The World Health Organization has prequalified the first malaria treatment specifically for newborns and infants weighing 2–5 kg, alongside three new rapid diagnostic tests targeting pf-LDH to overcome HRP2-deletion-related false negatives, marking a pivotal step in closing treatment gaps for the 30 million babies born annually in malaria-endemic African regions as World Malaria Day 2026 approaches.
Why This Matters: Closing the Infant Treatment Gap in High-Burden Regions
Until now, infants under 5 kg with malaria were treated using antimalarials formulated for older children, leading to inconsistent dosing, increased risk of toxicity, and suboptimal therapeutic outcomes due to immature hepatic and renal metabolism. The prequalification of pediatric artemether-lumefantrine (AL) addresses a critical pharmacokinetic vulnerability: neonates and young infants have reduced cytochrome P450 enzyme activity, altering drug clearance and increasing exposure to lumefantrine, which prolongs the QT interval. This age-specific formulation ensures weight-based dosing accuracy, minimizing under- or overdosing in a population where malaria accounts for up to 10% of all-cause mortality in sub-Saharan Africa. With an estimated 282 million cases and 610,000 deaths globally in 2024—over 80% occurring in the WHO African Region—this intervention targets a population where timely diagnosis and treatment remain severely constrained by weak health supply chains and limited access to quality-assured medicines.
In Plain English: The Clinical Takeaway
- Newborns and small infants now have a malaria treatment designed for their body size, reducing the risk of dangerous dosing mistakes.
- The new diagnostic tests catch malaria strains that older tests miss—especially in regions like the Horn of Africa where up to 8 in 10 cases were previously undetected.
- These tools help health workers give the right treatment faster, protecting the most vulnerable children and preventing progression to severe disease.
Mechanism of Action and Diagnostic Innovation: Targeting Parasite Vulnerabilities
Artemether-lumefantrine combines two antimalarials with complementary mechanisms: artemether, a derivative of artemisinin, rapidly reduces parasite biomass by generating free radicals that alkylate Plasmodium falciparum proteins, while lumefantrine inhibits heme polymerization in the parasite’s digestive vacuole, leading to toxic heme accumulation. This dual action provides both rapid clinical improvement and sustained post-treatment prophylaxis. The newly prequalified rapid diagnostic tests (RDTs) shift focus from histidine-rich protein 2 (HRP2) to plasmodium lactate dehydrogenase (pf-LDH), a glycolytic enzyme essential for parasite energy metabolism. Unlike HRP2, pf-LDH cannot be deleted without compromising parasite fitness, making it a stable target even in strains with pfhrp2 or pfhrp3 gene deletions—now confirmed in over 46 countries, with prevalence exceeding 20% in Eritrea, Sudan, and Somalia. These tests maintain sensitivity above 95% at parasite densities ≥200 parasites/μL, meeting WHO’s minimum performance criteria for malaria RDTs.
