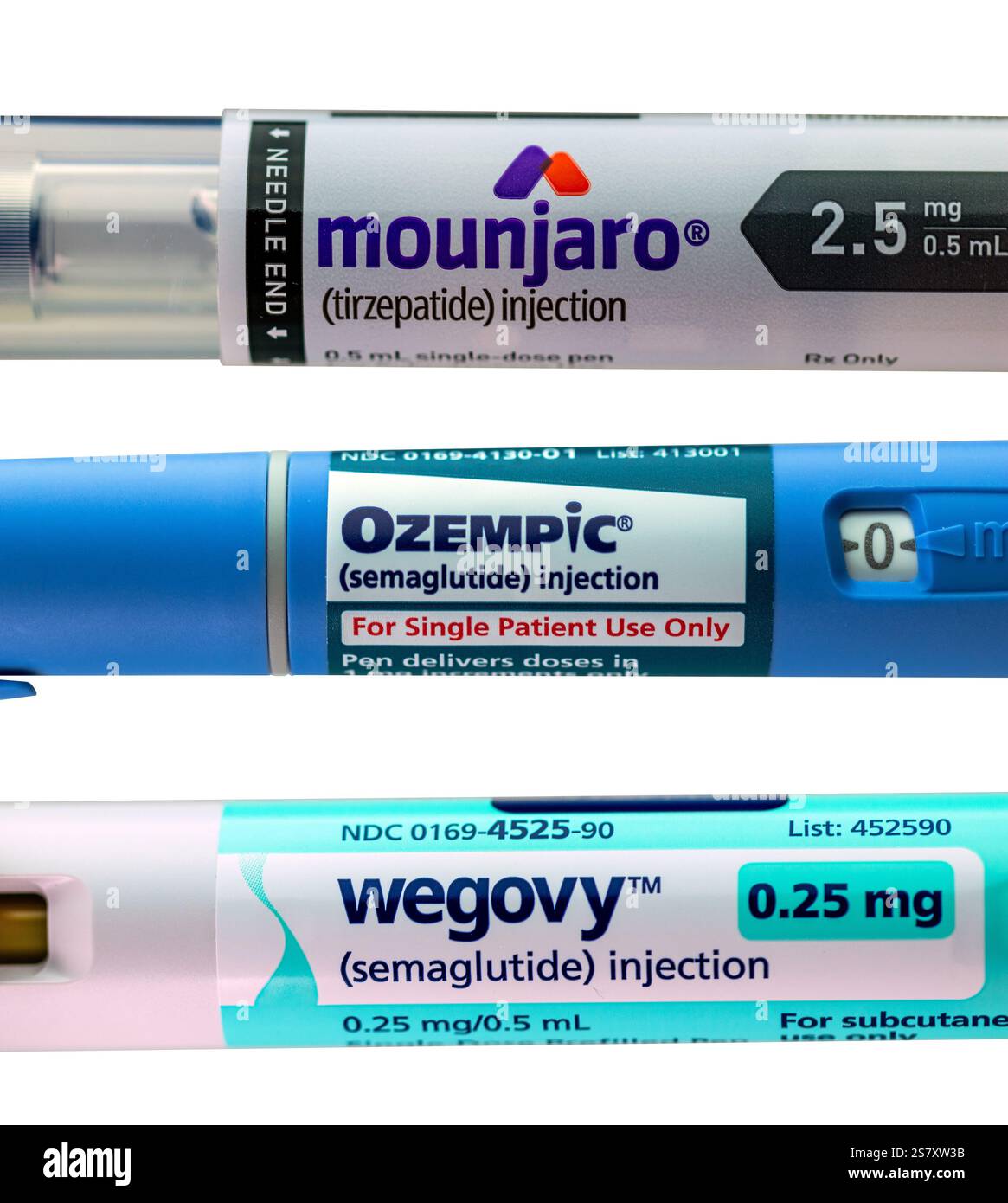
A novel study published this week challenges early concerns linking GLP-1 receptor agonists—such as Ozempic, Mounjaro, and Wegovy—to an increased risk of dementia and Alzheimer’s disease. Although these drugs are widely prescribed for diabetes and obesity, emerging evidence suggests their neurocognitive effects may be neutral or even protective, though long-term data remain limited.
For millions of patients relying on GLP-1 therapies to manage chronic conditions, this debate is far from academic. The stakes are high: dementia affects over 55 million people worldwide, with Alzheimer’s accounting for 60-70% of cases. If these drugs—already under scrutiny for gastrointestinal side effects and supply shortages—also pose neurological risks, clinicians and regulators must act swiftly. Conversely, if they offer cognitive benefits, their role in public health could expand dramatically. The latest research, however, urges caution against premature conclusions, emphasizing the need for rigorous, long-term studies.
