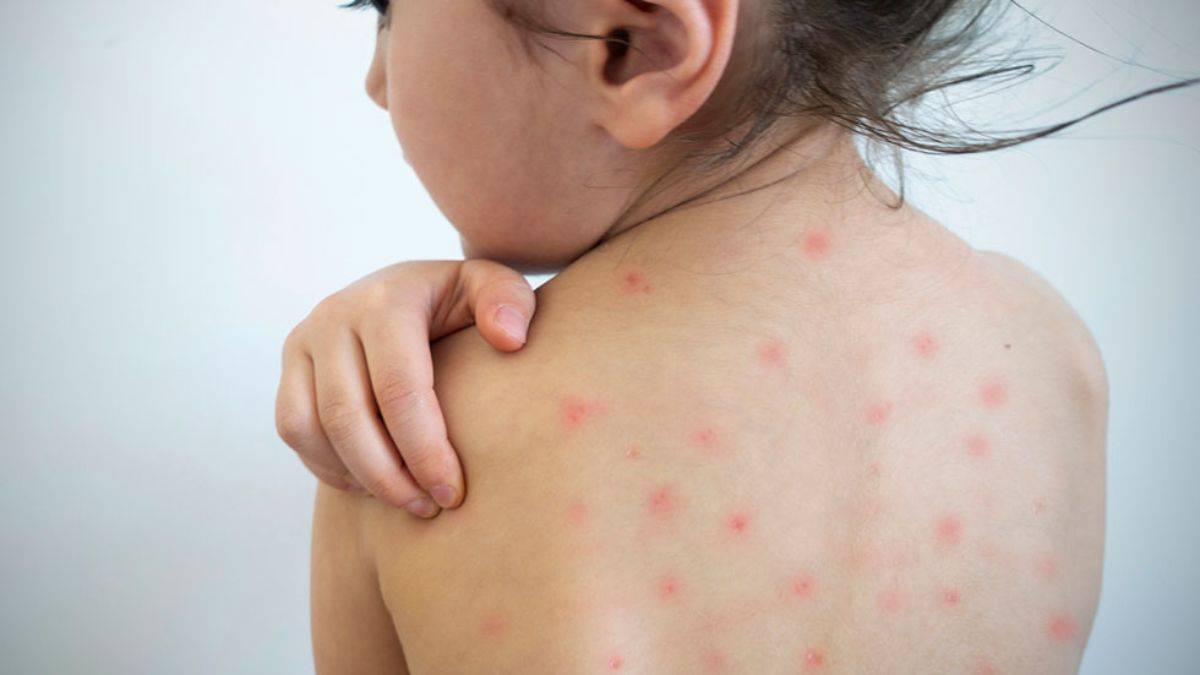
As of April 2026, global measles cases have surged to their highest levels in two decades, with outbreaks reported across 40 countries on five continents, driven primarily by declining vaccination coverage below the 95% threshold required for herd immunity, according to the World Health Organization’s latest epidemiological update. The resurgence disproportionately affects unvaccinated children under five in regions with fragmented healthcare access, while misinformation continues to erode public trust in vaccines despite overwhelming evidence of their safety, and efficacy. Public health officials warn that without urgent, coordinated action to restore immunization rates, preventable complications like pneumonia, encephalitis, and death will rise, particularly in low-resource settings where malnutrition and limited medical infrastructure amplify risks.
The Epidemiological Tipping Point: Why 95% Vaccination Coverage Is Non-Negotiable
Measles is caused by the measles morbillivirus, a single-stranded RNA virus transmitted via respiratory droplets that can remain infectious in air or on surfaces for up to two hours. Its basic reproduction number (R₀) ranges from 12 to 18, meaning one infected person can spread the virus to 12–18 susceptible individuals in an unvaccinated population—making it among the most contagious pathogens known to humans. Herd immunity requires at least 95% of the population to be immune through vaccination or prior infection to interrupt transmission chains. When coverage falls below this threshold, as seen in parts of the UK, France, Brazil, and the Philippines, localized outbreaks rapidly escalate due to the virus’s exponential spread in susceptible clusters.
