Medicaid serves as a crucial program providing extensive health and long-term care to individuals with low incomes, including access to vital prescription drugs. This program covers about one in five people in the United States, ensuring that those who are often most vulnerable can receive necessary medical treatment. However, in recent years, spending on Medicaid prescription drugs has surged, partly due to the introduction of new, high-cost medications, such as GLP-1s and advanced therapies for rare diseases. In light of a challenging fiscal environment and impending federal funding cuts, state Medicaid programs are increasingly focused on managing rising pharmacy costs.
Recent initiatives aimed at controlling prescription drug costs have emerged from various administrations, yet their effectiveness remains to be seen. This article outlines five key facts regarding Medicaid prescription drug coverage, payment, and administration, providing essential context for ongoing discussions about federal actions to address prescription drug costs.
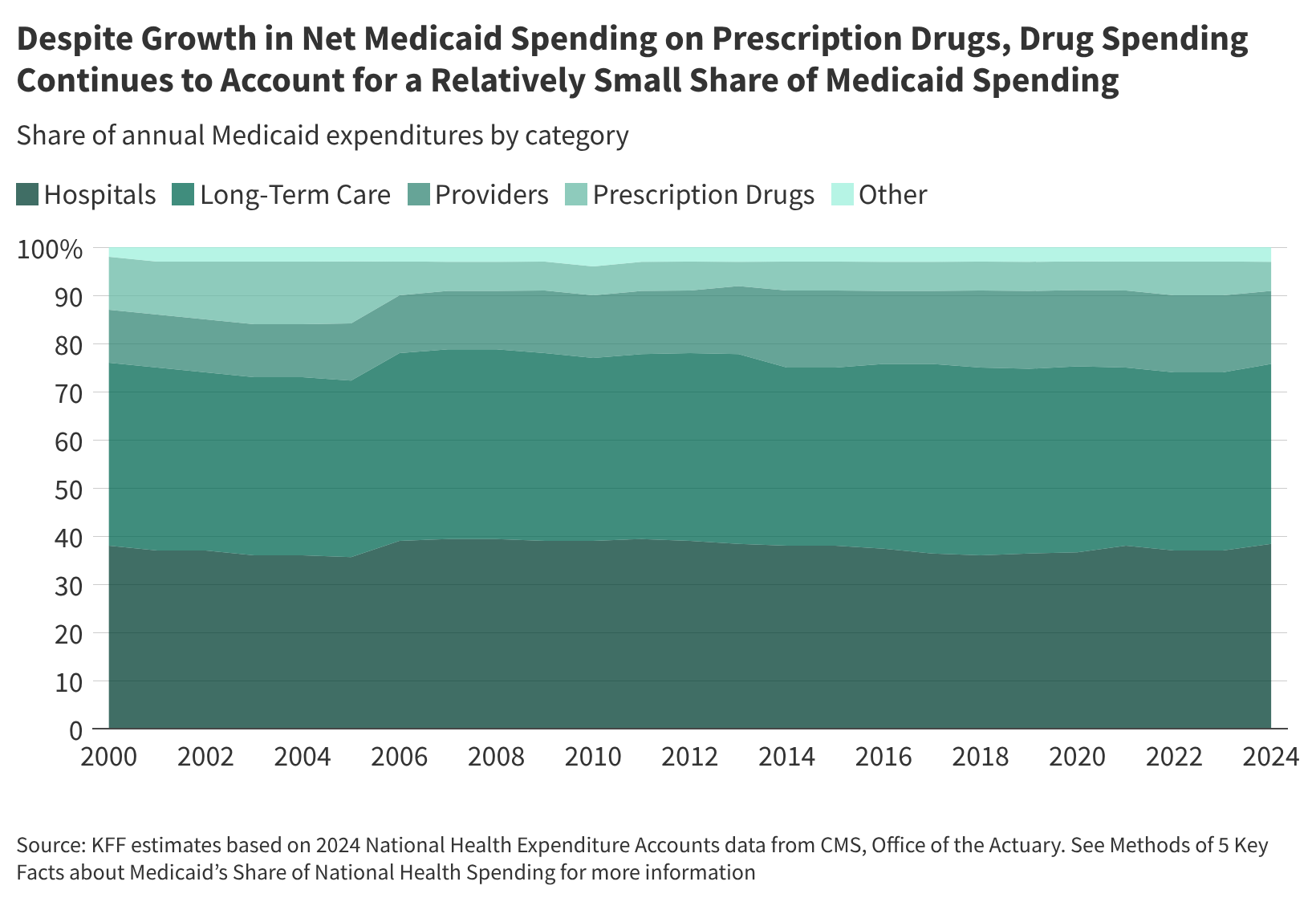
1. Prescription Drug Spending is a Slight Portion of Medicaid Budget
Whereas Medicaid spending on prescription drugs has increased, it still constitutes a relatively minor segment of overall Medicaid expenditures. In 2024, drug spending accounted for just 6% of total Medicaid spending, significantly less than expenditures on hospitals (38%), long-term care (37%), and provider services (15%). The percentage of Medicaid spending on prescription drugs has maintained stability between 5% and 7% since the implementation of the Medicare prescription drug benefit in 2006, which shifted some costs for dual-eligible beneficiaries to the federal government. Despite this stability, spending on prescription drugs has risen by 46% from fiscal year 2019 to 2024, mirroring the overall growth of Medicaid spending during the same period.