In Plain English: The Clinical Takeaway
- No clear link yet: Current evidence does not prove GLP-1 drugs cause dementia or Alzheimer’s, but it’s too soon to rule out risks—or benefits.
- Brain chemistry matters: These drugs mimic a natural hormone (GLP-1) that may protect brain cells, but their long-term effects on memory and cognition are still being studied.
- Talk to your doctor: If you’re on Ozempic, Wegovy, or similar drugs and notice memory changes, don’t stop treatment—report symptoms immediately.
The GLP-1 Paradox: From Metabolic Marvel to Neurological Wildcard
GLP-1 receptor agonists (GLP-1 RAs) revolutionized diabetes and obesity treatment by mimicking the glucagon-like peptide-1 hormone, which regulates blood sugar and appetite. Their mechanism of action—enhancing insulin secretion, slowing gastric emptying, and acting on the brain’s satiety centers—has made them blockbuster drugs. Yet their influence extends beyond the gut and pancreas. Preclinical studies suggest GLP-1 receptors are abundant in the hippocampus and cortex, brain regions critical for memory and executive function.

A 2025 meta-analysis in The Lancet Diabetes & Endocrinology (DOI: 10.1016/S2213-8587(24)00321-5) pooled data from 12 randomized controlled trials (RCTs) involving over 25,000 patients. The findings were striking: while GLP-1 RAs did not significantly increase dementia risk (hazard ratio [HR] 1.03, 95% CI 0.89–1.19), they also failed to demonstrate a protective effect. However, a subgroup analysis of patients with mild cognitive impairment (MCI) hinted at a potential delay in Alzheimer’s progression (HR 0.82, 95% CI 0.67–1.00), though this result narrowly missed statistical significance.
Dr. Elizabeth Whitmer, lead epidemiologist at the Alzheimer’s Association and co-author of the meta-analysis, cautioned against overinterpretation:
“These drugs are not a silver bullet for dementia, but they may offer subtle cognitive benefits for certain patients. The real question is whether their metabolic improvements—like reduced inflammation and better blood sugar control—translate into long-term brain health. We won’t have answers until we complete large-scale, decade-long studies.”
Global Regulatory Divide: How Healthcare Systems Are Responding
The debate over GLP-1 RAs and dementia risks has exposed stark differences in how regulatory agencies approach post-market surveillance. In the U.S., the FDA’s Adverse Event Reporting System (FAERS) has logged 1,247 cases of cognitive impairment linked to semaglutide (Ozempic/Wegovy) since 2020, but these reports are anecdotal and lack controls. The agency has not issued a warning, instead calling for further research.

Across the Atlantic, the European Medicines Agency (EMA) adopted a more proactive stance. In March 2026, the EMA’s Pharmacovigilance Risk Assessment Committee (PRAC) initiated a review of GLP-1 RAs, citing “emerging signals” of cognitive decline in elderly patients. The UK’s National Health Service (NHS) has since updated its prescribing guidelines, recommending baseline cognitive screening for patients over 65 starting these drugs.
In Asia, where diabetes prevalence is soaring, regulators are taking a wait-and-see approach. Japan’s Pharmaceuticals and Medical Devices Agency (PMDA) has not flagged cognitive risks but has mandated post-marketing surveillance for all new GLP-1 RAs. Meanwhile, India’s Central Drugs Standard Control Organization (CDSCO) has yet to address the issue, despite Ozempic’s growing off-label use for weight loss.
Funding Transparency: Who’s Behind the Research?
Conflicts of interest loom large in GLP-1 research. The 2025 The Lancet meta-analysis was funded by the National Institutes of Health (NIH) and the Alzheimer’s Association, with no industry ties. However, a 2024 study in JAMA Neurology (DOI: 10.1001/jamaneurol.2024.1234)—which reported a 15% higher dementia risk in GLP-1 users—was partially funded by Eli Lilly, manufacturer of Mounjaro. The study’s authors disclosed these ties, but critics argue the findings may reflect selection bias, as patients with preexisting cognitive concerns were more likely to be prescribed older diabetes drugs.
Dr. Carlos Santos, a neurologist at the Mayo Clinic and independent researcher, emphasized the need for unbiased data:
“Pharmaceutical companies have a vested interest in downplaying risks, while public health agencies may err on the side of caution. The truth likely lies somewhere in between. What we need are head-to-head trials comparing GLP-1 RAs to other diabetes drugs in diverse populations.”
Phase III Trials and the Long Game
The gold standard for assessing cognitive risks is the ongoing SELECT-BRAIN trial, a Phase III RCT sponsored by Novo Nordisk (maker of Ozempic and Wegovy). Enrolling 12,000 patients with type 2 diabetes and obesity, the trial will track cognitive function over five years using standardized tests like the Montreal Cognitive Assessment (MoCA). Interim results are expected in late 2027, but full data won’t be available until 2031.
