A recent maritime incident involving an elderly passenger aboard a vessel has highlighted the persistent public health risk of hantaviruses. While the individual remains under observation, the event underscores the importance of vector control in confined spaces and the clinical necessity of early recognition of zoonotic—animal-to-human—pathogens in international travel.
In Plain English: The Clinical Takeaway
- Transmission Reality: Hantaviruses are primarily transmitted via aerosolized excreta (dried urine, feces, or saliva) from infected rodents, not through direct human-to-human contact.
- Clinical Vigilance: Early symptoms often mimic influenza, including fever, myalgia (muscle pain), and fatigue, which can rapidly progress to respiratory distress.
- Preventative Strategy: If traveling or working in environments with potential rodent infestations, avoid disturbing nests and ensure adequate ventilation to prevent the inhalation of viral particles.
The Pathophysiology of Hantavirus Pulmonary Syndrome (HPS)
Hantaviruses, belonging to the family Hantaviridae, operate via a specific mechanism of action that targets the vascular endothelium—the thin membrane that lines the inside of the heart and blood vessels. When an individual inhales aerosolized viral particles, the virus enters the lungs and triggers a massive, systemic inflammatory response.
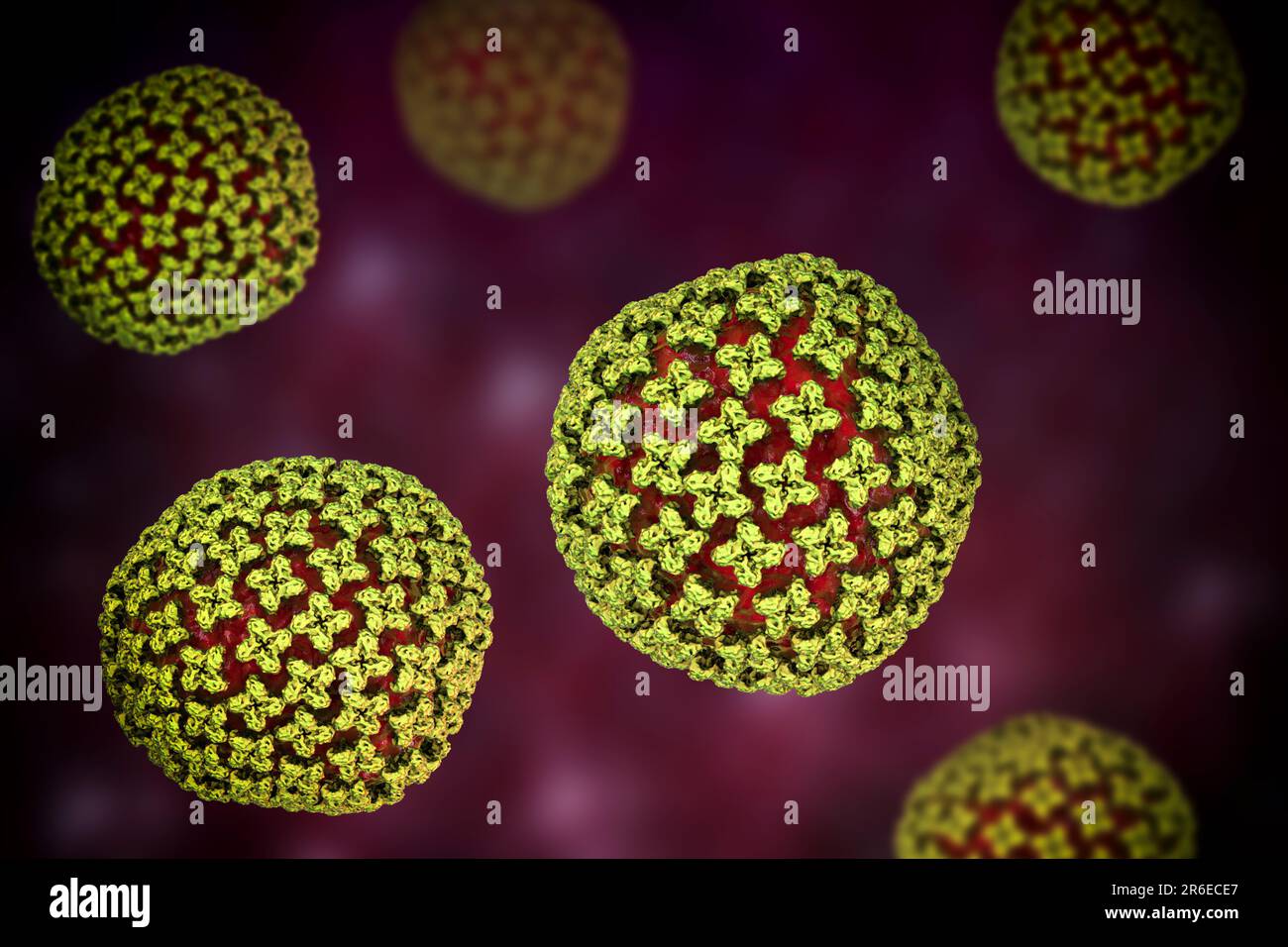
This response leads to increased capillary permeability, essentially causing blood vessels to “leak” fluid into the interstitial spaces of the lungs. This condition, known as Hantavirus Pulmonary Syndrome (HPS), results in non-cardiogenic pulmonary edema—a dangerous accumulation of fluid in the lungs that is not caused by heart failure. Unlike other viral infections, the primary morbidity in HPS is driven by the host’s own immune system attempting to contain the viral replication.
