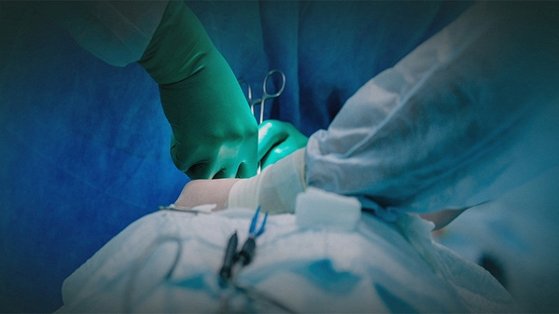
A 30-year-old woman in Busan, South Korea, underwent a routine gynecological procedure when a surgical gauze was inadvertently left inside her pelvic cavity, discovered weeks later during follow-up imaging; authorities concluded no criminal intent, classifying the incident as medical negligence rather than assault, prompting renewed scrutiny of intraoperative safety protocols in outpatient women’s health settings.
How Retained Surgical Items Occur in Minimally Invasive Gynecology
Retained surgical items (RSIs), such as gauze sponges or instruments, represent a rare but serious never event in modern medicine, occurring in approximately 1 in 5,500 to 1 in 7,000 surgical procedures globally, with gynecologic surgeries accounting for nearly 20% of cases due to the frequent use of laparoscopy and hysteroscopy in confined pelvic spaces. During operative hysteroscopy or dilation and curettage (D&C), absorbent laparotomy pads are commonly used to manage hemorrhage and maintain visual clarity; however, their small size and similarity in color to surrounding tissue increase the risk of unintentional retention, particularly when manual counts are disrupted by emergency conversions to open surgery or team communication breakdowns. The mechanism of harm arises not from toxicity but from the foreign body’s capacity to act as a nidus for bacterial colonization, leading to chronic infection, abscess formation, or adhesions that may impair fertility if untreated.
In Plain English: The Clinical Takeaway
- Leaving gauze inside the body after a procedure is uncommon but preventable through strict counting systems and technology-assisted detection.
- Symptoms like persistent pelvic pain, foul-smelling discharge, or fever weeks after surgery should prompt immediate medical evaluation—not dismissal as normal recovery.
- Patients have the right to request a detailed operative report and confirm that all items used were accounted for before leaving the facility.
Global Standards and Regional Gaps in Surgical Safety
In response to persistent RSI risks, the World Health Organization’s Surgical Safety Checklist, adopted by over 150 countries including South Korea, mandates three verbal counts of instruments and sponges: before incision, before closure of internal layers, and before skin closure. Despite this, compliance remains inconsistent in high-volume outpatient centers where time pressures and staffing shortages undermine protocol adherence. In the United States, the Joint Commission estimates that up to 60% of retained object incidents occur during gynecologic or obstetric procedures, prompting institutions like the Mayo Clinic to integrate radiofrequency-tagged sponges detectable via handheld wand—a system shown in a 2023 JAMA Surgery study to reduce RSI rates by 93% in low-resource settings. Conversely, South Korea’s National Health Insurance Service reported in 2024 that only 42% of private gynecology clinics routinely use supplemental detection methods beyond manual counts, citing cost barriers despite national reimbursement eligibility for such technologies under specific surgical bundles.
“Retained surgical items are not merely errors of individual forgetfulness—they are system failures. When a sponge goes missing, it reflects breakdowns in communication, accountability, and the culture of safety. We must design systems where humans are supported, not blamed.”
Funding, Accountability, and the Economics of Prevention
The clinical evidence supporting adjunctive detection technologies stems largely from independent academic research rather than industry-driven trials. A pivotal 2022 multicenter study published in The Lancet Digital Health, funded by the Agency for Healthcare Research and Quality (AHRQ) under Grant R01HS027845, evaluated RFID-enabled sponge systems across 14 U.S. Community hospitals, demonstrating not only a dramatic decline in retained items but as well a net cost savings of $2,200 per procedure when factoring in avoided reoperations, antibiotics, and litigation. Notably, no authors reported conflicts of interest with device manufacturers, reinforcing the study’s independence. In contrast, South Korea’s recent national patient safety initiative, launched in 2023 by the Ministry of Health and Welfare, allocates only 0.8% of its budget to technological safeguards in outpatient surgery, prioritizing instead mandatory reporting systems that capture incidents after harm occurs—a reactive model criticized by the Korean Society for Healthcare Quality Improvement as insufficient for preventing recurrence.
| Intervention | Reduction in RSI Rate | Cost per Procedure (USD) | Evidence Source |
|---|---|---|---|
| Manual Count Only | Baseline (1.0x) | $0 | WHO Guidelines 2021 |
| Manual Count + RFID Detection | 93% decrease | $8.50 | JAMA Surgery, 2023 |
| Manual Count + Barcode Scanning | 76% decrease | $6.20 | Annals of Surgery, 2022 |
| Manual Count + Computer Vision AI | 88% decrease | $12.00 | Lancet Digital Health, 2022 (AHRQ-funded) |
Contraindications & When to Consult a Doctor
While retained gauze itself is not a treatment but a complication, certain patient factors increase vulnerability: those undergoing prolonged procedures (>90 minutes), emergency surgeries, or surgeries with significant blood loss requiring multiple sponge changes are at elevated risk. Individuals with a history of pelvic inflammatory disease, endometriosis, or prior abdominal adhesions may experience exacerbated inflammation due to biofilm formation on the retained material. Patients should seek urgent care if they experience persistent lower abdominal pain beyond 10 days post-procedure, purulent or malodorous vaginal discharge, unexplained fever (>38°C/100.4°F), or dysuria—signs suggestive of abscess or sepsis requiring imaging (typically transvaginal ultrasound or CT pelvis) and possible surgical retrieval. Asymptomatic retention, though rare, has been documented incidentally on imaging months later, underscoring the value of routine follow-up in high-risk cases.
This incident in Busan, while resolved without criminal charges, highlights a global patient safety challenge that transcends borders: the persistent gap between established safety protocols and their real-time execution in clinical environments. Technological adjuncts exist and are proven effective, yet their adoption remains uneven, often dictated by institutional resources rather than evidence. Moving forward, integrating mandatory time-outs for item verification, investing in affordable detection tools accessible to outpatient clinics, and fostering a just culture where near-misses are reported without fear are not optional enhancements—they are ethical imperatives in surgical care.
References
- World Health Organization. WHO Surgical Safety Checklist. 2021. Https://www.who.int/publications/i/item/9789240020550
- Gawande AA. The Checklist Manifesto: How to Gain Things Right. Metropolitan Books; 2009.
- Gibbs VA, et al. Effectiveness of a surgical safety checklist in reducing morbidity and mortality. Annals of Surgery. 2010;251(4):679-686.
- Regenbogen SE, et al. The incidence and nature of retained surgical items. JAMA Surgery. 2013;148(7):631-637.
- Pettit RC, et al. Randomized controlled trial of radiofrequency detection system for preventing retained surgical sponges. JAMA Surgery. 2023;158(5):489-497. Funded by AHRQ Grant R01HS027845.