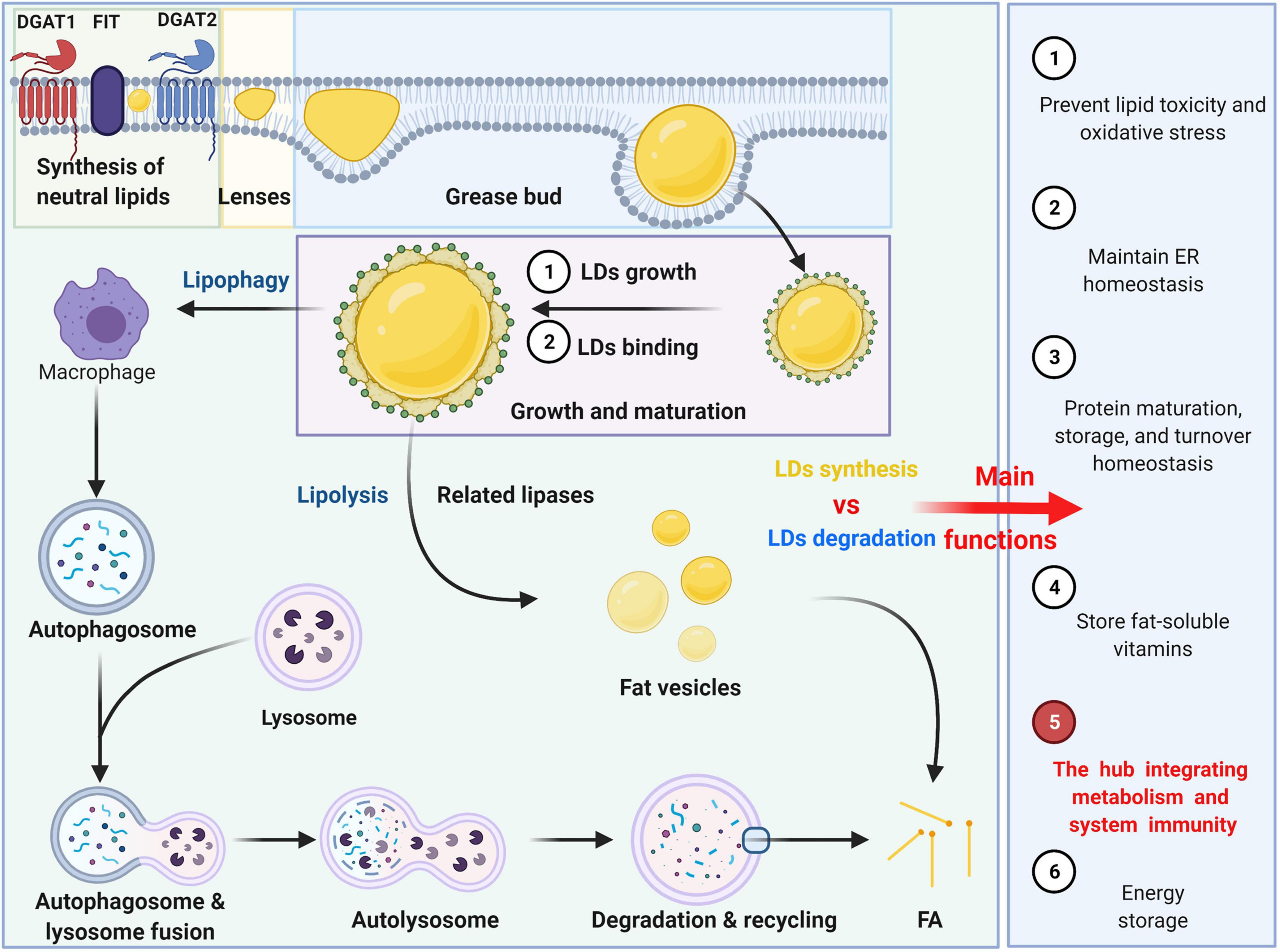
Researchers have identified a critical metabolic mechanism where leukemia cells accelerate lipid synthesis to fuel their own rapid growth. By hijacking fatty acid production pathways, these malignant cells create a sustainable energy source and structural components, offering a new potential target for precision therapies to starve cancer cells.
This discovery represents a paradigm shift in how we perceive the “fuel” for hematologic malignancies. For decades, the focus was primarily on glucose metabolism—the so-called Warburg Effect. However, we now understand that leukemia cells are not just sugar-hungry; they are lipid-dependent. By uncovering the specific enzymes and pathways that allow these cells to synthesize fats internally, scientists are opening the door to a new class of metabolic inhibitors that could potentially bypass the drug resistance seen in traditional chemotherapy.
In Plain English: The Clinical Takeaway
- The Discovery: Leukemia cells act like “fat factories,” creating their own lipids to build cell membranes and store energy for rapid division.
- The Potential: If One can block these “fat factories” with specific drugs, we can effectively starve the cancer cells without harming healthy blood cells.
- The Future: This moves us closer to “metabolic therapy,” where the goal is to disrupt the cancer’s food supply rather than just attacking its DNA.
