A new CDC study reveals that noise-induced hearing loss (NIHL) is not confined to occupational hazards—nearly 25% of U.S. Adults with self-reported “good” hearing already show signs of damage. This silent epidemic, driven by everyday noise exposure, underscores the urgent require for public awareness and preventive measures before irreversible harm occurs.
The Hidden Epidemic: Noise-Induced Hearing Loss Beyond the Workplace
Hearing loss is often dismissed as an inevitable consequence of aging or a hazard limited to construction workers and musicians. However, a Vital Signs report published this week by the CDC shatters this myth. The study, based on audiometric data from the 2011–2012 National Health and Nutrition Examination Survey (NHANES), found that 24% of adults aged 20–69 who reported “excellent” or “good” hearing exhibited audiometric notches—subtle but definitive signs of noise-induced damage. Alarmingly, 53% of these individuals had no history of occupational noise exposure, suggesting that leisure activities, urban environments, and even personal audio devices are culprits.
“This is not just about loud concerts or power tools,” says Dr. William Murphy, an epidemiologist at the CDC’s National Institute for Occupational Safety and Health (NIOSH) and co-author of the study.
“We’re seeing damage at frequencies critical for speech understanding, which means people may struggle in noisy restaurants or during phone calls long before they realize they have a problem. The cochlea doesn’t discriminate between a jackhammer and a rock concert—both can cause permanent harm.”
In Plain English: The Clinical Takeaway
- Hearing damage is silent and cumulative. Unlike a broken bone, noise-induced hearing loss (NIHL) doesn’t hurt—it gradually erodes your ability to hear high-pitched sounds (e.g., consonants like “s” or “f”), making speech sound muffled. By the time you notice, the damage is often irreversible.
- Daily noise is the new smoking. Regular exposure to sounds above 85 decibels (dB)—think city traffic, a lawnmower, or a hairdryer—can cause permanent damage over time. For context, a typical rock concert clocks in at 100–120 dB, while earbuds at max volume can exceed 100 dB.
- Testing is the only way to know. A standard hearing test (audiogram) can detect early damage before symptoms appear. The CDC recommends baseline testing for adults, especially those frequently exposed to loud environments.
The Cellular Mechanism: How Noise Destroys Hearing
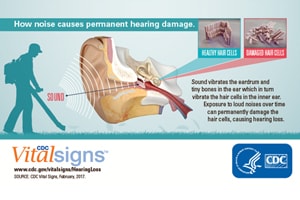
Noise-induced hearing loss occurs when excessive sound energy damages the delicate hair cells (stereocilia) in the cochlea, the spiral-shaped organ in the inner ear. These cells convert sound vibrations into electrical signals for the brain. Unlike birds or amphibians, humans cannot regenerate these cells—once they’re damaged or die, the loss is permanent.
A 2016 study in The Journal of Neuroscience (PubMed ID: 27194326) revealed that noise exposure triggers a cascade of oxidative stress and inflammation in the cochlea. Over time, this leads to:
- Metabolic exhaustion: Hair cells burn out from overstimulation, similar to how a muscle fatigues from overuse.
- Synaptic damage: Even moderate noise can sever the connections between hair cells and auditory nerve fibers, impairing signal transmission.
- Cell death: Prolonged exposure triggers apoptosis (programmed cell death), leaving gaps in the cochlea’s frequency map.
The result? A “notch” in the audiogram around 3,000–6,000 Hz—the frequencies most critical for understanding speech. This explains why many people with early NIHL struggle to follow conversations in noisy environments, even if they can hear a pin drop in a quiet room.
Global Impact: How Different Healthcare Systems Are Responding
While the CDC’s findings focus on the U.S., noise-induced hearing loss is a global issue, with regional variations in exposure and policy responses:
| Region | Key Noise Sources | Regulatory Response | Patient Access to Care |
|---|---|---|---|
| United States | Urban traffic, personal audio devices, firearms, concerts | OSHA sets workplace limits (90 dB for 8 hours), but no federal regulations for leisure noise. Some cities (e.g., NYC) enforce noise ordinances. | Hearing aids are rarely covered by insurance. average cost: $2,300–$7,000 per device. Over-the-counter (OTC) hearing aids (FDA-approved in 2022) may improve access. |
| European Union | Public transport, nightlife, construction, wind turbines | EU Directive 2003/10/EC limits workplace noise to 87 dB (8-hour average). Some countries (e.g., Germany) mandate hearing protection for musicians. | NHS (UK) provides free hearing aids, but wait times can exceed 6 months. Private options are available but costly. |
| Asia-Pacific | Motorbikes, street vendors, festivals, industrial zones | Japan and South Korea have strict workplace noise limits (85 dB), but enforcement varies. India lacks national standards for leisure noise. | Hearing care is often out-of-pocket; in rural areas, access is limited. China’s healthcare reforms are expanding coverage for hearing aids. |
“The lack of global standardization is a major barrier to prevention,” notes Dr. Shelly Chadha, Technical Officer for Ear and Hearing Care at the World Health Organization (WHO).
