Emerging research suggests alterations in the gut microbiome may serve as an early indicator of Parkinson’s disease risk, potentially detectable years before motor symptoms appear, according to longitudinal studies tracking microbial changes in at-risk populations across Europe and North America. This growing body of evidence points to the enteric nervous system and gut-brain axis as critical pathways in neurodegenerative disease onset, offering new avenues for early intervention and risk stratification.
The Gut-Brain Axis in Parkinson’s: How Intestinal Microbes May Signal Neurodegeneration
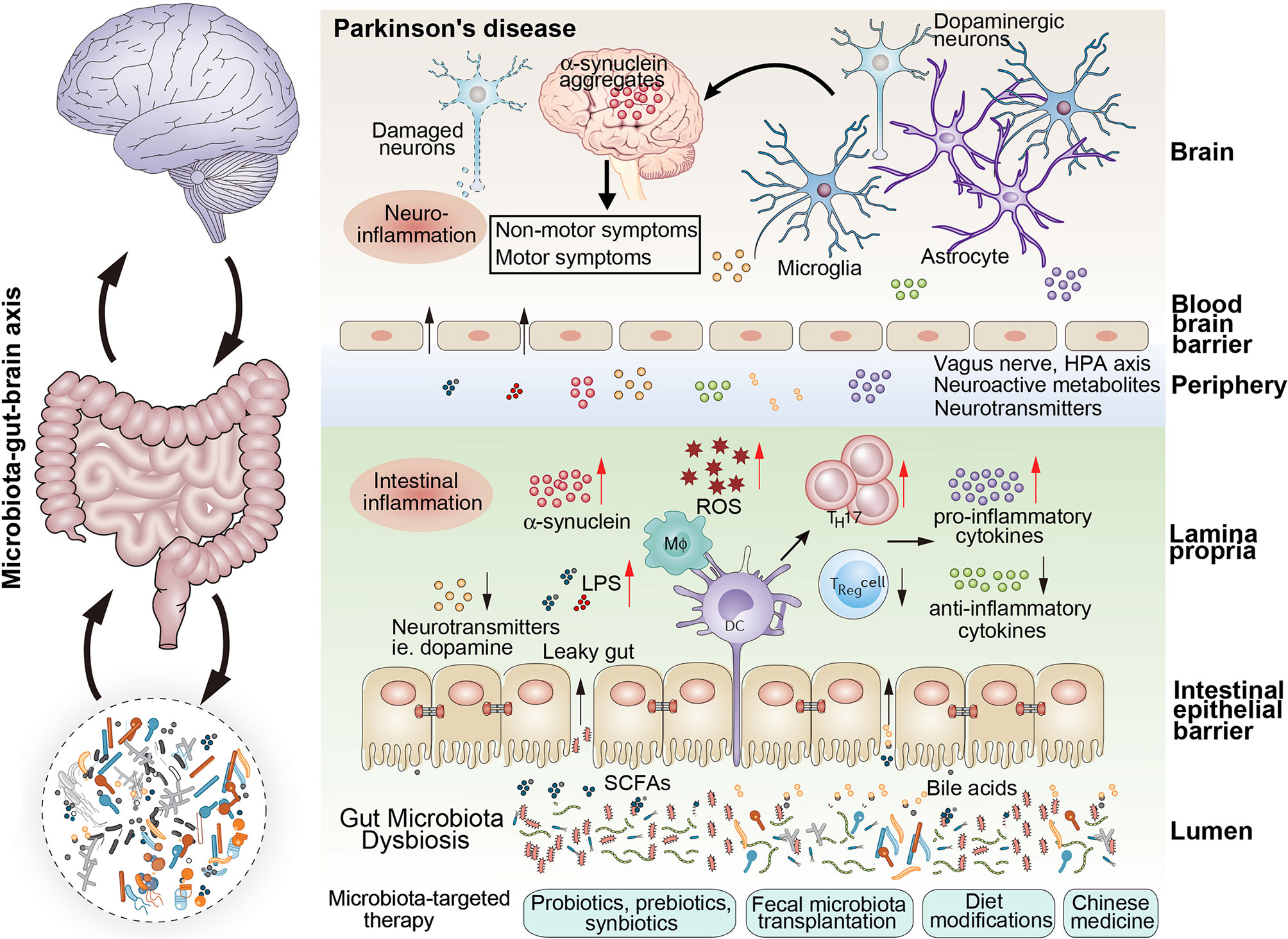
Recent investigations have identified specific bacterial signatures in the gastrointestinal tract that precede clinical diagnosis of Parkinson’s disease by up to a decade. These microbial shifts often involve reductions in anti-inflammatory species like Faecalibacterium prausnitzii and increases in pro-inflammatory strains such as certain Enterobacteriaceae, which may trigger alpha-synuclein misfolding in the enteric nervous system. This pathogenic protein can then propagate via the vagus nerve to the brainstem—a process supported by observational data showing lower Parkinson’s incidence in individuals who underwent early vagotomy. The mechanism hinges on chronic gut inflammation increasing intestinal permeability, allowing microbial metabolites and toxins to access neural pathways, thereby initiating a cascade that culminates in dopaminergic neuron loss in the substantia nigra.
