At the recent Retina World Congress, researchers established that the management of subretinal hemorrhage (SRH) in neovascular age-related macular degeneration (nAMD) is fundamentally dictated by lesion size. By classifying hemorrhages based on disc diameters, clinicians can now better determine the necessity of surgical intervention versus pharmacological management to preserve vision.
In Plain English: The Clinical Takeaway
- Size Matters: The physical extent of blood trapped under the retina—measured by “disc diameter”—is the primary factor in deciding if a patient needs surgery or just injections.
- Treatment Pathways: Small to medium hemorrhages may respond to anti-VEGF injections, while larger, thicker bleeds often require surgical removal to prevent permanent toxic damage to photoreceptor cells.
- Urgency is Key: Blood is toxic to the retina; early classification allows for rapid triage, which is the single most important factor in preventing irreversible vision loss.
The Pathophysiology of Subretinal Hemorrhage
In patients with neovascular age-related macular degeneration (nAMD), the growth of abnormal, fragile blood vessels—a process known as choroidal neovascularization—can lead to localized bleeding. When this blood breaches the retinal pigment epithelium and enters the subretinal space, it creates a subretinal hemorrhage (SRH). The central challenge for ophthalmologists is that blood is inherently toxic to the retina. The presence of heme (a component of hemoglobin) induces oxidative stress and iron-mediated damage to the photoreceptors, the specialized cells responsible for light detection.
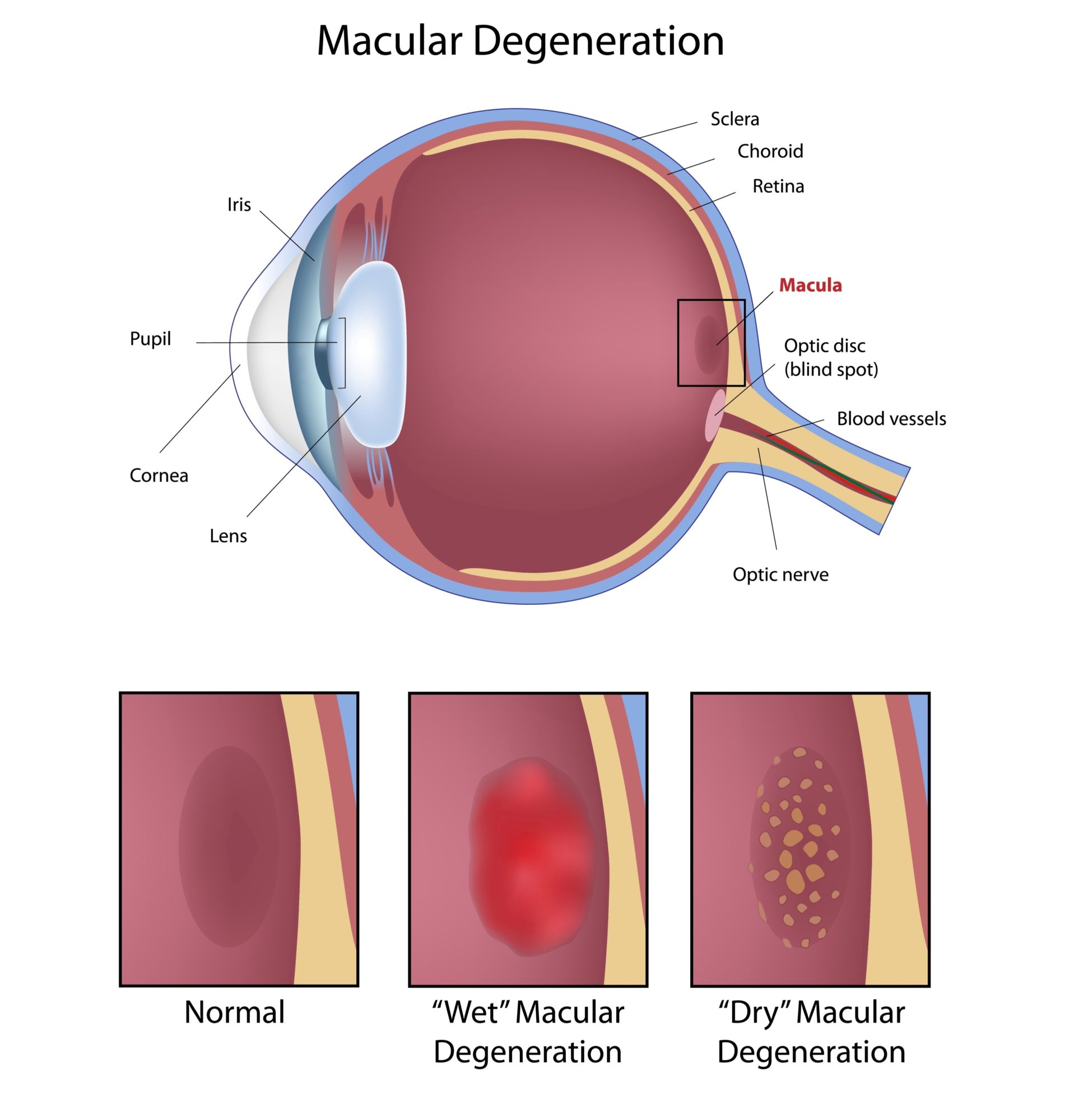
The classification system presented at the Retina World Congress provides a standardized framework for clinical decision-making. By categorizing SRH into small (1 to <4 disc diameters), medium, and large, physicians can move away from anecdotal treatment choices and toward a protocol-driven approach. This methodology is critical because the mechanism of action for treatments varies: anti-VEGF (vascular endothelial growth factor) inhibitors, such as aflibercept or ranibizumab, work by starving the neovascular membranes, while surgical vitrectomy with or without tissue plasminogen activator (tPA) is designed to physically displace the blood clot from the macula.
