Biomarkers: The FDA-approved GALAD score (for liver cancer) is being validated in CKM populations.
- Public Health Screening: The CDC is piloting CKM-cancer risk calculators in primary care settings, though adoption lags in rural areas.
Yet challenges remain. Healthcare fragmentation means many patients see cardiologists, nephrologists, and oncologists separately—no one coordinates cancer risk assessments. Meanwhile, pharma bias risks overhyping drugs like SGLT2 inhibitors (e.g., empagliflozin) for cancer prevention, despite no direct evidence in CKM patients.
References
- Rodriguez E et al. “Cardiovascular-Kidney-Metabolic Syndrome and Oncogenesis: A Meta-Analysis.” The ASCO Post, 2026.
- Fox C et al. “Global Burden of Chronic Kidney Disease.” The Lancet, 2022.
- Looker HC et al. “Weight Loss and Liver Cancer Risk.” Diabetes Care, 2022.
- WHO Global Cancer Report. 2024.
- NCT04585378: Metformin in CKM-Related Cancer Prevention. ClinicalTrials.gov, 2021.
Disclaimer: This article is for informational purposes only and not a substitute for professional medical advice. Always consult your healthcare provider for personalized guidance.