Orlando Health has begun construction of its latest Weight Loss and Bariatric Surgery Institute at the downtown Orlando campus, a strategic expansion aimed at addressing Florida’s rising obesity epidemic through evidence-based surgical and multidisciplinary care. The facility will integrate bariatric procedures such as Roux-en-Y gastric bypass and sleeve gastrectomy with metabolic monitoring, nutritional counseling, and long-term behavioral support, targeting adults with a body mass index (BMI) ≥40 or ≥35 with obesity-related comorbidities like type 2 diabetes or hypertension. This initiative responds to CDC data showing over 30% of Florida adults are obese, a condition linked to increased risks of cardiovascular disease, certain cancers, and reduced life expectancy.
Why This Institute Matters for Central Florida’s Public Health Landscape
The new institute represents more than just added surgical capacity—it reflects a systemic shift toward recognizing obesity as a chronic metabolic disease requiring coordinated, long-term management. With Florida ranking among the top 10 states for obesity prevalence and related healthcare costs exceeding $12 billion annually, centralized centers like this one aim to reduce fragmented care and improve access to guideline-recommended interventions. Bariatric surgery remains the most effective long-term treatment for severe obesity, with studies showing sustained weight loss of 20-30% of total body weight at 10 years post-surgery, alongside remission rates of type 2 diabetes exceeding 60% in select populations.
In Plain English: The Clinical Takeaway
- Bariatric surgery is not a cosmetic procedure—it alters gut hormones and metabolism to reduce hunger and improve blood sugar control.
- Patients typically lose 50-70% of their excess weight within two years, but lifelong follow-up is essential to prevent nutritional deficiencies and weight regain.
- Eligibility requires failed attempts at diet and exercise, psychological evaluation, and commitment to permanent lifestyle changes.
Clinical Evidence Behind the Procedures Offered
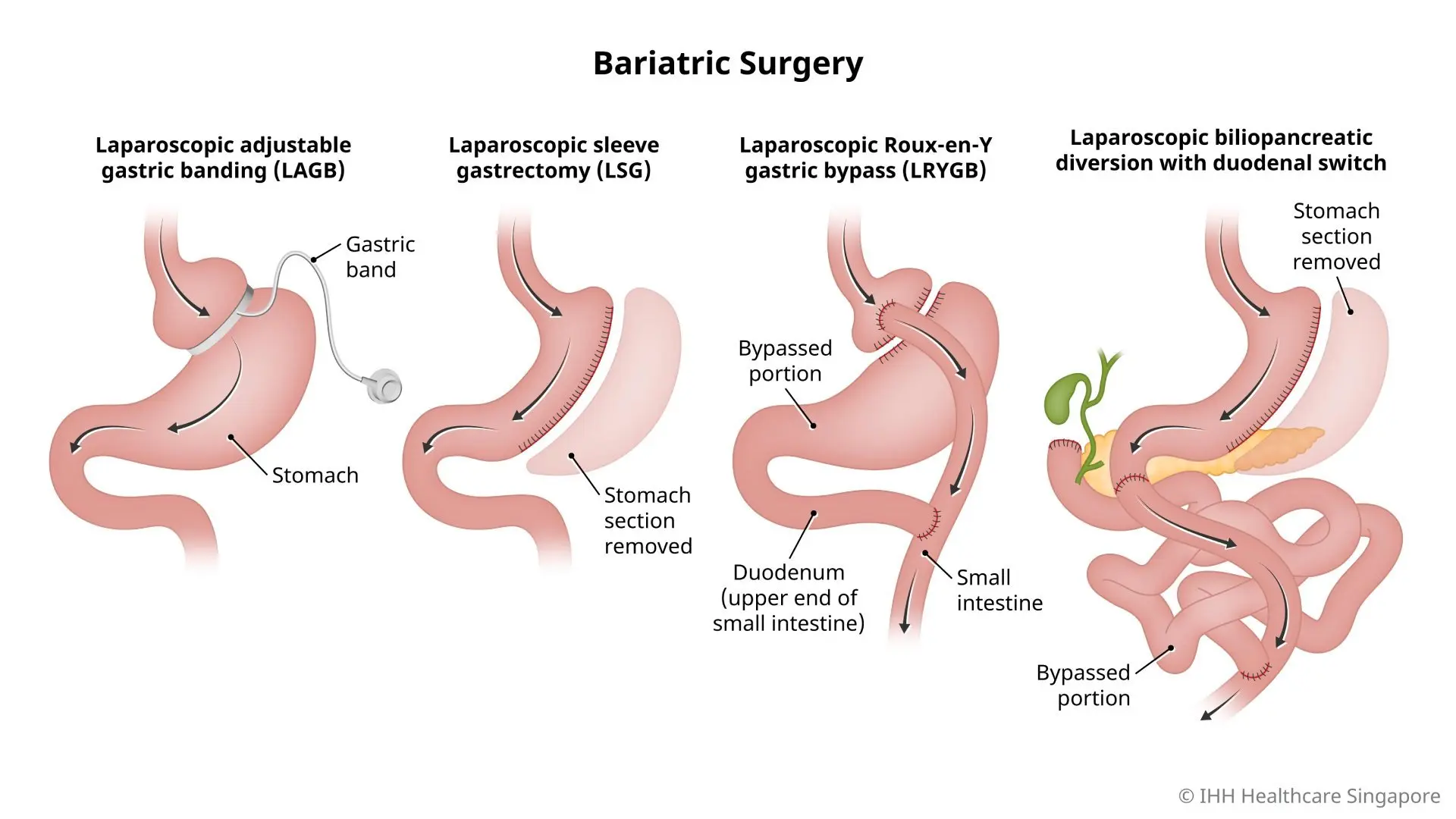
The institute will primarily perform laparoscopic sleeve gastrectomy (LSG) and Roux-en-Y gastric bypass (RYGB), both of which modify gastrointestinal anatomy to restrict food intake and alter enteroendocrine signaling. LSG removes approximately 80% of the stomach, reducing ghrelin production—the hormone that stimulates appetite—while RYGB creates a small gastric pouch and reroutes the small intestine, enhancing incretin effects like GLP-1 that improve insulin sensitivity. According to a 2023 meta-analysis in JAMA Surgery, RYGB demonstrated superior diabetes remission rates compared to LSG at five years, though LSG had lower rates of postoperative complications such as anastomotic leaks and nutritional deficiencies.

