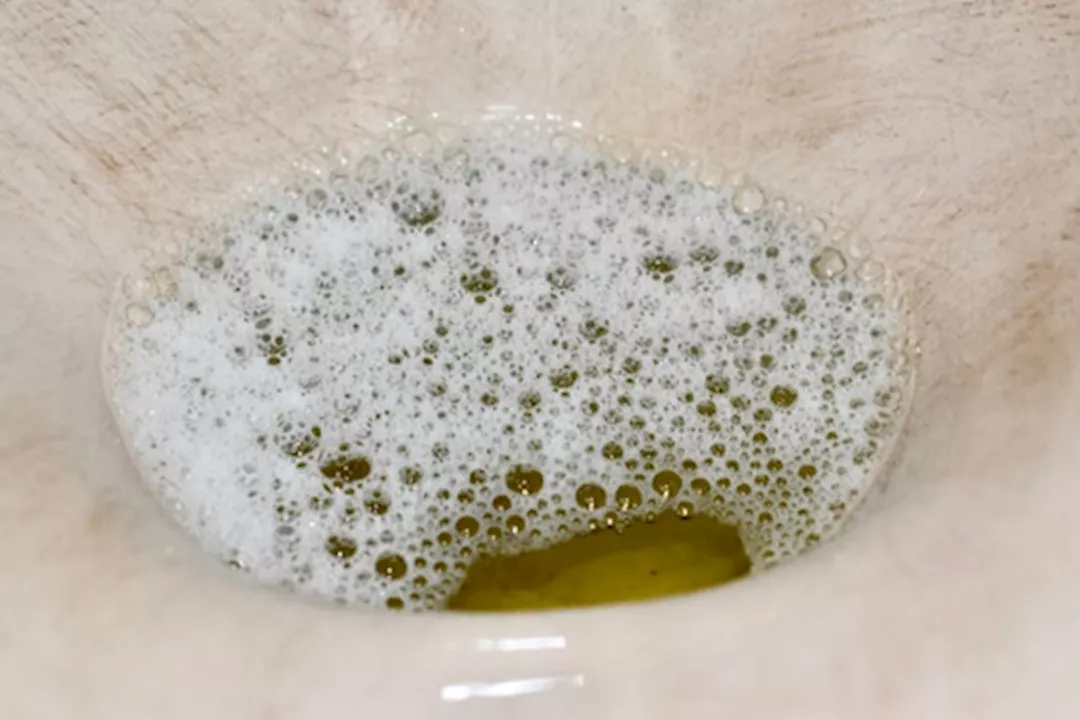
Foamy urine can be a benign result of urinary velocity or a critical clinical sign of proteinuria—the leakage of excess protein into the urine. While often harmless, persistent foam may indicate glomerular damage, necessitating immediate medical evaluation to prevent progression toward chronic kidney disease (CKD) and systemic organ failure.
For millions of patients globally, the appearance of foam in the toilet bowl is the first visible manifestation of a silent crisis. The kidneys serve as the body’s primary filtration system and when this system fails, the biological consequences are catastrophic. Understanding the distinction between “transient” foam and “pathological” foam is not merely a matter of curiosity. it is a vital step in early intervention for metabolic and renal disorders.
In Plain English: The Clinical Takeaway
- Foam is a Signal, Not a Diagnosis: Bubbles in urine can be caused by a fast stream or dehydration, but persistent, thick foam often means your kidneys are leaking protein.
- The “Filter” Analogy: Think of your kidney’s filters (glomeruli) as a fine sieve. When these sieves are damaged, proteins that should stay in your blood “leak” into your urine, creating a soap-like foam.
- Testing is Mandatory: You cannot diagnose kidney health by sight. A simple dipstick test or an Albumin-to-Creatinine Ratio (ACR) test is required to confirm if the foam is dangerous.
The Glomerular Filter: The Mechanism of Action Behind the Foam
To understand why urine foams, one must examine the mechanism of action—the specific biological process—of the glomerular filtration barrier. The glomerulus is a network of capillaries that filters waste from the blood. Under normal physiological conditions, the glomerular basement membrane (GBM) utilizes a negative electrical charge and a physical pore size to repel large molecules, specifically albumin, a key blood protein.
When the GBM is compromised due to inflammation or scarring, this “charge barrier” fails. Albumin leaks into the renal tubules and eventually into the urine. Because proteins act as surfactants—substances that reduce the surface tension of a liquid—they create stable bubbles when the urine hits the water. This is clinically termed proteinuria (the presence of abnormal quantities of protein in the urine).
