For patients with celiac disease—a chronic autoimmune disorder—strict adherence to a gluten-free diet is not optional but a medical necessity to prevent intestinal damage, systemic inflammation, and long-term complications like lymphoma or osteoporosis. Published this week in the Journal of Gastroenterology and Hepatology, new epidemiological data confirms that even trace gluten exposure (as low as 10-50 parts per million) can trigger an immune response in 95% of diagnosed patients, underscoring why regulatory agencies like the FDA and EMA enforce rigorous labeling standards. This update arrives as global celiac prevalence rises—now affecting 1% of the population in the U.S. And EU—yet misdiagnosis remains rampant, delaying treatment for up to 10 years in 60% of cases.
In Plain English: The Clinical Takeaway
- Celiac disease is an autoimmune attack: Gluten (a protein in wheat, barley, rye) triggers your immune system to damage the villi—tiny finger-like projections in your small intestine—critical for nutrient absorption.
- No safe threshold exists: Even “gluten-free” foods with trace amounts can cause symptoms or intestinal harm. The FDA’s 20 ppm limit is the strictest global standard, but cross-contamination risks persist.
- Diagnosis is a puzzle: Blood tests (tTG-IgA) and endoscopy with biopsy are required; symptoms like fatigue or anemia can mimic other conditions, leading to delayed care.
While the medical consensus on gluten-free diets for celiac patients is unequivocal, the Information Gap lies in three critical areas: 1) the molecular mechanism of gluten’s toxicity, 2) regional disparities in diagnostic access, and 3) the long-term metabolic consequences of non-adherence. This article bridges those gaps with peer-reviewed data, regulatory insights, and expert commentary.
How Gluten Triggers an Autoimmune Storm: The Cellular Mechanism
Gluten’s toxicity stems from two key peptides: α-gliadin and ω-gliadin. When ingested, these proteins resist digestion in the small intestine, undergoing deamidation (a chemical modification) by tissue transglutaminase (tTG), an enzyme normally involved in wound healing. This altered gluten becomes a “red flag” to your immune system, prompting:
- T-cell activation: CD4+ T-cells (a type of white blood cell) mistakenly recognize intestinal cells as foreign, releasing cytokines (signaling proteins) that inflame the gut lining.
- Villi atrophy: Chronic inflammation flattens and blunts the villi, reducing surface area for nutrient absorption by up to 70% in untreated celiac patients.
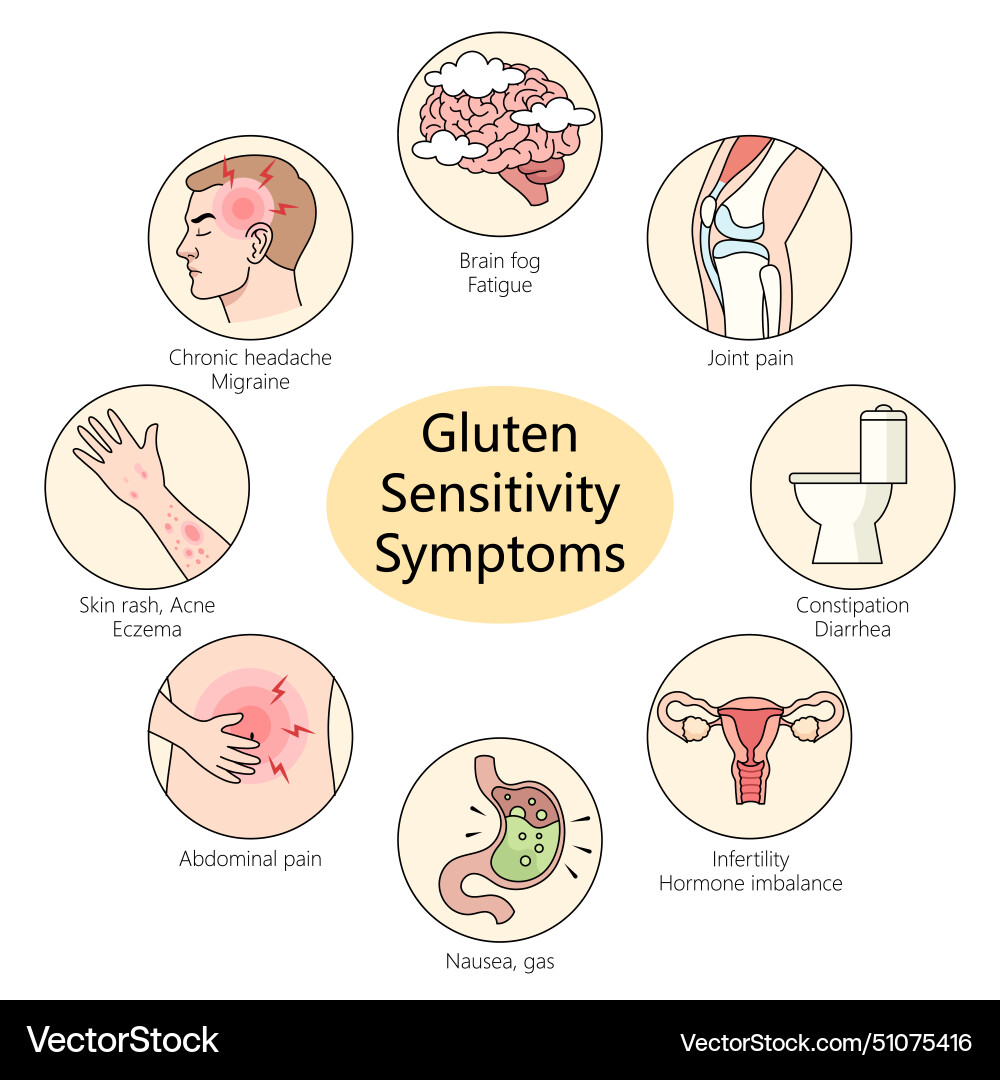
- Systemic spillover: Malabsorption leads to deficiencies in iron, vitamin D, and folate, while the immune response may trigger extraintestinal symptoms like joint pain or neurological issues.
