HPV awareness remains critically low among Canadian youth and men, despite the virus’s link to several cancers. This gap in public health literacy hinders vaccine uptake, leaving a significant portion of the population vulnerable to preventable malignancies beyond cervical cancer, including oropharyngeal and anal cancers.
The prevailing narrative surrounding the Human Papillomavirus (HPV) has long been sequestered within the realm of women’s health, specifically centered on cervical screenings. However, this gendered framing creates a dangerous clinical blind spot. By treating HPV as a “female-only” concern, we ignore the biological reality that men are both primary vectors and vulnerable hosts. As we analyze the current public health landscape this April, the failure to engage young men in vaccination and screening is not merely a communication lapse—it is a systemic failure in preventative oncology.
In Plain English: The Clinical Takeaway
- HPV is not just a “women’s virus”: It causes cancers of the throat, penis, and anus in men, as well as cervical cancer in women.
- Vaccines are preventative, not curative: The vaccine stops the virus from entering your cells but cannot “cure” an infection you already have.
- Gender-neutral vaccination is key: When both men and women are vaccinated, the overall amount of virus circulating in the community drops, protecting everyone.
The Molecular Mechanism: How VLPs Block Viral Entry
To understand why the HPV vaccine is a triumph of preventative medicine, one must understand its mechanism of action—the specific biological process by which it produces a result. The vaccines used globally, such as Gardasil 9, utilize Virus-Like Particles (VLPs). These are empty shells that mimic the exterior of the HPV virus but contain no genetic material.
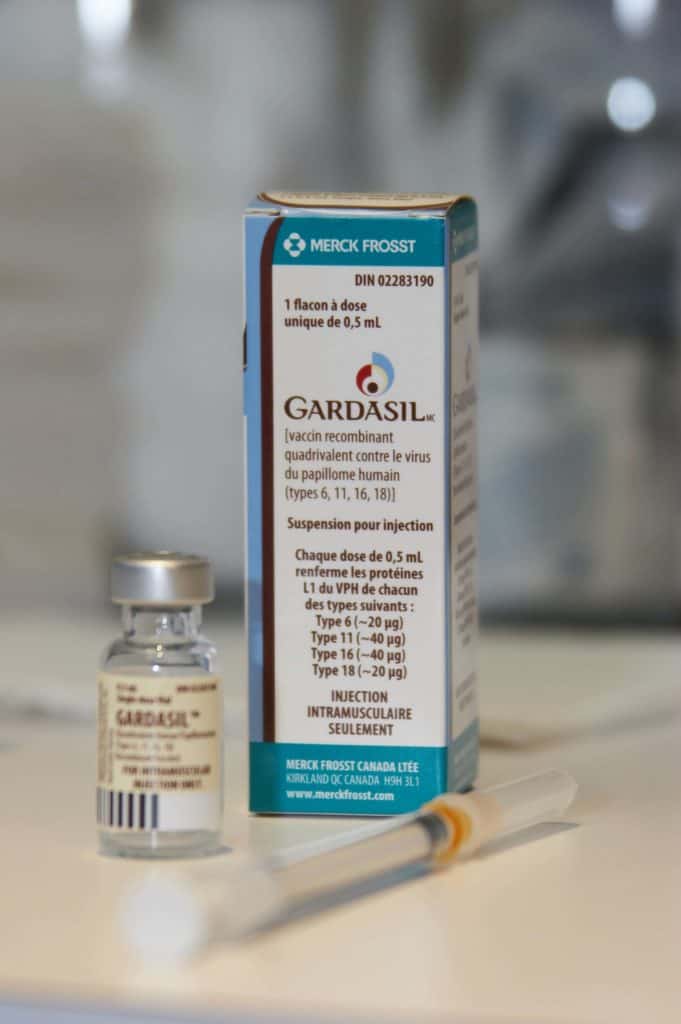
Because these VLPs lack DNA, they cannot cause infection. However, they are recognized by the immune system as foreign invaders. This triggers the production of neutralizing antibodies. If a vaccinated individual is later exposed to the actual virus, these antibodies bind to the L1 protein—the primary “key” the virus uses to unlock and enter human epithelial cells—effectively neutralizing the threat before it can integrate into the host’s genome.
