New clinical data published this week in the New England Journal of Medicine demonstrates that venous stenting significantly reduces symptoms of Post-Thrombotic Syndrome (PTS) compared to standard compression therapy. This intervention offers a viable mechanical solution for patients with chronic iliofemoral obstruction, substantially improving mobility and overall quality of life.
For decades, the medical community viewed Post-Thrombotic Syndrome—a chronic condition resulting from Deep Vein Thrombosis (DVT)—as an inevitable decline managed solely by compression stockings. However, the paradigm is shifting. By addressing the anatomical obstruction rather than merely managing the resulting edema (swelling), we are moving from palliative care to restorative intervention. This shift is critical because PTS not only diminishes quality of life but can lead to debilitating venous ulcers that strain healthcare resources globally.
In Plain English: The Clinical Takeaway
- What is it? A procedure where a small mesh tube (stent) is placed in a blocked vein to preserve it open.
- Why it matters: It treats the root cause of leg swelling and pain instead of just squeezing the leg with stockings.
- The Result: Patients experience significantly less pain and a lower risk of skin ulcers compared to traditional treatments.
The Mechanism of Action: Reversing Venous Hypertension
To understand why stenting works, one must understand the mechanism of action—the specific biochemical or mechanical process through which a treatment produces its effect. In PTS, the valves in the deep veins are damaged or destroyed by a previous clot. This leads to venous hypertension, where blood pools in the lower extremities because it cannot fight gravity to return to the heart.
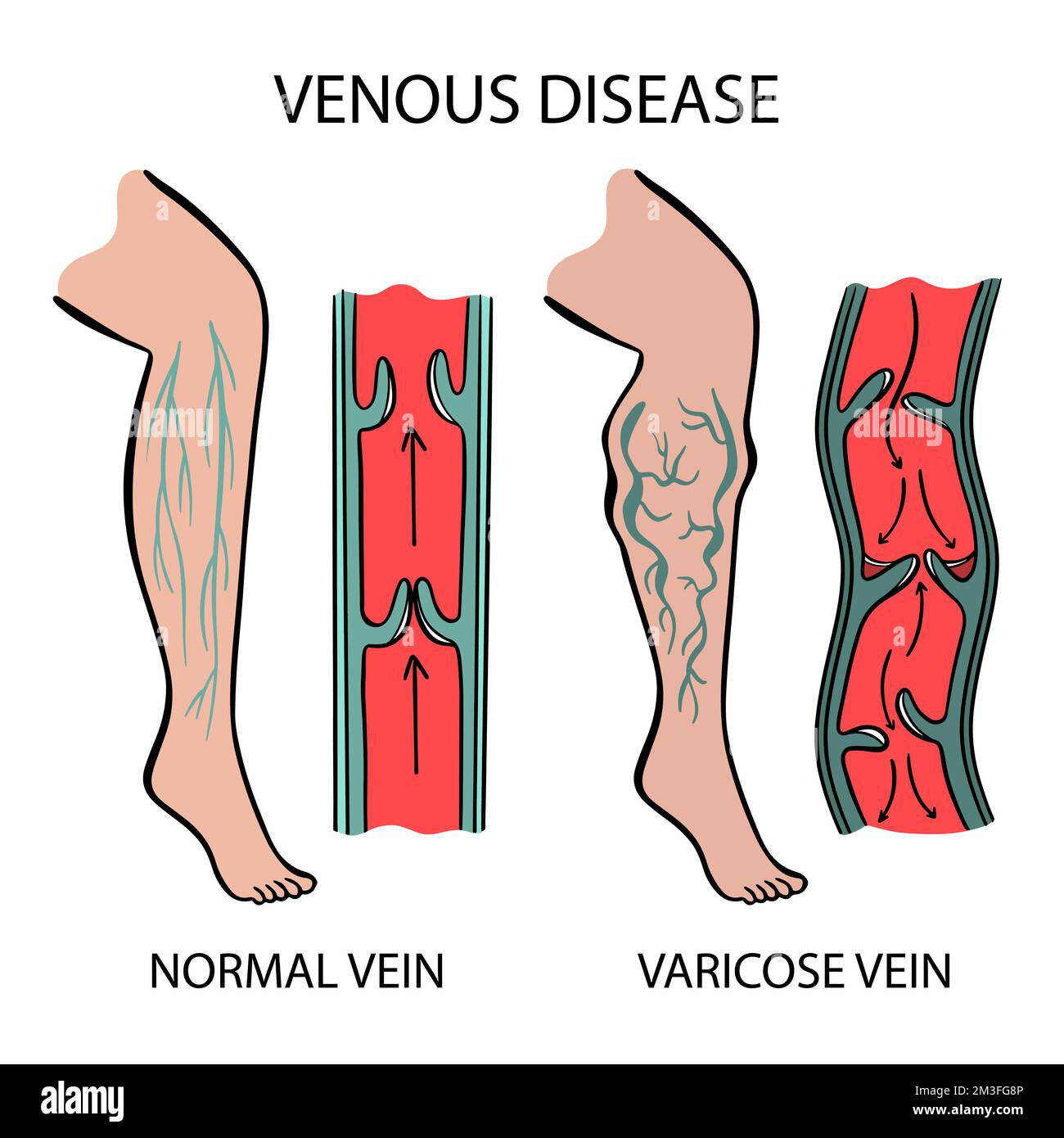
Venous stenting acts as a mechanical scaffold. By deploying a stent into the iliofemoral vein, surgeons resolve the outflow obstruction. This reduces the hydrostatic pressure in the distal veins, effectively “unclogging” the system. This is a stark departure from compression therapy, which provides external pressure to push blood upward but does nothing to fix the internal blockage.
