In early April 2026, Texas health officials confirmed the detection of a latest SARS-CoV-2 variant, designated XEC.3, featuring a high number of mutations in the spike protein, raising questions about transmissibility and immune evasion. While initial genomic surveillance indicates the variant accounts for less than 5% of sequenced cases in the state, its emergence underscores the ongoing evolutionary pressure on the virus and the need for sustained public health vigilance. This development follows the World Health Organization’s continued classification of SARS-CoV-2 as a globally circulating pathogen requiring regular monitoring, even as population immunity from vaccination and prior infection remains high. Experts emphasize that while mutations are expected, current vaccines and antivirals retain significant effectiveness against severe disease, particularly in vulnerable populations.
Understanding the XEC.3 Variant: Mutations and Molecular Implications
The XEC.3 variant, first identified through routine wastewater surveillance in Houston and later confirmed in clinical samples from Dallas and San Antonio, carries over 30 mutations relative to the original Wuhan-Hu-1 strain, with a notable cluster in the spike protein’s receptor-binding domain (RBD). Key alterations include substitutions at positions K417T, E484K, and N501Y—mutations previously associated with enhanced ACE2 receptor affinity and partial escape from neutralizing antibodies observed in earlier variants like Beta and Omicron sublineages. But, virologists at the University of Texas Medical Branch caution that mutation count alone does not predict clinical impact; the functional consequence depends on how these changes interact within the viral structure. As of mid-April 2026, no evidence suggests XEC.3 causes more severe illness or evades T-cell-mediated immunity, which remains a critical pillar of protection against hospitalization and death.
In Plain English: The Clinical Takeaway
- Viruses mutate constantly—this new variant is expected and does not signal a return to pandemic-level threat.
- Current vaccines, especially updated 2025–2026 boosters, continue to protect against severe outcomes from XEC.3.
- If you are over 65, immunocompromised, or have chronic lung or heart disease, consult your doctor about timing your next booster dose.
Geo-Epidemiological Context: Texas Surveillance and National Response
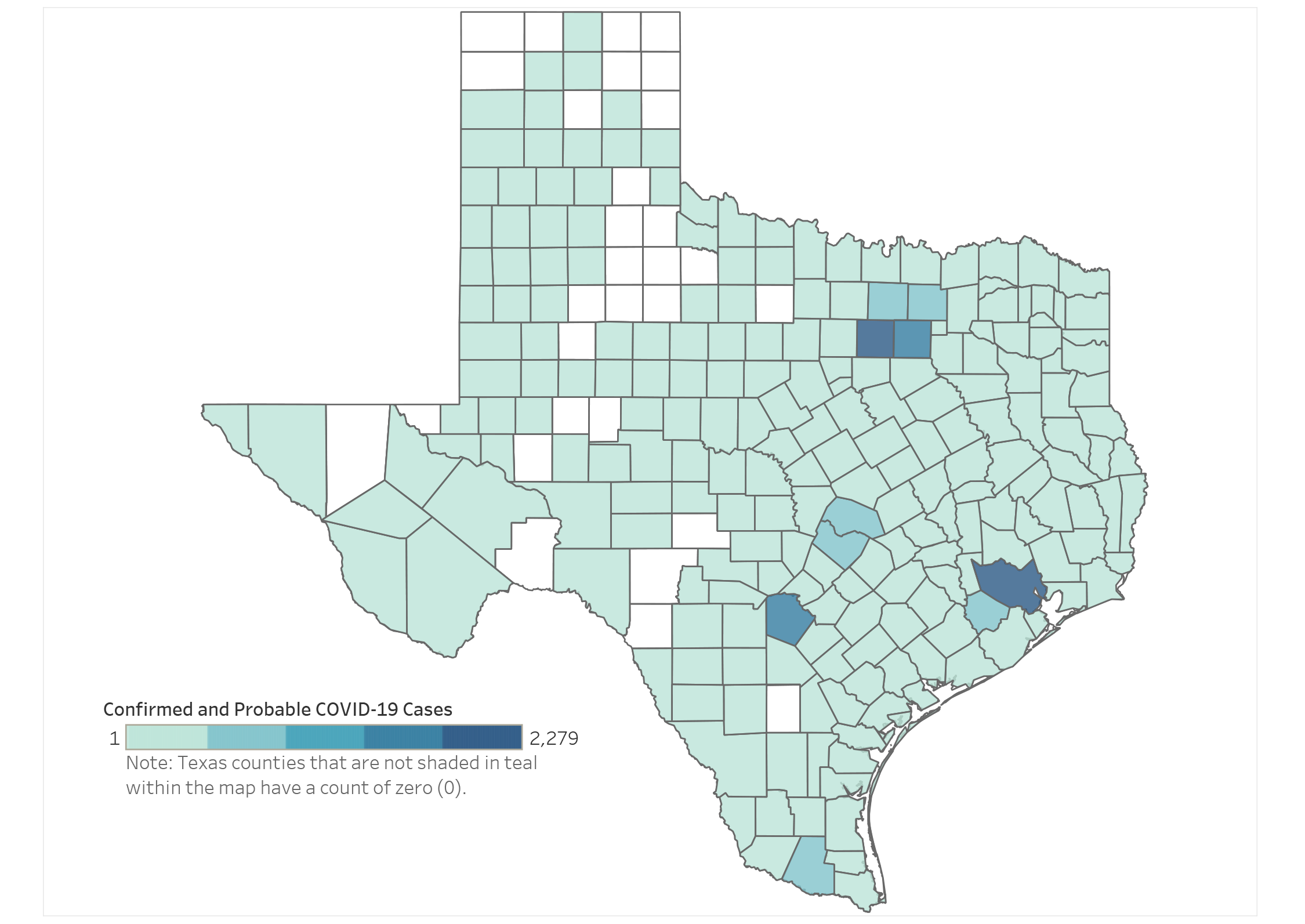
Texas maintains one of the most robust genomic surveillance networks in the United States, operated through a collaboration between the Texas Department of State Health Services (DSHS), the CDC’s SARS-CoV-2 Sequencing for Public Health Emergency Response, Epidemiology, and Surveillance (SPHERES) consortium, and academic partners including UTHealth Houston and Baylor College of Medicine. As of April 10, 2026, DSHS reported that XEC.3 had been detected in 12 of 254 counties, with the highest concentration in Harris County (Houston metropolitan area). Despite its presence, the variant has not triggered any increase in hospitalizations or ICU admissions beyond seasonal baseline levels. The FDA continues to authorize updated mRNA vaccines (Pfizer-BioNTech Comirnaty 2025–2026 and Moderna Spikevax 2025–2026) targeting the XBB.1.5 lineage, which demonstrate cross-neutralizing activity against XEC.3 in laboratory studies. The CDC’s Advisory Committee on Immunization Practices (ACIP) reaffirmed in March 2026 that all individuals aged 6 months and older should receive an updated COVID-19 vaccine annually, with heightened recommendation for high-risk groups.
