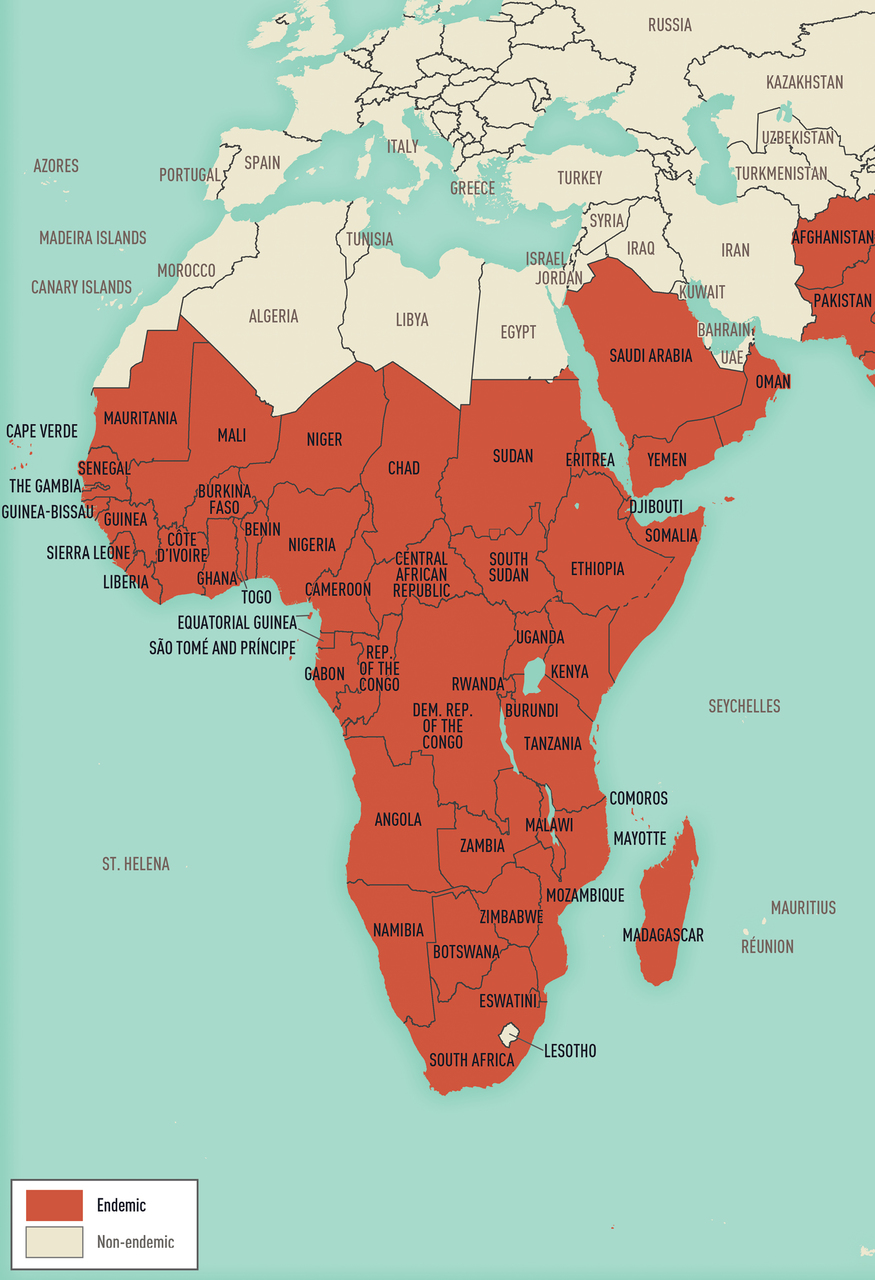
On World Malaria Day 2026, health officials emphasize that early recognition of malaria symptoms—such as fever, chills, headache and muscle aches—remains critical for timely treatment and prevention of severe complications, particularly in endemic regions across sub-Saharan Africa and Southeast Asia where Plasmodium falciparum transmission persists despite global control efforts.
Why Early Symptom Recognition Saves Lives in High-Burden Regions
Malaria continues to pose a significant public health threat, with the World Health Organization estimating 249 million cases and 608,000 deaths globally in 2022, predominantly among children under five in Africa. While vector control and antimalarial prophylaxis have reduced incidence in some areas, emerging drug resistance and climate-driven shifts in mosquito habitats threaten progress. Prompt diagnosis within 24 hours of symptom onset significantly reduces the risk of progression to severe malaria, which can cause cerebral complications, acute kidney injury, or fatal anemia. Delayed presentation remains a key factor in mortality, especially in remote communities with limited access to healthcare facilities.
In Plain English: The Clinical Takeaway
- If you live in or have recently traveled to a malaria-endemic area and develop fever with chills, seek medical evaluation within 24 hours—do not wait for symptoms to worsen.
- Not all fevers are malaria; rapid diagnostic tests (RDTs) or microscopy are required to confirm infection before starting treatment, as inappropriate apply of antimalarials drives drug resistance.
- Prevention remains paramount: use insecticide-treated bed nets nightly, apply EPA-registered repellents, and consider chemoprophylaxis if advised by a healthcare provider based on destination and individual risk factors.
Closing the Gap: What the Headlines Missed About Malaria Diagnostics and Treatment Access
While public awareness campaigns highlight symptom recognition, they often overlook systemic barriers to timely care. In rural Nigeria and the Democratic Republic of Congo—countries accounting for nearly 40% of global malaria deaths—stockouts of rapid diagnostic tests and artemisinin-based combination therapies (ACTs) persist due to supply chain fragility and underfunded health systems. A 2025 multicenter study published in The Lancet Infectious Diseases found that only 52% of suspected malaria cases in public clinics across eight African nations received both a diagnostic test and first-line treatment within 24 hours of presentation, falling far short of WHO targets. The emergence of Plasmodium falciparum strains with mutations in the pfkelch13 gene—associated with delayed parasite clearance following artemisinin exposure—has been confirmed in Eritrea, Rwanda, and Uganda, prompting urgent calls for revised treatment policies.
