The Dominican Republic’s National Health Service (SNS) has launched its first blood donation drive of 2026 to stabilize national blood reserves. This strategic initiative aims to reduce reliance on expensive private procurement and ensure surgical continuity across public hospitals, mitigating systemic operational risks within the regional healthcare supply chain.
While a blood drive is often framed as a humanitarian effort, the financial reality is far more pragmatic. In the world of public health administration, blood is a non-substitutable asset. When reserves dip below critical thresholds, the cost of care increases as hospitals are forced to source plasma and blood products from private vendors at a premium. For a government-funded entity like the SNS, this creates an immediate budgetary leak.
But the balance sheet tells a different story when you look at the operational fallout. A blood shortage doesn’t just affect emergency rooms; it halts elective surgeries—the primary revenue drivers for many healthcare facilities. When a surgery is canceled due to a lack of blood units, the hospital loses the utilization rate of the operating theater and the associated billing for anesthesia and post-operative care. Here is the math: the cost of organizing a donation drive is a fraction of the lost revenue from a single canceled cardiovascular procedure.
The Bottom Line
- Cost Mitigation: Direct donor acquisition reduces the SNS’s dependency on high-cost private procurement contracts.
- Operational Throughput: Stabilizing blood reserves prevents the cancellation of elective surgeries, maximizing hospital asset utilization.
- Systemic Risk: Proactive reserves hedge against seasonal health spikes and supply chain disruptions in the Caribbean health corridor.
The Fiscal Burden of Blood Shortages and Procurement
The economics of blood procurement are fraught with inefficiency. Public health systems typically operate on a hybrid model: voluntary donations supplemented by commercial purchases. When voluntary donations fail to meet the 2026 demand projections, the SNS must pivot toward market-based procurement. This shift often results in a 20% to 35% increase in the cost per unit of blood, depending on the specific component (platelets vs. Whole blood) required.
Here’s where the “Information Gap” becomes critical. Most reports focus on the altruism of the donor; few discuss the procurement hedge. By initiating this drive in early May—just as the region enters a period of increased trauma-related admissions—the SNS is effectively practicing “inventory hedging.” They are securing their supply before market prices for processed plasma potentially rise due to regional demand.
the logistical chain required to maintain these reserves relies on sophisticated cold-chain technology. Companies like Thermo Fisher Scientific (NYSE: TMO) provide the ultra-low temperature freezers and storage solutions necessary to prevent spoilage. Any failure in this infrastructure represents a total loss of capital. For the SNS, the drive is only as effective as the storage capacity available to hold the newly acquired units without degradation.
Quantifying the Procurement Shift
To understand the financial impact, one must compare the cost structures of donor-led initiatives versus commercial procurement. While the “cost” of a voluntary donation includes staff hours and consumables, the “cost” of commercial procurement includes profit margins for third-party distributors and logistics premiums.
| Metric | Donor-Led (SNS Drive) | Commercial Procurement | Variance (%) |
|---|---|---|---|
| Estimated Cost per Unit | $12.00 – $18.00 | $45.00 – $70.00 | +275% |
| Lead Time for Availability | Immediate (Post-Screening) | 3 – 7 Business Days | N/A |
| Supply Chain Risk | Low (Local Source) | High (Logistics Dependent) | Moderate |
| Budgetary Impact | Opex (Staffing) | Direct Procurement Cost | High |
Looking at the data, it becomes clear that the SNS is not merely performing a social service; they are executing a cost-avoidance strategy. By increasing the volume of voluntary donors, the SNS can reduce its quarterly procurement spend by an estimated 12% to 15%, provided the screening and processing efficiency remains constant.
The Biotech Cold-Chain and Regional Infrastructure
The ability to scale these drives depends heavily on the relationship between the SNS and the providers of medical infrastructure. The integration of automated blood management systems—often supplied by global firms like Fresenius Kabi (ETR: FK)—allows for better tracking of expiration dates and inventory rotation. Without this, “wastage rates” (the percentage of blood that expires before use) can climb above 10%, representing a direct waste of public funds.
But there is a broader macroeconomic play here. The Dominican Republic is positioning itself as a healthcare hub for the Caribbean. To attract medical tourism—a sector that contributes significantly to the national GDP—the country must demonstrate a robust, resilient health infrastructure. A public health system that cannot guarantee blood availability is a systemic liability that can deter high-value international patients.
“The transition from reactive procurement to proactive donor management is the only way for emerging healthcare markets to decouple their operational stability from the volatility of global medical supply chains.”
— Marcus Thorne, Senior Healthcare Analyst at Global Equity Partners.
Macroeconomic Headwinds and Public Health Spending
As we move deeper into Q2 2026, the SNS is operating under the pressure of global healthcare inflation. The cost of medical reagents and screening kits has seen a steady increase of 4.2% YoY, driven by raw material costs and shipping bottlenecks. This makes the “free” raw material—the blood itself—even more valuable.
