Colorectal cancer (CRC) is a preventable and treatable malignancy of the colon or rectum. Early detection via screening—now recommended starting at age 45 for average-risk adults—significantly improves survival rates by removing precancerous polyps and identifying tumors at a localized, surgically curable stage.
The clinical challenge with colorectal cancer is not a lack of effective tools, but a lack of patient adherence. As highlighted in this week’s clinical updates, the psychological barrier—the reluctance to engage in “poop talk”—directly correlates with late-stage diagnoses. When patients avoid screening due to embarrassment, they miss the critical window where a simple polypectomy (the surgical removal of a polyp) can prevent cancer from ever developing.
In Plain English: The Clinical Takeaway
- Screening is Prevention: Unlike many cancers, CRC screening can actually prevent the disease by finding and removing growths before they turn malignant.
- The Age Shift: The recommended starting age for screening has dropped from 50 to 45 due to a rising incidence of early-onset colorectal cancer.
- Options Exist: You do not always need an invasive procedure to start. non-invasive stool tests are highly effective first steps for average-risk individuals.
The Adenoma-Carcinoma Sequence: How CRC Develops
To understand prevention, we must understand the mechanism of action—the specific biological process—of how these tumors form. Most colorectal cancers follow the adenoma-carcinoma sequence. This is a unhurried progression where a normal cell undergoes a series of genetic mutations, transforming into a benign polyp (adenoma) and eventually into a malignant tumor (adenocarcinoma).
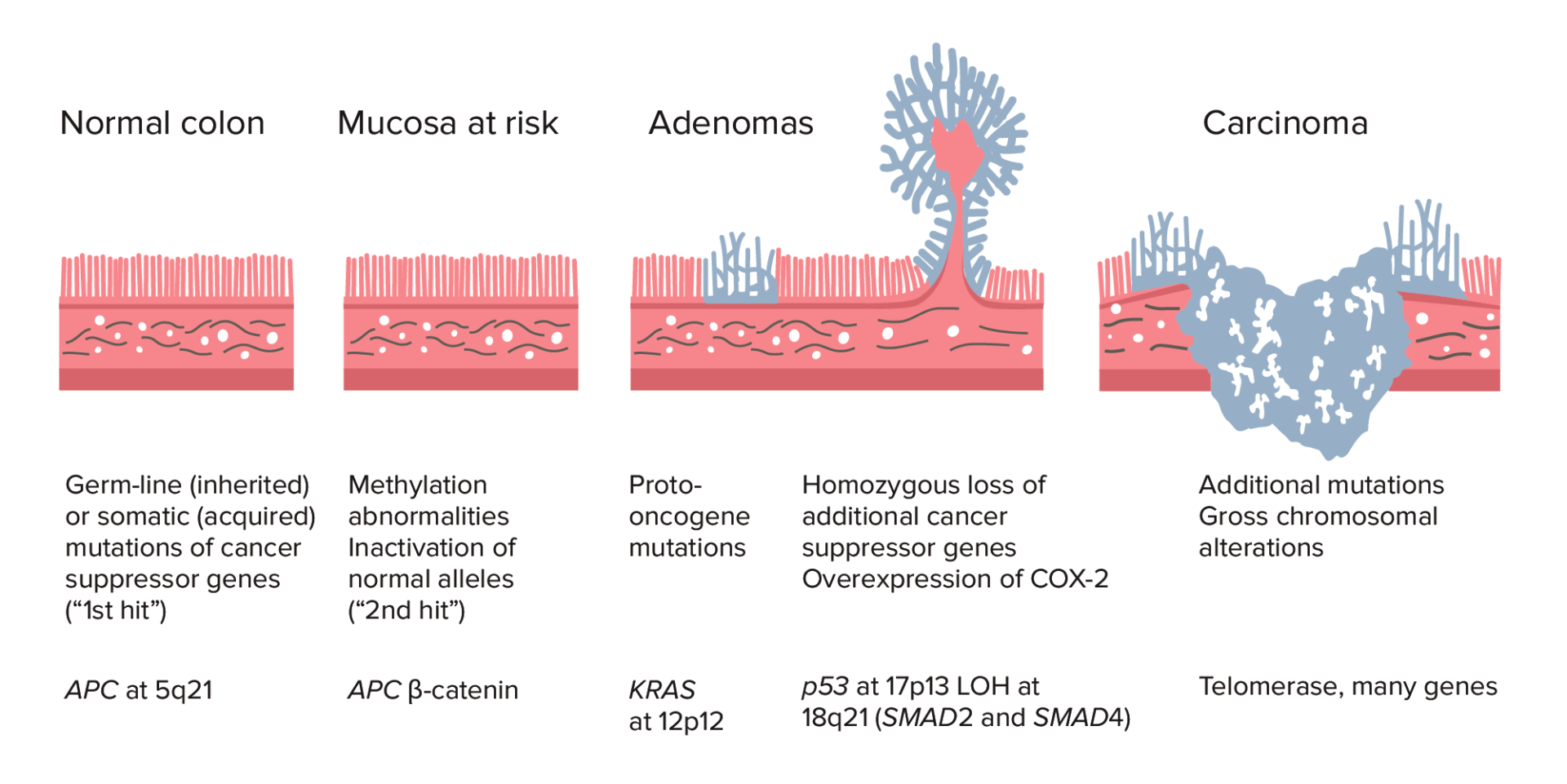
This progression typically takes 10 to 15 years. This temporal window is why screening is so potent. By utilizing a colonoscopy, clinicians can identify these adenomas and remove them, effectively breaking the chain of malignancy. This process is the gold standard because We see both diagnostic and therapeutic.