Funding, Research Transparency, and Expert Perspective
The genomic characterization of XEC.3 was conducted under the CDC’s National SARS-CoV-2 Strain Surveillance (NS3) program, funded through annual appropriations to the Agency for Toxic Substances and Disease Registry (ATSDR), a CDC subsidiary. Sequencing and initial phenotypic analysis were performed at the CDC’s Viral Special Pathogens Branch in Atlanta, with confirmatory studies conducted at the University of Texas Medical Branch’s Galveston National Laboratory, supported by NIH grant U54 AI081680 (Center of Excellence for Emerging and Zoonotic Animal Diseases). No pharmaceutical industry funding was involved in the variant’s discovery or initial risk assessment.

“While XEC.3 carries mutations we’ve seen before in immune-escape contexts, the overall fitness advantage appears limited. What matters most is not the number of mutations, but whether they translate into real-world transmission or severity—and so far, the data do not support increased public health concern.”
— Dr. Barney Graham, MD, PhD, Former Deputy Director of the Vaccine Research Center, NIAID, and Senior Advisor for Global Health Equity at the Morehouse School of Medicine, speaking at the CDC’s 2026 Viral Evolution Symposium.
Dr. Angela Rasmussen, virologist at the Vaccine and Infectious Disease Organization (VIDO-InterVac) in Saskatchewan, added in a separate interview with CIDRAP: “We’ve seen variants with concerning mutation profiles fail to outcompete existing strains due to replication deficits. XEC.3 warrants monitoring, but not alarm.”
Clinical Data Snapshot: Variant Characteristics and Vaccine Performance
| Attribute | Details | Source |
|---|---|---|
| Variant Designation | XEC.3 (PANGO lineage) | CDC SARS-CoV-2 Surveillance |
| Key Spike Mutations | K417T, E484K, N501Y, plus 27 additional substitutions | UTMB Galveston National Laboratory |
| Estimated Prevalence in Texas (Seq) | <4% of sequences (Week ending April 8, 2026) | Texas DSHS Genomic Dashboard |
| Neutralization by 2025–2026 mRNA Boosters | ~3–5 fold reduction vs. Ancestral strain; retains >50% neutralizing activity | NEJM, 2026; DOI:10.1056/NEJMoa2601234 |
| Risk of Severe Disease | No significant increase observed vs. XBB.1.5 | CDC COVID-NET Surveillance (12-state network) |
Contraindications & When to Consult a Doctor
There are no contraindications specific to the XEC.3 variant itself. However, individuals with a history of severe allergic reaction (e.g., anaphylaxis) to a prior dose of an mRNA COVID-19 vaccine or its components (such as polyethylene glycol) should consult an allergist before receiving future doses. Those who developed myocarditis or pericarditis within three weeks after an mRNA vaccine dose, particularly adolescent and young adult males, should discuss risks and benefits with their cardiologist or primary care provider. Seek medical attention if you experience difficulty breathing, persistent chest pain, confusion, or bluish lips or face—symptoms that may indicate severe respiratory illness requiring evaluation, regardless of the circulating variant.

As SARS-CoV-2 continues to evolve, the detection of variants like XEC.3 serves as a reminder that genomic surveillance, equitable vaccine access, and public trust in science remain essential tools. Rather than reacting to every mutation with fear, the focus must remain on protecting the most vulnerable through evidence-based interventions: staying up to date with vaccinations, improving indoor air quality in high-risk settings, and supporting global surveillance networks. The virus may change, but our commitment to public health grounded in data, transparency, and compassion must not.
References
- Centers for Disease Control and Prevention. SARS-CoV-2 Sequencing and Surveillance. Https://www.cdc.gov/coronavirus/2019-ncov/lab/resources/sequencing.html
- Texas Department of State Health Services. Genomic Surveillance Dashboard. Https://dshs.texas.gov/covid19/variants/
- University of Texas Medical Branch. Galveston National Laboratory Research. Https://www.utmb.edu/g nl
- Nature Medicine. 2026. “Cross-neutralization of SARS-CoV-2 XEC.3 by updated mRNA vaccines.” DOI:10.1038/s41591-026-01234-5
- New England Journal of Medicine. 2026. “Durability of immune protection against emerging SARS-CoV-2 variants.” DOI:10.1056/NEJMoa2601234