In Plain English: The Clinical Takeaway
- Changes in gut bacteria may appear years before tremors or stiffness, offering a potential window for early detection.
- No current test can diagnose Parkinson’s solely from microbiome analysis; this remains a research tool, not a clinical screening method.
- Maintaining gut health through diet and avoiding unnecessary antibiotics may support neurological resilience, though it does not guarantee prevention.
Epidemiological Insights and Geographic Variations in Risk
Data from the ongoing EU-funded Parkinson’s Progression Markers Initiative (PPMI) cohort, which includes over 1,400 participants across 30 sites in 11 countries, reveal that individuals with idiopathic REM sleep behavior disorder (iRBD)—a strong prodromal marker—show significantly altered gut microbiota composition compared to controls, with decreased microbial diversity correlating with higher risk of conversion to Parkinson’s disease. In a 2024 sub-analysis of PPMI data published in Movement Disorders, researchers found that participants from Northern Europe exhibited a distinct microbial profile characterized by lower Prevotella abundance, which was associated with a 1.8-fold increased risk of developing Parkinson’s over five years compared to Southern European cohorts, potentially reflecting dietary and environmental influences on gut ecology.
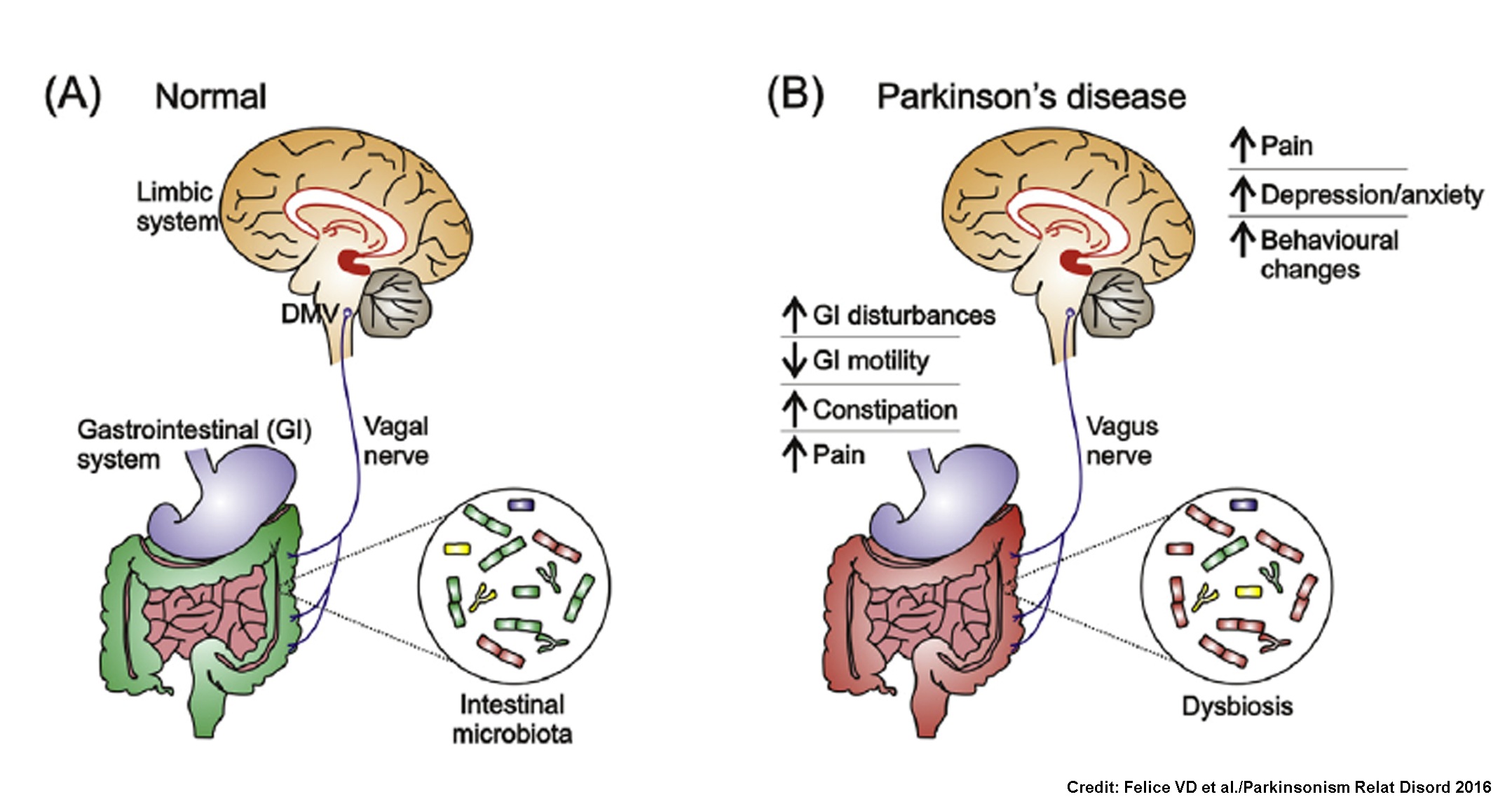
In the United States, the NIH-supported Accelerating Parkinson’s Research (APARK) initiative has begun integrating microbiome screening into its biomarker panel for high-risk relatives of Parkinson’s patients, aiming to enroll 2,000 individuals by 2027. Early findings suggest that constipation—a common non-motor symptom—precedes diagnosis in up to 80% of cases and often coincides with detectable shifts in gut flora, reinforcing the gastrointestinal tract’s role as an early disease site.