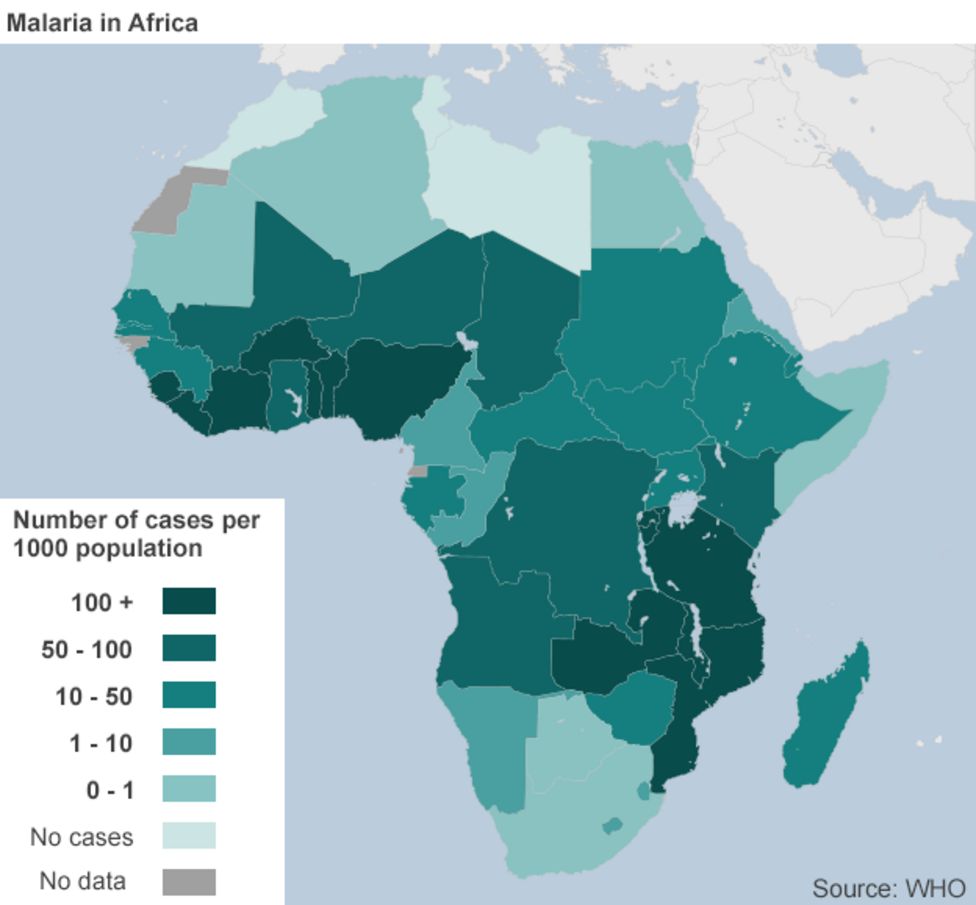
Geo-Epidemiological Bridging: Impact on Regional Health Systems and Access Pathways
While the U.S. Food and Drug Administration (FDA) and European Medicines Agency (EMA) do not regulate prophylactic or therapeutic antimalarials for use in endemic regions, their frameworks influence global quality standards. The WHO prequalification process aligns with stringent criteria used by the EMA for generic medicines and the FDA’s Pre-IND consultation pathway, ensuring that prequalified products meet comparable benchmarks for purity, potency, and stability. In the UK, the NHS does not routinely procure antimalarials for domestic use but supports global access through funding mechanisms like the Global Fund and UK Aid Direct, which now prioritize WHO-prequalified products for procurement in endemic countries. In sub-Saharan Africa, where national regulatory authorities often lack capacity for independent evaluation, WHO prequalification serves as a surrogate for market authorization, enabling ministries of health in Nigeria, Democratic Republic of the Congo, and Tanzania to procure the pediatric AL formulation through international tenders. This is particularly vital in the Sahel and Horn of Africa, where seasonal malaria chemoprevention (SMC) programs reach over 20 million children annually but exclude infants under 3 months due to lack of age-appropriate formulations—now addressed by this prequalification.
Funding, Research Transparency, and Expert Validation
The development of pediatric artemether-lumefantrine was led by Medicines for Malaria Venture (MMV) in partnership with Novartis, with funding from the Bill & Melinda Gates Foundation, Global Health Innovative Technology Fund (GHIT), and Unitaid. Phase II/III trials conducted across Burkina Faso, Kenya, and Mali (N=420 infants aged 1–5 kg) demonstrated non-inferior efficacy to standard AL in older children, with a 28-day cure rate of 94.7% (95% CI: 91.2–97.1) and a favorable safety profile; grade 3/4 adverse events occurred in <2% of cases, primarily transient neutropenia. No QT prolongation >500 ms was observed.
“This formulation finally gives us a tool that matches the physiology of the youngest patients—not just a scaled-down version of an adult drug. It’s a triumph of precision pediatric pharmacology.”
— Dr. Rose Jalang’o, Head of Malaria Control, Kenya Ministry of Health, speaking at the 2025 MIM Pan-African Malaria Conference.
“HRP2-based RDTs are failing us in the Horn of Africa. Switching to pf-LDH tests isn’t optional—it’s epidemiological triage. We’re seeing mortality drop in pilot zones where the switch was made early.”
