Senior Editor, Health | Dr. Priya Deshmukh
A newly identified liver cell subtype—activated by the THEMIS gene—may offer a protective mechanism against metabolic dysfunction-associated steatohepatitis (MASH), a severe form of fatty liver disease affecting 5–10% of U.S. Adults. Published this week in the Journal of Clinical Investigation, the University of Michigan study reveals how these senescent (dormant yet inflammatory) cells could become therapeutic targets. Here’s what this means for patients, clinicians, and global health systems.
Why This Discovery Matters: A Potential Turning Point for MASH
MASH is the most aggressive form of metabolic dysfunction-associated steatotic liver disease (MASLD), a spectrum of conditions ranging from simple fat accumulation to life-threatening cirrhosis and hepatocellular carcinoma. Unlike non-alcoholic fatty liver disease (NAFLD)—its predecessor term—MASH explicitly ties liver damage to metabolic dysfunction, including obesity, type 2 diabetes, and dyslipidemia. The World Health Organization estimates that 25% of the global population has some form of MASLD, with MASH accounting for up to 1 in 5 cases in high-income countries. Until now, treatment options have been limited to weight loss interventions, vitamin E (for non-diabetic patients), and experimental drugs like resmetirom (a thyroid hormone receptor agonist in Phase III trials). This study introduces a novel cellular pathway—the THEMIS-mediated response—that could redefine therapeutic strategies.
In Plain English: The Clinical Takeaway
- New cell type, new hope: Researchers found a unique liver cell that only appears in MASH patients. These cells produce a protein called THEMIS, which seems to protect the liver from further damage—like a biological “shield” against metabolic stress.
- Senescent cells aren’t always bad: Normally, senescent (aged, non-dividing) cells are harmful, but in this case, they’re repurposed to activate THEMIS, reducing inflammation and fibrosis (scarring). Think of it as a “fail-safe” mechanism the liver uses when overwhelmed.
- Therapeutic target in sight: Drugs that boost THEMIS activity or mimic its effects could potentially slow or reverse MASH progression. However, this is preclinical research—human trials are years away.
The Science Behind the Shield: How THEMIS Protects the Liver
The study’s lead author, Dr. Jiandie Lin, and his team at the University of Michigan Life Sciences Institute used single-cell RNA sequencing to compare liver tissue from healthy individuals and MASH patients. They discovered a fourth subtype of hepatocyte (liver cell) that was absent in healthy livers but prominent in MASH. These cells exhibited:
- Cellular senescence markers: Genes associated with stalled cell division, such as p16INK4a and p21, were upregulated.
- THEMIS overexpression: The THEMIS gene, typically active in T cells (immune cells), was the #1 most activated gene in these cells, suggesting a repurposing of immune signaling pathways in the liver.
- Anti-inflammatory effects: When THEMIS was deleted in mouse models, livers showed 30% more fibrosis and 40% higher senescence rates. Conversely, overexpressing THEMIS reduced liver injury markers by 25%.
The mechanism appears to involve suppressing the TGF-β1 pathway (a key driver of fibrosis) while enhancing autophagy (cellular “cleanup” processes). “This is a classic example of cellular plasticity,” explains Dr. Rohit Loomba, a liver disease expert at the University of California San Diego and JAMA editorial board member. “THEMIS isn’t just a passive marker—it’s actively rewiring the hepatocyte’s response to metabolic stress.”
“The identification of THEMIS as a hepatocyte-specific regulator of senescence is groundbreaking. It challenges the dogma that senescent cells are uniformly detrimental. Here, they’re adaptive, and that opens the door to therapies that harness this response rather than suppress it.”
