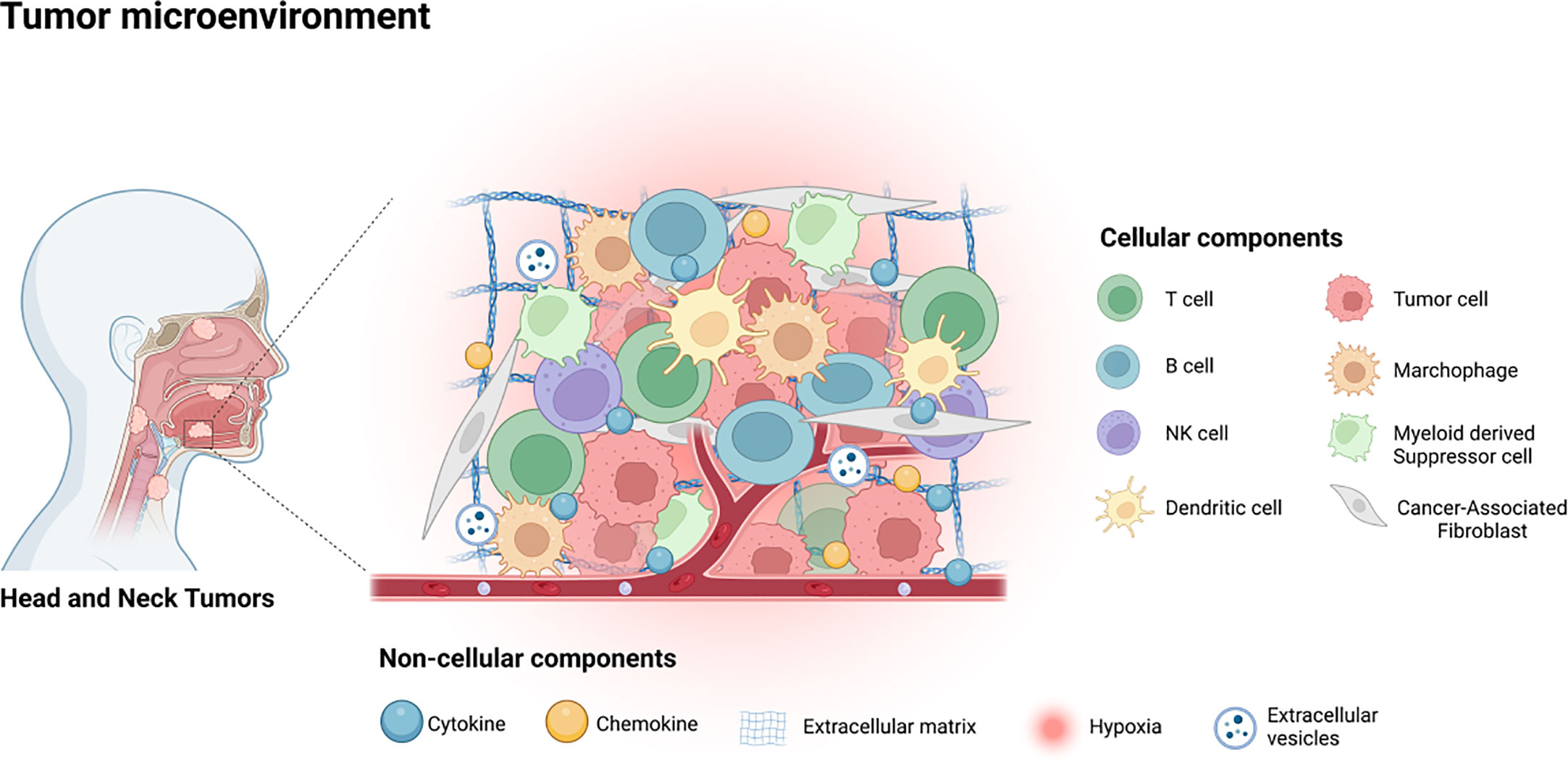
Recent research indicates that chewing gum containing specific antimicrobial compounds may reduce levels of human papillomavirus (HPV) and other bacteria associated with oral cancer in patients with head and neck squamous cell carcinoma (HNSCC), offering a potential low-cost adjunctive strategy to target microbial drivers of tumor progression.
