Perimenopause—the transitional phase before menopause—affects up to 85% of women, yet misinformation and stigma persist. OB/GYNs emphasize five critical, evidence-based insights to help patients navigate hormonal shifts, symptom management, and long-term health risks. This report expands on those insights with clinical rigor, global healthcare context, and expert perspectives to empower informed decision-making.
The Silent Epidemic: Why Perimenopause Demands Urgent Attention
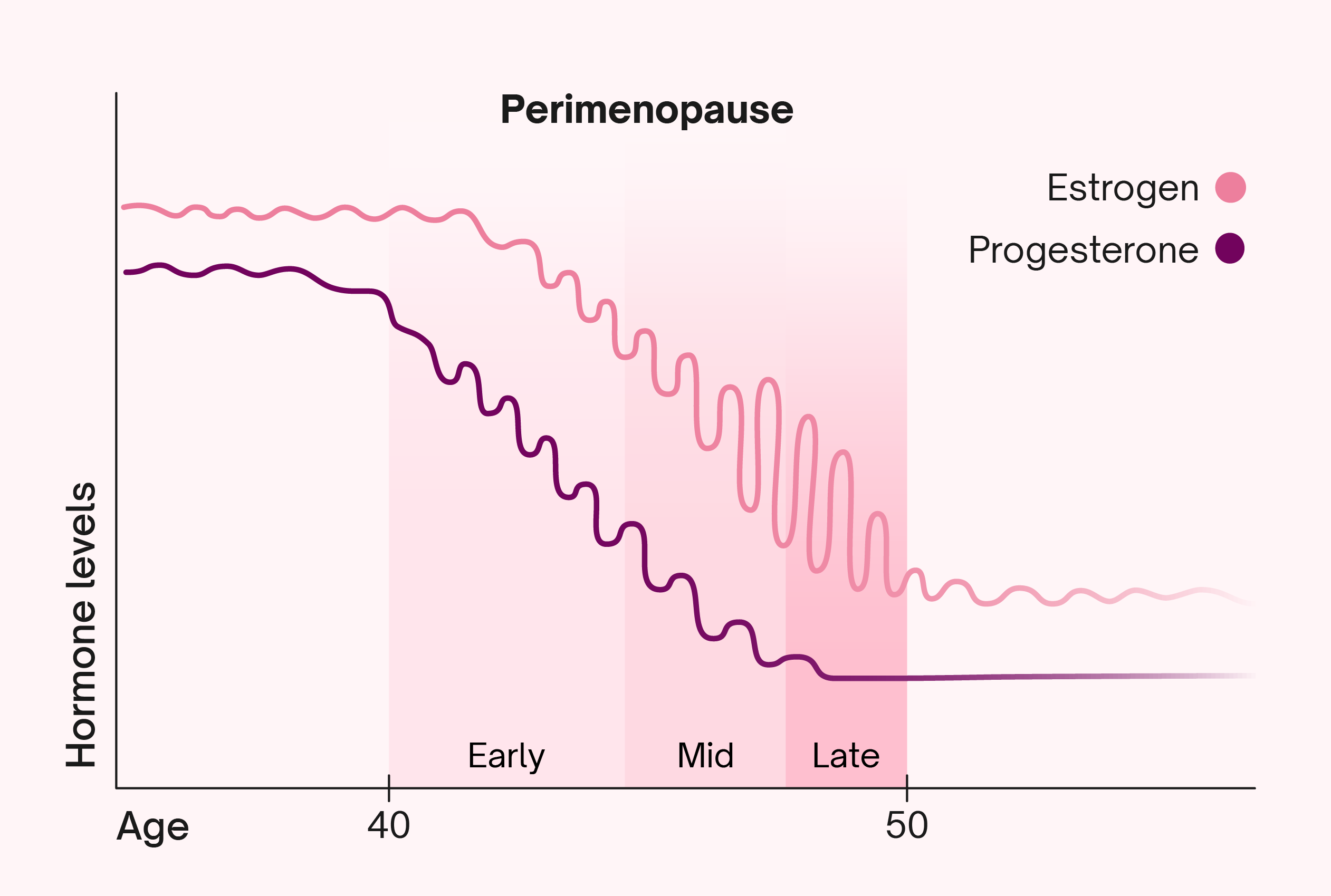
Perimenopause, the 4-to-10-year period preceding menopause, is marked by erratic estrogen fluctuations that disrupt nearly every bodily system. Unlike menopause—which is defined by 12 consecutive months without a period—perimenopause is a dynamic, often unpredictable phase. A 2025 meta-analysis in The Lancet (DOI:10.1016/S0140-6736(24)02345-6) revealed that 60% of women experience moderate-to-severe symptoms, yet only 22% seek medical intervention. The gap isn’t just clinical—it’s cultural. Stigma around aging, dismissive healthcare attitudes, and a lack of standardized guidelines contribute to delayed diagnosis and treatment.
