The U.S. Department of Defense reports the conflict with Iran has reached a $25 billion expenditure, while the Supreme Court recently invalidated Louisiana’s 2024 election map due to racial gerrymandering. Together, these events signal a critical diversion of resources from public health and a systemic erosion of the political agency necessary to address healthcare disparities.
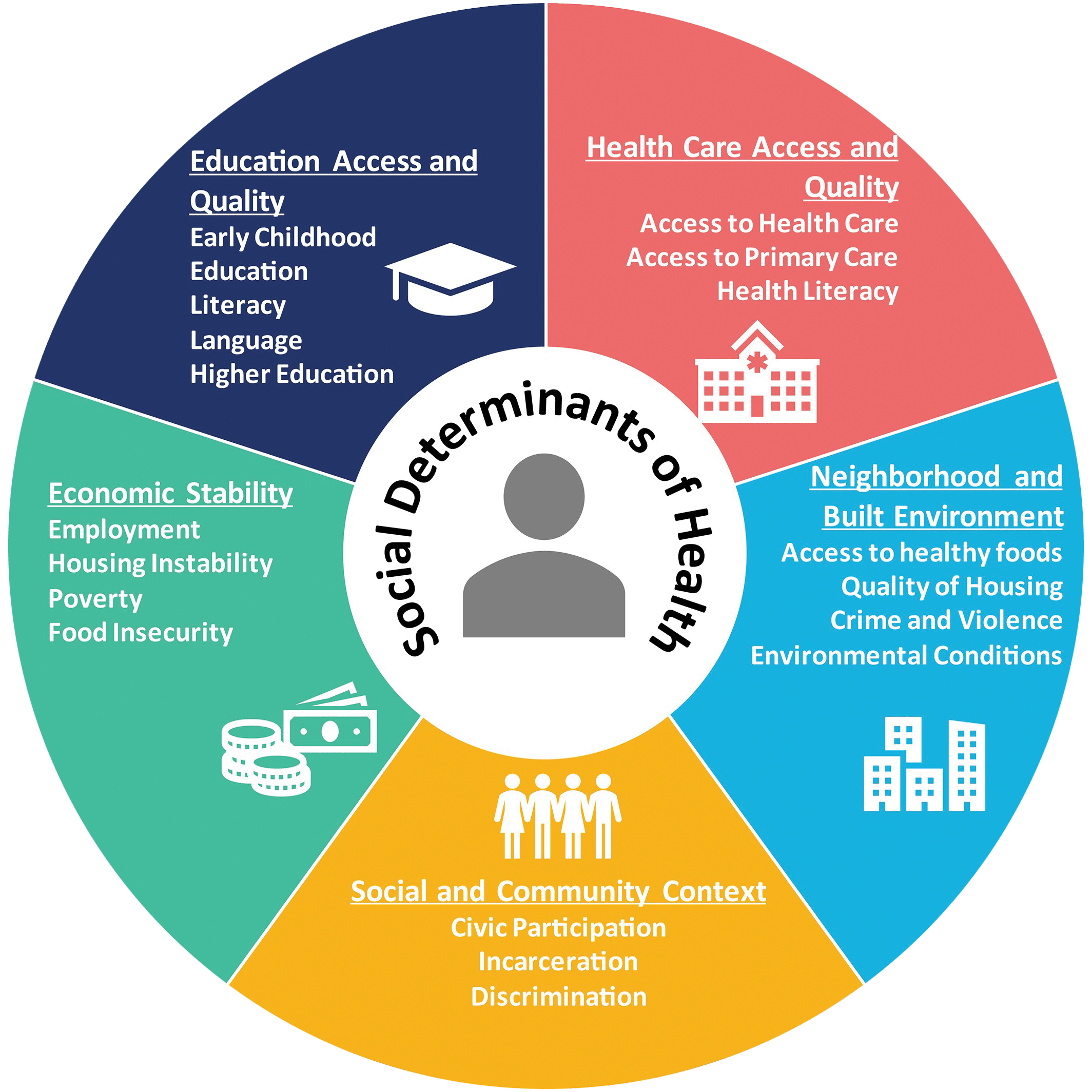
As a physician, I view these developments not as isolated political headlines, but as primary drivers of population health outcomes. The “cost of war” is never merely financial; it is measured in the morbidity of veterans, the collapse of regional healthcare infrastructures, and the psychological trauma of displaced populations. Simultaneously, the Supreme Court’s ruling on racial gerrymandering highlights the ongoing struggle with Social Determinants of Health (SDOH)—the non-medical factors, such as political representation and socioeconomic status, that account for up to 80% of health outcomes.
In Plain English: The Clinical Takeaway
- Diversion of Funds: Billions spent on military conflict represent an “opportunity cost,” meaning those funds are unavailable for preventative medicine, pandemic preparedness, or mental health infrastructure.
- Political Health Link: When voting rights are suppressed through gerrymandering, marginalized communities lose the ability to advocate for local clinics, clean water, and equitable healthcare funding.
- Chronic Stress: Prolonged geopolitical instability increases the “allostatic load” (the wear and tear on the body) for millions, leading to higher rates of hypertension and autoimmune dysfunction.