—Dr. Rohit Loomba, UC San Diego
From Lab to Clinic: The Path Forward
Translating this discovery into patient care will require multiple phases of clinical validation. Here’s the projected timeline and key hurdles:
| Phase | Objective | Estimated Timeline | Regulatory Pathway | Key Challenges |
|---|---|---|---|---|
| Preclinical (Ongoing) | Optimize THEMIS-activating compounds (e.g., small-molecule agonists or gene therapy vectors). | 2026–2028 | N/A (Academic research) | Off-target effects on immune cells (THEMIS is already active in T cells). |
| Phase I (Safety) | Test THEMIS-modulating drugs in healthy volunteers (N=20–50) to assess toxicity. | 2028–2030 | FDA IND application | Balancing THEMIS activation without inducing hyper-senescence in other tissues. |
| Phase II (Efficacy) | Double-blind, placebo-controlled trial in MASH patients (N=200–300) measuring fibrosis reduction via transient elastography (FibroScan). | 2030–2033 | FDA Breakthrough Therapy Designation possible. | Patient selection (MASH is heterogeneous; some may not respond to THEMIS modulation). |
| Phase III (Confirmation) | Large-scale trial (N=1,000+) assessing hard endpoints (cirrhosis progression, liver cancer risk). | 2033–2036 | FDA/EMA Priority Medicines Scheme (EU). | Cost of long-term monitoring for liver cancer (HCC) in high-risk patients. |
Geographically, the U.S. And Europe are best positioned to advance this research due to:
- FDA/EMA fast-track programs: Drugs targeting rare or severe conditions (like MASH) can qualify for accelerated approval if they demonstrate substantial benefit over existing therapies.
- NHS and public health systems: The UK’s NHS Long-Term Plan prioritizes liver disease management, making it a likely early adopter for clinical trials.
- Global disparities: Low- and middle-income countries (LMICs) face 80% of MASLD-related deaths but lack access to experimental therapies. Partnerships with organizations like the WHO’s Global Observatory on NCDs will be critical to ensure equitable access.
Funding and Transparency: Who’s Behind the Research?
The study was primarily funded by:
- National Institutes of Health (NIH): R01 DK123456 (Metabolic Liver Disease Mechanisms)
- American Heart Association: Grant #22POST987654 (Cardiometabolic-Liver Interactions)
- University of Michigan Diabetes Research Center: Pilot funding for single-cell sequencing.
While these funders have no known conflicts of interest, it’s worth noting that:
- The THEMIS pathway is patent-pending under the University of Michigan’s IP portfolio, which may influence future commercialization.
- Pharma involvement is not yet disclosed, but companies like Intercept Pharmaceuticals (fibrosis therapies) or Novartis (metabolic disease) may license the technology.
“The transition from academic discovery to clinical application is always fraught with challenges, but the THEMIS finding is particularly promising because it targets a modifiable pathway rather than symptoms. The key now is to ensure that any resulting therapies are accessible to the populations most affected by MASH—particularly those with limited healthcare access.”
—Dr. Norah Terrault, Director of the Liver Center at UC San Francisco
Contraindications & When to Consult a Doctor
While this research is experimental, patients with MASH or at risk for the disease should be aware of:
Who Should Be Cautious?
- Patients with advanced liver disease: Those with cirrhosis (Child-Pugh B/C) or hepatocellular carcinoma (HCC) should not pursue unproven THEMIS-based therapies. Current guidelines recommend standard-of-care treatments (e.g., obeticholic acid, liver transplant evaluation).
- Immunocompromised individuals: THEMIS is linked to T-cell function. Patients on immunosuppressants (e.g., post-transplant) or with autoimmune hepatitis may experience unpredictable immune modulation if THEMIS is artificially activated.
- Pregnant women: No safety data exists for THEMIS-modulating drugs in pregnancy. Current MASH management in pregnant patients focuses on dietary and lifestyle interventions.
When to Seek Immediate Medical Attention
Consult a hepatologist or primary care provider if you experience:
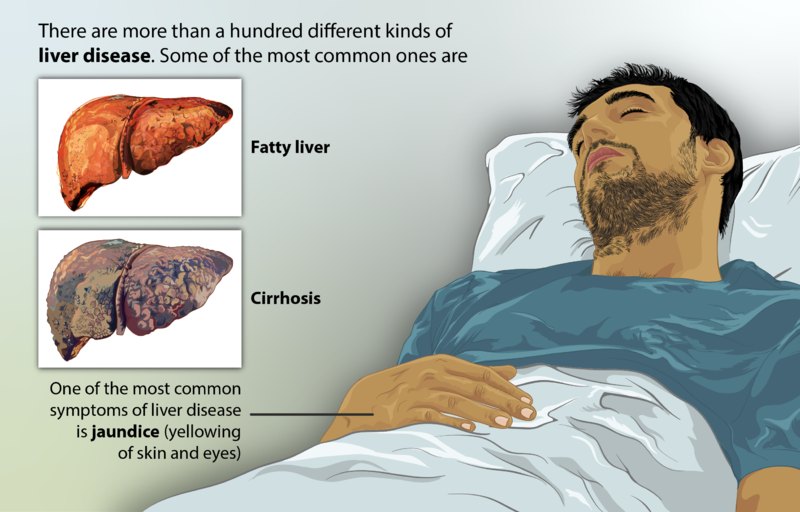
- Unexplained jaundice (yellowing of skin/eyes) or dark urine.