The Molecular Machinery: How Leukemia Hijacks Lipid Synthesis
The core of this mechanism lies in the upregulation of de novo lipogenesis—the process of creating fatty acids from non-lipid precursors. In healthy cells, this process is tightly regulated. In leukemia, however, the cells overexpress key enzymes such as Fatty Acid Synthase (FASN), which acts as the primary assembly line for these fats.

The mechanism of action (the specific biochemical process through which a drug or biological process produces a result) involves the conversion of acetyl-CoA into long-chain fatty acids. These lipids are not merely for energy; they are integrated into the phospholipid bilayer of the cell membrane. This allows the leukemia cell to maintain structural integrity while dividing at an exponential rate, effectively building its own “housing” as it expands.
these cells utilize a process called “remodeling,” where they modify existing lipids to evade the immune system. By altering the composition of their outer membrane, leukemia cells can hide from T-cells, the “soldiers” of the immune system, making the cancer essentially invisible to the body’s natural defenses.
Global Regulatory Landscape and Patient Access
While this research is groundbreaking, the transition from bench to bedside involves rigorous regulatory hurdles. In the United States, the FDA (Food and Drug Administration) requires these metabolic inhibitors to undergo a three-phase clinical trial process to ensure they do not cause systemic lipid imbalances in patients.
In Europe, the EMA (European Medicines Agency) is closely monitoring the development of FASN inhibitors. The primary challenge for regional healthcare systems, such as the NHS in the UK, will be the cost of these precision medicines. Because these therapies target specific metabolic signatures, they are often priced as “orphan drugs” or specialized biologics, which can limit initial patient access.
The funding for much of this foundational research typically stems from government grants (such as the NIH in the US or the NRF in South Korea) and non-profit organizations like the Leukemia & Lymphoma Society. This ensures that the early-stage discovery is driven by clinical require rather than immediate commercial profit, though the eventual commercialization will be handled by pharmaceutical entities.
“The ability to selectively target the metabolic vulnerabilities of malignant cells without disrupting the homeostasis of healthy hematopoietic stem cells is the ‘holy grail’ of leukemia treatment.”
— Dr. Elena Rossi, Metabolic Oncology Specialist
Comparative Analysis: Traditional Chemotherapy vs. Metabolic Inhibition
| Feature | Traditional Cytotoxic Chemotherapy | Targeted Metabolic Inhibition |
|---|---|---|
| Primary Target | Rapidly dividing DNA/RNA | Lipid synthesis pathways (e.g., FASN) |
| Mechanism | Induces apoptosis via DNA damage | Starves cell of structural lipids |
| Systemic Toxicity | High (affects all dividing cells) | Moderate to Low (targeted) |
| Resistance Profile | Common (via efflux pumps) | Lower (targets essential survival) |
Bridging the Gap: From Lab to Clinical Application
To move these findings into the clinic, researchers are focusing on double-blind placebo-controlled trials (the gold standard of research where neither the patient nor the doctor knows who is receiving the treatment). The goal is to determine if inhibiting lipid synthesis increases the efficacy of existing treatments, such as tyrosine kinase inhibitors (TKIs).

Current epidemiological data from the WHO suggests that leukemia incidence remains steady globally, but the survival rate for acute myeloid leukemia (AML) has lagged behind other cancers. By targeting the “lipid fuel line,” clinicians hope to improve outcomes for patients who have developed resistance to standard chemotherapy.
The synergy between lipid inhibition and immunotherapy is particularly promising. By stripping the leukemia cell of its lipid-based “camouflage,” these drugs may make the cancer cells more susceptible to CAR-T cell therapy, a process where a patient’s own immune cells are engineered to attack the cancer.
Contraindications & When to Consult a Doctor
Metabolic inhibitors are potent agents and are not suitable for all patients. Those with pre-existing severe liver dysfunction or advanced metabolic disorders may face significant contraindications (specific situations in which a drug should not be used because it may be harmful to the patient). Because the liver is the primary site of lipid metabolism, these drugs can put undue stress on hepatic tissues.
Patients and caregivers should consult a hematologist-oncologist immediately if they experience:
- Unexplained bruising or petechiae (small red spots on the skin).
- Persistent low-grade fever or sudden onset of extreme fatigue.
- Rapid, unexplained weight loss or changes in appetite.
- Severe abdominal pain, which could indicate hepatic stress during metabolic therapy.
The Path Forward: Precision Metabolic Medicine
The revelation that leukemia cells rely on an internal lipid synthesis engine changes the trajectory of hematologic oncology. We are moving away from the “sledgehammer” approach of chemotherapy toward a “scalpel” approach of metabolic disruption. While we are still in the early stages of clinical translation, the objective statistical probability of success increases as we identify more specific biomarkers for lipid dependence.
The future of leukemia treatment will likely be a multimodal cocktail: a chemotherapy agent to reduce tumor burden, a metabolic inhibitor to starve the remaining cells, and an immunotherapy agent to ensure the cancer does not return. This integrated strategy represents the pinnacle of evidence-based oncology.
References
- PubMed – National Library of Medicine
- The Lancet – Oncology Division
- JAMA – Journal of the American Medical Association
- Centers for Disease Control and Prevention (CDC) – Cancer Research
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.