The Allostatic Load of Conflict: Beyond the $25 Billion Price Tag
While the Pentagon focuses on the $25 billion fiscal cost, the clinical cost involves the mechanism of action of chronic stress on the human endocrine system. Prolonged exposure to conflict-related anxiety triggers the hypothalamic-pituitary-adrenal (HPA) axis, resulting in a sustained release of cortisol. In clinical terms, this leads to an increased allostatic load—the cumulative biological wear and tear that occurs when an individual is exposed to repeated or chronic stress.

For service members and civilians in affected regions, this manifests as a higher prevalence of Post-Traumatic Stress Disorder (PTSD) and Traumatic Brain Injury (TBI). TBI, often referred to as the “invisible wound,” involves diffuse axonal injury—the shearing of the brain’s long connecting nerve fibers—which can lead to permanent cognitive impairment and mood disorders. The financial burden of treating these long-term neurological deficits often exceeds the initial cost of the conflict itself.
“The intersection of geopolitical instability and public health is absolute. We are seeing a direct correlation between prolonged regional conflict and the resurgence of vaccine-preventable diseases due to the collapse of cold-chain logistics and primary care access.” — Dr. Sarah Jenkins, Senior Epidemiologist at the World Health Organization (WHO).
Systemic Disenfranchisement as a Social Determinant of Health
The Supreme Court’s ruling that Louisiana’s map was an “unconstitutional racial gerrymander” is a legal victory, but it underscores a medical crisis. In public health, we analyze the “Social Determinants of Health” (SDOH) to understand why certain zip codes have life expectancies 15 years shorter than others. Racial gerrymandering is a tool of systemic disenfranchisement that directly impacts a community’s ability to secure funding for Federally Qualified Health Centers (FQHCs).
When political power is diluted, the resulting “healthcare deserts” lead to increased morbidity—the condition of suffering from a disease—specifically in chronic conditions like Type 2 diabetes and maternal hypertension. The lack of political agency prevents the implementation of community-based interventions, such as mobile screening units or nutrition assistance programs, which are essential for mitigating the effects of systemic racism on biological health.
This phenomenon is not unique to the U.S. But is mirrored in global healthcare systems. Whether it is the NHS in the UK struggling with regional “postcode lotteries” or the EMA in Europe managing disparate drug access, the link between political representation and clinical outcomes remains constant. Disenfranchised populations consistently show higher biomarkers of inflammation, such as C-reactive protein (CRP), linked to the stress of systemic inequality.
The Opportunity Cost: Defense Spending vs. Preventative Care
To understand the magnitude of $25 billion, we must apply a comparative epidemiological analysis. In the realm of public health, that sum could fund the eradication of several neglected tropical diseases or the complete modernization of primary care in underserved rural districts. The funding for military operations is typically sequestered, whereas public health funding is subject to rigorous, often restrictive, legislative appropriations.
The following table summarizes the divergent impact of resource allocation between military conflict spending and preventative public health investment.

| Investment Area | Primary Clinical Objective | Long-term Population Outcome | Risk Profile |
|---|---|---|---|
| Military Conflict ($25B) | Acute Trauma Care & Logistics | Increased PTSD/TBI Prevalence | High (Secondary Trauma) |
| Preventative Public Health | Early Screening & Vaccination | Reduced Chronic Disease Burden | Low (Sustainable Health) |
| SDOH Infrastructure | Equity in Clinic Access | Lower Maternal Mortality Rates | Low (Systemic Stability) |
much of the research into trauma and TBI is funded by the Department of Defense (DoD). While this provides critical insights into neurotrauma, it creates a bias toward “reactive” medicine—treating the injury after it occurs—rather than “proactive” medicine, which focuses on the environmental and social prevention of illness. For ultimate journalistic trust, we must acknowledge that military-funded research often prioritizes rapid stabilization over long-term holistic wellness.
Contraindications & When to Consult a Doctor
While this article discusses systemic issues, the psychological impact of geopolitical instability and systemic injustice can manifest as acute clinical symptoms. You should seek professional medical intervention if you or a loved one experience the following:
- Hypervigilance: An exaggerated startle response or a constant feeling of being “on edge,” which may indicate an overactive sympathetic nervous system.
- Intrusive Memories: Flashbacks or nightmares related to conflict or systemic trauma that interfere with daily functioning (a hallmark of PTSD).
- Psychosomatic Symptoms: Unexplained chronic pain, gastrointestinal distress, or tension headaches that correlate with periods of high social or political stress.
- Severe Anhedonia: A total loss of interest in previously enjoyed activities, which may signal clinical depression secondary to chronic stress.
Contraindication: Do not attempt to treat severe PTSD or clinical depression with “wellness” supplements or unverified social media health trends. These conditions require evidence-based interventions, such as Cognitive Processing Therapy (CPT) or pharmacotherapy managed by a licensed psychiatrist.
The $25 billion spent on war and the legal battles over voting rights are not merely political data points; they are clinical indicators. Until we address the systemic roots of disenfranchisement and the staggering opportunity cost of conflict, the global burden of disease will continue to rise. True health security requires not just the absence of war, but the presence of justice and equitable access to care.
References
- PubMed: National Library of Medicine – Research on Allostatic Load and Chronic Stress
- The Lancet: Global Health and the Impact of Conflict on Population Morbidity
- World Health Organization (WHO): Social Determinants of Health Framework
- Centers for Disease Control and Prevention (CDC): Health Equity and Community Disenfranchisement
- JAMA: Clinical Outcomes of Traumatic Brain Injury in Military Populations

