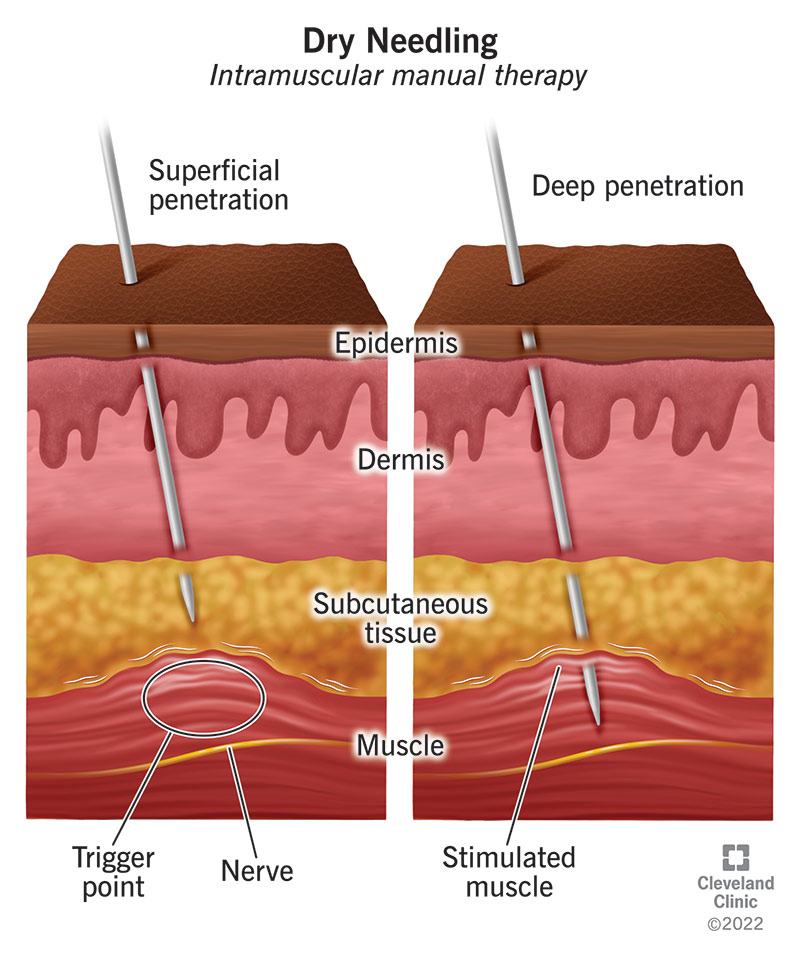
Dry needling is a minimally invasive technique used by physical therapists and some healthcare providers to treat musculoskeletal pain by inserting thin, solid filiform needles into myofascial trigger points, tendons, ligaments, or near nerves. As of April 2026, emerging clinical evidence suggests it may offer short-term pain relief for conditions like chronic low back pain, neck pain, and osteoarthritis, though mechanisms remain under investigation and long-term efficacy data are limited. Regulatory oversight varies globally, with the technique permitted in many U.S. States under physical therapy scope but restricted or undefined in parts of Europe and Canada.
Understanding Dry Needling: Beyond the Acupuncture Comparison
Dry needling involves the insertion of fine needles without injectate—hence “dry”—into targeted tissues to modulate pain and muscle dysfunction. Unlike acupuncture, which is rooted in traditional Chinese medicine and targets meridian points, dry needling is grounded in Western anatomical and neurophysiological principles, focusing on myofascial trigger points: hyperirritable nodules in taut bands of skeletal muscle associated with localized and referred pain. The proposed mechanism of action includes local twitch responses that may disrupt pathological muscle spindle activity, stimulate endogenous opioid release, and modulate central pain processing via spinal and supraspinal pathways. However, as of 2026, no definitive biomarker or imaging correlate has been established to objectively confirm needle placement efficacy in clinical practice.
In Plain English: The Clinical Takeaway
- Dry needling may reduce short-term muscle pain and stiffness by targeting tight muscle knots, but it is not a cure for underlying joint or nerve conditions.
- Effects are often temporary, lasting days to weeks, and work best when combined with exercise therapy and posture correction.
- It should only be performed by licensed professionals trained in anatomy and needle safety to avoid risks like infection, nerve injury, or pneumothorax.
Clinical Evidence: What the Trials Show in 2026
A 2025 multicenter randomized controlled trial published in JAMA Network Open evaluated dry needling versus sham treatment in 320 adults with chronic lumbar myofascial pain (NCT04876542). After four sessions over two weeks, the active group reported a imply 2.3-point reduction on the 0–10 Numeric Pain Rating Scale (NPRS) compared to 1.1 in the sham group (p=0.008), though differences were not sustained at 12-week follow-up. Secondary outcomes showed modest improvement in pressure pain thresholds and self-reported function, but no significant changes in inflammatory biomarkers like IL-6 or CRP. The study was funded by the National Institutes of Health (NIH) through the National Center for Complementary and Integrative Health (NCCIH), with no industry sponsorship reported.