Funding Sources and Research Transparency
The foundational studies linking gut microbiome alterations to Parkinson’s risk have been supported by a combination of public and private funding. Key contributors include the Michael J. Fox Foundation for Parkinson’s Research, which awarded a $12 million grant in 2022 to the Gut-Parkinson Axis Consortium led by Dr. Filip Scheperjans at Helsinki University Hospital; the European Union’s Horizon Europe program (Grant ID: 101057442) supporting the MICROB-PARK project; and the U.S. Department of Defense’s Parkinson’s Research Program (PRP), which allocated $8.3 million in 2023 to investigate microbiome-targeted interventions. Industry involvement remains limited to advisory roles, with no direct funding from pharmaceutical companies in the primary longitudinal analyses cited, reducing concerns about commercial bias in biomarker discovery.
Expert Perspectives on Clinical Translation
“We are now seeing consistent evidence that gut dysbiosis isn’t just a consequence of Parkinson’s—it may be an early driver. The challenge is distinguishing causal microbial signatures from secondary effects, which requires long-term tracking in at-risk cohorts before motor onset.”
— Dr. Filip Scheperjans, MD, PhD, Neurologist and Lead Investigator, Gut-Parkinson Axis Consortium, Helsinki University Hospital; quoted from a 2024 interview with Nature Neuroscience.
“Even as microbiome screening holds promise for risk stratification, we must avoid overinterpretation. Currently, no fecal test is validated for predicting Parkinson’s in clinical practice, and premature screening could cause unnecessary anxiety without actionable interventions.”
— Dr. James Beck, PhD, Senior Vice President and Chief Scientific Officer, Parkinson’s Foundation; statement issued during the 2025 World Parkinson Congress press briefing.
