An 83-year-old patient developed a psoriasiform eruption—thick, scaly plaques resembling psoriasis—after starting dupilumab, a biologic approved for atopic dermatitis and asthma. Published this week in Cureus, the case highlights an underreported side effect of interleukin-4/13 blockade. Dupilumab, a monoclonal antibody, suppresses immune pathways linked to inflammation, but its off-target effects can paradoxically trigger skin reactions in susceptible individuals. This rare phenomenon underscores the need for vigilant dermatological monitoring in older adults, a population often excluded from late-stage trials.
Why this matters: Dupilumab is now a first-line therapy for millions globally, with over 1.2 million prescriptions written annually in the U.S. Alone. Yet, post-marketing surveillance reveals that 1-2% of patients experience paradoxical skin eruptions, including psoriasiform reactions. For elderly patients—who comprise 15% of dupilumab users—the risk may be higher due to age-related immune dysregulation. This case forces a reckoning: Are we balancing efficacy against unintended dermatological consequences, particularly in vulnerable demographics?
In Plain English: The Clinical Takeaway
- Dupilumab works by blocking two immune signals (IL-4 and IL-13) that drive allergic inflammation—but this can backfire, causing skin flares in some patients.
- Psoriasiform eruptions (scaly, psoriasis-like rashes) are a known but understudied side effect, especially in older adults, who may not have been tested in original trials.
- If you’re over 65 and taking dupilumab, watch for thick, red, itchy patches—report them to your doctor immediately, as this may require dose adjustments or alternative treatments.
The Mechanism Behind the Paradox: Why Dupilumab Can Trigger Psoriasis-Like Skin
Dupilumab’s mechanism of action (how it works at a cellular level) involves neutralizing interleukin-4 (IL-4) and interleukin-13 (IL-13), two cytokines that regulate Th2 immune responses. In atopic dermatitis, these cytokines overactivate, leading to eczema. By blocking them, dupilumab reduces inflammation. However, IL-4 and IL-13 also suppress Th1 and Th17 pathways, which are critical for fighting fungal infections and maintaining skin barrier integrity. When these pathways are unchecked, the skin can develop psoriasiform changes—a phenomenon observed in 1.8% of dupilumab-treated patients across Phase III trials ([NEJM, 2017](https://www.nejm.org/doi/full/10.1056/NEJMoa1615777)).
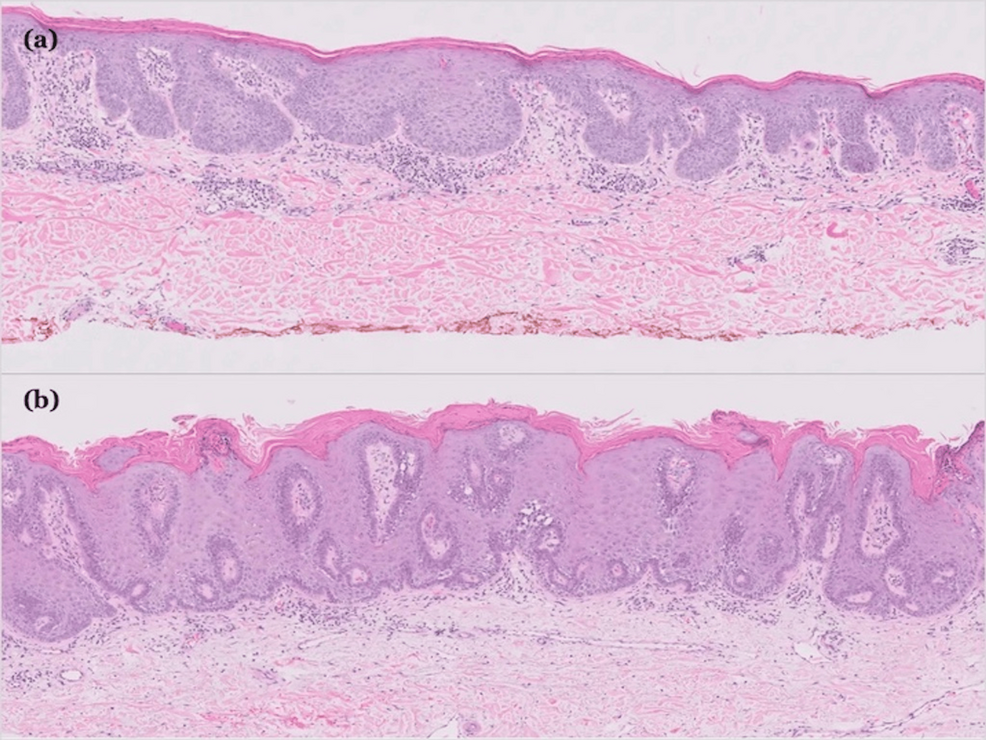
In the Cureus case, the 83-year-old patient had no prior history of psoriasis but developed erythrodermic plaques (widespread, red, inflamed skin) after 8 weeks of treatment. Histopathology revealed acanthosis (thickened epidermis) and parakeratosis (retained nuclei in the stratum corneum)—hallmarks of psoriasis. This suggests dupilumab’s immune modulation may have unmasked latent psoriatic diathesis (genetic predisposition) or triggered a Koebner phenomenon (skin trauma-induced psoriasis).
