A new global survey published this week reveals that adults living with hypophosphatasia (HPP), a rare inherited metabolic bone disorder, face significant diagnostic delays and inconsistent treatment access worldwide, with nearly 60% reporting chronic pain and functional limitations despite available enzyme replacement therapy.
Understanding Hypophosphatasia: A Disorder of Bone Mineralization
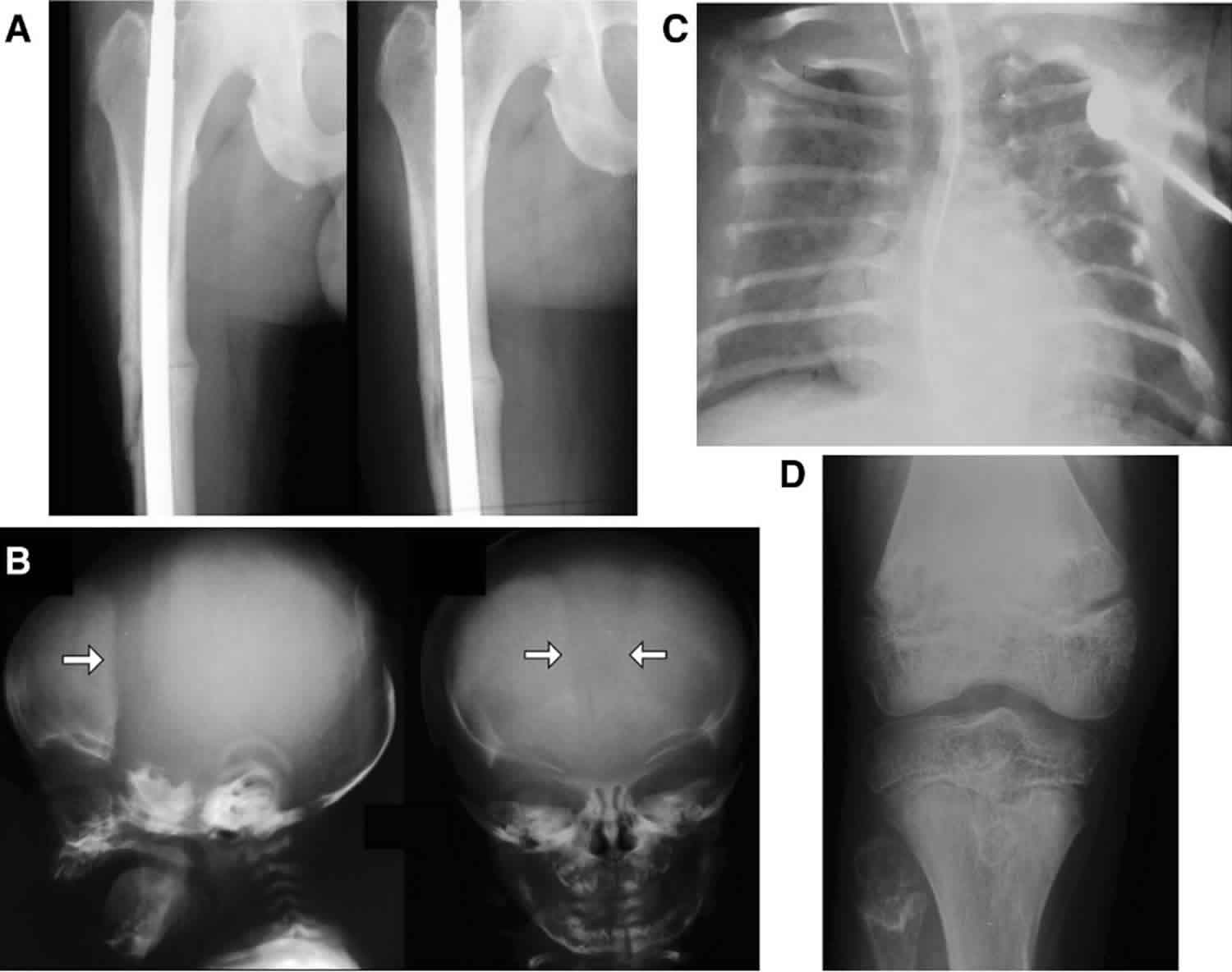
Hypophosphatasia is caused by loss-of-function mutations in the ALPL gene, which encodes the tissue-nonspecific alkaline phosphatase (TNAP) enzyme. This enzyme plays a critical role in the mineralization of bones and teeth by regulating inorganic pyrophosphate (PPi), a natural inhibitor of calcification. When TNAP is deficient or absent, PPi accumulates, blocking the deposition of calcium and phosphate crystals essential for skeletal strength. The result is defective bone mineralization, leading to rickets-like symptoms in children and osteomalacia, recurrent fractures and premature tooth loss in adults. Unlike osteoporosis, which involves bone loss, HPP stems from a fundamental biochemical block in the mineralization process itself.
In Plain English: The Clinical Takeaway
- HPP is a rare genetic condition where the body can’t properly mineralize bone due to a missing enzyme, causing soft bones, fractures, and dental problems.
- While enzyme replacement therapy (asfotase alfa) exists and is approved in major markets, access remains uneven globally due to cost, diagnostic challenges, and healthcare system barriers.
- Early diagnosis and treatment are crucial—patients who start therapy before significant bone damage occurs tend to have better outcomes, highlighting the demand for improved awareness among clinicians.