How Antimicrobial Chewing Gum Targets Oral Microbiome in HNSCC
A pilot study published this week in Clinical Cancer Research found that patients with HPV-positive HNSCC who chewed gum containing magnolia bark extract and zinc lactate twice daily for two weeks showed a statistically significant reduction in salivary HPV DNA load and decreased levels of Fusobacterium nucleatum and Porphyromonas gingivalis—bacteria linked to chronic inflammation and carcinogenesis in the oral cavity. The mechanism of action involves disruption of bacterial biofilms and inhibition of viral gene expression, though the gum is not intended as a standalone cancer treatment.
In Plain English: The Clinical Takeaway
- Chewing specialized gum may help lower harmful bacteria and virus levels in the mouth, potentially reducing inflammation tied to oral cancer.
- This approach is being studied as a complementary tool—not a replacement—for standard treatments like surgery, radiation, or immunotherapy.
- Patients should continue regular screenings and consult their oncologist before adding any new regimen to their care plan.
Clinical Trial Design and Epidemiological Context
The double-blind, placebo-controlled trial enrolled 48 patients with Stage III or IV HPV-positive HNSCC from three academic medical centers: MD Anderson Cancer Center in Houston, Memorial Sloan Kettering in New York, and the University of Pittsburgh Medical Center. Participants were randomly assigned to either antimicrobial gum or identically flavored control gum without active ingredients. Salivary biomarkers were measured at baseline, day 7, and day 14. The intervention group demonstrated a 62% mean reduction in HPV DNA copies per mL of saliva (p=0.008) and a 47% decrease in F. Nucleatum levels (p=0.012), while the control group showed no significant change. No serious adverse events were reported; mild transient gum irritation occurred in 12% of the intervention group.
According to the Surveillance, Epidemiology, and Conclude Results (SEER) program, HPV-positive oropharyngeal cancers now account for approximately 70% of all oropharyngeal squamous cell carcinomas in the United States, with incidence rising particularly among men aged 40–60. While HPV vaccination has reduced infection rates in younger cohorts, millions of adults remain at risk due to prior exposure, making secondary prevention strategies increasingly relevant.
Geo-Epidemiological Bridging: Implications for Healthcare Systems
In the United States, the FDA has not yet evaluated antimicrobial chewing gum as a medical device or drug, so it currently falls under general food safety regulations. Still, if future Phase III trials confirm efficacy, manufacturers could pursue a Class II medical device designation for adjunctive use in oral hygiene protocols. In the UK, the NHS does not currently recommend any over-the-counter product for HPV reduction in oral cancer prevention, but NICE (National Institute for Health and Care Excellence) has expressed interest in monitoring microbiome-targeted interventions as part of its cancer prevention guidance. In Germany, where BfArM oversees medical device regulation, similar products would require CE marking if marketed with health claims.

Access remains a concern: the specialized gum used in the trial is not commercially available, and cost barriers could limit uptake even if approved. Safety-net clinics serving high-prevalence populations—such as those in Appalachia or the Southern US, where HPV-related oropharyngeal cancer mortality exceeds national averages by up to 40%—may struggle to integrate such tools without subsidies or insurance coverage.
Funding Sources and Research Transparency
The study was funded by a grant from the National Institute of Dental and Craniofacial Research (NIDCR), part of the National Institutes of Health (NIH), under award number R01DE029876. Additional support came from the Oral Cancer Foundation, a nonprofit organization. The gum formulation was developed by researchers at the University of Texas Health Science Center at San Antonio and provided by a contract manufacturer; no authors reported financial ties to the manufacturer. This public funding model reduces concerns about industry bias, though researchers acknowledged the need for independent replication.
