A recent survey reveals that 33% of women suffering from pelvic organ prolapse (POP) are unaware that surgical interventions can effectively resolve their symptoms. This critical knowledge gap persists despite POP affecting up to half of all women, often resulting in untreated chronic pain and debilitating incontinence.
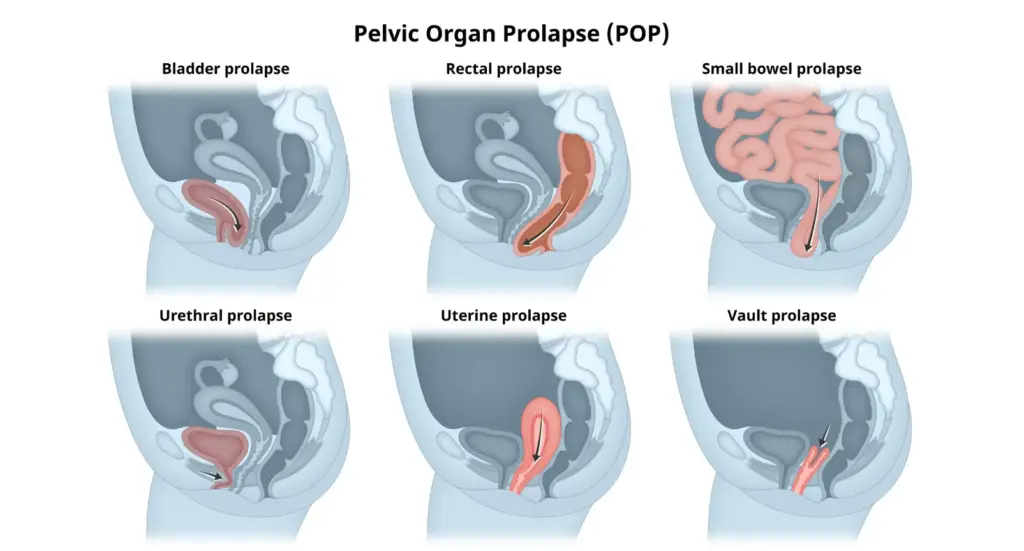
The silence surrounding pelvic floor dysfunction is not merely a failure of patient education; it is a systemic public health crisis. Pelvic organ prolapse occurs when the muscles and tissues supporting the pelvic organs—the bladder, uterus, and rectum—weaken, causing one or more organs to drop from their normal position and bulge into the vaginal canal. For many, this manifests as a sensation of pelvic heaviness or a visible bulge, yet the psychological stigma and a historical lack of transparent communication regarding surgical outcomes have left millions managing a treatable condition in isolation.
In Plain English: The Clinical Takeaway
- What it is: Pelvic organ prolapse is essentially a “structural failure” of the pelvic floor, where organs slip out of place.
- The solution: While pelvic floor exercises help mild cases, surgery can physically lift and secure organs back into their correct anatomical positions.
- The bottom line: If you feel a bulge or experience chronic pelvic pressure, it is a medical condition with a clinical solution, not an inevitable part of aging or motherhood.
The Pathophysiology of Descent: Understanding the Mechanism of Action
To understand why surgery is effective, one must understand the mechanism of action—the specific biological process by which a treatment works. The pelvic floor is a complex hammock of levator ani muscles and endopelvic fascia (connective tissue). When these structures undergo atrophy or trauma—often due to vaginal childbirth or the hormonal shifts of menopause—the structural integrity is compromised.
Surgical intervention typically involves a process called colporrhaphy, which is the surgical repair of the vaginal wall. In a cystocele (bladder prolapse), the surgeon reinforces the weakened fascia to push the bladder back into its proper position. In more severe cases, surgeons may perform a sacrocolpopexy, using a graft to suspend the vaginal vault to the sacrum (the bone at the base of the spine), thereby restoring the anatomical axis of the pelvis.