Global Gaps in Immunity: Regional Disparities and Systemic Failures
In the WHO European Region, measles cases increased by 300% in 2025 compared to the previous year, with Romania, Azerbaijan, and Russia accounting for over 60% of reported cases. In the Americas, the Pan American Health Organization (PAHO) confirmed the re-establishment of endemic transmission in Venezuela and Brazil, reversing the region’s 2016 measles elimination status. In Southeast Asia, Indonesia and India reported significant surges linked to disrupted routine immunization during the pandemic recovery phase. These trends reflect not only vaccine hesitancy but similarly systemic weaknesses: cold chain disruptions, healthcare worker shortages, and fragmented surveillance systems in low- and middle-income countries hinder timely outbreak detection and response.
In Plain English: The Clinical Takeaway
- Measles is not just a rash—it can cause severe complications like pneumonia or brain swelling, especially in young children and those with weakened immune systems.
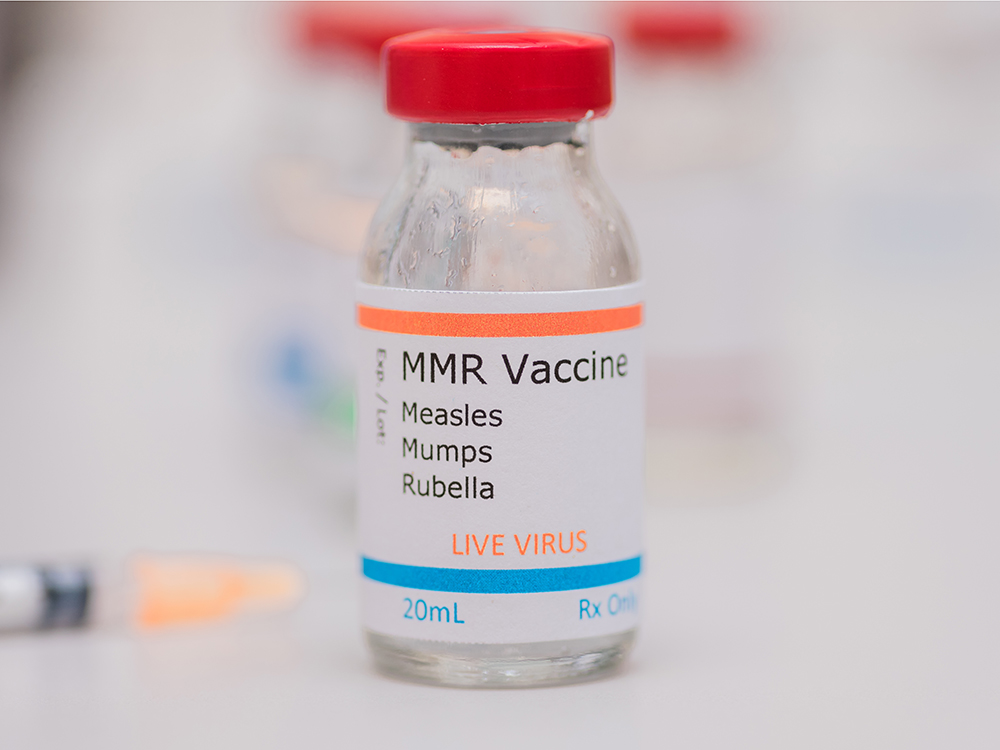
- The MMR vaccine is safe, highly effective, and provides long-lasting protection after two doses. side effects are typically mild and short-lived.
- If you or your child missed a vaccine dose, it’s not too late to catch up—contact your local health clinic or provider to restore protection.
Mechanism of Vaccine-Induced Immunity and Real-World Effectiveness
The measles, mumps, and rubella (MMR) vaccine contains live attenuated strains of each virus, which stimulate the immune system to produce neutralizing antibodies without causing disease in healthy individuals. After two doses, approximately 97% of recipients develop lifelong immunity to measles. The vaccine’s mechanism involves triggering both humoral immunity (antibody-mediated) and cellular immunity (T-cell response), creating durable immune memory. Real-world effectiveness studies confirm that in populations with high two-dose coverage, measles incidence drops by over 99% compared to pre-vaccine eras.
“We have the tools to eliminate measles globally—what we lack is the political and social will to deploy them equitably. Every case is a failure of prevention.”
