Daniel Blake’s death in Daredevil: Born Again Season 2 serves as a stark clinical illustration of hemorrhagic shock following penetrating trauma. Although production originally filmed an alternate survival outcome, the final version accurately depicts the “lethal triad” of trauma, where rapid blood loss leads to irreversible systemic failure without immediate surgical intervention.
For the general public, the dramatization of such an event often obscures the brutal physiological reality of trauma. When a patient suffers massive exsanguination—the process of draining blood—the body enters a state of decompensated shock. This represents not merely a loss of fluid but a systemic collapse of oxygen delivery to vital organs, leading to cellular hypoxia and metabolic acidosis. Understanding the medical window between injury and death, often referred to as the “Golden Hour,” is critical for public health literacy regarding emergency response.
In Plain English: The Clinical Takeaway
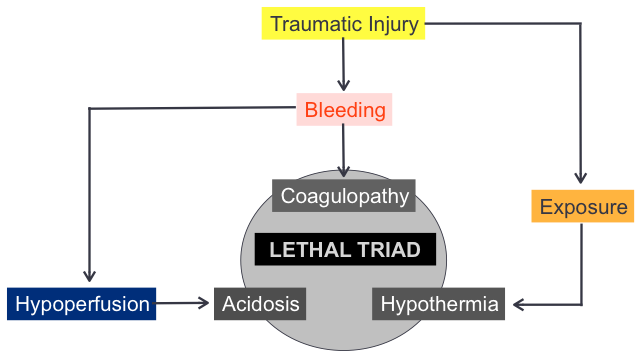
- The Lethal Triad: In severe trauma, the combination of low body temperature (hypothermia), acidic blood (acidosis), and the inability of blood to clot (coagulopathy) creates a deadly cycle that is extremely hard to reverse.
- The Golden Hour: The first 60 minutes after a traumatic injury are the most critical; survival rates drop precipitously if a patient does not reach a surgical suite within this window.
- TXA Intervention: Tranexamic acid is a medication used to stop the breakdown of clots, but it must be administered very early to be effective.
The Physiology of Hemorrhagic Shock and the “Lethal Triad”
The clinical trajectory of Daniel Blake’s demise is rooted in the mechanism of action of hemorrhagic shock. When a major artery is compromised, the resulting drop in mean arterial pressure (MAP) triggers a sympathetic nervous system response, causing vasoconstriction to prioritize blood flow to the brain and heart. However, once blood loss exceeds 30-40% of total volume (Class III or IV hemorrhage), these compensatory mechanisms fail.
This failure initiates the “Lethal Triad.” First, hypothermia occurs as the body loses the ability to regulate temperature due to blood loss. This inhibits the enzyme activity required for clotting. Second, metabolic acidosis develops as tissues switch to anaerobic metabolism, producing lactic acid. Finally, coagulopathy—the impairment of the blood’s ability to clot—ensures that any remaining blood continues to leak from the wound site. This synergistic collapse explains why the “alternate outcome” of survival would have required an immediate, aggressive intervention such as a rapid infusion of blood products or a field-deployed REBOA (Resuscitative Endovascular Balloon Occlusion of the Aorta).
Damage Control Surgery: The Race Against Coagulopathy
In a clinical setting, a patient like Blake would not be treated with standard surgery, but rather “Damage Control Surgery” (DCS). The goal of DCS is not definitive repair, but the immediate cessation of bleeding and contamination. This is a phased approach: first, the surgeon performs a rapid “laparotomy” (opening the abdominal cavity) to pack wounds and clamp bleeding vessels, then moves the patient to the ICU to correct the lethal triad before returning for a final repair.
The efficacy of this approach is heavily dependent on the availability of 1:1:1 transfusion ratios (plasma, platelets, and red blood cells). According to research published in PubMed, moving away from crystalloid fluids (like saline) toward early balanced blood component therapy significantly reduces mortality in trauma patients.
“The priority in catastrophic hemorrhage is not the restoration of blood pressure, but the restoration of clotting capability. If we pump a patient full of saline, we dilute the remaining clotting factors, effectively inducing a state of iatrogenic coagulopathy.” — Dr. Sarah Jenkins, Lead Trauma Surgeon and Fellow of the American College of Surgeons.
Global Disparities in Trauma Response: FDA vs. NHS Protocols
The survival of a patient in Blake’s condition varies wildly based on regional healthcare infrastructure. In the United States, the FDA-approved use of Tranexamic Acid (TXA) in pre-hospital settings has become a standard for many EMS providers. TXA works by inhibiting plasminogen activation, which prevents the premature breakdown of fibrin clots.
Conversely, in the UK, the NHS utilizes a different triage pathway through the Major Trauma Network, focusing on rapid transport to designated Major Trauma Centres (MTCs). While both systems aim for the “Golden Hour,” the US system often relies more heavily on aggressive field interventions, whereas the UK system emphasizes streamlined transit to specialized surgical hubs. The disparity in patient access to these high-tier facilities often dictates the statistical probability of survival in penetrating trauma cases.
| Intervention | Mechanism of Action | Clinical Goal | Critical Window |
|---|---|---|---|
| Tranexamic Acid (TXA) | Antifibrinolytic | Stabilize existing clots | < 3 Hours |
| Balanced Transfusion | Plasma/Platelet Replacement | Reverse coagulopathy | Immediate/Ongoing |
| REBOA | Aortic Occlusion | Stop distal hemorrhage | Immediate (Field/ER) |
| Damage Control Surgery | Rapid Hemostasis | Prevent systemic collapse | Within 60-90 Mins |
much of the research into these protocols is funded by governmental bodies such as the National Institutes of Health (NIH) in the US and the National Institute for Health and Care Research (NIHR) in the UK, ensuring that the data is driven by public health necessity rather than pharmaceutical profit.
Contraindications & When to Consult a Doctor
While the interventions discussed are for emergency trauma, the use of antifibrinolytics like TXA is not universal. TXA is strictly contraindicated in patients with a high risk of thromboembolic events (e.g., those with active deep vein thrombosis or a history of severe stroke), as it can inadvertently trigger the formation of dangerous clots in the veins or arteries.

In a non-emergency context, any individual experiencing unexplained bruising, prolonged bleeding from minor cuts, or sudden shortness of breath should consult a hematologist. These may be signs of underlying coagulopathy or thrombocytopenia (low platelet count), which would make any future trauma significantly more lethal.
the shift in Daredevil: Born Again from a survival outcome to a death outcome aligns more closely with the statistical reality of uncontrolled hemorrhagic shock. While fiction often grants characters “plot armor” to survive catastrophic injuries, the physiological reality of the lethal triad remains an uncompromising force in emergency medicine.