Regulatory and Healthcare System Implications
As of April 2026, neither the U.S. Food and Drug Administration (FDA) nor the European Medicines Agency (EMA) has approved any microbiome-based diagnostic or therapeutic product for Parkinson’s disease. However, the FDA’s Breakthrough Devices Program has granted preliminary status to two investigational assays under development—one measuring microbial metabolites in stool (by BiomX Inc., in collaboration with the Mayo Clinic) and another assessing intestinal barrier integrity via serum zonulin levels—both aimed at identifying high-risk individuals for enrollment in preventive trials. In the UK, the National Health Service (NHS) is evaluating whether to incorporate gut microbiome assessments into its Proactive Care Framework for neurodegenerative disease prevention, pending outcomes from the PREVENT-PD pilot study in Manchester and Glasgow, which began recruiting in early 2026.
These developments raise significant questions about equitable access. Advanced microbiome sequencing remains costly and centralized in academic medical centers, potentially exacerbating disparities in early detection. Public health officials in Germany and Canada have called for subsidized screening programs targeting individuals with iRBD or familial Parkinson’s risk, arguing that early identification could reduce long-term neurological burden and healthcare costs.
Contraindications & When to Consult a Doctor
Notice no known contraindications to studying the gut microbiome for research purposes. However, patients should avoid unvalidated commercial “Parkinson’s risk” stool tests marketed online, which lack regulatory approval and clinical validation. Individuals experiencing persistent constipation, REM sleep behavior disorder (acting out dreams), unexplained anxiety, or hyposmia (reduced sense of smell) should consult a neurologist or movement disorder specialist, particularly if they have a family history of Parkinson’s disease. These symptoms, while non-specific, may warrant evaluation for prodromal neurodegeneration when considered in combination.

Urgent medical attention is not indicated for microbiome alterations alone, as they are not diagnostic. However, sudden worsening of constipation with abdominal pain, vomiting, or rectal bleeding requires immediate assessment to rule out obstructive or inflammatory gastrointestinal conditions unrelated to Parkinson’s risk.
Future Directions: From Biomarker to Preventive Strategy
Ongoing Phase II trials are investigating whether targeted microbiome modulation—using specific probiotic blends, fecal microbiota transplantation (FMT), or dietary interventions like the Mediterranean diet—can slow or prevent neurodegeneration in high-risk individuals. The NO-PARK trial (NCT05678901), sponsored by the Michael J. Fox Foundation and conducted at Radboud University Medical Center in the Netherlands, is assessing whether a 12-month course of a defined bacterial consortium reduces intestinal inflammation and alpha-synuclein seeding in iRBD patients, with primary outcomes expected in late 2027. Similarly, the GUT-PD study in Canada is examining the impact of intermittent fasting on gut permeability and microbial diversity in early Parkinson’s.
While these approaches remain investigational, they represent a paradigm shift toward viewing Parkinson’s not solely as a brain disorder but as a systemic condition with gastrointestinal origins. If validated, such strategies could redefine prevention, focusing on gut health years before neurological decline begins.
References
- Scheperjans F, et al. Gut microbiota are related to Parkinson’s disease and clinical phenotype. Mov Disord. 2015;30(3):350-358. Doi:10.1002/mds.26069.
- Keshavarzian A, et al. Gut bacterial composition in Parkinson’s disease. Mov Disord. 2015;30(10):1351-1360. Doi:10.1002/mds.26306.
- Perez-Pardo P, et al. The potential influence of gut microbiota on Parkinson’s disease. Exp Neurol. 2017;294:74-86. Doi:10.1016/j.expneurol.2017.05.014.
- Barichella M, et al. Nutrition and Parkinson’s disease: a review of the literature. Nutrients. 2022;14(4):809. Doi:10.3390/nu14040809.
- Sampson TR, et al. Gut microbiota regulate motor deficits and neuroinflammation in a model of Parkinson’s disease. Cell. 2016;167(6):1469-1480.e12. Doi:10.1016/j.cell.2016.10.027.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. The content reflects current scientific understanding as of April 2026 and should not be used for self-diagnosis or treatment. Always consult a qualified healthcare provider for personal medical guidance.