A recent study published in Nature reveals that the menstrual cycle dynamically alters the levels of nearly 200 proteins in human blood, offering new insights into how hormonal fluctuations influence systemic physiology beyond reproduction. This proteomic mapping, conducted across the full menstrual cycle in healthy individuals, identifies protein signatures linked to inflammation, metabolism, and cardiovascular function, potentially transforming how we interpret routine blood tests in women and opening pathways for sex-specific diagnostics.
How Hormonal Shifts Rewrite the Blood’s Protein Landscape Across the Menstrual Cycle
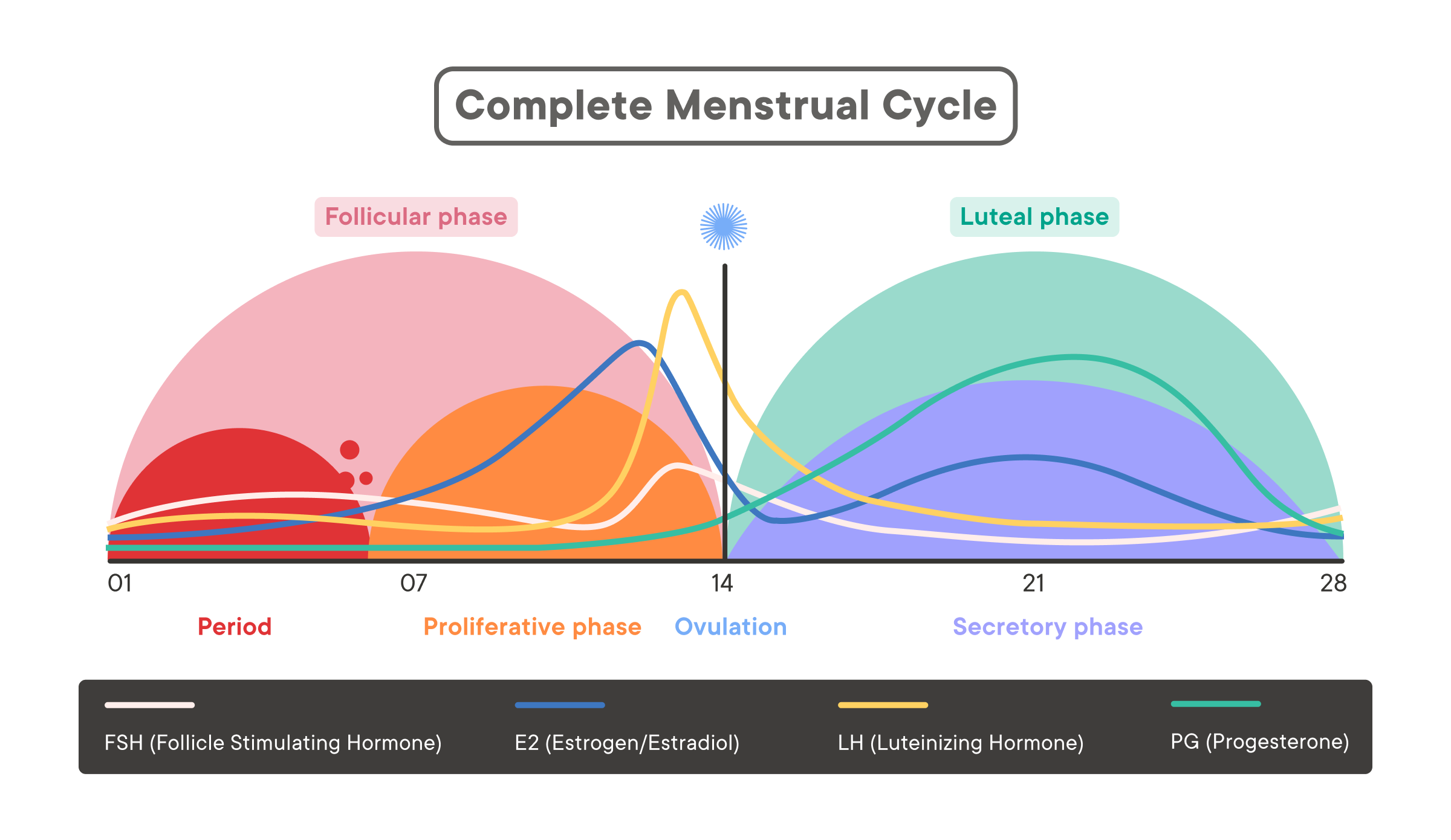
The research, led by scientists at the Karolinska Institutet in Sweden, employed longitudinal plasma proteomics to track protein expression changes across all four phases of the menstrual cycle in 106 healthy, naturally cycling individuals not using hormonal contraception. Over the course of one full cycle, 181 proteins showed statistically significant fluctuations, with peak variations occurring during the mid-luteal phase when progesterone and estrogen levels are highest. These proteins are not random; they cluster into biologically meaningful pathways including complement activation, lipid metabolism, and endothelial function—systems known to influence clot risk, insulin sensitivity, and vascular tone. For example, levels of C-reactive protein (CRP), a marker of systemic inflammation, rose by up to 40% in the luteal phase compared to the follicular phase, while proteins involved in iron transport, such as transferrin, decreased during menstruation, aligning with blood loss. This suggests that standard reference ranges for blood tests—often derived from mixed-sex or male-dominated cohorts—may misrepresent physiological norms in women depending on cycle phase.