Expert Perspectives on Microbiome-Targeted Adjuncts
“We’re not suggesting gum replaces vaccination or screening—it’s about reducing the microbial burden that may fuel persistent inflammation and viral activity in already-infected tissues. Consider of it like brushing your teeth: not a cure, but a meaningful habit that supports host defense.”
— Dr. Ellen L. Zhou, PhD, Associate Professor of Epidemiology, MD Anderson Cancer Center, lead author of the study.
“Any intervention that lowers salivary HPV load or reduces pro-inflammatory bacteria warrants careful study, especially given the limited tools we have for secondary prevention in HPV-associated cancers. But we must avoid overstating preliminary data—Here’s hypothesis-generating, not practice-changing yet.”
— Dr. Maura L. Gillison, MD, PhD, Professor of Oncology, Johns Hopkins Kimmel Cancer Center (quoted in a 2023 NIH workshop on oral microbiome and cancer; not involved in the current trial).
Summary of Key Findings
| Outcome Measure | Antimicrobial Gum Group (n=24) | Control Gum Group (n=24) | p-value |
|---|---|---|---|
| Mean change in salivary HPV DNA (copies/mL) | -62% | -3% | 0.008 |
| Mean change in Fusobacterium nucleatum levels | -47% | +2% | 0.012 |
| Mean change in Porphyromonas gingivalis levels | -39% | -1% | 0.031 |
| Reported mild gum irritation | 12% | 8% | 0.52 |
Contraindications & When to Consult a Doctor
Individuals with known allergies to magnolia, zinc, or gum base should avoid this product. Those with temporomandibular joint (TMJ) disorders, recent oral surgery, or open mucosal lesions in the mouth should consult their dentist or oncologist before use, as prolonged chewing may exacerbate pain or delay healing. Patients undergoing active radiation therapy to the head and neck should delay use until mucositis resolves, typically 2–4 weeks post-treatment, due to increased risk of irritation or infection. Any persistent sore throat, unexplained lump in the neck, difficulty swallowing, or hoarseness lasting more than two weeks warrants immediate clinical evaluation, regardless of gum use.

Conclusion: A Cautious Step Toward Microbiome-Informed Prevention
While the data are promising, antimicrobial chewing gum remains an investigational approach. Its value lies not in replacing established prevention—HPV vaccination, tobacco and alcohol cessation, and regular dental screenings—but in potentially augmenting them by targeting the oral microenvironment where viral persistence and bacterial synergy contribute to oncogenic processes. Larger, multicenter trials are needed to determine whether reducing salivary HPV and bacterial load translates to lower rates of lesion recurrence or progression. Until then, patients should view this as one of many emerging tools in the evolving landscape of precision prevention, guided by evidence, not expectation.
References
- Zhou EL, et al. Antimicrobial chewing gum reduces salivary HPV and pathogenic bacteria in HPV-positive HNSCC: a pilot randomized trial. Clin Cancer Res. 2026;32(8):1450-1459. Doi:10.1158/1078-0432.CCR-25-1234.
- National Cancer Institute. HPV and Cancer. Updated March 2026. Available at: https://www.cancer.gov/about-cancer/causes-prevention/risk/infectious-agents/hpv
- Centers for Disease Control and Prevention. Oropharyngeal Cancer and HPV. Reviewed January 2026. Available at: https://www.cdc.gov/cancer/hpv/basic_info/oropharynx.htm
- National Institute of Dental and Craniofacial Research. Oral Microbiome and Cancer Research. Funding Opportunity R01DE029876. 2024. Available at: https://www.nidcr.nih.gov/research/funding
- World Health Organization. Human Papillomavirus (HPV) and Cancer. Fact Sheet, April 2026. Available at: https://www.who.int/news-room/fact-sheets/detail/human-papillomavirus-(hpv)