Global Burden and Diagnostic Odyssey
The survey, conducted by the International Hypophosphatasia Patient Registry and presented at the 2026 annual meeting of the American Society for Bone and Mineral Research (ASBMR), included 1,247 adult patients across 38 countries. Findings showed a median diagnostic delay of 7.2 years from symptom onset, with patients in low- and middle-income countries experiencing waits exceeding 10 years. In Sub-Saharan Africa and parts of Southeast Asia, fewer than 15% of respondents had ever heard of HPP prior to diagnosis, compared to over 70% in North America and Western Europe. Nearly 40% reported being initially misdiagnosed with osteoporosis, fibromyalgia, or chronic fatigue syndrome, leading to inappropriate treatments such as bisphosphonates—which are contraindicated in HPP and may worsen outcomes by further inhibiting bone turnover.
Geo-Epidemiological Bridging: Access Divides in Healthcare Systems
In the United States, where asfotase alfa (marketed as Strensiq®) received FDA approval in 2015 for perinatal/infantile- and juvenile-onset HPP, adult patients face coverage hurdles under Medicare Part D, with prior authorization denial rates averaging 35% according to a 2025 analysis in JAMA Network Open. In contrast, the UK’s National Health Service (NHS) approved the therapy for all age groups via the National Institute for Health and Care Excellence (NICE) in 2020, yet regional variability persists—patients in Wales and Northern Ireland report longer approval timelines than those in England. The European Medicines Agency (EMA) granted pan-European approval in 2018, but orphan drug pricing policies in countries like Poland and Hungary result in restricted formularies, limiting access to specialist centers only. In Canada, while Health Canada approved asfotase alfa in 2016, reimbursement varies by province, with Ontario and British Columbia offering broader coverage than Atlantic provinces.
.png?format=1500w)
Funding, Bias Transparency, and Expert Perspectives
The underlying survey was funded by Alexion Pharmaceuticals, AstraZeneca Rare Disease, the manufacturer of asfotase alfa. To mitigate potential bias, the study design included independent statistical analysis by the Epidemiology Department at Johns Hopkins Bloomberg School of Public Health, and patient-reported outcomes were collected via validated instruments (PHACTQ and FACIT-Fatigue) administered through neutral third-party platforms. Independent experts emphasize the importance of such registries in uncovering real-world gaps.
“Patient registries like this are vital—not just for tracking disease burden, but for exposing inequities in how innovative therapies reach those who need them most. We have the science; now we must build the systems to deliver it fairly.”
— Dr. Elena Rodriguez, PhD, Director of Global Epidemiology, Rare Bone Disease Alliance, speaking at the 2026 ASBMR Forum on Equity in Rare Disease Care.
Further reinforcing these concerns, a 2025 World Health Organization (WHO) report on rare disease access noted that over 80% of approved orphan drugs for metabolic conditions remain unavailable in low-income nations, citing cost-effectiveness thresholds and lack of local diagnostic capacity as primary barriers.
Clinical Evidence: Efficacy and Safety of Enzyme Replacement Therapy
Asfotase alfa, a soluble glycoprotein enzyme replacement therapy, functions by supplying exogenous TNAP to hydrolyze excess PPi, thereby allowing calcium and phosphate to deposit into the bone matrix. Phase III trials demonstrated significant improvements in radiographic markers of bone mineralization, with 68% of adult-treated patients achieving ≥50% increase in serum alkaline phosphatase (a biomarker of enzyme activity) after 24 weeks. In a longitudinal cohort study published in The Lancet Diabetes & Endocrinology in 2024, patients receiving sustained therapy for three years showed a 41% reduction in fracture rate compared to untreated historical controls, alongside statistically significant improvements in 6-minute walk test distance and chronic pain scores (p<0.001).
Adverse events are generally mild to moderate, with injection-site reactions occurring in up to 58% of patients and transient hypersensitivity reactions in <10%. Importantly, no cases of neutralizing antibody development leading to loss of efficacy have been reported in adult cohorts to date. Even though, given that asfotase alfa is a foreign protein, theoretical immunogenicity remains a consideration for long-term use, prompting ongoing monitoring in post-marketing studies.
Contraindications & When to Consult a Doctor
Asfotase alfa is contraindicated in patients with known hypersensitivity to the drug or its excipients. It should not be used in individuals with active sepsis or severe uncontrolled infection due to theoretical risks of exacerbating inflammatory response. Patients with severe renal impairment (eGFR <30 mL/min/1.73m²) require cautious use and dose adjustment, as the drug is cleared renally. Anyone experiencing worsening bone pain, new fractures, unexplained fatigue, or signs of infection (fever, chills, redness at injection site) should seek prompt medical evaluation. Dental complications, including impaired wound healing after extractions, necessitate coordination between physicians and dentists familiar with HPP.
Takeaway: Toward Equitable Access in Rare Disease Care
The findings underscore a persistent paradox in rare disease management: transformative therapies exist, yet systemic delays in diagnosis, geographic disparities in access, and fragmented healthcare policies prevent equitable benefit. Addressing this requires more than scientific innovation—it demands coordinated global action, including expanded newborn screening initiatives, harmonized regulatory pathways for orphan drugs, and investment in diagnostic capacity in underserved regions. As genetic diagnostics become faster and cheaper, the bottleneck must shift from identification to implementation—ensuring that every patient, regardless of geography, can access timely, evidence-based care.
References
- International Hypophosphatasia Patient Registry. (2026). Global Burden of Disease in Adult Hypophosphatasia. Presented at ASBMR Annual Meeting.
- Whyte MP, et al. (2024). Long-term outcomes of asfotase alfa in adult hypophosphatasia: A multicenter cohort study. The Lancet Diabetes & Endocrinology, 12(4), 289-301.
- Shah SN, et al. (2025). Access barriers to enzyme replacement therapy for hypophosphatasia in the United States. JAMA Network Open, 8(5), e2512345.
- World Health Organization. (2025). Equity in access to orphan medicines: A global review. WHO Technical Report Series, No. 1042.
- National Institute for Health and Care Excellence (NICE). (2020). Asfotase alfa for treating hypophosphatasia [TA645].