“Hantaviruses remain a critical zoonotic concern because they demonstrate high case-fatality rates, often exceeding 35 percent in untreated populations. The challenge for clinicians is that the prodromal phase—the period before characteristic symptoms appear—is clinically indistinguishable from common viral illnesses, necessitating a high index of suspicion based on exposure history.” — Dr. Elena Rossi, Epidemiologist, Global Infectious Disease Research Initiative.
Geo-Epidemiology and Regulatory Surveillance
The incident aboard the ship serves as a reminder that zoonotic risks are not tethered to landmasses. Maritime vessels, due to their storage capacities and potential for rodent harborage, can become mobile vectors for pathogens. In the European Union, the European Centre for Disease Prevention and Control (ECDC) maintains rigorous surveillance protocols for zoonotic diseases, yet the transient nature of maritime travel complicates contact tracing.
In the United States, the Centers for Disease Control and Prevention (CDC) classifies specific hantavirus strains, such as the Sin Nombre virus, as reportable conditions. Clinicians in both regions are instructed to prioritize patient travel history when presenting with acute, unexplained respiratory failure. Access to supportive care—specifically mechanical ventilation and, in severe cases, extracorporeal membrane oxygenation (ECMO)—is the gold standard for treatment, as there is currently no FDA- or EMA-approved antiviral medication specifically indicated for HPS.
| Clinical Feature | Hantavirus Pulmonary Syndrome (HPS) | Influenza A/B |
|---|---|---|
| Primary Transmission | Aerosolized rodent excreta | Respiratory droplets |
| Target System | Vascular endothelium (capillary leak) | Upper/Lower respiratory epithelium |
| Case Fatality Rate | High (up to 35-40%) | Low (<0.1%) |
| Diagnostic Focus | IgM/IgG ELISA serology | PCR/Rapid Antigen Testing |
Research Transparency and Funding
Epidemiological research into hantavirus transmission is largely supported by governmental public health agencies, including the National Institutes of Health (NIH) and various European public health consortia. It is essential for the public to note that these studies are generally peer-reviewed and devoid of commercial bias, as there is currently no high-profit pharmaceutical vaccine or therapeutic market driving this research. The focus remains strictly on containment, environmental hygiene, and rapid diagnostic intervention.
Contraindications & When to Consult a Doctor
There are no “treatments” for hantavirus in the home setting. If you have been in an area with known rodent activity and develop symptoms, you must seek immediate medical evaluation. Consult a physician if you experience:
- Fever exceeding 38.5°C (101.3°F) accompanied by unexplained, severe muscle aches.
- Rapid onset of dyspnea (shortness of breath) or a non-productive cough.
- Dizziness or hypotension (low blood pressure) following a period of flu-like illness.
Contraindications: Do not attempt to manage respiratory distress at home with over-the-counter suppressants, as these can mask the progression of pulmonary edema. If you suspect exposure, inform healthcare providers of your travel history or contact with rodent-infested environments immediately to facilitate proper diagnostic testing (e.g., serology or RT-PCR).
Future Trajectory of Zoonotic Surveillance
As global trade and travel increase, the intersection of human and wildlife habitats will continue to present risks. The clinical community is shifting toward a “One Health” approach, which recognizes that human health is inextricably linked to animal health and the environment. Future efforts will likely focus on faster, bedside diagnostic assays that can detect viral RNA in real-time, allowing for immediate quarantine and supportive care initiation long before a patient reaches a critical state of respiratory failure.
References
- Centers for Disease Control and Prevention (CDC) – Hantavirus Information
- World Health Organization (WHO) – Zoonotic Disease Fact Sheet
- The Lancet Infectious Diseases – Global Epidemiology of Hantavirus Infections
- European Centre for Disease Prevention and Control (ECDC) – Surveillance and Risk Assessment
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