Clinical Evidence and Global Regulatory Perspectives
The shift toward size-based classification aligns with data seen in large-scale clinical trials investigating nAMD outcomes. While the FDA and EMA have approved several anti-VEGF agents for nAMD, the specific management of massive SRH remains a nuanced surgical sub-specialty. Large-scale studies, including those published in The Lancet, have highlighted that while anti-VEGF therapy is the gold standard for nAMD, it is often insufficient for displacing significant subretinal blood volumes, necessitating a multimodal approach.
“The prognosis for patients with subretinal hemorrhage is highly dependent on the speed of clearance. We are moving toward a paradigm where the anatomical configuration of the hemorrhage dictates the surgical urgency, rather than relying solely on visual acuity, which can be misleading in the acute phase of an event.” — Dr. Arshad Khanani, Director of Clinical Research at Sierra Eye Associates.
From a public health perspective, the burden of nAMD is rising globally as the population ages. In the United Kingdom, the NHS has integrated strict monitoring protocols for patients receiving long-term anti-VEGF therapy. However, the geographic variability in access to vitreoretinal surgery—the specialized procedure required for large SRH—remains a barrier to equitable care. Patients in rural or underserved regions may experience delays in triage, which directly correlates with poorer long-term visual outcomes.
| Hemorrhage Size (Disc Diameter) | Recommended Primary Strategy | Mechanism of Action |
|---|---|---|
| Small (1 to <4 DD) | Anti-VEGF Monotherapy | Inhibition of new vessel growth; gradual resorption |
| Medium (4 to 8 DD) | Combined Anti-VEGF + Gas Bubble | Displacement of blood via pneumatic tamponade |
| Large (>8 DD) | Surgical Vitrectomy + tPA | Mechanical removal of clot and toxic heme |
Funding and Research Integrity
The research presented regarding SRH classification is supported by ongoing investigations into retinal vascular diseases. It is essential for patients to note that while many clinical trials are sponsored by pharmaceutical entities—such as Regeneron or Genentech—the classification models themselves are the result of academic collaboration among retina specialists. Transparency in these disclosures remains a cornerstone of the medical community’s commitment to objective, patient-centered care.

Contraindications & When to Consult a Doctor
Patients currently receiving treatment for nAMD must remain vigilant. While anti-VEGF injections are generally safe, they carry rare risks of endophthalmitis (a severe intraocular infection) or retinal detachment. Surgical intervention for large SRH is contraindicated in patients with uncontrolled systemic hypertension or those on anticoagulation therapy without proper medical clearance.
Seek immediate emergency ophthalmic care if you experience:
- A sudden, dramatic “curtain-like” loss of vision in one eye.
- The sudden onset of new, dark “floaters” or a localized red patch in your field of vision.
- Persistent metamorphopsia (straight lines appearing wavy) that worsens significantly over a period of 24–48 hours.
Early intervention is the only way to mitigate the toxic effects of subretinal blood. If you are currently under the care of a retina specialist, ensure you have a clear plan for how your clinic manages acute hemorrhagic events. As we move through 2026, the adoption of standardized classification for SRH will likely become a benchmark for quality care in ophthalmology practices worldwide.
References
- Journal of VitreoRetinal Diseases: Clinical management of massive subretinal hemorrhage.
- The Lancet: Global epidemiology and treatment trends in neovascular age-related macular degeneration.
- American Academy of Ophthalmology: Preferred Practice Pattern for Age-Related Macular Degeneration.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.

