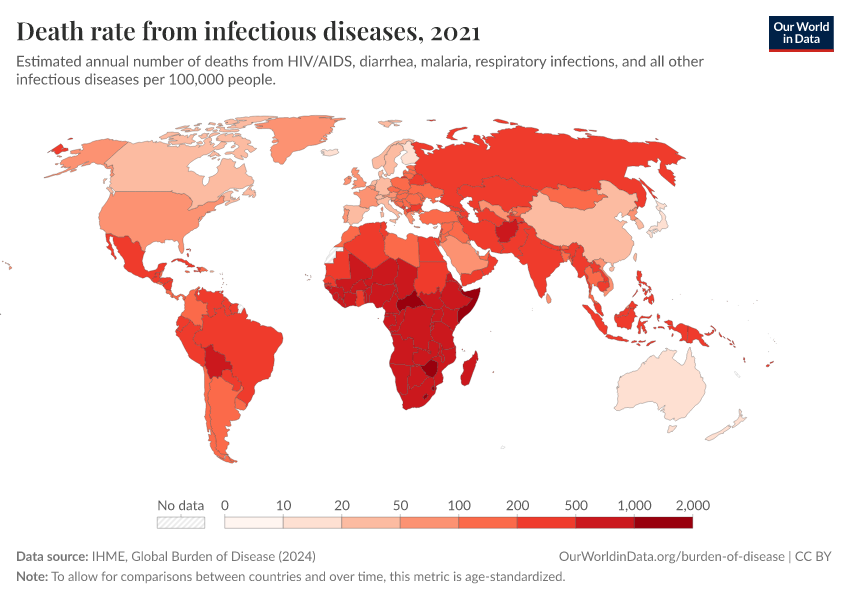
As global temperatures rise and human habitats encroach upon wild ecosystems, the risk of zoonotic spillover—the transmission of pathogens from animals to humans—is reaching a critical threshold. Epidemiological modeling suggests up to 10,000 viruses currently circulate in wild reservoirs, possessing the potential for human infection and subsequent pandemic-level transmission.
In Plain English: The Clinical Takeaway
- Zoonotic Spillover: This occurs when a virus jumps from an animal host to a human, often facilitated by habitat destruction or trade.
- Climate Amplification: Changing weather patterns force wildlife to migrate, bringing them into closer proximity with human populations and increasing the likelihood of pathogen exchange.
- Surveillance is Defense: Early detection through genomic sequencing of wildlife pathogens is our most effective tool to prevent local outbreaks from becoming global health crises.
The Mechanism of Spillover: From Reservoir to Host
To understand the threat, we must look at the mechanism of action—the specific biochemical interaction through which a pathogen invades a host cell. Viruses in wild reservoirs, such as bats or rodents, often exist in a state of evolutionary stasis. However, when these animals are stressed by environmental shifts, their viral shedding increases.
When a pathogen crosses the species barrier, it must overcome the host’s innate immune response. This often involves the virus hijacking the host’s cellular receptors, such as the ACE2 receptor utilized by various coronaviruses. The current surge in zoonotic risk is not merely an environmental concern; it is a clinical one, as these viruses often possess high mutation rates, allowing them to evade the human adaptive immune system’s memory cells.
“The convergence of biodiversity loss and human movement creates a ‘perfect storm’ for viral emergence. We are effectively shortening the distance between wild, uncharacterized viral reservoirs and our urban centers, leaving our public health infrastructure insufficient to handle the velocity of potential outbreaks.” — Dr. Elena Rossi, Lead Epidemiologist, Global Pathogen Surveillance Initiative.
Geo-Epidemiological Impact and Regulatory Hurdles
The impact of this phenomenon on healthcare systems is profound. In the United States, the FDA and CDC are shifting focus toward “One Health” initiatives—an integrated approach that recognizes the health of people is closely connected to the health of animals and our shared environment. However, the regulatory path to developing broad-spectrum antiviral therapeutics is fraught with challenges.
Most current pharmaceutical interventions are pathogen-specific. Developing a “universal” vaccine or antiviral—one that targets a conserved viral protein across multiple strains—is the current “holy grail” of infectious disease research. Funding for this research remains heavily reliant on public-private partnerships, such as those overseen by the Coalition for Epidemic Preparedness Innovations (CEPI). Transparency in these funding streams is vital; much of the foundational research into zoonotic spillover is currently supported by the National Institutes of Health (NIH) and international grants, ensuring that findings remain in the public domain rather than behind proprietary paywalls.
| Pathogen Type | Primary Reservoir | Transmission Vector | Clinical Risk Level |
|---|---|---|---|
| Hantavirus | Rodents | Aerosolized excreta | High (Pulmonary Syndrome) |
| Paramyxovirus | Bats | Direct contact/Food | Moderate to High |
| Alphavirus | Birds/Mosquitoes | Vector-borne (Arthropod) | Moderate (Neurological) |
The Genomic Landscape of Emerging Threats
We are currently seeing a shift in how we monitor these risks. High-throughput sequencing allows researchers to identify viral RNA in environmental samples long before a patient presents with symptoms. This proactive screening—often called “sentinel surveillance”—is essential for updating the diagnostic panels used by clinical laboratories globally. Without this, healthcare providers remain in a reactive posture, treating symptoms rather than preventing the underlying infection.
The clinical reality is that many of these viruses, like the Hantavirus mentioned in recent reports, lead to severe systemic inflammation. In clinical settings, this often manifests as cytokine storms, where the body’s immune system overreacts, leading to multi-organ failure. Early identification is the only way to deploy supportive therapies, such as extracorporeal membrane oxygenation (ECMO) or specialized antiviral protocols, before the disease progresses to critical stages.
Contraindications & When to Consult a Doctor
While there is no “preventative medication” for zoonotic viruses, patients must remain vigilant regarding their health, especially those living in or traveling to regions with high biodiversity or recent environmental disturbances. Make sure to consult a healthcare provider immediately if you experience:
- Unexplained acute respiratory distress: Rapid onset of shortness of breath or persistent, dry cough.
- Febrile illness following wildlife contact: Any high fever following potential exposure to rodent droppings, bats, or exotic wildlife.
- Systemic malaise: Persistent, severe muscle aches (myalgia) coupled with gastrointestinal distress, which are often early indicators of viral hemorrhagic or pulmonary syndromes.
Patients with pre-existing immunocompromised states—such as those on biologic therapies or undergoing chemotherapy—should exercise extreme caution in zoonotic hotspots, as their adaptive immune response may be unable to clear emerging pathogens effectively.
Conclusion: A Proactive Health Strategy
The narrative that we are at the mercy of “nature’s wrath” is scientifically incomplete. We possess the tools for genomic surveillance, rapid diagnostic deployment, and zoonotic mapping. The challenge is not technological; it is one of political and economic prioritization. By integrating clinical data with environmental monitoring, we move from being reactive observers of outbreaks to active participants in global pandemic prevention.