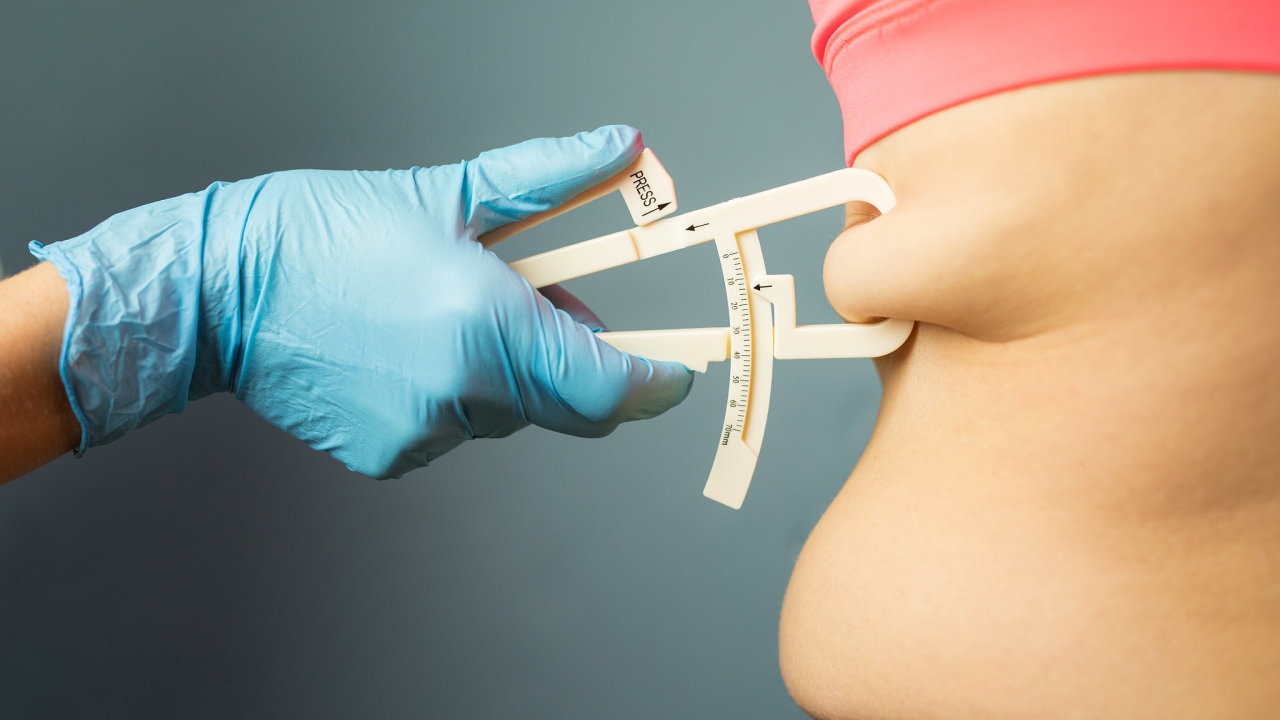
In April 2024, Czech researchers revealed that visceral fat accumulation around the waistline is a more reliable predictor of imminent heart failure than Body Mass Index (BMI), with a simple reduction in waist circumference offering significant protective benefits—a finding that has since spurred innovation in wearable health tech and AI-driven preventive cardiology, as clinicians seek objective, continuous biomarkers beyond episodic clinical measurements.
Why Waist Circumference Outperforms BMI in Cardiac Risk Stratification
BMI’s failure as a standalone predictor stems from its inability to distinguish between subcutaneous and visceral adipose tissue, the latter being metabolically active and directly linked to inflammation, insulin resistance, and ectopic fat deposition in organs like the heart and liver. A 2023 study published in the European Heart Journal found that individuals with normal BMI but elevated waist-to-height ratio (>0.5) had a 2.3x higher risk of cardiovascular events than those with low visceral fat, regardless of overall weight. This visceral fat secretes adipokines like leptin and resistin while suppressing adiponectin, creating a pro-inflammatory milieu that accelerates atherosclerosis and endothelial dysfunction—processes BMI overlooks entirely.
