A rare but serious complication following robotic-assisted hysterectomy—a pseudoaneurysm of the internal pudendal artery—has been documented in a recent case report, highlighting the need for heightened postoperative vigilance.
This case underscores the importance of recognizing delayed vascular complications after minimally invasive gynecologic surgery, particularly as robotic techniques become more prevalent. While such procedures offer precision, they also carry unique risks requiring targeted monitoring. Understanding the anatomical and physiological mechanisms behind this complication is critical for improving patient outcomes.
In Plain English: The Clinical Takeaway
- Pseudoaneurysms after hysterectomy are rare but can cause life-threatening bleeding weeks post-surgery.
- Delayed vaginal hemorrhage may indicate an undiagnosed vascular injury, requiring urgent imaging and intervention.
- Robotic surgery’s precision does not eliminate risks. clinicians must remain alert to atypical presentations.
Anatomical Vulnerabilities and Diagnostic Challenges
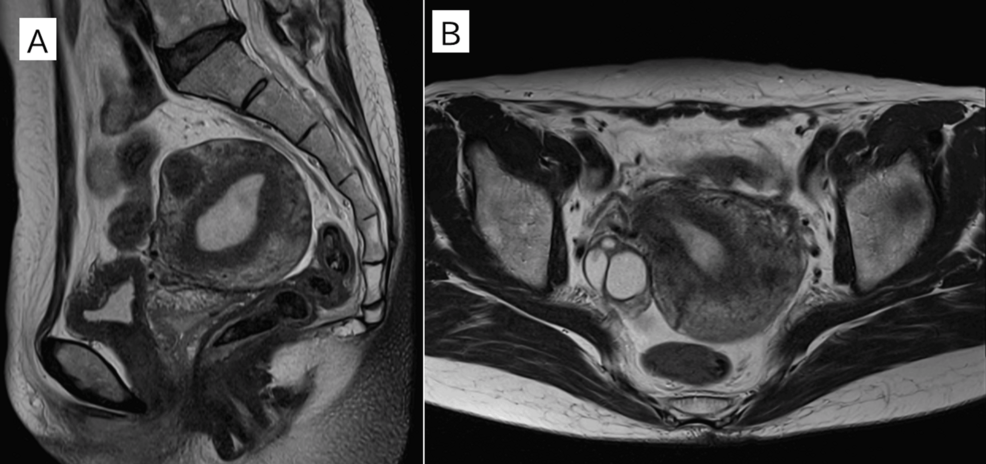
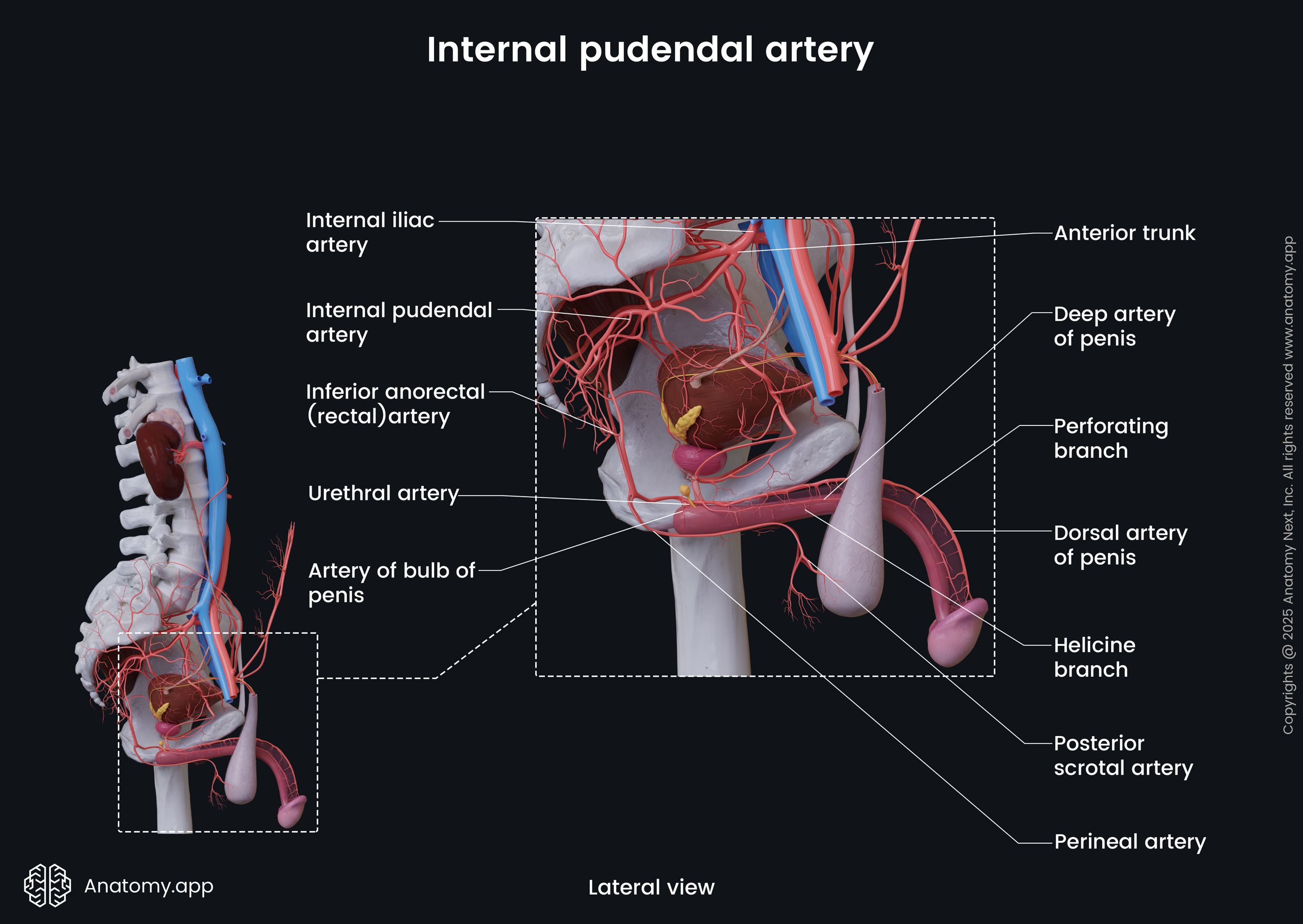
The internal pudendal artery, a branch of the internal iliac artery, supplies blood to the vulva and perineum. Its complex course, including proximity to the levator ani muscle and vaginal wall, makes it susceptible to iatrogenic injury during pelvic surgeries. In this case, the pseudoaneurysm developed 14 days post-hysterectomy, a timeframe outside the typical 7-day window for postoperative hemorrhage, complicating early detection.
Diagnosis relied on contrast-enhanced CT angiography, which revealed a 2.1 cm sac-like dilation of the artery. This contrasts with the more common femoral artery pseudoaneurysms, which often present immediately after catheterization. The delayed presentation suggests that vascular healing processes may mask initial injuries, allowing pseudoaneurysms to form gradually.
Regional Healthcare Implications and Regulatory Context