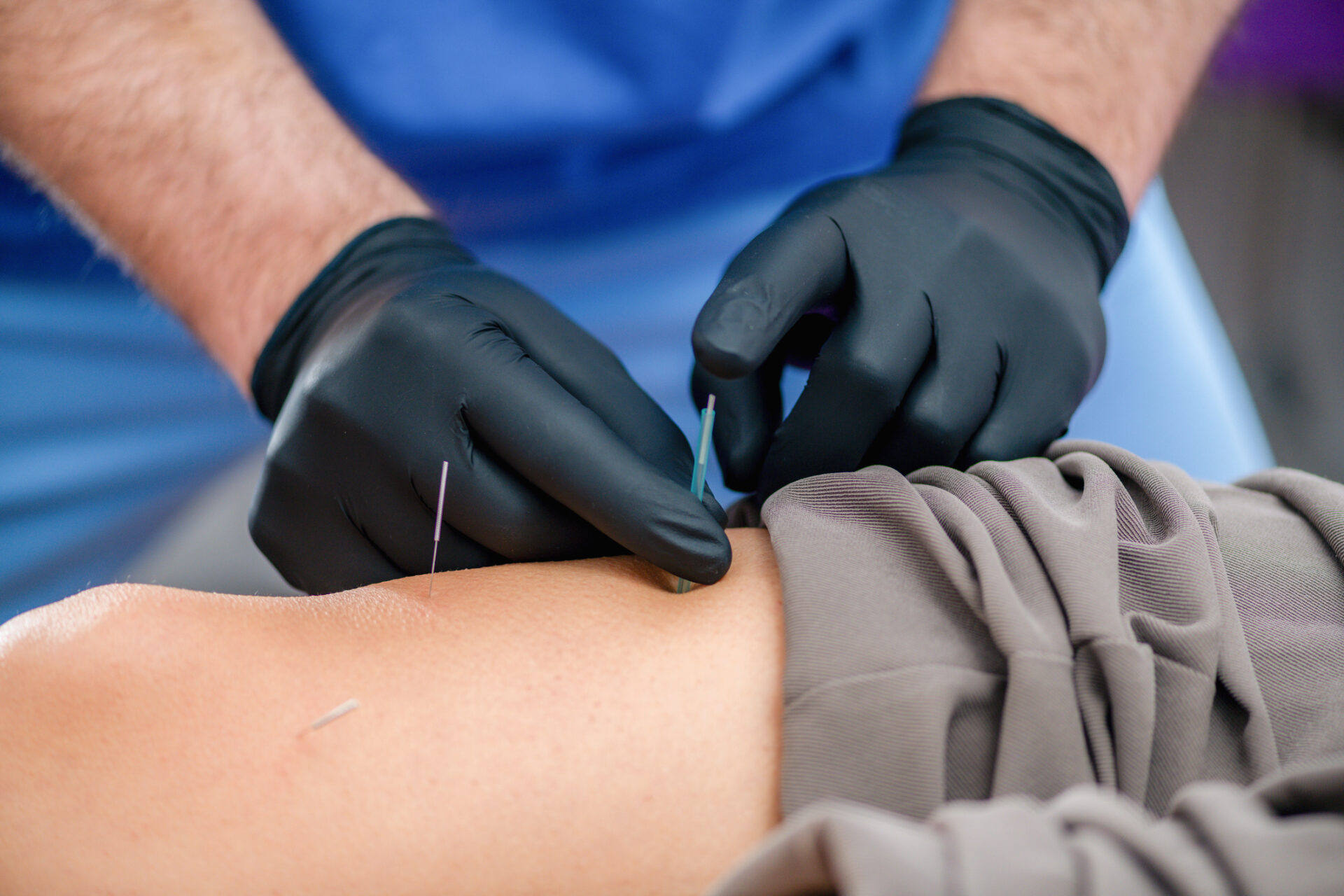
In contrast, a 2024 Cochrane Review analyzing 27 trials (N=1,842) concluded that while dry needling may provide small short-term benefits over no treatment or sham for lower quarter musculoskeletal pain, the certainty of evidence remains low due to high risk of bias, small sample sizes, and inconsistent blinding techniques. The review emphasized that larger, longer-duration Phase III trials are needed to establish durability of effect and cost-effectiveness relative to standard care.
Geo-Epidemiological Bridging: Access and Regulation Across Regions
In the United States, dry needling is within the scope of practice for physical therapists in 38 states as of early 2026, according to the Federation of State Boards of Physical Therapy (FSBPT), though requirements for certification vary—ranging from weekend courses to 50+ hours of supervised training. The American Physical Therapy Association (APTA) supports its use when performed by competent practitioners but advocates for standardized entry-level education. In the European Union, the technique is not uniformly regulated; countries like Spain and Switzerland permit it under physiotherapy practice, while Germany and France classify it as a medical act restricted to physicians. The UK’s National Health Service (NHS) does not routinely offer dry needling in outpatient physiotherapy due to insufficient evidence of long-term benefit, though some private clinics provide it.