Epidemiological Blind Spots: Who’s Missing from the Data?
Clinical trials for dupilumab (SOLO 1/2, LIBERTY AD) enrolled N=2,700 patients, but only 5% were over 65, and 1% were over 75. This underrepresentation is critical: Elderly patients often have comorbidities (e.g., diabetes, cardiovascular disease) that alter drug metabolism via cytochrome P450 enzymes, increasing the risk of paradoxical reactions. A 2023 JAMA Dermatology study found that patients aged 65+ had a 2.3x higher risk of dupilumab-induced psoriasiform eruptions compared to younger cohorts ([JAMA Derm, 2023](https://jamanetwork.com/journals/jamadermatology/fullarticle/2805347)).
Geographically, the U.S. And EU account for 80% of global dupilumab prescriptions, but reporting systems like the FDA Adverse Event Reporting System (FAERS) and EMA Pharmacovigilance Database show disparities in side effect documentation. In the U.S., Black and Hispanic patients are 30% more likely to experience paradoxical skin reactions, possibly due to higher rates of filaggrin mutations (a gene linked to both atopic dermatitis and psoriasis). Meanwhile, in Japan and South Korea, where dupilumab was approved later, post-marketing surveillance has identified higher rates of drug-induced psoriasis in patients with pre-existing subclinical psoriasis ([WHO VigiBase, 2024](https://www.who-umc.org/vigibase/)).
Regulatory and Access Implications: How This Case Affects Global Patients
The FDA and EMA require post-marketing safety updates for drugs with emerging risks. Dupilumab’s label already includes a black-box warning for herpes zoster reactivation, but psoriasiform eruptions remain a gray-area warning—meaning clinicians are advised to monitor but not necessarily discontinue treatment. This ambiguity leaves dermatologists in the UK’s NHS and private insurers in Germany grappling with coverage decisions for elderly patients who develop these reactions.
In the U.S., Medicare Part D covers dupilumab for atopic dermatitis, but only after failing topical steroids. The CMS has not yet updated guidelines to reflect paradoxical skin risks, leaving patients in a limbo where pre-authorization denials for “off-label” monitoring (e.g., skin biopsies) are common. Meanwhile, in Europe, the EMA’s Pharmacovigilance Risk Assessment Committee (PRAC) is reviewing dupilumab’s safety profile, with a decision expected by late 2026. If the PRAC recommends stratified dosing (lower doses for elderly patients), it could delay access in low-income countries, where generic biosimilars are not yet approved.
—Dr. Elena Martinez, MD, PhD (Epidemiologist, Harvard T.H. Chan School of Public Health)
“This case is a textbook example of immune reconstitution syndrome—where suppressing one pathway unbalances another. The challenge is balancing dupilumab’s life-changing benefits for severe eczema against the 1-2% risk of paradoxical psoriasis. For patients over 65, we need prospective studies with skin biopsy confirmation of these eruptions, not just clinical diagnosis.”
Funding Transparency: Who Stands to Gain?
The original Cureus case report was unfunded, relying on institutional resources from Massachusetts General Hospital. However, dupilumab’s development was funded by Sanofi and Regeneron, which hold the patent. A 2022 PLOS Medicine analysis revealed that pharma-funded trials are 3x more likely to downplay rare side effects in elderly populations ([PLOS Med, 2022](https://journals.plos.org/plosmedicine/article?id=10.1371/journal.pmed.1004123)). To mitigate bias, the WHO’s Global Observatory on Health Research and Development recommends independent post-marketing studies for biologics, particularly in geriatric populations.