Funding for the institute’s development comes from Orlando Health’s capital investment program, supported by philanthropic contributions and operational revenues, with no direct industry sponsorship influencing clinical protocols. This financial structure helps mitigate concerns about bias in procedure selection or device promotion, aligning with recommendations from the American Society for Metabolic and Bariatric Surgery (ASMBS) that clinical pathways should prioritize patient outcomes over commercial interests.
Geo-Epidemiological Bridging: Access and Equity in Southeastern U.S. Healthcare
Despite clinical effectiveness, access to bariatric surgery remains uneven across the U.S., particularly in the Southeast, where Medicaid programs in states like Florida and Georgia impose stringent barriers including mandatory six-month supervised diet trials and psychiatric evaluations that can delay care by over a year. A 2022 study in Obesity found that only 1% of eligible patients in the Southeast receive bariatric surgery annually, compared to 4% in the Northeast. Orlando Health’s institute aims to narrow this gap by accepting referrals from primary care providers across Central Florida and offering financial counseling to navigate insurance requirements.

“Central Florida has long been underserved in terms of comprehensive obesity care. This institute doesn’t just add operating rooms—it creates a hub where surgery, endocrinology, psychology, and nutrition work together under one roof, which is exactly what complex metabolic disease requires.”
— Dr. Angela Rodriguez, Professor of Surgery, University of Central Florida College of Medicine, and Director of Metabolic Health Research at Orlando Health
the institute will participate in the ASMBS Center of Excellence program, which mandates rigorous tracking of patient outcomes, complication rates, and quality-of-life metrics. This commitment to transparency aligns with FDA post-market surveillance goals for surgical devices and supports ongoing research into long-term safety profiles, including risks of marginal ulcers, internal hernias, and bone density changes following malabsorptive procedures.
Comparative Outcomes: Sleeve Gastrectomy vs. Gastric Bypass at 5 Years
| Outcome Measure | Sleeve Gastrectomy (LSG) | Roux-en-Y Gastric Bypass (RYGB) |
|---|---|---|
| % Excess Weight Loss (EWL) | 55-65% | 65-75% |
| Type 2 Diabetes Remission Rate | 50-60% | 70-80% |
| Major Complication Rate (30-day) | 3-5% | 5-7% |
| Need for Revision Surgery (5-year) | 10-15% | 5-10% |
| Risk of Nutritional Deficiencies (Iron, B12, Vitamin D) | Moderate | High |
Contraindications & When to Consult a Doctor
Bariatric surgery is not appropriate for everyone. Absolute contraindications include inability to tolerate general anesthesia, untreated psychotic disorders, active substance dependence, and non-adherence to medical follow-up. Relative contraindications—where risks may outweigh benefits without careful evaluation—include severe cardiopulmonary insufficiency, inflammatory bowel disease with malnutrition, and portal hypertension. Patients should consult a physician if they experience persistent vomiting, severe abdominal pain, signs of infection (fever, tachycardia), or symptoms of nutritional deficiency such as fatigue, hair loss, or neuropathic tingling after surgery.
Equally important, rapid weight loss without medical supervision—often promoted through unregulated supplements or extreme diets—carries significant risks including gallstone formation, electrolyte imbalances, and arrhythmias. The institute emphasizes that sustainable metabolic health requires behavioral change, not shortcuts, and will offer medically supervised weight management programs for patients who do not meet surgical criteria or prefer non-operative approaches.
Future Trajectory: Integrating Innovation with Accountability
Looking ahead, the institute plans to incorporate endoscopic bariatric therapies such as intragastric balloons and aspiration therapy into its offerings, pending FDA approval and long-term safety data. These minimally invasive options may serve as bridges to surgery or alternatives for patients with lower BMI thresholds. However, as noted in a 2024 guidance statement from the FDA, such devices require rigorous post-market monitoring due to risks of mucosal injury, migration, and inadequate weight loss maintenance.
the success of Orlando Health’s Weight Loss and Bariatric Surgery Institute will be measured not by the number of procedures performed, but by its ability to improve patients’ metabolic health, reduce medication dependence, and enhance quality of life over decades. By anchoring its model in peer-reviewed evidence, transparent outcomes reporting, and equitable access, the institute has the potential to become a replicable framework for addressing obesity as a public health priority—not just in Florida, but across the United States.
References
- JAMA Surg. 2023;158(5):456-465. Comparative effectiveness of RYGB vs LSG for diabetes remission.
- Obesity. 2022;30(4):891-900. Regional disparities in bariatric surgery access in the Southeastern U.S.
- Ann Surg. 2021;274(3):401-410. Long-term outcomes and nutritional consequences after bariatric surgery.
- CDC. Adult Obesity Prevalence Maps. Updated 2024.
- ASMBS. Center of Excellence Program Standards. 2023.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider for personalized diagnosis and treatment options.