This process is essential because HPV-driven cancers are caused by “high-risk” strains (primarily HPV-16 and 18) that integrate their DNA into the host cell, disrupting the regulation of cell growth and leading to malignancy. By preventing the initial infection, we eliminate the possibility of this genomic disruption.
The Oropharyngeal Crisis: The Rising Burden on Men
While cervical cancer rates are declining in regions with high vaccination, we are seeing a paradoxical rise in oropharyngeal squamous cell carcinoma (OPSCC)—cancer of the back of the throat, including the base of the tongue and tonsils. Clinical data indicates that a growing percentage of these cases are HPV-positive, with a disproportionate impact on men.

“The shift in the epidemiology of head and neck cancers is stark. We are seeing a younger demographic of men presenting with HPV-driven oropharyngeal cancers, which underscores the urgent need to move beyond the ‘cervical cancer’ label and frame HPV vaccination as a universal cancer prevention tool.” — Dr. Ian Bassett, Epidemiologist and Public Health Researcher.
The danger here is a lack of screening. Unlike the cervix, there is no routine “Pap test” for the throat. Diagnosis often occurs only after symptoms—such as a persistent sore throat or a lump in the neck—become apparent. This makes the primary prevention (vaccination) the only reliable tool for reducing the incidence of these specific malignancies.
| HPV Strain Type | Primary Associated Risks | Vaccine Coverage | Clinical Impact |
|---|---|---|---|
| Low-Risk (e.g., HPV-6, 11) | Genital Warts | Included in Gardasil 9 | High morbidity, low mortality |
| High-Risk (e.g., HPV-16, 18) | Cervical, Anal, Oropharyngeal Cancer | Included in Gardasil 9 | High mortality if undetected |
| Other High-Risk | Vulvar, Vaginal, Penile Cancers | Partial coverage | Variable based on strain |
Geo-Epidemiological Bridging: Canada vs. Global Standards
Canada’s approach to HPV has historically been fragmented across provinces. While many have moved toward gender-neutral programs, the “awareness gap” persists. In contrast, the UK’s National Health Service (NHS) implemented a highly centralized, school-based program that normalized the vaccine for all genders early on, leading to some of the highest coverage rates globally.
In the United States, the CDC (Centers for Disease Control and Prevention) has long advocated for vaccination starting at age 11 or 12, regardless of gender. The disparity in Canada often stems from a lack of targeted outreach to adolescent boys and their parents, who may still perceive the vaccine as unnecessary for males. This gap is a critical vulnerability; men act as significant reservoirs for the virus, facilitating transmission even if female vaccination rates are high.
Regarding funding and transparency, while the primary clinical trials for HPV vaccines were funded by the manufacturers (Merck and GSK), long-term population-level efficacy data has been independently verified by public health agencies such as the World Health Organization (WHO) and the CDC, ensuring that the benefits far outweigh the risks.
Contraindications & When to Consult a Doctor
The HPV vaccine is generally safe, but certain contraindications—medical reasons why a treatment should not be used—exist. Individuals with a severe allergic reaction (anaphylaxis) to any component of the vaccine, including yeast, should avoid the injection. Those who are currently moderately or severely ill should postpone vaccination until their condition stabilizes.
You should consult a healthcare provider immediately if you notice the following:
- The appearance of new, unexplained growths or warts in the genital or anal regions.
- A persistent lump in the neck or a sore throat that does not resolve with standard treatment.
- Abnormal results on a cervical screening (for those with a cervix).
The Path Forward: De-Gendering Cancer Prevention
The lack of awareness among Canadian men and youth is a solvable problem, but it requires a shift in medical communication. We must stop talking about “the cervical cancer vaccine” and start talking about “the HPV cancer vaccine.”

The clinical evidence is irrefutable: the vaccine is a highly effective tool for reducing the global burden of multiple cancers. By integrating HPV education into general adolescent health check-ups for all genders and leveraging school-based delivery systems, Canada can close the awareness gap and prevent thousands of avoidable diagnoses in the coming decades.