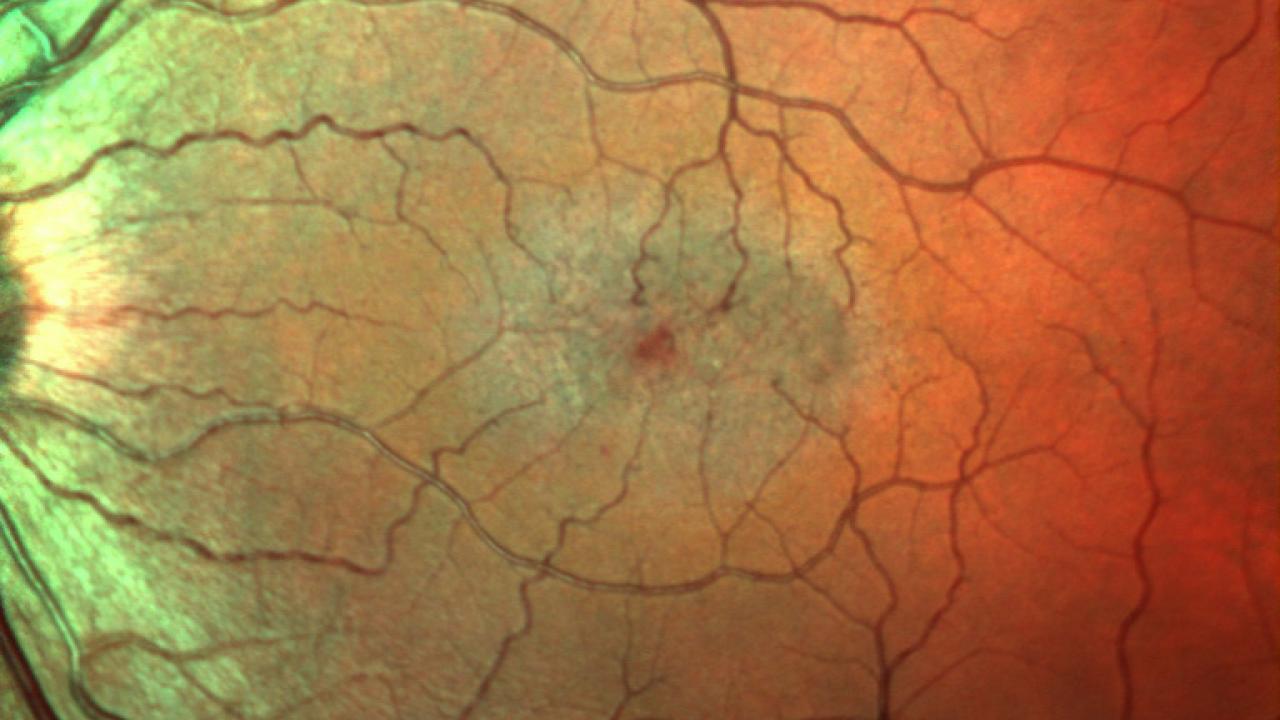
Researchers have utilized lab-grown human retinas (organoids) to identify a specific genetic mutation causing a rare childhood blindness. By mimicking human ocular development in vitro, the team uncovered how a gene change disrupts retinal layering, providing a critical blueprint for developing future gene-editing therapies to restore vision.
This breakthrough represents a paradigm shift in how we approach “orphan diseases”—rare conditions that often lack the funding or patient volume for traditional large-scale clinical trials. By creating a cellular mirror of a patient’s eye, scientists can now observe the mechanism of action (the specific biochemical process through which a drug or genetic mutation produces its effect) without risking patient safety in early-stage experimentation.
In Plain English: The Clinical Takeaway
- Precision Diagnosis: Doctors can now use “mini-eyes” grown from a patient’s own cells to find the exact genetic “typo” causing blindness.
- Safe Testing: New drugs can be tested on these lab-grown retinas first, ensuring they perform before they are ever injected into a human eye.
- Hope for Rare Cases: This method opens the door for personalized medicine for children with rare eye conditions that previously had no known cause or cure.
Decoding the Cellular Architecture of Childhood Blindness
The study centers on the use of retinal organoids—three-dimensional structures grown from pluripotent stem cells that mimic the complex layering of the human retina. In healthy eyes, the retina consists of distinct layers of photoreceptors, bipolar cells, and ganglion cells that transmit light signals to the brain.