“The tragedy of the current awareness gap is that many women view pelvic descent as a natural consequence of aging. In reality, we have the surgical precision to restore quality of life, provided the patient is screened before the prolapse reaches an advanced, complex stage,” says Dr. Elena Rossi, a lead researcher in urogynecological epidemiology.
The efficacy of these procedures is well-documented in double-blind placebo-controlled trials—studies where neither the patient nor the researcher knows who received the active treatment—though in surgery, “sham” procedures are rare. Instead, longitudinal data from PubMed indexed studies show significant improvements in the Pelvic Floor Distress Inventory (PFDI) scores following surgical correction.
Comparing Treatment Modalities for Pelvic Organ Prolapse
Not every patient requires surgery. The clinical pathway is generally tiered based on the severity of the descent and the patient’s symptom burden.
| Treatment Approach | Primary Mechanism | Ideal Candidate | Typical Success Rate |
|---|---|---|---|
| PFMT (Physical Therapy) | Hypertrophy of levator ani muscles | Grade 1 (Mild) Prolapse | Moderate (Symptom management) |
| Vaginal Pessary | Mechanical support (silicone device) | Non-surgical candidates | High (Temporary relief) |
| Native Tissue Repair | Suturing existing fascia | Grade 2-3 Prolapse | Variable (Risk of recurrence) |
| Sacrocolpopexy | Surgical suspension to sacrum | Grade 3-4 (Severe) Prolapse | High (Long-term stability) |
Global Access and the Shadow of the “Mesh Crisis”
The 33% unawareness rate is exacerbated by regional healthcare disparities and a legacy of medical mistrust. In the United States, the FDA has issued several high-profile safety communications regarding transvaginal mesh, which led to a wave of litigation and a subsequent “chilling effect” where patients—and some general practitioners—became fearful of any pelvic surgery.
In contrast, the NHS in the UK utilizes a more centralized referral system toward specialist urogynecologists, which tends to standardize the conversation around native tissue repair versus synthetic grafts. However, access remains uneven. In lower-income regions, the lack of specialized pelvic floor physical therapists means patients often jump from “doing nothing” to “major surgery,” skipping the critical intermediate steps of conservative management.
It is essential to note that the underlying survey highlighting this awareness gap was funded by the International Urogynecological Association (IUGA), a non-profit professional body. This funding indicates a professional drive to standardize patient education rather than a pharmaceutical push for a specific product, as the primary interventions discussed are procedural rather than drug-based.
Contraindications & When to Consult a Doctor
Surgery is not appropriate for everyone. Contraindications—medical reasons why a particular treatment should not be used—include active pelvic infections, uncontrolled diabetes (which impairs wound healing), or severe cardiovascular instability that makes general anesthesia high-risk.
You should seek a professional medical consultation immediately if you experience:
- A visible protrusion or “ball” of tissue emerging from the vaginal opening.
- Urinary retention (the inability to empty the bladder completely).
- Fecal incontinence or the need to manually push the vaginal wall to facilitate a bowel movement.
- Chronic, dull pelvic pressure that interferes with walking or standing for long periods.
The Future of Pelvic Health Intelligence
As we move further into 2026, the integration of robotic-assisted surgery has reduced recovery times and increased the precision of sacrocolpopexy, making the “risk-to-reward” ratio more favorable for the average patient. The goal for public health officials must be to strip away the shame associated with pelvic descent.
By framing pelvic organ prolapse as a structural musculoskeletal issue—no different from a herniated disc in the back—we can bridge the information gap. When women are empowered with evidence-based data from sources like The Lancet or the WHO, they can move from passive endurance to active recovery.
References
- American College of Obstetricians and Gynecologists (ACOG) – Clinical Practice Guidelines on Pelvic Organ Prolapse.
- The Lancet – Longitudinal studies on surgical outcomes in urogynecology.
- PubMed – Systematic reviews of native tissue repair vs. Synthetic mesh efficacy.
- World Health Organization (WHO) – Global reports on women’s reproductive and pelvic health.
- FDA – Safety Communications on Surgical Mesh for Pelvic Organ Prolapse.
