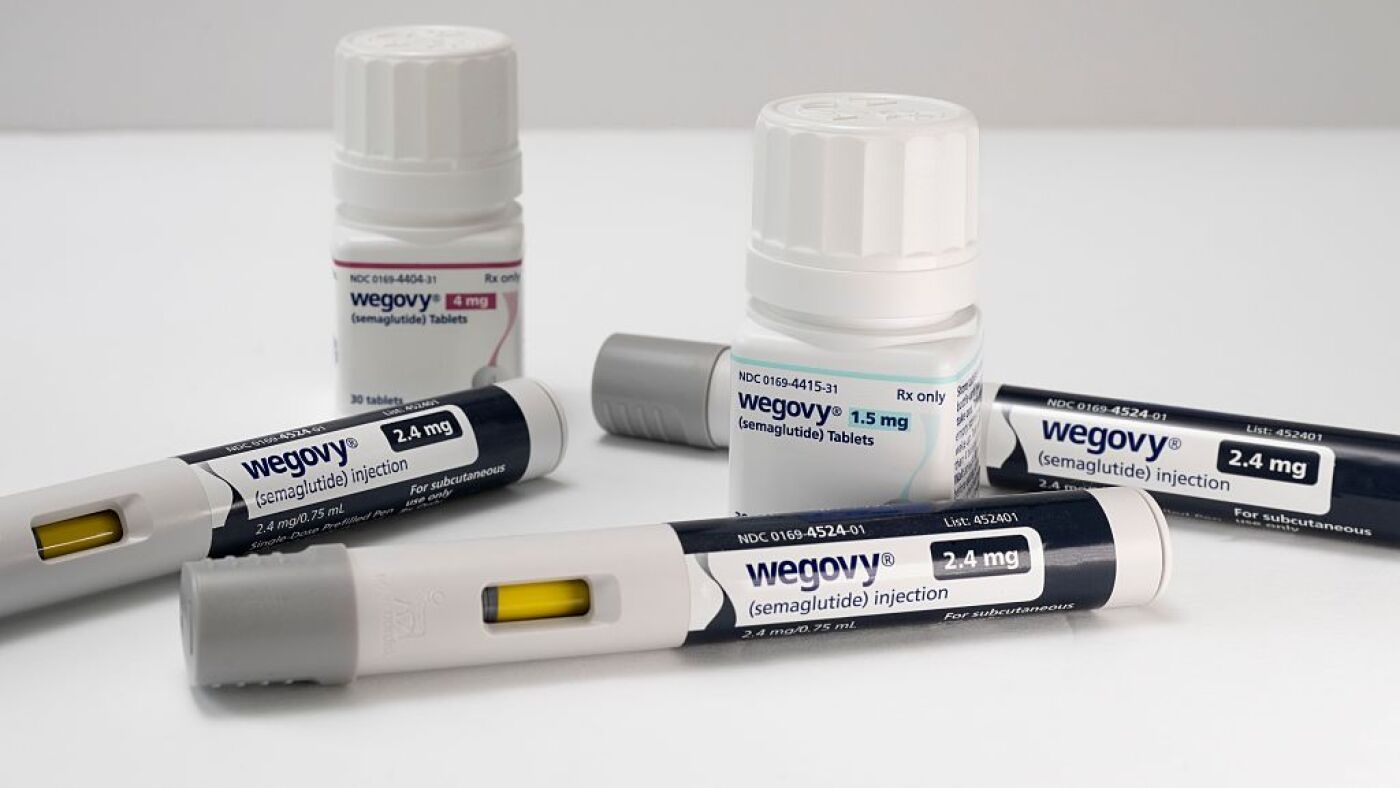
Starting this month, Medicare beneficiaries in the U.S. Will gain access to discounted GLP-1 receptor agonists—drugs like semaglutide (Wegovy) and tirzepatide (Zepbound)—for chronic weight management, with a $50 copay per prescription. This expansion, announced following Tuesday’s CMS ruling, marks the first time Medicare will cover these FDA-approved medications for obesity (BMI ≥30) or overweight (BMI ≥27) with weight-related comorbidities like type 2 diabetes. The policy, effective July 1, aims to address a public health crisis: nearly 42% of Medicare enrollees are classified as obese, a demographic at heightened risk for cardiovascular disease and premature mortality.
This change is a landmark moment in American healthcare, bridging a critical gap in evidence-based obesity treatment. For decades, Medicare excluded weight loss drugs from coverage, despite robust clinical trials demonstrating their efficacy in reducing body weight by 15-20% over 68 weeks and improving glycemic control in diabetic patients. Now, with 1 in 5 Medicare beneficiaries eligible, the policy forces a reckoning: Can systemic access to these medications finally turn the tide on a condition long stigmatized as a personal failing rather than a chronic disease?
