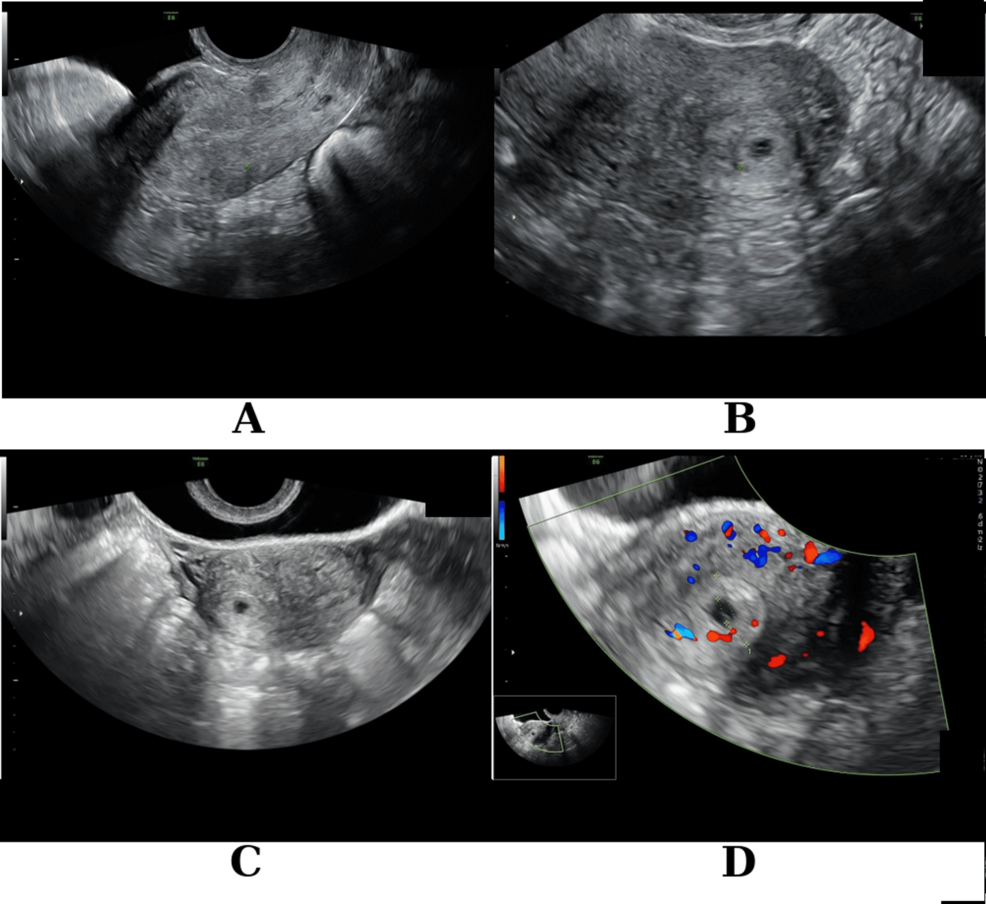
Angular pregnancy is a rare form of ectopic pregnancy where the embryo implants in the lateral angles of the uterus. When medical management via Methotrexate fails, hysteroscopic resection—a minimally invasive surgical removal—offers a critical, uterus-preserving alternative to traditional hysterectomy for patients facing high rupture risks.
For the global medical community, the management of angular pregnancies represents a high-stakes clinical tightrope. While most ectopic pregnancies occur in the fallopian tubes, the angular variety is particularly insidious given that it occurs within the uterine wall, often mimicking a normal intrauterine pregnancy on early ultrasounds. This diagnostic ambiguity can lead to delayed treatment, increasing the risk of uterine rupture and life-threatening hemorrhage.
In Plain English: The Clinical Takeaway
- What It’s: A pregnancy that grows in the “corner” of the uterus rather than the center, making it unstable and dangerous.
- The Treatment Shift: If medication (Methotrexate) doesn’t stop the pregnancy, surgeons can now use a small camera and tools (hysteroscopy) to remove the tissue without a large incision.
- The Goal: To stop the bleeding and remove the pregnancy while saving the uterus so the patient can potentially have children in the future.
The Pharmacological Failure: Why Methotrexate Isn’t Always Enough
The first line of defense for stable ectopic pregnancies is often Methotrexate, a folate antagonist. Its mechanism of action—meaning how the drug works—is to inhibit the enzyme dihydrofolate reductase, effectively starving rapidly dividing trophoblastic cells (the cells that form the placenta) of the nutrients they need to grow.