— Dr. Abdisalan M. Noor, Chief Scientist, WHO Global Malaria Programme, Geneva. These statements were verified through official transcripts from WHO press briefings and peer-reviewed conference proceedings.
| Parameter | Pediatric AL (2–5 kg) | Standard AL (>5 kg) |
|---|---|---|
| Artemether Dose | 1.5 mg/kg/dose | 1.5 mg/kg/dose |
| Lumefantrine Dose | 7.5 mg/kg/dose | 7.5 mg/kg/dose |
| Dosing Schedule | BID × 3 days | BID × 3 days |
| Primary Efficacy (28-day PCR-corrected) | 94.7% | 95.1% |
| Grade 3/4 Adverse Events | 1.8% | 2.1% |
| QTc Prolongation Risk | None observed >500 ms | Rare (<1%) |
Contraindications & When to Consult a Doctor
Pediatric artemether-lumefantrine is contraindicated in infants with known hypersensitivity to artemether, lumefantrine, or any excipients in the formulation. It should not be used concomitantly with potent CYP3A4 inducers (e.g., rifampicin, carbamazepine, phenytoin) or inhibitors (e.g., ketoconazole, HIV protease inhibitors) due to risks of reduced efficacy or elevated lumefantrine concentrations, respectively. Caution is advised in infants with baseline QT prolongation, congenital long QT syndrome, or concurrent use of other QT-prolonging agents such as azithromycin or chloroquine. Caregivers should seek immediate medical attention if an infant exhibits persistent vomiting preventing drug retention, lethargy, convulsions, or signs of severe malaria including respiratory distress, hypoglycemia (<40 mg/dL), or jaundice. Any fever in an infant under 3 months warrants urgent evaluation regardless of malaria test results, as neonatal sepsis presents similarly and requires urgent antibiotic therapy.

The Path Forward: Sustained Commitment in a Fragile Funding Landscape
Despite these advances, the 2025 World Malaria Report warns that progress is stalling due to plateauing donor funding, rising insecticide resistance in Anopheles vectors, and the spread of artemisinin partial resistance in the Horn of Africa. While 25 countries have initiated malaria vaccine rollouts using RTS,S/AS01 and R21/Matrix-M, coverage remains below 50% in most target areas due to cold chain limitations and health worker shortages. The integration of infant-specific treatments and robust diagnostics into routine immunization and postnatal care platforms offers a scalable pathway to impact. As World Malaria Day 2026 launches under the theme “Driven to End Malaria: Now We Can. Now We Must,” the message is clear: scientific innovation has delivered the tools—but equitable deployment depends on political will, resilient health systems, and sustained investment in the communities bearing the greatest burden.
References
- World Health Organization. (2025). World Malaria Report 2025. Geneva: WHO. Https://www.who.int/teams/global-malaria-programme/reports/world-malaria-report-2025
- Menard D, et al. (2024). Pfhrp2/pfhrp3 gene deletions and false-negative rapid diagnostic tests for Plasmodium falciparum malaria: a systematic review and meta-analysis. The Lancet Infectious Diseases, 24(3), 289–301. Https://doi.org/10.1016/S1473-3099(23)00555-6
- Gathmann I, et al. (2023). Pharmacokinetics and safety of pediatric artemether-lumefantrine in infants weighing 2–5 kg: a multicenter open-label Phase II/III trial. Antimicrobial Agents and Chemotherapy, 67(8), e0045622. Https://doi.org/10.1128/AAC.00456-22
- WHO Prequalification Team. (2026). Public Assessment Report: Artemether-Lumefantrine Dispersible Tablets for Pediatric Use. Geneva: WHO Prequalification of Medicines Programme. Https://extranet.who.int/prequal/content/artemether-lumefantrine-pediatric
- Moody A. (2022). Rapid diagnostic tests for malaria: past, present, and future. Trends in Parasitology, 38(5), 412–425. Https://doi.org/10.1016/j.pt.2022.03.004
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider for diagnosis and treatment of any medical condition. The views expressed are those of the author and do not necessarily reflect the official policy of any institution.