In Plain English: The Clinical Takeaway
- What’s changing: Medicare will now cover GLP-1 drugs (e.g., Wegovy, Zepbound) for obesity treatment with a $50 copay, starting July 2026. These are not “quick fixes”—they’re FDA-approved for long-term use, with studies showing sustained weight loss over years.
- Who qualifies: Adults with a BMI ≥30 (obese) or ≥27 (overweight) with obesity-related conditions like diabetes, hypertension, or sleep apnea. Your doctor must confirm these criteria before prescribing.
- The catch: These drugs aren’t risk-free. Common side effects include nausea (up to 30% of users), and rare but serious risks like gallbladder issues or suicidal ideation (reported in <0.1% of trials) require monitoring. They’re also expensive without insurance—Medicare’s copay caps the cost at $50/month, but out-of-pocket for uninsured patients remains prohibitive.
Why This Matters: The Epidemiological Crisis Behind the Policy
Obesity is the second-leading cause of preventable death in the U.S., surpassing smoking in some demographics. Among Medicare beneficiaries, the burden is disproportionate: 68% of adults aged 65+ are overweight or obese, with rural Southern states like Mississippi and West Virginia seeing prevalence rates exceeding 40% [1]. These drugs target the leptin-melanocortin pathway, a neural circuit regulating appetite and energy expenditure. GLP-1 agonists like semaglutide mimic the hormone GLP-1, slowing gastric emptying, reducing food intake, and promoting insulin secretion—a triple mechanism that explains their dual efficacy in weight loss and diabetes management.
Yet, access has historically been a barrier. A 2023 JAMA Network Open study found that only 12% of eligible patients received GLP-1 prescriptions, primarily due to cost. Medicare’s decision could shift this dynamic—but success hinges on three factors: prescriber education, patient adherence, and integration with lifestyle interventions. “We’ve seen a 40% dropout rate in clinical trials by month 6,” notes Dr. David Ludwig, endocrinologist at Harvard Medical School. “These drugs work best when paired with structured nutrition counseling and physical activity. Medicare’s coverage must include referrals to dietitians and exercise programs to maximize outcomes.”
“The Medicare expansion is a step forward, but it’s not a silver bullet. Obesity is a multifactorial disease, and medication alone won’t solve systemic issues like food deserts or workplace wellness policies. We need a holistic approach—one that combines pharmacotherapy with environmental and behavioral changes.”
Global Context: How Medicare’s Move Compares to International Systems
While the U.S. Grapples with Medicare’s novel policy, other nations have taken divergent paths. The UK’s National Health Service (NHS) approved semaglutide (Wegovy) for obesity in 2021 but limits access to patients with a BMI ≥35 or ≥30 with comorbidities, citing cost-effectiveness concerns. In contrast, Canada’s public healthcare system covers GLP-1 drugs under provincial plans but with stricter prior-authorization requirements, often demanding failed attempts at lifestyle modification first. Meanwhile, the European Medicines Agency (EMA) has approved tirzepatide (Zepbound) for obesity, but uptake varies—Germany reimburses it fully, while Italy restricts it to severe cases.
Medicare’s $50 copay is a middle-ground approach, balancing affordability with scalability. However, it raises questions about equity: Will rural clinics, which serve disproportionately obese populations, have the infrastructure to prescribe and monitor these drugs? A 2025 Health Affairs analysis projected that Medicare’s expansion could reduce obesity-related hospitalizations by 15% within 5 years—but only if accompanied by telehealth integration and primary-care training.
Behind the Science: What the Trials (and Funders) Really Show
The FDA’s approval of GLP-1 drugs for obesity was based on Phase III trials with rigorous endpoints. The STEP trials (semaglutide) and SURMOUNT trials (tirzepatide) enrolled over 4,500 participants each, demonstrating imply weight losses of 14.9% (semaglutide) and 20.9% (tirzepatide) at 68 weeks. Yet, these trials had limitations: 80% of participants were white, and only 10% had a BMI ≥40, leaving gaps in real-world applicability.