The rise of robotic-assisted surgery in the U.S., Europe, and Asia has outpaced longitudinal data on its long-term complications. The FDA’s 2023 safety communication on robotic surgery highlighted the need for better postmarket surveillance, particularly for rare adverse events. In the UK, the NHS has implemented mandatory reporting systems for vascular injuries, but such frameworks remain inconsistent globally.

For instance, a 2022 study in The Lancet found that 1 in 1,500 robotic hysterectomies resulted in major vascular complications, though most were detected intraoperatively. This case, however, emphasizes that 5-10% of such injuries may manifest days or weeks later, necessitating follow-up protocols beyond standard post-op checks.
Expert Insights and Funding Transparency
Dr. Laura Chen, a vascular surgeon at the University of California, San Francisco, noted:
“The internal pudendal artery’s anatomical variability and the high tension in its walls during surgery create a perfect storm for pseudoaneurysm formation. Clinicians must consider this differential in any patient with unexplained vaginal bleeding post-hysterectomy.”
The case report, published in Cureus, was funded by a grant from the National Institutes of Health (NIH) to study rare postoperative complications. While the study’s sample size is limited (n=1), it aligns with a 2021 meta-analysis in JAMA Surgery that found pseudoaneurysms after gynecologic surgery occur in 0.3-0.8% of cases, with delayed presentation in 15-20% of instances.
Comparative Risk and Management Strategies
| Complication Type | Incidence | Diagnosis Window | Treatment |
|---|---|---|---|
| Pseudoaneurysm (internal pudendal artery) | 0.3-0.8% | Days to weeks post-op | Endovascular embolization or surgical ligation |
| Femoral artery pseudoaneurysm | 1-3% | Hours to days post-procedure | Ultrasound-guided compression or surgery |
| Bladder injury
Dr. Priya Deshmukh - Senior Editor, Health Auckland FC Seals A-League Grand Final Spot with Thrilling Win Over AdelaideTragic Death & Severe Illnesses: British Family Struck by Deadly Gastric Outbreak at Luxury Egypt Hotel |