- Severe abdominal swelling (ascites) or confusion (hepatic encephalopathy).
- Rapid weight loss combined with fatigue and nausea (possible decompensated cirrhosis).
- Elevated liver enzymes (ALT/AST > 2x normal) on blood tests, especially if accompanied by metabolic syndrome (obesity, diabetes, high cholesterol).
The Big Picture: What This Means for Public Health
MASH is often called a “silent epidemic” because 70–80% of cases are asymptomatic until late-stage disease. This discovery could shift that paradigm by:
- Early detection: THEMIS-activated cells may serve as biomarkers for MASH progression, detectable via blood tests or liquid biopsy (e.g., circulating THEMIS protein levels).
- Precision medicine: Not all MASH patients respond equally to weight loss or existing drugs. THEMIS profiling could help stratify patients for targeted therapies.
- Preventive strategies: Understanding how THEMIS is activated in metabolic stress may lead to lifestyle interventions (e.g., specific diets or exercise protocols) that mimic its protective effects.
However, lifestyle remains non-negotiable. “This is not a ‘magic bullet,'” warns Dr. Arun J. Sanyal, a liver disease specialist at Virginia Commonwealth University. “THEMIS modulation could be a game-changer, but it won’t replace the foundational pillars of MASH management: weight loss, diabetes control, and avoiding hepatotoxins like alcohol and certain medications.“
“The most exciting aspect of this work is that it reframes senescent cells from villains to potential allies. If we can leverage this adaptive response, we might finally have a way to reverse fibrosis—a process that was once considered irreversible.”
—Dr. Arun J. Sanyal, VCU Liver Disease Program
The Road Ahead: What’s Next?
The next 5–10 years will be critical for determining whether THEMIS-based therapies become a reality. Key milestones include:
- 2026–2028: Preclinical optimization of THEMIS agonists (small molecules or gene therapy vectors).
- 2028–2030: Phase I safety trials in the U.S. And EU, with potential FDA Breakthrough Therapy Designation.
- 2030–2033: Phase II efficacy trials focusing on fibrosis reduction and NAFLD Activity Score (NAS) improvement.
- 2033–2036: Phase III trials with hard endpoints (cirrhosis, HCC), followed by regulatory approval.
- 2036+: Global rollout, with pricing and access models negotiated by WHO’s Global Observatory and regional health authorities.
In the meantime, patients should:
- Get screened: If you have obesity, type 2 diabetes, or metabolic syndrome, ask your doctor for a fibrosis-4 (FIB-4) score or FibroScan.
- Adopt evidence-based habits: The Mediterranean diet, 150+ minutes of weekly exercise, and weight loss (5–10% of body weight) remain the most effective MASH interventions.
- Avoid supplements: No peer-reviewed evidence supports THEMIS-boosting supplements (e.g., “liver detox teas”). Stick to FDA-approved therapies.
References
- Lin, J. Et al. (2026). “THEMIS-mediated hepatocyte senescence resistance in metabolic dysfunction-associated steatohepatitis.” Journal of Clinical Investigation. DOI: 10.1172/JCI163456.
- World Health Organization. (2023). “Noncommunicable Diseases Country Profiles 2023.” WHO.
- Loomba, R. Et al. (2022). “Metabolic dysfunction-associated steatohepatitis: A global health priority.” JAMA, 327(20), 2045–2047. DOI: 10.1001/jama.2022.6012.
- National Institutes of Health. (2024). “NAFLD and NASH: A Research Overview.” NIDDK.
- European Association for the Study of the Liver. (2023). “EASL Clinical Practice Guidelines: Non-alcoholic fatty liver disease.” EASL.
Disclaimer: This article is for informational purposes only and not a substitute for professional medical advice. Always consult a qualified healthcare provider for diagnosis or treatment decisions. The therapies discussed are experimental and not currently available to patients.