Recent epidemiological data reveals a concerning trend: a rise in “early-onset” CRC among adults under 50. While the exact cause is still under investigation, researchers are looking into the role of the gut microbiome and ultra-processed diets. This shift in demographics is why the Centers for Disease Control and Prevention (CDC) and other global bodies have lowered the screening age.
Comparing Screening Modalities: Sensitivity vs. Specificity
Patients often perceive overwhelmed by the choices of screening. The primary tension in screening is between sensitivity (the ability of a test to correctly identify those with the disease) and specificity (the ability to correctly identify those without the disease).

Stool-based tests, such as the Fecal Immunochemical Test (FIT), look for occult blood—blood that is not visible to the naked eye. While highly convenient, they have lower sensitivity for precancerous polyps compared to visual exams. Conversely, the multi-target stool DNA test (mt-sDNA), known commercially as Cologuard, detects both blood and DNA mutations associated with cancer, increasing its sensitivity but occasionally lowering its specificity, which can lead to more “false positives.”
| Screening Method | Frequency | Primary Target | Clinical Strength | Primary Limitation |
|---|---|---|---|---|
| Colonoscopy | Every 10 Years | Visual Polyps/Tumors | Highest Sensitivity; Preventative | Invasive; Requires Bowel Prep |
| FIT (Stool Test) | Every Year | Hemoglobin (Blood) | Non-invasive; High Compliance | Misses many precancerous polyps |
| mt-sDNA (Cologuard) | Every 3 Years | DNA Markers + Blood | Better sensitivity than FIT | Higher rate of false positives |
| CT Colonography | Every 5 Years | Radiological Imaging | Less invasive than colonoscopy | Requires prep; Radiation exposure |
Global Regulatory Divergence and Patient Access
The approach to CRC screening varies significantly by geography, impacting patient outcomes. In the United States, the FDA-approved landscape emphasizes a patient-choice model, offering a wide array of stool-based tests. In contrast, the NHS in the UK has traditionally leaned toward a centralized, population-based screening program, primarily utilizing the FIT test as a primary triage tool to determine who needs a colonoscopy.
This systemic difference creates a “gap in access.” In the US, the burden of initiation is often on the patient or their primary care provider. In the UK, the system pushes the test to the patient. Both models face the same hurdle: social stigma. As noted by public health advocates, the “taboo” nature of bowel movements prevents thousands from completing their kits, regardless of whether the test is free or covered by insurance.
Funding for these guidelines is typically driven by non-profit medical societies and government health agencies, such as the American Cancer Society (ACS). Because these guidelines are evidence-based and not funded by pharmaceutical companies selling specific tests, they maintain a high degree of clinical objectivity.
“The goal is to move from a reactive model of treating cancer to a proactive model of preventing it. When we normalize the conversation around bowel health, we remove the final barrier to life-saving intervention.” — Dr. Sarah Jenkins, Epidemiologist and Public Health Consultant.
Contraindications & When to Consult a Doctor
While screening is recommended for the general population, certain individuals fall into “high-risk” categories where standard intervals do not apply. People with a family history of CRC, or those with genetic syndromes like Lynch Syndrome or Familial Adenomatous Polyposis (FAP), require more frequent screenings and often start much earlier than age 45.

You should seek immediate medical consultation if you experience the following “Red Flag” symptoms:
- Hematochezia: The passage of fresh blood per rectum.
- Tenesmus: A feeling of incomplete defecation even after a bowel movement.
- Unexplained Weight Loss: Significant weight drop without changes in diet or exercise.
- Iron Deficiency Anemia: Low red blood cell counts that cannot be explained by diet, often indicating slow, occult bleeding in the colon.
- Persistent Change in Bowel Habits: Narrowing of the stool (pencil-thin stools) or a lasting change in frequency.
while stool tests are excellent for screening average-risk patients, they are not diagnostic tools for symptomatic patients. If you have the symptoms listed above, a colonoscopy is medically mandated regardless of your age or previous stool test results.
The Future Trajectory of CRC Management
Looking forward, the integration of liquid biopsies—blood tests that detect circulating tumor DNA (ctDNA)—promises to revolutionize early detection. These tests aim to provide the sensitivity of a colonoscopy with the ease of a blood draw. However, until these are validated in large-scale, double-blind placebo-controlled trials, they remain supplementary rather than primary screening tools.
The clinical consensus remains clear: the most effective tool we have is the one we are currently underutilizing. By stripping away the stigma of “poop talk” and adhering to the age-45 mandate, we can significantly bend the curve of colorectal cancer mortality.