2. Low Out-of-Pocket Costs Enhance Access to Medications
Federal regulations limit the amount Medicaid enrollees must pay out-of-pocket for prescription medications. For individuals with incomes at or below 150% of the federal poverty level, the maximum copay is capped at $4 for preferred drugs and $8 for non-preferred drugs. Certain populations, including most children and pregnant women, are exempt from these costs. This structure enables Medicaid beneficiaries to avoid the common practice of rationing medications due to cost, which is a significant issue for uninsured adults.
Approximately two-thirds of adults enrolled in Medicaid filled a prescription in the past year, a figure similar to that of those with private insurance but considerably higher than uninsured adults. Despite the nominal cost limits, some families may still find these expenses burdensome. Although recent proposals for federal prescription drug initiatives may influence overall Medicaid spending, their impact on affordability for enrollees is expected to be minimal.
3. Variability in Administration Among States
Every state Medicaid program is mandated to cover prescription drugs, yet the approaches to administering this benefit vary widely. States have considerable discretion in managing their pharmacy benefits within federal guidelines for payment and medical necessity. Currently, capitated managed care is the predominant method for delivering prescription drug services to Medicaid enrollees, with only eight out of 42 states operating under a fee-for-service model by July 2025. In managed care states, the pharmacy benefit is typically included in the overall capitation rate, though specific drugs may still be “carved out” for separate management.
many states contract with pharmacy benefit managers (PBMs) to oversee pharmacy benefits, performing tasks such as negotiating rebates and managing drug utilization. As of mid-2023, 33 states utilized PBMs for their fee-for-service pharmacy benefit. However, the role of PBMs has come under scrutiny, prompting states to implement reforms aimed at increasing transparency.
4. Complex Payment Policies for Prescription Drugs
Payment for prescription drugs within Medicaid is governed by a complex set of regulations. The total cost for a given outpatient drug is calculated based on the pharmacy’s reimbursement after accounting for manufacturer rebates. States determine the ingredient cost, which can be influenced by the actual acquisition cost or average manufacturer price. Federal regulations stipulate that reimbursements must not exceed the lesser of the pharmacy’s usual charge or a combination of the ingredient cost and a professional dispensing fee.
Manufacturers are obligated to participate in the Medicaid Drug Rebate Program (MDRP), which requires them to rebate a portion of the drug payments in exchange for Medicaid coverage of nearly all FDA-approved drugs. The rebate amounts vary by drug type, with brand-name drugs typically incurring a rebate of at least 23.1% of the average manufacturer price, while generic drugs have a fixed rebate of 13%.
5. Diverse Strategies to Manage Drug Expenditures
Although states are required to cover most FDA-approved medications, they employ a variety of strategies to manage prescription drug expenditures. For instance, state Medicaid programs often implement preferred drug lists (PDLs) and prior authorization processes to control costs and ensure appropriate medication use. These tools can incentivize the use of cost-effective medications while establishing limits on certain prescriptions.
States similarly utilize innovative payment strategies, including value-based arrangements that tie reimbursement rates to drug performance. Continuous updates and expansions of these strategies reflect the evolving landscape of Medicaid drug spending. Recent surveys indicate that many states are actively developing initiatives aimed at containing costs, especially concerning high-cost specialty drugs that have been driving up overall Medicaid spending.
As the landscape of Medicaid prescription drug coverage continues to shift amid financial challenges and policy changes, stakeholders will need to monitor the effectiveness of these strategies and their implications for patient access and affordability. Ongoing discussions will likely shape the future of Medicaid and its role in providing essential healthcare services.
For more information on Medicaid and prescription drug management, please share your thoughts and experiences in the comments below.
Disclaimer: This article is for informational purposes only and does not constitute medical or professional advice.