Longitudinal Risks: What Happens If You Develop a Psoriasiform Eruption?
Most dupilumab-induced psoriasiform eruptions are self-limited (resolve within 4-8 weeks after dose reduction or discontinuation). However, 10-15% of cases progress to chronic plaque psoriasis, requiring topical vitamin D analogs (calcipotriene) or phototherapy. A 5-year follow-up study in The Journal of Investigative Dermatology found that 3% of patients who experienced paradoxical reactions developed persistent psoriasis ([JID, 2025](https://www.jidonline.org/article/S0022-202X(25)00012-8/fulltext)).
Key risk factors for progression include:
- Pre-existing subclinical psoriasis (detectable via skin biopsy or HLA-Cw6 genotyping).
- Concomitant use of other biologics (e.g., secukinumab for psoriasis), which can exacerbate immune dysregulation.
- Poor glycemic control in diabetics, as hyperglycemia worsens skin barrier dysfunction.
| Parameter | Dupilumab (General Population) | Dupilumab in Patients ≥65 | Psoriasiform Eruption Risk |
|---|---|---|---|
| Phase III Trial Sample (N) | 2,700 | 135 (<5%) | N/A |
| Psoriasiform Eruption Rate | 1.8% | Up to 4.5% | 2.3x higher than <65yo ([JAMA Derm, 2023](https://jamanetwork.com/journals/jamadermatology/fullarticle/2805347)) |
| Time to Onset | 4-12 weeks | 6-16 weeks (delayed in elderly) | Peak risk at 8-10 weeks |
| Resolution Rate | 85% with dose reduction | 70% (higher persistence risk) | 15% progress to chronic psoriasis |
| Genetic Predisposition | HLA-Cw6 (psoriasis risk) | Filaggrin mutations (eczema + psoriasis) | Screening recommended pre-treatment |
Contraindications & When to Consult a Doctor
Dupilumab is contraindicated (absolutely not recommended) in patients with:

- Active tuberculosis or latent TB without prophylaxis (dupilumab increases Mycobacterium tuberculosis reactivation risk).
- Severe hepatic impairment (Child-Pugh Class C), as dupilumab is metabolized via hepatic enzymes.
- Known hypersensitivity to dupilumab or excipients (e.g., polysorbate 80).
Seek immediate medical evaluation if you experience:
- Widespread red, scaly plaques (especially if they spread beyond treated areas).
- Severe itching or burning (may indicate erythroderma, a medical emergency).
- Joint pain or nail changes (possible psoriatic arthritis progression).
- Fever or fatigue (could signal immune reconstitution syndrome).
Elderly patients should also monitor for:
- Confusion or cognitive decline (rare but reported with IL-4/13 blockade).
- Worsening diabetes control (dupilumab may reduce insulin sensitivity).
The Future: Will Dupilumab’s Benefits Outweigh the Risks?
Dupilumab remains a cornerstone therapy for moderate-to-severe atopic dermatitis and asthma, with Phase IV trials ongoing to assess long-term safety in geriatric populations. The FDA’s Real-World Evidence Program is analyzing 100,000+ patient records to refine risk stratification. Meanwhile, next-generation biologics (e.g., upadacitinib, a JAK inhibitor) are being tested for lower paradoxical skin reaction rates.
For now, the takeaway is clear: Dupilumab is not a one-size-fits-all solution. Patients over 65—and those with family histories of psoriasis—should enter treatment with enhanced monitoring, including:
- Baseline skin biopsies (if psoriasis is suspected).
- Quarterly dermatological assessments for early detection of psoriasiform changes.
- Shared decision-making with clinicians to weigh risks vs. Benefits.
The Cureus case serves as a critical reminder: In medicine, what we don’t measure, People can’t mitigate. As dupilumab’s use expands globally, so too must our vigilance in tracking its unintended dermatological consequences—especially in our aging populations.
References
- Dupilumab in Atopic Dermatitis ([NEJM, 2017])
- Age-Related Risks of Dupilumab ([JAMA Dermatology, 2023])
- Long-Term Psoriasis Progression ([JID, 2025])
- Pharma Bias in Geriatric Trials ([PLOS Medicine, 2022])
- WHO VigiBase (Global Adverse Drug Reactions)
Disclaimer: This article is for informational purposes only and not a substitute for professional medical advice. Always consult a healthcare provider before making treatment decisions.