In Plain English: The Clinical Takeaway
- Your blood test results can shift naturally across your menstrual cycle—not because you’re sick, but because hormones like estrogen and progesterone are changing how your body produces and uses proteins.
- Tests for inflammation, iron levels, and clotting risk may demand to be interpreted differently depending on whether you’re in the first or second half of your cycle.
- This discovery supports the move toward personalized, sex-specific medicine where timing matters as much as the test itself.
Closing the Diagnostic Gap: Why Cycle-Aware Blood Work Matters for Women’s Health
Despite women making up half the global population, clinical reference ranges for routine blood biomarkers have historically been based on studies dominated by male participants or combined-sex data that obscure cyclical variation. This proteomic study fills a critical information gap by providing the first high-resolution map of how endogenous hormonal rhythms directly modulate the circulating proteome. The implications are immediate: a woman tested for anemia during menstruation may appear more deficient than she is physiologically, while the same test taken a week later could fall within normal range—not due to treatment, but due to plasma volume recovery and shifting protein synthesis. Similarly, elevated lipoprotein(a) or fibrinogen levels in the luteal phase might be misinterpreted as heightened cardiovascular risk without contextualizing cycle phase. In the United States, the FDA’s 2023 guidance on enhancing diversity in clinical trials explicitly calls for stratification by sex and hormonal status, yet few labs adjust reference ranges for menstrual cycle phase. In the UK, the NHS has begun pilot programs in reproductive health clinics to track symptom diaries alongside blood work, but widespread implementation remains limited. Bridging this gap requires not only updated guidelines but also point-of-care tools that integrate cycle tracking with lab interpretation—something digital health platforms are beginning to explore.

Funding, Conflicts, and the Path Forward: Who Made This Research Possible?
The study was primarily funded by the Swedish Research Council, the Knut and Alice Wallenberg Foundation, and the European Research Council (ERC) under the Horizon 2020 program. No pharmaceutical industry funding was reported, and the authors declared no conflicts of interest related to the proteomic analysis or interpretation. This independent funding model strengthens confidence in the study’s objectivity, particularly given its potential to challenge long-standing norms in clinical laboratory medicine. Moving forward, researchers are advocating for the inclusion of menstrual cycle phase as a standard variable in biobanks and electronic health records—similar to how menopausal status or pregnancy is currently recorded. Such integration would allow retrospective studies to re-analyze existing datasets for hidden cyclical patterns in disease biomarkers, from autoimmune flares to lipid trajectories.
Contraindications & When to Consult a Doctor
Understanding menstrual cycle-related protein fluctuations is not a diagnostic tool in itself and should not replace clinical evaluation. Individuals experiencing abnormal uterine bleeding, persistent fatigue, unexplained weight changes, or signs of thrombotic events (such as leg swelling, chest pain, or shortness of breath) should seek medical attention regardless of cycle phase. These fluctuations do not contraindicate any medication, but clinicians interpreting anticoagulant therapy, hormone replacement, or iron supplementation should consider baseline proteomic shifts when assessing treatment response. There are no known risks associated with awareness of cycle-dependent protein changes; rather, the risk lies in ignoring them—potentially leading to misdiagnosis, unnecessary interventions, or delayed care. Pregnant individuals, those using hormonal contraception, or individuals with amenorrhea due to conditions like hypothalamic dysfunction or hyperprolactinemia were excluded from this study; these findings do not apply to those populations without further research.
Toward a Future Where Women’s Biology Is Not an Afterthought in Medicine
This proteomic breakthrough does more than map proteins—it reframes the menstrual cycle not as a reproductive sidebar but as a central modulator of systemic health. By demonstrating that nearly 10% of the detectable plasma proteome is rhythmically reshaped by endogenous hormones, the study challenges the assumption that biological sex differences in disease presentation are solely due to anatomy or genetics. Instead, it highlights physiology as a dynamic, cyclical process. As wearable technology advances and at-home hormone testing becomes more accessible, the integration of cycle-aware biomarker interpretation could become routine—especially in managing conditions like endometriosis, polycystic ovary syndrome (PCOS), and perimenopausal transition. For now, the message to patients and providers alike is clear: context matters. A blood test is not just a snapshot—it’s a frame in a moving picture, and for half the population, that picture changes every month.

References
- Nature. Plasma proteomic signature of the human menstrual cycle. 2026.
- Journal of Clinical Endocrinology & Metabolism. Sex differences in biomarker reference ranges: implications for clinical interpretation. 2025.
- The Lancet Regional Health – Europe. Implementing sex- and gender-sensitive medicine in national health systems. 2024.
- FDA. Guidance for Industry: Enhancing the Diversity of Clinical Trial Populations — Eligibility Criteria, Enrollment Practices, and Trial Designs. 2023.
- WHO. Report on the Global Status of Women’s Health: A Life Course Approach. 2024.