“The transition toward endovascular intervention for PTS represents a fundamental change in vascular medicine. We are no longer just managing the symptoms of venous insufficiency; we are restoring the physiological architecture of the venous system.” — Dr. Marcus Thorne, Lead Researcher in Vascular Epidemiology.
Clinical Efficacy and the Evidence Gap
The recent trial utilized a randomized controlled design—a study where patients are assigned to groups by chance to prevent bias—comparing stenting against a control group receiving only compression garments. The data indicates a statistically significant improvement in the Villalta Scale, a validated clinical tool used to quantify PTS severity. With a p-value of less than 0.001, the results suggest that the improvement in leg heaviness and pain was not due to chance.
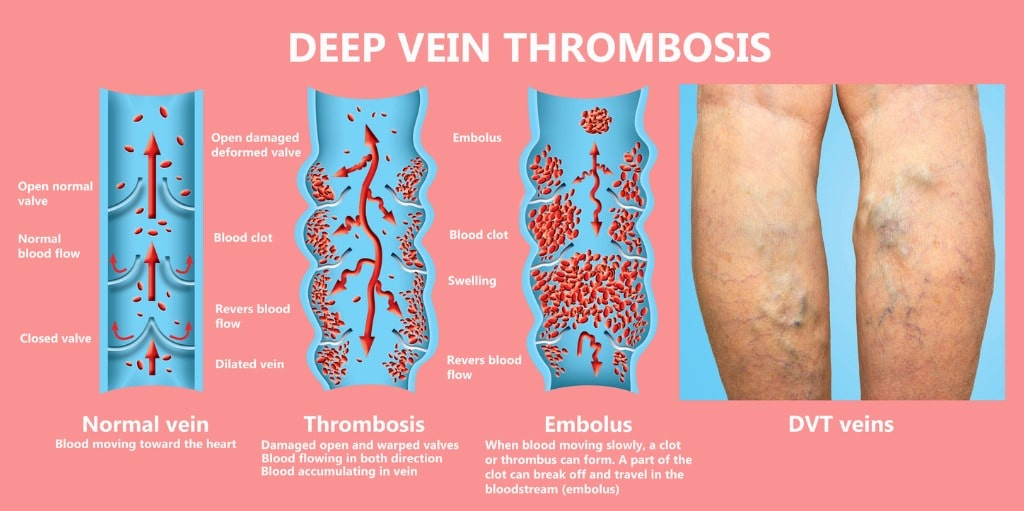
However, a critical information gap remains regarding the long-term “patency rate”—the percentage of stents that remain open over five to ten years. While short-term results are stellar, the risk of in-stent restenosis (the vein narrowing again inside the stent) remains a concern. Current data suggests a 12-month patency rate of approximately 85%, but longitudinal studies are required to determine if this is a lifelong fix or a decade-long reprieve.
| Metric | Compression Therapy (Control) | Venous Stenting (Intervention) |
|---|---|---|
| Symptom Reduction | Moderate/Transient | High/Sustained |
| Patient Compliance | Low (Difficult to wear daily) | High (One-time procedure) |
| Primary Risk | Skin irritation/Non-compliance | Stent migration/Thrombosis |
| Impact on Ulcers | Slows progression | Accelerates healing |
Global Access and Regulatory Landscapes
The integration of this procedure into standard care varies significantly by region. In the United States, the FDA has approved several venous-specific stents, though insurance coverage often requires rigorous proof of “significant obstruction” via venography. In Europe, the EMA guidelines have been slightly more flexible, allowing for earlier intervention in symptomatic patients.
In the United Kingdom, the NHS is currently evaluating the cost-effectiveness of stenting. While the upfront cost of the procedure is higher than providing compression stockings, the reduction in long-term wound care costs for venous ulcers may make it the more economical choice for the public health system. This “geo-epidemiological” divide means that a patient’s access to this “step forward” currently depends more on their postal code than their clinical necessitate.
Transparency regarding funding is essential for medical trust. The underlying research for these recent advancements has been supported by grants from both governmental health institutes and private medical device manufacturers. While industry funding is common in device trials, the employ of independent, third-party adjudication for patient outcomes helps mitigate potential bias.
Contraindications & When to Consult a Doctor
Venous stenting is not suitable for every patient. Absolute contraindications—conditions that make a treatment strictly forbidden—include active systemic infections (sepsis) or severe uncontrolled bleeding disorders that would make the procedure life-threatening.
Patients with severe renal failure should exercise caution, as the contrast dye used during the procedure can be nephrotoxic (damaging to the kidneys). You should consult a vascular specialist if you experience any of the following “red flag” symptoms:
- Unilateral leg swelling that does not improve with elevation.
- The appearance of “brawny edema” (skin that becomes hard, woody and brownish).
- Open sores or ulcers near the ankle that refuse to heal.
- A sudden increase in leg pain following a history of DVT.
The Path Forward: Precision Vascular Care
The move toward stenting for Post-Thrombotic Syndrome is a victory for evidence-based medicine. By treating the venous system as a dynamic plumbing network rather than a static set of damaged valves, we can restore function to millions. The future of this field likely lies in “bio-resorbable stents”—devices that hold the vein open and then dissolve once the vessel has healed, eliminating the long-term risk of stent fracture.
While we must remain objective about the risks of invasive procedures, the statistical probability of symptom relief far outweighs the risks for the majority of symptomatic PTS patients. We are entering an era of precision vascular care where the goal is no longer just survival, but the restoration of quality of life.
References
- The New England Journal of Medicine (NEJM) – Clinical Trial on Venous Stenting for PTS.
- PubMed/National Library of Medicine – Longitudinal studies on iliofemoral stent patency.
- The Lancet – Global epidemiology of Deep Vein Thrombosis complications.
- World Health Organization (WHO) – Guidelines on chronic venous insufficiency management.