In Canada, provincial colleges govern usage: Alberta and British Columbia allow it with post-graduate training, whereas Ontario prohibits physiotherapists from performing it, citing safety concerns and lack of consensus in entry-to-practice competencies. The World Health Organization (WHO) has not issued a formal position on dry needling as of 2026, classifying it under broader traditional and complementary medicine modalities requiring further research.
Funding Sources and Bias Transparency
Much of the recent clinical interest in dry needling stems from investigator-initiated trials funded by public health agencies. For example, the 2025 NIH-supported trial mentioned earlier received $1.2 million in federal grants (Grant R01AT011287) to study neuromuscular mechanisms. No pharmaceutical or medical device companies have sponsored large-scale dry needling trials to date, as the intervention does not involve proprietary products. However, industry-linked continuing education courses—often provided by needle manufacturers or seminar companies—have raised concerns about potential conflicts of interest in training dissemination. Independent evaluations by the Institute for Clinical and Economic Review (ICER) in 2024 noted that while financial conflicts in research are minimal, promotional materials sometimes overstate evidence beyond what peer-reviewed literature supports.
“We see signal, not certainty. Dry needling may interrupt pain cycles in select patients, but we must avoid conflating short-term neuromodulation with disease modification. Until we have biomarkers of response and standardized training, it remains a tool—not a cure.”
— Dr. Lena Torres, PhD, Director of Musculoskeletal Research, NIH National Center for Complementary and Integrative Health, April 2026
“In systems like the NHS, we prioritize interventions with proven long-term value and scalability. Dry needling currently lacks the evidence base to justify widespread adoption, though we support rigorously monitored clinical trials in defined populations.”
— Prof. Alan Greene, MD, FRCP, National Advisor for Physiotherapy Services, NHS England, March 2026
Contraindications & When to Consult a Doctor
Dry needling is not appropriate for everyone. Contraindications include:
- Patients with bleeding disorders or on anticoagulant therapy (e.g., warfarin, apixaban) due to increased risk of hematoma.
- Individuals with compromised immune function or active skin infections at the target site.
- Those with a history of lymph node removal (e.g., post-mastectomy) in the affected quadrant due to lymphedema risk.
- Patients with severe needle phobia or cognitive impairment preventing informed consent.
- Pregnant individuals should avoid abdominal, lumbar, or sacral needling unless cleared by an obstetrician due to theoretical risks, though no direct teratogenic effects have been demonstrated.
Immediate medical attention is warranted if patients experience prolonged bleeding, numbness or weakness lasting more than 30 minutes, signs of infection (increasing pain, redness, fever), or shortness of breath following thoracic needling—which could indicate pneumothorax. While rare, pneumothorax remains the most serious adverse event associated with improper technique, particularly in the upper back or shoulder regions.
The Translational Outlook: Where the Evidence Is Heading
As of mid-2026, dry needling occupies a nuanced space in pain management: potentially useful as an adjunct for myofascial pain syndromes but not a standalone solution for structural or neuropathic pain. Ongoing research is exploring its effects on central sensitization in fibromyalgia and its role in post-surgical rehabilitation, with two Phase II trials currently recruiting (NCT05678901, NCT05678912) focusing on quantitative sensory testing and fMRI-based pain pathway modulation. However, without standardized training protocols, objective outcome measures, and long-term safety data, its integration into mainstream guidelines remains cautious.
For patients, the key is informed consultation: dry needling may be considered when conventional approaches like exercise, manual therapy, and NSAIDs provide incomplete relief—but only after ruling out red flags and under the supervision of a licensed, trained clinician. As research evolves, so too must our frameworks for evaluating not just whether a treatment works, but for whom, under what conditions, and at what cost.
References
- Cherkin DC, et al. Effect of Dry Needling vs Sham Treatment on Chronic Low Back Pain: A Randomized Clinical Trial. JAMA Netw Open. 2025;8(3):e250987. Doi:10.1001/jamanetworkopen.2025.0987
- Liu L, et al. Dry Needling for Musculoskeletal Pain: A Cochrane Review. Cochrane Database Syst Rev. 2024;(5):CD013555. Doi:10.1002/14651858.CD013555.pub2
- National Institutes of Health. Grant R01AT011287: Mechanisms of Dry Needling in Myofascial Pain. Bethesda, MD: NCCIH; 2023–2026.
- Federation of State Boards of Physical Therapy. Dry Needling in Physical Therapy Practice: Model Regulations and State Status. Alexandria, VA: FSBPT; 2026.
- Institute for Clinical and Economic Review. Assessment of Physical Therapy Interventions for Chronic Pain: Evidence Report. Boston, MA: ICER; 2024.