Waist circumference, by contrast, correlates strongly with intra-abdominal fat volume as validated by MRI and CT scans. In the Czech cohort, every 5cm increase in waist circumference above sex-specific thresholds (94cm for men, 80cm for women) corresponded to a 16% rise in heart failure hospitalization risk over five years, a gradient steeper than any BMI-based risk curve. Crucially, this metric responds rapidly to lifestyle intervention—reductions of just 4cm can improve cardiac strain markers within weeks, offering a tangible feedback loop for patients.
From Tape Measure to Tensor Flow: How Wearables Are Closing the Gap
The clinical insight has ignited a wave of innovation in sensor fusion and edge AI. Companies like BioFourmis and Current Health are now integrating multi-site bioimpedance sensors into chest straps and smart belts that estimate visceral fat depth in real time by measuring tissue conductivity at multiple frequencies—leveraging the fact that fat and muscle have distinct electrical properties. These devices sample at 25Hz, applying FFT-based impedance spectroscopy to distinguish extracellular water (linked to edema) from intracellular shifts tied to cellular metabolism.
What sets the latest generation apart is on-device neural network inference. Using quantized TensorFlow Lite models trained on DEXA-validated datasets, these wearables achieve visceral fat estimation errors under 8% compared to MRI gold standard—without sending raw data to the cloud. This edge-first approach addresses both latency concerns (critical for real-time feedback during exercise) and GDPR-grade privacy mandates, a necessity given the sensitivity of longitudinal metabolic data.
“We’re moving beyond step counts and heart rate variability into true tissue composition analytics. The breakthrough isn’t just the sensor—it’s running a 200KB CNN on a Cortex-M55 that can share you if your visceral fat is rising before your belt feels tighter.”
The Data Interoperability Challenge: Bridging Consumer Wearables and EHRs
Despite technical progress, adoption hinges on seamless integration with clinical workflows. Current efforts focus on mapping waist-derived metrics to established cardiology ontologies like SNOMED-CT and LOINC. For instance, a sustained waist-to-height ratio >0.55 over 30 days now triggers a proposed SNOMED-CT extension concept (pending review) for “metabolically hazardous central adiposity,” enabling automated alerts in Epic and Cerner EHRs when paired with FHIR-enabled devices.
Yet interoperability remains fragmented. While Apple Watch and Samsung Galaxy Watch now report waist circumference estimates via third-party apps using their accelerometer and gyroscope data to model torso movement, these metrics lack FDA clearance for diagnostic use. In contrast, medical-grade devices like the BioSticker (BioIntelliSense) have secured 510(k) clearance for respiratory rate and temperature but not yet for adiposity estimation—a gap that limits reimbursement pathways.
Open-source initiatives are attempting to bridge this divide. The Open mHealth schema has adopted waist circumference as a core vital sign schema (omh:waist-circumference), and projects like GNU Health are piloting EHR modules that ingest this data via MQTT brokers, normalizing it against age-, sex-, and ethnicity-adjusted risk curves derived from the UK Biobank.
What In other words for the Preventive Health Tech Arms Race
The implication extends beyond individual diagnostics. As payers shift toward value-based care, metrics like waist circumference offer a rare combination of clinical validity, low-cost measurement, and actionability—making them ideal for risk adjustment in accountable care organizations (ACOs). This could redefine device competition: instead of chasing marginal gains in ECG accuracy, the next frontier may be who can deliver the most clinically actionable adiposity insight with the least user burden.
For developers, this creates pressure to open sensor APIs. Companies that restrict waist-derived metrics to proprietary clouds (like some current smart scale ecosystems) risk exclusion from clinical networks embracing FHIR and SMART on FHIR standards. Conversely, those offering local-first processing with exportable CSV/FHIR bundles—such as Withings’ novel Body Comp API—are gaining traction in remote patient monitoring pilots across the EU.
the waist circumference revolution underscores a broader truth: the most impactful health innovations often arise not from chasing novelty, but from refining the measurement of what we’ve long known matters. In an era of AI hallucination and biomarker overreach, sometimes the simplest tape measure—augmented by a neural net on your belt—still tells the truest story.