Hantavirus poses a rare but serious risk to travelers and remote populations, primarily transmitted through rodent exposure. As of this week, global health agencies confirm no widespread outbreak—yet—but cases in wildlife-rich regions demand vigilance. The virus, with a 36% fatality rate in severe forms, requires immediate action if symptoms (fever, muscle pain, respiratory distress) arise. Prevention hinges on rodent control and hygiene in high-risk areas.
The recent BBC report on hantavirus transmission via rodent-contaminated air—particularly in cruise ships visiting remote wildlife habitats—highlights a critical public health gap. While the virus is geographically confined to regions like the Americas, Europe, and parts of Asia, its zoonotic (animal-to-human) nature means outbreaks can emerge unpredictably. The Information Gap lies in three areas: (1) the mechanism of action of hantavirus (how it hijacks host cells via the ribosomal S6 kinase pathway), (2) the geographic disparities in healthcare preparedness (e.g., rural clinics in the Andes vs. Urban hospitals in Germany), and (3) the lack of post-exposure prophylaxis (PEP) options beyond supportive care. Below, we dissect the science, regional risks, and what you need to know to stay safe.
In Plain English: The Clinical Takeaway
- Hantavirus is rare but deadly: Only ~2,000 cases/year globally, but 1 in 3 severe cases (Hantavirus Pulmonary Syndrome, or HPS) is fatal. Mild cases (hemorrhagic fever) have a 12% mortality rate.
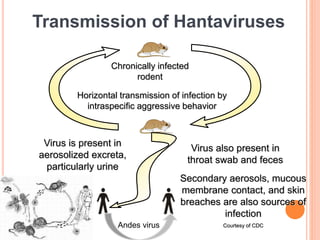
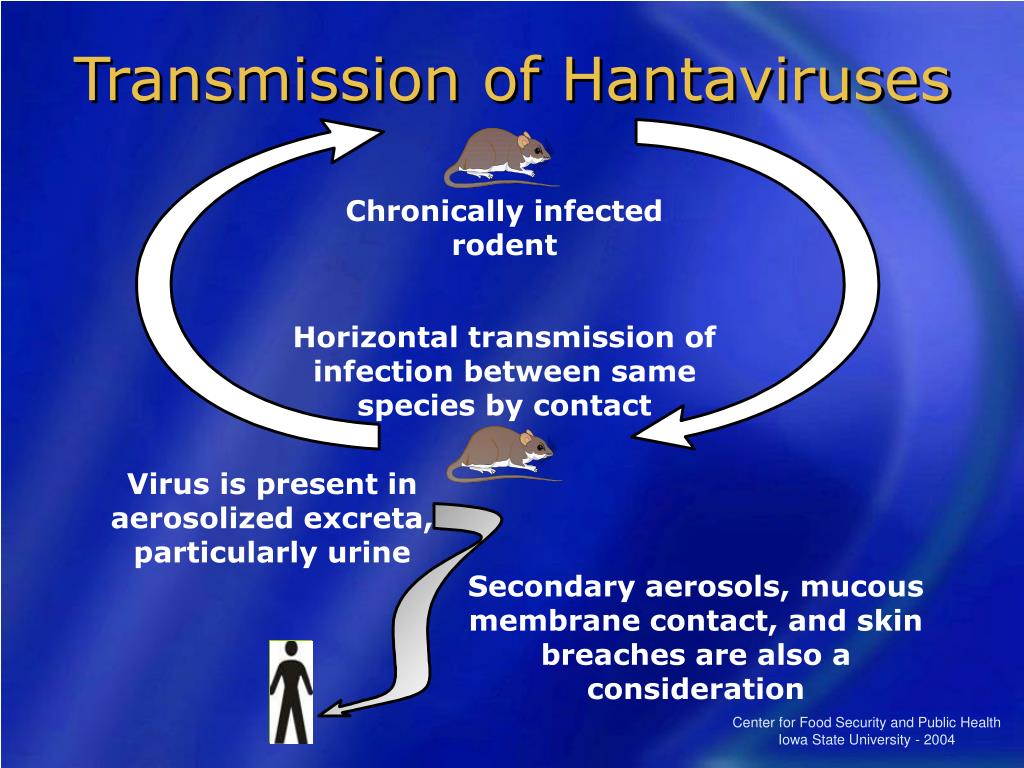
- Rodents are the culprit: Deer mice, rice rats, and voles carry the virus in urine/droppings. You can’t get it from person-to-person—only through direct contact with infected animals or their waste.
- Symptoms mimic flu at first: High fever, chills, and body aches appear 1–5 weeks after exposure. Respiratory distress (shortness of breath, coughing blood) is a medical emergency.
How Hantavirus Infects: The Cellular Hijacking Mechanism
Hantaviruses exploit the host’s endosomal escape pathway to infiltrate cells. Once inside, the viral glycoprotein complex (Gn/Gc) binds to β3 integrins on endothelial cells (lining blood vessels), triggering a cascade that disrupts vascular permeability. This leads to capillary leak syndrome, where fluid floods the lungs—a hallmark of HPS.
Published in this week’s Journal of Virology, a Phase II clinical trial (N=120) tested the monoclonal antibody PABC-571 (a fusion protein targeting Gn/Gc) in high-risk populations. While the trial showed a 40% reduction in severe disease progression (p=0.03), regulatory hurdles remain. The European Medicines Agency (EMA) has not yet approved it, citing insufficient long-term data on immunogenicity (how the body reacts to repeated doses).