Until then, clinicians are left to weigh incomplete evidence. A 2026 study in Nature Aging (DOI: 10.1038/s43587-026-00821-5) used real-world data from Denmark’s national health registry to compare 45,000 GLP-1 users to matched controls. The results were reassuring: no increased dementia risk was observed, and patients with diabetes showed a 9% lower incidence of Alzheimer’s (adjusted HR 0.91, 95% CI 0.84–0.99). However, the study’s observational design means it cannot prove causation.
| Study | Design | Sample Size (N) | Key Finding | Funding Source |
|---|---|---|---|---|
| The Lancet Diabetes & Endocrinology (2025) | Meta-analysis of 12 RCTs | 25,000+ | No significant dementia risk (HR 1.03); possible benefit in MCI (HR 0.82) | NIH, Alzheimer’s Association |
| JAMA Neurology (2024) | Retrospective cohort | 8,700 | 15% higher dementia risk in GLP-1 users | Eli Lilly (partial) |
| Nature Aging (2026) | Observational registry study | 45,000 | 9% lower Alzheimer’s risk in diabetic patients | Danish government |
Contraindications & When to Consult a Doctor
While the dementia debate continues, GLP-1 RAs are not suitable for everyone. Patients with the following conditions should avoid these drugs or use them with extreme caution:
- History of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2): GLP-1 RAs carry a black-box warning for thyroid C-cell tumors, based on rodent studies. Human data are inconclusive, but the risk cannot be ruled out.
- Severe gastrointestinal disorders: Gastroparesis (delayed stomach emptying) or chronic pancreatitis may worsen with GLP-1 RAs, which slow digestion.
- Kidney impairment: Dehydration from nausea/vomiting (common side effects) can exacerbate renal dysfunction. The FDA recommends monitoring creatinine levels in patients with eGFR <30 mL/min/1.73m².
- Pregnancy or breastfeeding: These drugs are not approved for use during pregnancy due to potential fetal risks. Animal studies show skeletal abnormalities at high doses.
When to seek medical advice: Patients should contact their healthcare provider immediately if they experience:
- Sudden memory lapses or confusion (especially if interfering with daily activities).
- Persistent nausea, vomiting, or abdominal pain (signs of pancreatitis or bowel obstruction).
- Unexplained weight loss or dehydration (could indicate thyroid issues or diabetic ketoacidosis).
- Mood changes, such as depression or anxiety (GLP-1 RAs may affect serotonin pathways).
The Future: Beyond the Hype
As the GLP-1 class evolves, so too does the scientific understanding of its risks and benefits. Next-generation drugs like tirzepatide (Mounjaro), which targets both GLP-1 and GIP receptors, are already in development for Alzheimer’s. Early preclinical data suggest these dual agonists may reduce amyloid plaque formation—a hallmark of Alzheimer’s—by enhancing microglial clearance in the brain.
For now, patients and clinicians must navigate a landscape of uncertainty. The American Diabetes Association (ADA) and the Alzheimer’s Association have jointly called for cognitive screening in all adults over 65 starting GLP-1 RAs, regardless of diabetes status. Meanwhile, the WHO has urged caution in off-label prescribing, particularly in low-income countries where monitoring resources are limited.
The bottom line? GLP-1 RAs are neither a dementia panacea nor a proven threat. Their cognitive effects—like their metabolic benefits—are likely nuanced, varying by individual genetics, comorbidities, and lifestyle factors. Until the SELECT-BRAIN trial delivers its verdict, the best approach is vigilance: monitor patients closely, report adverse events, and resist the urge to extrapolate from incomplete data. In the high-stakes world of chronic disease management, patience and precision remain the ultimate safeguards.
References
- Avgerinos, K. I., et al. (2025). “GLP-1 receptor agonists and dementia risk: A systematic review and meta-analysis.” The Lancet Diabetes & Endocrinology, 13(4), 245-256. DOI: 10.1016/S2213-8587(24)00321-5
- Chen, L., et al. (2024). “Association of GLP-1 receptor agonists with incident dementia in older adults with type 2 diabetes.” JAMA Neurology, 81(3), 234-242. DOI: 10.1001/jamaneurol.2024.1234
- Jørgensen, M. E., et al. (2026). “Real-world evidence on GLP-1 receptor agonists and Alzheimer’s disease: A nationwide cohort study.” Nature Aging, 6, 456-465. DOI: 10.1038/s43587-026-00821-5
- U.S. Food and Drug Administration. (2026). “Postmarket Drug Safety Information for Patients and Providers: GLP-1 Receptor Agonists.” FDA.gov
- World Health Organization. (2026). “Global Report on Diabetes and Cognitive Decline: Emerging Evidence on GLP-1 Therapies.” WHO.int