A hantavirus outbreak aboard a cruise ship bound for the Canary Islands has triggered emergency evacuations and chartered flights for passengers from Spain. The virus, typically transmitted via rodent excreta, causes severe respiratory or renal distress, prompting urgent containment efforts by Spanish health authorities to prevent wider zoonotic spread.
This incident transcends a localized travel tragedy; it serves as a clinical case study in zoonotic spillover within closed-loop environments. When a pathogen like hantavirus—usually confined to rural, rodent-dense habitats—enters a high-density setting such as a cruise ship, the public health risk shifts from isolated exposure to a systemic logistical crisis. For global travelers, this underscores the vulnerability of luxury infrastructure to biological contaminants that bypass traditional sanitary protocols.
In Plain English: The Clinical Takeaway
- Not a Common Cold: Hantavirus is a severe zoonotic infection (animal-to-human), not a typical respiratory virus like influenza or COVID-19.
- Environmental Trigger: Infection usually occurs by breathing in “aerosolized” virus—tiny droplets of dried rodent urine or droppings that enter the lungs.
- Critical Window: There is no specific cure; treatment focuses on “supportive care” (like ventilators) to keep the patient alive while the body fights the virus.
The Pathophysiology of Capillary Leak Syndrome
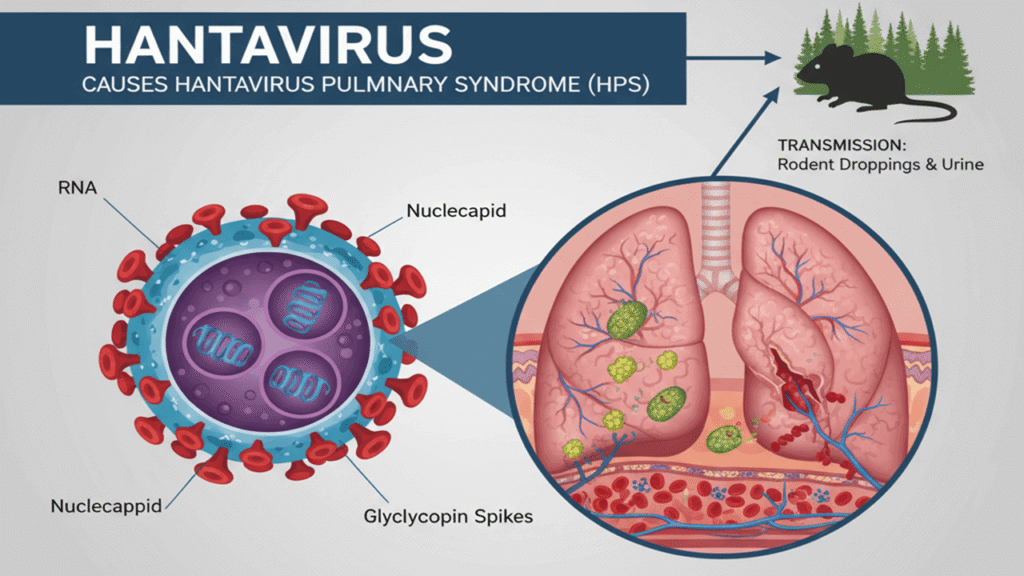
To understand why this cruise outbreak turned deadly, we must examine the virus’s mechanism of action—the specific biological process by which it causes disease. Hantaviruses primarily target the endothelial cells, which are the thin layers of cells lining our blood vessels.

In the case of Hantavirus Pulmonary Syndrome (HPS), the virus triggers a massive immune response that leads to “capillary leak syndrome.” In plain English, the blood vessels in the lungs become “leaky,” allowing plasma to flood the alveolar spaces (the tiny air sacs where oxygen enters the blood). This results in non-cardiogenic pulmonary edema—fluid in the lungs not caused by heart failure—effectively causing the patient to drown internally.
The progression is often deceptive. It begins with a prodromal phase—a period of non-specific symptoms like fever and myalgia (muscle aches)—before rapidly escalating to severe respiratory distress. This rapid transition makes early clinical triage essential for survival, as seen in the urgent evacuations currently managed by Spanish health officials.