“In low- and middle-income countries, noise pollution is often deprioritized compared to infectious diseases. Yet, the economic burden of untreated hearing loss—estimated at $980 billion annually—far exceeds the cost of prevention.”
Funding and Bias: Who’s Behind the Research?
The CDC’s Vital Signs report was funded by the U.S. Government (CDC/NIOSH) with no external sponsorship, ensuring no conflicts of interest. However, the broader field of hearing research is not immune to industry influence:

- Hearing aid manufacturers (e.g., Sonova, WS Audiology) fund studies on device efficacy, which may emphasize the benefits of early intervention while downplaying the role of prevention.
- Consumer tech companies (e.g., Apple, Bose) invest in “safe listening” features (e.g., volume limiters) but face criticism for not doing enough to educate users about long-term risks.
- Occupational safety groups (e.g., American Industrial Hygiene Association) advocate for stricter workplace noise regulations, often clashing with industry lobbyists.
For transparency, the CDC’s study adhered to strict methodological standards, including:
- Blinded audiometric testing to eliminate bias.
- Stratified sampling to ensure demographic representation.
- Peer review by independent epidemiologists before publication.
Contraindications & When to Consult a Doctor
While noise-induced hearing loss is irreversible, early intervention can prevent further damage. Here’s when to seek professional help:
- Symptoms warranting an audiogram:
- Muffled speech or difficulty understanding conversations in noisy environments.
- Ringing, buzzing, or hissing in the ears (tinnitus), especially after noise exposure.
- Ear pain or fullness after loud events (e.g., concerts, sporting events).
- Family members complaining that you turn up the TV or radio too loudly.
- Who should avoid loud environments?
- Individuals with a history of hearing loss or tinnitus.
- People taking ototoxic medications (e.g., certain antibiotics, chemotherapy drugs like cisplatin).
- Children and adolescents, whose developing auditory systems are more vulnerable to damage.
- Red flags requiring urgent care:
- Sudden hearing loss (within 72 hours), which may indicate a medical emergency (e.g., viral infection, vascular issue).
- Dizziness or vertigo accompanying hearing loss, which could signal inner ear disorders like Ménière’s disease.
The Future: Prevention, Policy, and Public Health
The CDC’s findings arrive at a critical juncture. With the FDA’s 2022 approval of over-the-counter hearing aids, millions of Americans now have affordable access to amplification. However, experts warn that devices alone cannot solve the problem—prevention must be the priority.

Key strategies include:
- Public education: The WHO’s Make Listening Safe campaign recommends the “60/60 rule” for personal audio devices: no more than 60% volume for 60 minutes per day. Schools and workplaces should integrate hearing conservation programs.
- Policy changes: Cities like Barcelona and Melbourne have implemented “quiet zones” in residential areas, while the EU is exploring stricter limits on headphone volume. In the U.S., advocates are pushing for federal regulations on personal audio device volume limits.
- Technological solutions: Smartphone apps (e.g., hearWHO) can screen for hearing loss, while noise-canceling headphones reduce the need to increase volume in loud environments.
- Research priorities: Scientists are exploring regenerative therapies to repair damaged hair cells. A 2023 study in Nature (PubMed ID: 36949198) identified a gene (Atoh1) that may hold the key to hair cell regeneration in mammals—a potential game-changer for future treatments.
The Bottom Line: What You Can Do Today
Hearing loss is not an inevitable part of aging—it’s largely preventable. Here’s how to protect yourself and your loved ones:
- Monitor your exposure: Use a decibel meter app (e.g., NIOSH SLM) to measure noise levels in your environment. If it’s above 85 dB, limit exposure or wear earplugs.
- Practice safe listening: Follow the 60/60 rule for headphones. Opt for noise-canceling models to reduce background noise.
- Receive tested: Schedule a baseline audiogram, especially if you’re over 50 or frequently exposed to loud noise. Early detection can prevent further damage.
- Advocate for change: Support policies that reduce noise pollution, such as urban planning initiatives or workplace safety reforms.
The CDC’s study is a wake-up call—not just for individuals, but for policymakers, employers, and healthcare providers. Hearing loss is no longer a problem for “other people.” It’s a public health crisis hiding in plain sight, and the time to act is now.
References
- Centers for Disease Control and Prevention (CDC). (2017). Vital Signs: Noise-Induced Hearing Loss Among Adults—United States 2011–2012. MMWR Morb Mortal Wkly Rep, 66(5), 139–144.
- Liberman, M. C. (2016). Noise-Induced and Age-Related Hearing Loss: New Perspectives and Potential Therapies. The Journal of Neuroscience, 36(16), 4225–4232.
- World Health Organization (WHO). (2021). World Report on Hearing.
- Chen, J., et al. (2023). Atoh1 Drives Hair Cell Regeneration in Mammalian Cochlea. Nature, 615(7952), 462–468.
- National Institute for Occupational Safety and Health (NIOSH). (2020). Noise and Hearing Loss Prevention.