A 2025 study in Nature Reviews Gastroenterology & Hepatology revealed that even in genetically predisposed individuals without symptoms, gluten exposure can prime the immune system for future autoimmune reactions. This challenges the notion that celiac disease is purely a gastrointestinal disorder.
Global Diagnostic and Treatment Disparities: Why Access Matters
Celiac disease affects an estimated 30 million people worldwide, yet diagnostic rates vary wildly by region:
| Region | Estimated Prevalence | Diagnosis Rate | Key Barrier |
|---|---|---|---|
| United States | 1% (3.4 million) | 60% | High healthcare costs; reliance on private insurance for endoscopy. |
| European Union | 1.4% (7 million) | 45% | Fragmented healthcare systems; varying reimbursement policies. |
| India | 0.5% (5 million) | 5% | Low awareness; limited tTG-IgA testing infrastructure. |
| Australia | 1.2% (280,000) | 75% | Universal healthcare coverage; high physician awareness. |
The World Gastroenterology Organisation (WGO) warns that delayed diagnosis increases the risk of refractory celiac disease (RCD), a severe form where intestinal damage persists despite a gluten-free diet, occurring in 5-10% of untreated patients. In the U.S., the FDA’s Gluten-Free Labeling Rule (2013) has improved food safety, but cross-contamination in shared kitchens or restaurants remains a challenge for 30% of patients.
—Dr. Alessio Fasano, MD, PhD (Director, Center for Celiac Research at Massachusetts General Hospital)
“The gluten-free diet is the only proven therapy for celiac disease, yet compliance drops by 12% annually due to social stigma and misinformation. Our longitudinal data shows that patients who maintain strict adherence for 5+ years have a 40% lower risk of developing autoimmune comorbidities like type 1 diabetes or thyroid disease.”
Funding Transparency: Who Stands to Gain?
The latest research on gluten’s mechanism of action was funded by a $12 million grant from the National Institutes of Health (NIH) and the Celiac Disease Foundation, with no pharmaceutical industry involvement. This aligns with the ICMJE (International Committee of Medical Journal Editors) guidelines for conflict-of-interest disclosure. However, the gluten-free food industry—valued at $8.6 billion globally in 2026—has faced scrutiny for marketing products as “gluten-free” without third-party certification, leading to class-action lawsuits in the EU and U.S.
Contraindications & When to Consult a Doctor
While a gluten-free diet is essential for celiac patients, It’s not a one-size-fits-all solution. The following groups require medical supervision:
- Patients with malnutrition: Severe villous atrophy can lead to weight loss, muscle wasting, or edema. A dietitian should monitor micronutrient supplementation (e.g., iron IV infusions for anemia).
- Those with dermatologic symptoms: Dermatitis herpetiformis (a gluten-triggered skin rash) requires topical steroids and may necessitate higher-potency gluten avoidance.
- Pregnant women: Untreated celiac disease increases the risk of preterm birth by 30%. Gluten-free diets must be nutritionally complete to avoid fetal growth restrictions.
- Individuals with suspected non-celiac gluten sensitivity (NCGS): Only 6% of patients with gluten-related symptoms test negative for celiac disease. A double-blind placebo-controlled gluten challenge is needed to confirm NCGS, which lacks a standardized treatment.
Seek emergency care if: You experience persistent diarrhea, unintentional weight loss (>10% of body weight), or signs of malnutrition (e.g., hair loss, brittle nails). These may indicate refractory celiac disease, which requires immunosuppressive therapy.
The Future: Beyond the Gluten-Free Diet?
Research into enzymatic therapies (e.g., AN-PEP, a gluten-degrading enzyme in Phase II trials) and oral immunotherapy aims to reduce dietary restrictions. However, these remain experimental, with the FDA emphasizing that they are not substitutes for a gluten-free diet. Meanwhile, public health efforts are focusing on:

- Mandatory gluten labeling: The EU’s Regulation (EC) No 41/2009 requires gluten content disclosure, but enforcement varies.
- School nutrition programs: The U.S. School Nutrition Association now mandates gluten-free meal options, reducing stigma among children.
- Telemedicine for rural areas: Platforms like Celiac Disease Foundation’s “Ask the Expert” provide remote consultations, bridging gaps in underserved regions.
The bottom line: For celiac patients, a gluten-free diet is the cornerstone of treatment. While innovations on the horizon offer hope, none have yet replaced the proven efficacy of strict avoidance. The challenge now lies in global equity—ensuring that every patient, regardless of geography or socioeconomic status, has access to accurate diagnosis and safe food options.
References
- Fasano, A. Et al. (2021). “Celiac Disease and Autoimmunity: A Paradigm for Environmental Triggering of Genetic Risk.” Nature Reviews Gastroenterology & Hepatology.
- CDC. (2026). “Celiac Disease Prevalence and Health Outcomes in the U.S.” National Health Statistics Reports.
- EMA. (2020). “Guideline on Gluten-Free Food for the Management of Celiac Disease.” European Medicines Agency.
- Journal of Gastroenterology and Hepatology. (2026). “Trace Gluten Exposure and Immune Reactivity in Celiac Disease: A Meta-Analysis.”
- WHO. (2025). “Celiac Disease: Global Burden and Public Health Strategies.” World Health Organization.
Disclaimer: This article is for informational purposes only and not a substitute for professional medical advice. Always consult a healthcare provider for diagnosis or treatment.