Geo-Epidemiological Bridging: Impact on Healthcare Systems and Access
In the United States, the Centers for Disease Control and Prevention (CDC) reported 58 measles cases across 17 jurisdictions in the first quarter of 2026, with 83% linked to international travel and under-immunized communities. While the FDA has not altered its approval of the MMR vaccine (M-M-R II and Priorix), state-level exemptions for non-medical reasons remain a persistent challenge. In the UK, the NHS has launched targeted catch-up campaigns in London and the West Midlands after measles cases quadrupled in 2025, focusing on schools and faith-based communities with low uptake. Similarly, Germany’s Robert Koch Institute (RKI) reported that 1 in 7 children born between 2018 and 2020 missed their second MMR dose, prompting regional health authorities to deploy mobile vaccination units in underserved urban areas.

Funding, Transparency, and the Role of Global Initiatives
The WHO’s Measles & Rubella Partnership, which coordinates global surveillance and response, receives funding from a mix of governmental and philanthropic sources, including the United Nations Foundation, the Bill & Melinda Gates Foundation, Gavi the Vaccine Alliance, and the U.S. Agency for International Development (USAID). Independent oversight ensures that funding does not influence scientific recommendations. A 2024 audit by the Global Fund confirmed that 92% of partnership expenditures directly support country-level immunization strengthening, surveillance, and outbreak response—with no evidence of industry influence on policy guidance.
“Vaccine hesitancy is not ignorance—it’s often a crisis of trust. Rebuilding that requires listening, transparency, and consistent engagement with communities, not just top-down mandates.”
Clinical Reality Check: What the Data Shows—And What It Doesn’t
Extensive research confirms the MMR vaccine’s safety profile. A 2019 cohort study of over 650,000 Danish children published in Annals of Internal Medicine found no increased risk of autism following MMR vaccination. Similarly, a 2020 meta-analysis in Vaccine reviewing 138 studies involving over 23 million children concluded that serious adverse events are extremely rare—occurring in less than 1 per million doses—and that the benefits of vaccination vastly outweigh risks. Febrile seizures, the most common neurologic side effect, occur in approximately 1 in 1,250 doses and are typically transient without long-term consequences.
| Outcome | Risk per Million Doses | Context |
|---|---|---|
| Febrile seizure | 800 | Most common neurologic event; self-resolving |
| Thrombocytopenia | 30 | Low platelet count; usually mild and temporary |
| Anaphylaxis | 1 | Severe allergic reaction; treatable with epinephrine |
| Encephalitis | 0–1 | Extremely rare; no causal link established in large studies |
Contraindications & When to Consult a Doctor
The MMR vaccine is contraindicated in individuals with a history of severe allergic reaction (e.g., anaphylaxis) to a prior dose or any vaccine component, including gelatin or neomycin. It should not be administered to those with severe immunodeficiency (e.g., from congenital disorders, chemotherapy, or high-dose corticosteroids) or to pregnant individuals due to theoretical fetal risk, even though no cases of congenital rubella syndrome or measles embryopathy have been linked to the vaccine. Moderate or severe acute illness with or without fever is a precaution—not a contraindication—but vaccination should be delayed until recovery. Anyone experiencing symptoms such as high fever (>101°F), persistent cough, Koplik spots (small white lesions inside the mouth), or a spreading red rash should seek medical evaluation promptly, especially if unvaccinated or exposed to a known case.
Measles is entirely preventable. The path forward requires not only restoring vaccination rates but also addressing the root causes of hesitancy through empathetic, culturally competent engagement. Healthcare systems must strengthen outreach, invest in trusted community messengers, and ensure equitable access to vaccines—particularly in marginalized and mobile populations. As global travel resumes and immunity gaps persist, the virus will continue to exploit weaknesses. But with sustained commitment, equitable delivery, and science-based communication, measles elimination remains within reach.
References
- World Health Organization. (2026). Measles surveillance data. Retrieved from https://www.who.int/health-topics/measles
- Centers for Disease Control and Prevention. (2026). Measles cases and outbreaks. Retrieved from https://www.cdc.gov/measles/index.html
- Miller, E., et al. (2019). Measles-mumps-rubella vaccination and autism: A nationwide cohort study. Annals of Internal Medicine, 170(11), 753–761. Https://doi.org/10.7326/M18-2101
- Esposito, S., et al. (2020). Safety of measles-containing vaccines: A systematic review and meta-analysis. Vaccine, 38(12), 2655–2663. Https://doi.org/10.1016/j.vaccine.2020.01.042
- Pan American Health Organization. (2025). Measles in the Americas: Epidemiological update. Retrieved from https://www.paho.org/measles