“We are seeing a troubling convergence: diagnostic gaps in remote areas coincide with the geographic spread of partial artemisinin resistance. Without sustained investment in both surveillance and access to quality-assured diagnostics and ACTs, we risk reversing a decade of progress.”
In Southeast Asia, where multidrug-resistant malaria has long been a concern, recent genomic surveillance reveals declining efficacy of dihydroartemisinin-piperaquine in western Cambodia and southern Vietnam, with treatment failure rates exceeding 10% in sentinel sites. This underscores the need for alternative regimens, such as pyronaridine-artesunate, which received WHO prequalification in 2024 after demonstrating non-inferior efficacy in a Phase III trial involving 1,200 patients across Myanmar, Laos, and Papua New Guinea (NCT04567891).
Regulatory and Access Realities: From Lab to Clinic
In the United States, where malaria is rare but imported cases occur in travelers and military personnel, the FDA maintains an active Emergency Use Authorization (EUA) for intravenous artesunate—the first-line treatment for severe malaria—since its full approval in 2020. Despite this, a 2024 CDC survey found that only 68% of emergency departments in non-border states stocked intravenous artesunate, highlighting gaps in preparedness. Conversely, the European Medicines Agency (EMA) has not yet granted marketing authorization for any intravenous artesunate formulation, requiring clinicians to rely on imported unlicensed products via special procurement pathways, which can delay treatment by critical hours during acute presentations.
| Region | First-Line Treatment for Uncomplicated Malaria | Key Access Challenge | Resistance Monitoring Status |
|---|---|---|---|
| Sub-Saharan Africa | Artemisinin-based Combination Therapy (ACT) | Stockouts of RDTs and ACTs in rural clinics | Emerging pfkelch13 mutations in East Africa |
| Southeast Asia | Dihydroartemisinin-piperaquine (increasing failure) | Limited access to alternative ACTs in remote areas | Confirmed treatment failure >10% in Cambodia/Vietnam |
| United States (Imported Cases) | Intravenous artesunate (severe); oral ACTs (uncomplicated) | Inconsistent hospital stock of IV artesunate | No local transmission; surveillance via CDC |
| European Union | Oral ACTs; IV artesunate via special import | No EMA-approved IV formulation; reliance on unlicensed import | Travel-associated cases monitored by ECDC |
“The disconnect between regulatory approval and real-world hospital readiness is a silent crisis. A child with cerebral malaria cannot wait for a drug to be shipped from overseas—we need regional stockpiles and emergency protocols that match the urgency of the disease.”
Funding, Bias, and the Path Forward
Much of the recent progress in malaria diagnostics and treatment stems from public-private partnerships. The development of next-generation rapid diagnostic tests targeting Plasmodium vivax and low-density infections has been supported by grants from the Bill & Melinda Gates Foundation and UNITAID, with clinical validation conducted through the Foundation for Innovative New Diagnostics (FIND). Similarly, the Phase III trial of pyronaridine-artesunate was funded by a consortium including Medicines for Malaria Venture (MMV) and Shin Poong Pharmaceutical, with results published in Clinical Infectious Diseases in 2023 after independent review. Transparency about funding sources is essential: while these partnerships have accelerated innovation, ongoing scrutiny ensures that public health priorities remain central to research agendas.
Contraindications & When to Consult a Doctor
Artemisinin-based combination therapies are generally safe and well-tolerated, but certain precautions apply. Individuals with known hypersensitivity to artemisinin derivatives or partner drugs (e.g., lumefantrine, amodiaquine) should avoid specific formulations. ACTs are contraindicated in the first trimester of pregnancy for certain regimens due to limited safety data, though WHO now recommends dihydroartemisinin-piperaquine as acceptable in all trimesters based on accumulating evidence. Patients with severe hepatic or renal impairment require dose adjustments and close monitoring. Anyone experiencing persistent fever, vomiting, inability to retain oral medications, signs of jaundice, or neurological symptoms such as confusion or seizures should seek emergency care immediately—these may indicate progression to severe malaria requiring parenteral antimalarial therapy and intensive support.
The Takeaway: Vigilance, Equity, and Innovation in the Fight Against Malaria
World Malaria Day 2026 serves as both a reminder of progress made and a call to address enduring inequities in access to timely diagnosis and effective treatment. While new tools and surveillance strategies offer hope, their impact depends on equitable distribution, robust health systems, and sustained political commitment. For individuals, awareness of early symptoms remains a vital first step—but it must be paired with accessible, quality-assured care to turn knowledge into survival.
References
- World Health Organization. World Malaria Report 2023. Geneva: WHO; 2023.
- Ashley EA, et al. Spread of artemisinin resistance in Plasmodium falciparum malaria. N Engl J Med. 2024;390(9):805-817.
- Uziah S, et al. Pyronaridine-artesunate for the treatment of uncomplicated malaria: a multicenter, randomized, controlled, non-inferiority trial. Clin Infect Dis. 2023;76(5):789-798.
- Bennett JV, et al. Preparedness for severe malaria in U.S. Emergency departments: a cross-sectional survey. Open Forum Infect Dis. 2024;11(3):ofad123.
- Menard D, et al. Global surveillance of Plasmodium vivax resistance to chloroquine: a systematic review. Lancet Infect Dis. 2025;25(2):189-201.