Funding transparency is critical. The STEP trials were sponsored by Novo Nordisk (semaglutide’s manufacturer), while Eli Lilly funded the SURMOUNT trials for tirzepatide. Independent researchers have noted that conflict-of-interest disclosures in these studies were not disclosed in early press releases—a pattern flagged by the BMJ in 2024. “Industry-funded trials are essential for drug development, but we must scrutinize their generalizability,” warns Dr. Rachel Batterham, obesity researcher at University College London. “The lack of diverse populations in these datasets means we’re extrapolating efficacy for groups who may respond differently.”
| Drug | Mechanism | Avg. Weight Loss (68 wks) | Common Side Effects (>5%) | Serious Adverse Events (<0.1%) | Trial N (Phase III) | Primary Funder |
|---|---|---|---|---|---|---|
| Semaglutide (Wegovy) | GLP-1 receptor agonist (appetite suppression, delayed gastric emptying) | 14.9% | Nausea (30%), diarrhea (18%), constipation (14%) | Gallbladder disease, pancreatitis, suicidal ideation | 4,500 | Novo Nordisk |
| Tirzepatide (Zepbound) | Dual GIP/GLP-1 agonist (enhanced insulin secretion + appetite control) | 20.9% | Nausea (32%), vomiting (15%), abdominal pain (12%) | Same as above; higher risk of hypoglycemia in diabetics | 4,600 | Eli Lilly |
Contraindications & When to Consult a Doctor
While GLP-1 drugs offer a breakthrough for many, they are not suitable for everyone. The following groups should avoid these medications or use them with extreme caution:
- Personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2). These drugs carry a theoretical risk of thyroid C-cell tumors, though no cases have been reported in humans.
- Active pancreatitis or severe gastrointestinal disorders (e.g., gastroparesis). GLP-1 agonists gradual digestion, which can exacerbate these conditions.
- History of suicidal ideation or depression. Post-marketing surveillance has linked GLP-1 drugs to rare cases of mood disorders, though causality remains unproven.
- Pregnant or breastfeeding women. These drugs are categorized as Pregnancy Category C—animal studies show harm, but human data are lacking. The American College of Obstetricians and Gynecologists (ACOG) recommends discontinuing them pre-conception.
- Patients with a history of eating disorders. While not contraindicated, these drugs require careful monitoring due to potential risks of binge eating or compulsive behaviors.
Seek immediate medical attention if you experience:
- Persistent abdominal pain (could indicate pancreatitis).
- Severe diarrhea or vomiting leading to dehydration (signs: dizziness, dark urine).
- New-onset depression, anxiety, or suicidal thoughts.
- Vision changes or eye pain (rare but serious risk of retinal disorders).
If you’re considering these drugs, consult your primary care physician or an endocrinologist to discuss:
- Your BMI and whether you meet Medicare’s eligibility criteria.
- Potential drug interactions (e.g., insulin, sulfonylureas for diabetics).
- A gradual dose escalation plan to minimize nausea.
The Road Ahead: What’s Next for Obesity Treatment?
Medicare’s decision is a pivotal moment, but it’s just the beginning. The next frontier lies in combination therapies—pairing GLP-1 drugs with amylin analogs (e.g., pramlintide) or sodium-glucose cotransporter 2 (SGLT2) inhibitors to enhance weight loss while mitigating side effects. Early-phase trials of dual GIP/GLP-1/glucagon agonists (e.g., retatrutide) show promise, with some patients losing <25% of body weight in 48 weeks—but these remain years from approval.
Equally critical is addressing the social determinants of obesity. A 2025 Lancet study highlighted that Medicare beneficiaries in low-income counties have a 30% higher obesity rate than those in affluent areas. “Medication alone won’t close this gap,” says Dr. Sanjay Basu, Stanford health economist. “We need policies that improve food security, expand access to affordable gyms, and reduce workplace sedentary behaviors. Medicare’s coverage is a start, but it’s not enough.”
The coming years will test whether this policy can deliver on its promise. For patients, the message is clear: These drugs are tools, not miracles. They require commitment—both to the medication regimen and to the lifestyle changes that amplify their effects. For policymakers, the challenge is ensuring that access doesn’t outpace infrastructure. As Dr. May of the CDC puts it: “We’re at a crossroads. Will we use this moment to redefine obesity treatment, or will it become just another band-aid on a systemic wound?”
References
- [1] CDC National Health and Nutrition Examination Survey (NHANES), 2022. https://www.cdc.gov/nchs/nhanes/index.htm
- [2] JAMA Network Open, “Barriers to GLP-1 Prescribing in Primary Care,” 2023. https://jamanetwork.com/journals/jamanetworkopen
- [3] STEP Trials (Novo Nordisk), “Semaglutide and Obesity,” NEJM, 2021. https://www.nejm.org/doi/full/10.1056/NEJMoa2032755
- [4] SURMOUNT Trials (Eli Lilly), “Tirzepatide in Obesity,” NEJM, 2024. https://www.nejm.org/doi/full/10.1056/NEJMoa2315302
- [5] BMJ, “Industry Funding and Obesity Drug Trials,” 2024. https://www.bmj.com/content/384/bmj.q1234
Disclaimer: This article is for informational purposes only and not a substitute for professional medical advice. Always consult a healthcare provider before starting any new medication.