The severity of this leakage is often graded by the amount of protein lost per 24 hours. While minor leakage can occur during intense exercise or high fever, chronic proteinuria is a hallmark of nephrotic syndrome, a condition where the kidneys leak massive amounts of protein, leading to severe edema (swelling) in the legs and ankles.
Systemic Drivers: Diabetes, Hypertension, and the Global Epidemic
The prevalence of proteinuria is inextricably linked to the global rise in Type 2 Diabetes and hypertension. In diabetic nephropathy, high blood glucose levels cause the kidneys to over-filter (hyperfiltration), which eventually damages the glomeruli. This process is a primary driver of End-Stage Renal Disease (ESRD) worldwide.
From a geo-epidemiological perspective, the approach to managing these risks varies. In the United States, the FDA has recently expanded the indications for SGLT2 inhibitors—a class of medications originally designed for diabetes—to include the treatment of CKD in non-diabetic patients due to their ability to reduce intraglomerular pressure. Similarly, the National Health Service (NHS) in the UK and the European Medicines Agency (EMA) emphasize the early use of ACE inhibitors or ARBs to “shield” the kidneys by lowering systemic blood pressure and reducing protein leakage.
“Proteinuria is not just a symptom of kidney disease; it is an independent risk factor for cardiovascular events. When the kidneys leak protein, it signals a systemic vascular vulnerability that affects the heart and brain as well.” — Consensus statement from the National Kidney Foundation (NKF).
The funding for the majority of these large-scale longitudinal studies, such as the DAPA-CKD trials, is often a hybrid of pharmaceutical investment and government grants (such as the NIH in the US). While pharmaceutical funding is common, the peer-reviewed nature of these trials ensures that the efficacy of these drugs is measured against rigorous double-blind placebo-controlled standards—meaning neither the patient nor the doctor knows who receives the drug, eliminating bias.
Comparing Proteinuria Levels and Clinical Significance
The following table outlines the clinical thresholds used by nephrologists to categorize protein leakage and determine the urgency of intervention.
| Category | Albuminuria Level (mg/g Creatinine) | Clinical Interpretation | Primary Action/Risk |
|---|---|---|---|
| Normal | < 30 mg/g | Healthy filtration | Routine monitoring |
| Microalbuminuria | 30 – 300 mg/g | Early-stage kidney stress | Aggressive BP and Glucose control |
| Macroalbuminuria | > 300 mg/g | Overt kidney damage | High risk of progression to ESRD |
Contraindications & When to Consult a Doctor
It is critical to distinguish between “lifestyle foam” and “clinical foam.” Foamy urine caused by dehydration or a rapid urinary stream is not a medical emergency. However, certain contraindications—factors that make a situation more dangerous—require immediate triage.
You must consult a physician immediately if foamy urine is accompanied by:
- Peripheral Edema: Noticeable swelling in the ankles, feet, or around the eyes (periorbital edema).
- Hypertension: Unexplained spikes in blood pressure that do not respond to standard medication.
- Hematuria: The presence of blood in the urine, which may appear pink, red, or cola-colored.
- Oliguria: A significant decrease in the volume of urine produced daily.
Patients already taking NSAIDs (non-steroidal anti-inflammatory drugs) like ibuprofen or naproxen should be particularly vigilant, as these medications can exacerbate glomerular damage and accelerate proteinuria in predisposed individuals.
The Future of Renal Diagnostics
As we move further into 2026, the medical community is shifting toward “precision nephrology.” We are moving away from simple dipstick tests toward more sensitive biomarkers that can detect kidney stress before protein even enters the urine. The integration of AI-driven screening in primary care settings is expected to reduce the time between the first appearance of foamy urine and the initiation of nephroprotective therapy.
foamy urine is a biological warning light. When addressed with evidence-based medicine and early diagnostic rigor, the progression to kidney failure is not inevitable, but preventable.
References
- PubMed: National Library of Medicine – Glomerular Filtration and Proteinuria Studies
- The Lancet: Global Burden of Kidney Disease and Diabetes
- World Health Organization (WHO): Noncommunicable Diseases and Renal Health
- Centers for Disease Control and Prevention (CDC): Chronic Kidney Disease Guidelines
- KDIGO (Kidney Disease: Improving Global Outcomes) Clinical Practice Guidelines