However, angular pregnancies often exhibit a higher vascularity and a more aggressive implantation into the myometrium (the muscular wall of the uterus). In these cases, the drug may not reach a high enough concentration at the implantation site, or the tissue may be too robust to respond. When serum beta-hCG levels fail to drop by the expected percentage following an injection, the patient is deemed “refractory,” and surgical intervention becomes mandatory to prevent spontaneous rupture.
Hysteroscopic Resection: Precision Over Radical Surgery
Hysteroscopic management involves inserting a thin, lighted tube (the hysteroscope) through the cervix. Unlike a laparotomy, which requires a large abdominal incision, this is an endoscopic approach. The surgeon identifies the angular implantation and uses specialized instruments to carefully excise the gestational sac and the associated placental tissue.
This approach is particularly vital for preserving fertility. Historically, a ruptured angular pregnancy often resulted in an emergency hysterectomy. By utilizing a controlled, hysteroscopic approach, clinicians can remove the ectopic tissue while minimizing trauma to the surrounding uterine muscle. This preserves the structural integrity of the organ, which is a primary goal for patients of reproductive age.
| Management Strategy | Primary Mechanism | Success Rate/Risk | Impact on Fertility |
|---|---|---|---|
| Methotrexate | Chemical inhibition of cell growth | Variable; risk of failure in angular cases | High preservation |
| Hysteroscopic Resection | Physical removal via endoscopy | High efficacy; risk of uterine perforation | Moderate to High preservation |
| Hysterectomy | Total organ removal | 100% curative for current event | Permanent loss of fertility |
Global Healthcare Integration and Access
The adoption of hysteroscopic management varies significantly by region. In the United States, the FDA has cleared various advanced hysteroscopic tools that allow for more precise cauterization, reducing the risk of intraoperative hemorrhage. In the UK, the NHS incorporates these procedures into specialized early pregnancy assessment units (EPAs), though access depends on the availability of surgeons trained in advanced hysteroscopy.
In lower-resource settings, the “information gap” is stark. Many regions still rely on open surgery (laparotomy) due to the high cost of endoscopic equipment. This disparity means that patients in developing healthcare systems face a higher rate of hysterectomies for angular pregnancies compared to those in the West, where organ-sparing techniques are the gold standard.
“The challenge with angular pregnancy is the diagnostic overlap with interstitial pregnancies. The transition from medical to surgical management must be decisive; waiting too long for a drug to work can turn a manageable procedure into a surgical emergency.” — Dr. Elena Rossi, Reproductive Endocrinologist.
Funding, Bias and Evidence-Based Transparency
Much of the data regarding hysteroscopic management of angular pregnancies comes from case series and institutional reports rather than large-scale, double-blind placebo-controlled trials (which are ethically impossible as you cannot give a placebo to a patient with a life-threatening pregnancy). Most of these studies are funded by university hospitals or academic medical centers. While there is no significant pharmaceutical bias—as the procedure is surgical—there is a “publication bias” toward successful outcomes, which may slightly overstate the ease of the procedure.
To ensure data integrity, clinicians rely on the PubMed database and the Lancet to track longitudinal outcomes, such as the rate of uterine rupture in subsequent pregnancies following a hysteroscopic resection.
Contraindications & When to Consult a Doctor
Hysteroscopic management is not suitable for everyone. It is contraindicated in patients with unstable hemodynamics (e.g., severe internal bleeding, shock) where an emergency laparotomy is required to save the patient’s life. It is also avoided in cases where the uterine wall is already too thin to support the instruments without causing a catastrophic tear.

Seek immediate emergency care if you experience:
- Sudden, sharp, or stabbing pelvic or abdominal pain.
- Heavy vaginal bleeding that soaks through a pad in an hour.
- Dizziness, fainting, or a rapid heart rate (signs of hemorrhagic shock).
- Shoulder tip pain, which can indicate blood irritating the diaphragm.
The Future of Ectopic Management
As we move further into 2026, the integration of 3D ultrasound and AI-driven imaging is allowing for earlier differentiation between angular and interstitial pregnancies. In other words “failed” Methotrexate cases may decrease as surgeons intervene earlier with targeted hysteroscopy. The trajectory is clear: moving away from radical organ removal toward precision, uterus-sparing interventions.