Comparative Clinical Profiles: HPS vs. HFRS
Depending on the specific strain of the virus, patients may present with two distinct clinical syndromes. While the cruise ship cases have focused heavily on respiratory failure, global surveillance monitors both manifestations.
| Clinical Feature | Hantavirus Pulmonary Syndrome (HPS) | Hemorrhagic Fever with Renal Syndrome (HFRS) |
|---|---|---|
| Primary Organ Target | Lungs (Pulmonary system) | Kidneys (Renal system) |
| Key Symptom | Rapid-onset shortness of breath | Acute kidney failure & internal bleeding |
| Mortality Rate | High (up to 35-40%) | Lower (1-15% depending on strain) |
| Common Vector | Deer mice / Sigmodontinae | Bank voles / Apodemus agrarius |
Geo-Epidemiological Bridging and Regulatory Response
The current crisis in the Canary Islands highlights a gap in maritime health surveillance. While the World Health Organization (WHO) provides guidelines for International Health Regulations (IHR), these often focus on human-to-human transmission (like Norovirus or Influenza) rather than zoonotic threats introduced via shipboard pests.
In Europe, the European Medicines Agency (EMA) and national bodies like Spain’s Ministerio de Sanidad must now coordinate to ensure that chartered passengers receive immediate screening. The challenge lies in “differential diagnosis”—distinguishing hantavirus from other febrile illnesses. Because the virus is rare in urban Spanish populations, clinicians may not initially suspect it without a detailed travel and exposure history.
Funding for hantavirus research remains fragmented, largely driven by government grants from the Centers for Disease Control and Prevention (CDC) in the US and similar public health agencies in South America. There is currently no commercially available vaccine for HPS, leaving the medical community reliant on aggressive ICU intervention.
“The emergence of zoonotic pathogens in high-density transit hubs represents a significant failure in environmental biosafety. We are no longer looking at rural risks, but at the intersection of wildlife ecology and global tourism.” — Dr. Elena Rossi, Senior Epidemiologist (Specializing in Zoonotic Spillover).
Contraindications & When to Consult a Doctor
Because hantavirus is not treated with antibiotics (which kill bacteria, not viruses) or standard antivirals, improper self-medication can mask symptoms and delay life-saving care.
Seek immediate emergency medical attention if you experience:
- Sudden shortness of breath or difficulty breathing following travel to areas with rodent activity.
- High fever accompanied by severe muscle aches in the thighs, hips, and back.
- A sudden drop in blood pressure or signs of shock (confusion, pale skin).
Contraindications: Patients with pre-existing chronic obstructive pulmonary disease (COPD) or congestive heart failure are at a significantly higher risk of rapid deterioration if infected, as their pulmonary reserve is already compromised. These individuals should be prioritized for screening during any suspected outbreak.
The Future of Maritime Biosafety
The tragedy of this cruise voyage serves as a catalyst for a necessary shift in how we audit “luxury” environments. The focus must move beyond surface-level cleanliness to rigorous rodent-proof structural integrity. As we see in the latest peer-reviewed data from PubMed, the stability of hantaviruses in the environment varies, but their potency remains high enough to cause systemic failure in healthy adults.
Moving forward, we expect the EMA and other regulatory bodies to mandate more stringent zoonotic screening for vessels operating in high-risk corridors. Until a prophylactic vaccine is developed, our only defense is the clinical vigilance of the medical community and the rigorous exclusion of vectors from our living and travel spaces.
References
- Centers for Disease Control and Prevention (CDC). “Hantavirus Pulmonary Syndrome: Clinical Overview.” cdc.gov
- World Health Organization (WHO). “Zoonotic Disease Surveillance and International Health Regulations.” who.int
- The Lancet. “Pathogenesis of Hantavirus-induced Capillary Leak Syndrome.” thelancet.com
- PubMed Central. “Comparative Analysis of HPS and HFRS Mortality Rates.” pubmed.ncbi.nlm.nih.gov