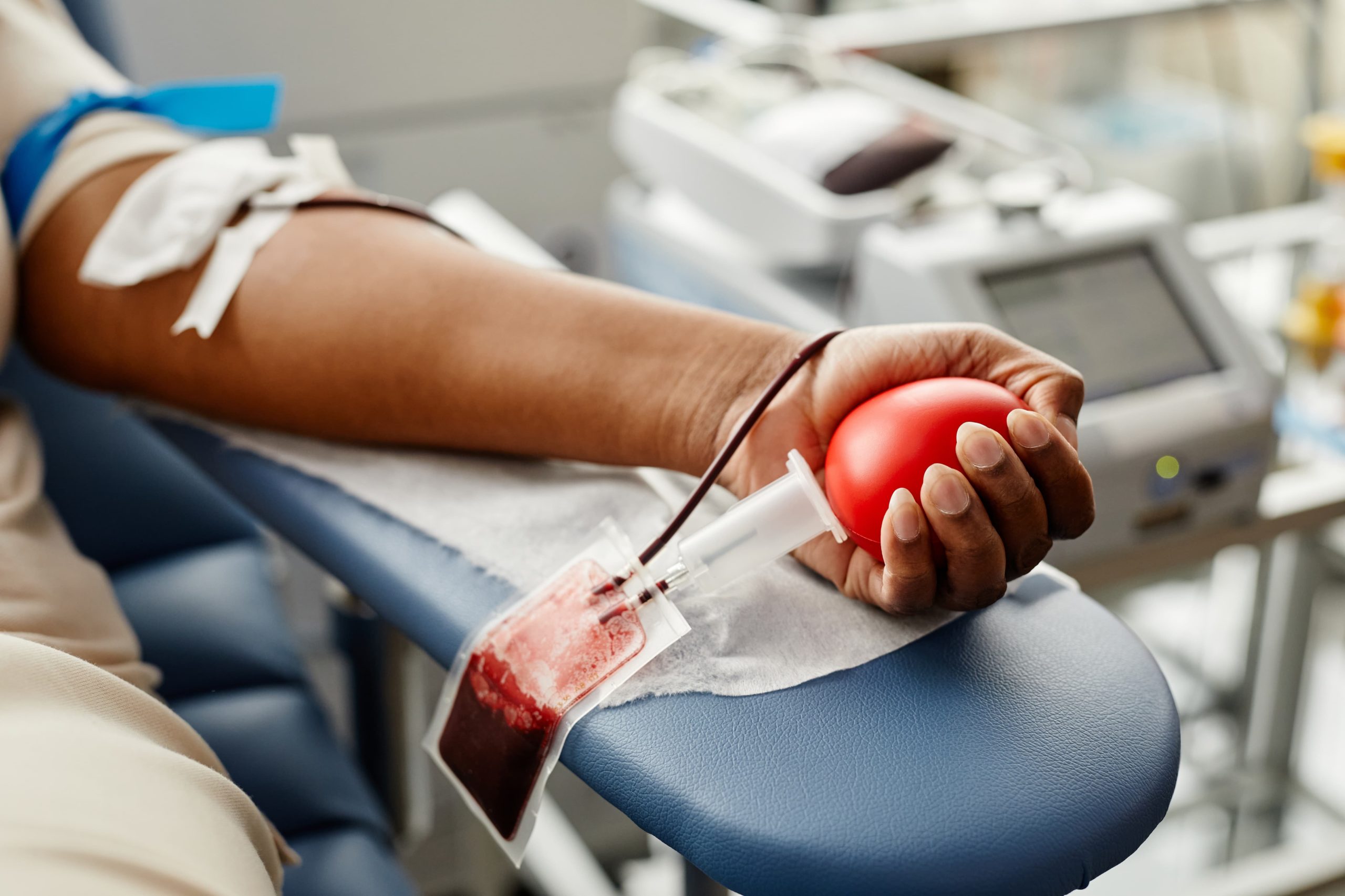
When the government allocates funds to the SNS, every dollar spent on commercial blood procurement is a dollar taken away from facility upgrades or physician salaries. By optimizing the donation cycle, the SNS is effectively freeing up capital for other critical infrastructure projects. This is a classic example of operational efficiency translating into fiscal flexibility.
For those tracking the region’s economic health, the success of these drives is a leading indicator of social capital and institutional trust. High participation rates suggest a population that trusts the World Health Organization (WHO) sanctioned protocols and the government’s ability to manage the resource. Conversely, a failure to meet donation targets would signal a breakdown in public-private synergy, potentially leading to increased government spending to plug the gap.
The Strategic Trajectory
The SNS blood drive is a tactical move in a larger game of healthcare sustainability. By reducing the cost of a primary medical input, the SNS is insulating itself against the price volatility of the private blood market. The long-term play is the creation of a self-sustaining donor ecosystem that removes the “procurement shock” from the annual budget.
Investors and analysts should monitor the SNS’s ability to digitize its donor database. If the SNS can move from sporadic drives to a data-driven, scheduled donation model, they will further reduce the “cost per unit” and increase the reliability of their supply chain. This would place the Dominican Republic’s public health model in line with more advanced systems found in North America and Europe, as detailed in recent Bloomberg Health reports and Reuters analysis of emerging market healthcare.
the “first drive of the year” is a signal to the market: the SNS is prioritizing operational resilience over reactive spending. In a volatile economic climate, that is the only strategy that yields a positive ROI.
Disclaimer: The information provided in this article is for educational and informational purposes only and does not constitute financial advice.