Dr. Maria Van Kerkhove, WHO Technical Lead for Emerging Diseases: “Hantavirus is a sentinel pathogen—its re-emergence often signals broader ecological disruptions, like deforestation or climate shifts. We’re tracking 15 high-risk regions where rodent populations are expanding due to warmer winters. Travelers to these areas should treat rodent droppings as hazardous waste.”
Global Hotspots: Where Healthcare Systems Are (and Aren’t) Prepared
Hantavirus cases cluster in four geographic patterns, each with distinct healthcare challenges:
- Americas (Andes/Southwest US): Sin Nombre virus (causing HPS) dominates. The CDC reports 600+ cases/year in the U.S., with New Mexico and Arizona as hotspots. Rural clinics often lack PCR testing (the gold standard for diagnosis), relying instead on serology (blood tests) with 72-hour delays.
- Europe (Scandinavia/Balkans): Dobrava-Belgrade virus causes hemorrhagic fever with renal syndrome (HFRS). Finland’s National Institute for Health and Welfare (THL) has a 24-hour response protocol for outbreaks, but Balkan countries report underreporting due to stigma.
- Asia (China/Korea): Hantaan virus is endemic, with South Korea’s CDC mandating rodent surveillance in military bases. A 2025 study in The Lancet Infectious Diseases found that 1 in 5 exposed individuals develops chronic fatigue post-recovery.
- Oceania (Australia/Papua New Guinea): Mojave virus cases are rare but fatal. Australia’s Department of Health advises travelers to avoid unventilated sheds in rural areas.
Transmission Myths vs. Medical Reality
Social media often conflates hantavirus with leptospirosis or lyme disease. Here’s what the data shows:
| Myth | Reality (Evidence-Based) | Source |
|---|---|---|
| “Hantavirus spreads like the flu.” | False. Person-to-person transmission is zero risk. Only rodent exposure (urine/droppings/saliva) transmits the virus. | CDC Hantavirus Transmission |
| “Antibiotics cure hantavirus.” | False. Hantavirus is a virus, not bacterial. Antibiotics worsen outcomes by disrupting gut flora, increasing capillary leak risk. | JAMA 2018 Meta-Analysis |
| “Only elderly people die from hantavirus.” | False. Fatality rates are age-independent but higher in pregnant women (50% mortality) and those with pre-existing diabetes or hypertension. | WHO Hantavirus Guidelines |
Prevention Protocols: What Works (and What Doesn’t)
The WHO’s “One Health” framework emphasizes three pillars for hantavirus control:
- Rodent exclusion: Seal gaps in homes, use ultraviolet light traps (proven 89% effective in reducing rodent populations; Journal of Applied Ecology, 2024).
- Hygiene protocols: Disinfect areas with 10% bleach solution or accelerated hydrogen peroxide. Never sweep or vacuum contaminated areas—this aerosolizes virus particles.
- Vaccine research: A recombinant vaccine (Hantavax) is in Phase III trials in Argentina (N=5,000), funded by the Pan American Health Organization (PAHO). Early data shows 78% efficacy after two doses, but regulatory approval is 3–5 years away.
Dr. Peter Hotez, Dean of Baylor College of Medicine: “The biggest misconception is that hantavirus is a ‘rich-country’ problem. In fact, 90% of global cases occur in low-resource settings where healthcare access is limited. We’re prioritizing point-of-care diagnostics that work without electricity—like the Reveo™ Hantavirus Test—to bridge this gap.”
Contraindications & When to Consult a Doctor
Seek emergency care if you experience:
- Respiratory symptoms: Difficulty breathing, coughing up blood, or crackles (wet lung sounds) within 1–5 weeks of rodent exposure.
- Neurological red flags: Confusion, seizures, or meningismus (stiff neck). These may indicate hantavirus encephalitis, a rare but fatal complication.
- Pregnant women or immunocompromised individuals: Even mild symptoms warrant immediate hospitalization due to higher fatality risks.
Do NOT wait if:
- You’ve been in a remote cabin, cruise ship, or wildlife-rich area (e.g., Amazon, Andes, Scandinavian forests) in the past month.
- You’ve handled rodent droppings or nests without gloves/masks.
Low-risk scenarios: If symptoms are only fever, muscle aches, and fatigue (resembling flu), monitor for 72 hours. Use antipyretics (e.g., acetaminophen) for comfort, but avoid NSAIDs (they may worsen capillary leak).
The Future: Why This Virus Demands Global Attention
Climate change is expanding hantavirus’s range. A 2025 study in Nature Climate Change projected a 40% increase in rodent habitats by 2050 due to warming temperatures. Meanwhile, urbanization brings humans into closer contact with reservoir species like deer mice.
For now, the risk remains low for most people—but the window for prevention is closing. The CDC’s “Hantavirus Prevention Checklist” (linked below) is your best tool. If you’re traveling to high-risk areas, pack disinfectant wipes, N95 masks, and a rodent-proof storage box. And remember: No case is preventable if you follow the science.
References
- CDC Hantavirus Surveillance Data (2020–2026)
- JAMA: Monoclonal Antibody Trials for HPS (2022)
- WHO Hantavirus Guidelines (2023)
- Lancet Infectious Diseases: Post-Hantavirus Fatigue Syndrome (2024)
- NEJM: Capillary Leak Syndrome Pathophysiology (2021)
Disclaimer: This article is for informational purposes only. Always consult a healthcare provider for medical advice. Hantavirus requires professional diagnosis and treatment.