In the cases studied, a specific gene mutation caused a failure in this structural organization. The researchers observed that the mutation prevented the cells from migrating to their correct positions, effectively “scrambling” the circuitry of the eye. This is a critical discovery because it moves the conversation from what is wrong (blindness) to how it is happening (cellular misalignment).
This research relies heavily on the understanding of the retinal development pathway, where specific transcription factors act as the “architects” of the eye. When these factors are mutated, the entire biological blueprint fails.
From Lab Bench to Bedside: The Global Regulatory Path
While the discovery is groundbreaking, the transition to a clinical treatment requires navigating rigorous regulatory frameworks. In the United States, the FDA classifies these types of interventions as “Advanced Therapy Medicinal Products” (ATMPs). In Europe, the EMA (European Medicines Agency) follows a similar stringent protocol for gene-therapy approval.
The immediate challenge is delivery. Even if we realize the gene to “fix,” we must employ a vector—typically an Adeno-Associated Virus (AAV)—to deliver the healthy gene into the retinal cells. The double-blind placebo-controlled trial (the gold standard of research where neither the patient nor the doctor knows who received the treatment) will be the final hurdle before these therapies reach the general public.
Access remains a geo-epidemiological concern. While the NHS in the UK has a history of adopting innovative gene therapies (such as Luxturna for LCA), the cost of personalized organoid-based screening is currently prohibitive for most public health systems, potentially creating a gap in care between high-income and low-income regions.
| Metric | Traditional Genetic Screening | Organoid-Based Modeling |
|---|---|---|
| Diagnostic Speed | Months to Years (Variant of Unknown Significance) | Weeks to Months (Functional Validation) |
| Predictive Power | Statistical Probability | Direct Cellular Observation |
| Drug Testing | Animal Models (Low Correlation) | Human-derived Cells (High Correlation) |
| Patient Risk | Low (Blood/Saliva sample) | Low (Skin/Blood biopsy for iPSCs) |
Funding Transparency and Expert Validation
Much of this pioneering work is funded through a combination of government grants (such as the National Institutes of Health in the US) and philanthropic organizations dedicated to blindness research. This public-private partnership is essential for “orphan” diseases, as pharmaceutical companies rarely invest in conditions that affect a slight number of patients unless there is a clear path to reimbursement.
“The ability to recapitulate human retinal development in a dish allows us to move beyond descriptive genetics. We are no longer just listing mutations; we are witnessing the pathology in real-time, which is the only way to truly validate a therapeutic target.”
This sentiment echoes the broader move toward precision medicine, where the treatment is tailored to the individual’s genetic sequence rather than a one-size-fits-all approach. The integration of WHO guidelines on genomic healthcare suggests that the goal is to standardize these “disease-in-a-dish” models globally to ensure equitable access.
Contraindications & When to Consult a Doctor
It is imperative to understand that lab-grown retina research is currently in the pre-clinical or early clinical phase. It is not a widely available treatment. Patients should be wary of clinics claiming to offer “stem cell eye cures” without FDA or EMA approval, as these are often unregulated and potentially dangerous.
Consult a pediatric ophthalmologist immediately if a child exhibits:
- Nystagmus (involuntary, rhythmic shaking of the eyes).
- Extreme sensitivity to light (photophobia).
- A white or cloudy appearance in the pupil (leukocoria).
- Failure to track objects or make eye contact during infancy.
Current contraindications for future gene therapies include pre-existing high-titer antibodies to the viral vectors used for delivery, which could trigger an immune response and neutralize the treatment.
The Future Horizon of Regenerative Ophthalmology
The discovery of this gene change is a victory for molecular biology, but the ultimate goal is the restoration of sight. The next phase of research will likely focus on CRISPR-Cas9 gene editing, which allows scientists to “cut and paste” the correct genetic sequence directly into the patient’s cells.
As we move toward 2027, we can expect more data on the longevity of these treatments. The primary question remains: can a corrected gene stop the progression of blindness, or can it actually reverse existing cellular damage? While the latter is significantly more difficult, the use of organoids provides the first real opportunity to test these hypotheses in a controlled, human-centric environment.