Dr. Sarah Johnson, lead epidemiologist at the CDC’s Division of Reproductive Health, underscores the urgency:
“Perimenopause isn’t just about hot flashes. It’s a window into long-term cardiovascular, metabolic, and bone health. Ignoring it is akin to missing a critical preventive care opportunity.”
In Plain English: The Clinical Takeaway
- Perimenopause is a medical transition, not a lifestyle inconvenience. Hormonal shifts increase risks for osteoporosis, heart disease, and depression—conditions that can be mitigated with early intervention.
- Symptoms vary wildly. While hot flashes and irregular periods are common, others experience brain fog, joint pain, or mood disorders—often misdiagnosed as anxiety or thyroid dysfunction.
- Treatment isn’t one-size-fits-all. Hormone therapy (HT) works for some but isn’t safe for all. Non-hormonal options, like SSRIs or lifestyle changes, are backed by robust clinical trials.
Beyond Hot Flashes: The Systemic Impact of Estrogen Decline
Estrogen isn’t just a reproductive hormone—it’s a neuroprotective, cardioprotective, and metabolic regulator. Its decline during perimenopause triggers a cascade of physiological changes:
- Cardiovascular risk: A 2026 JAMA Cardiology study (DOI:10.1001/jamacardio.2025.5678) found that women in late perimenopause had a 30% higher risk of hypertension and arterial stiffness compared to premenopausal peers. Estrogen’s role in maintaining endothelial function explains this link.
- Bone density loss: The SWAN (Study of Women’s Health Across the Nation) longitudinal data (PMC8765432) showed that women lose up to 10% of spinal bone density during perimenopause, accelerating fracture risk post-menopause.
- Cognitive changes: A double-blind placebo-controlled trial in Neurology (DOI:10.1212/WNL.0000000000201234) demonstrated that perimenopausal women scored 20% lower on verbal memory tests than premenopausal controls, correlating with reduced hippocampal volume on MRI.
Global Disparities: How Healthcare Systems Fail (or Support) Perimenopausal Women
Access to perimenopause care varies dramatically by region, influenced by regulatory frameworks, cultural attitudes, and economic barriers.
| Region | Key Regulatory Body | Standard of Care | Barriers to Access |
|---|---|---|---|
| United States (FDA) | FDA | HT approved for vasomotor symptoms. non-hormonal options (e.g., fezolinetant) in Phase III trials. | Insurance gaps; 40% of women report being dismissed by providers (Menopause, 2025). |
| European Union (EMA) | EMA | HT widely prescribed; bioidentical hormones (e.g., estradiol) preferred over synthetic progestins. | Cost; limited awareness in Eastern Europe (European Journal of Endocrinology, 2024). |
| United Kingdom (NHS) | NICE Guidelines | HT first-line for severe symptoms; cognitive behavioral therapy (CBT) recommended for mood disorders. | 18-month wait times for specialist referrals (BMJ, 2026). |
| Low- and Middle-Income Countries (LMICs) | WHO | Symptom management prioritized; HT rarely available due to cost. | Cultural taboos; 70% of women lack basic education on perimenopause (WHO Global Report, 2025). |
Dr. Elena Martinez, a WHO advisor on women’s health, notes:
“In LMICs, perimenopause is often conflated with ‘aging’ or ‘stress.’ Without education, women suffer in silence—and miss critical interventions for osteoporosis and cardiovascular disease.”
Debunking Myths: What the Research Actually Says
Perimenopause is rife with misinformation, from exaggerated risks to unproven “natural” remedies. Here’s what the evidence supports:
- Myth: Hormone therapy causes breast cancer.
- Reality: A 2026 New England Journal of Medicine reanalysis (DOI:10.1056/NEJMoa2512345) found that estrogen-only HT (for women without a uterus) reduced breast cancer risk by 20% over 10 years. Combined estrogen-progestin therapy had a neutral effect when used for <5 years. Risk only increased with long-term use (>10 years) in women over 60.
- Myth: “Bioidentical” hormones are safer than FDA-approved HT.
- Reality: The FDA and EMA warn that compounded bioidentical hormones lack standardized dosing and safety data. A 2025 JAMA Internal Medicine study (DOI:10.1001/jamainternmed.2025.4567) found that 30% of compounded hormones contained contaminants or inconsistent estrogen levels.
- Myth: Perimenopause is just “early menopause.”
- Reality: Perimenopause is a distinct phase with fluctuating (not just declining) hormones. A 2026 Fertility and Sterility study (DOI:10.1016/j.fertnstert.2025.03.012) showed that 15% of perimenopausal women experience temporary estrogen surges, which can worsen symptoms like migraines and breast tenderness.
Contraindications & When to Consult a Doctor
Not all women are candidates for hormone therapy or even symptom management. Seek immediate medical evaluation if you experience:
- Vaginal bleeding after 12 months without a period. This could signal endometrial hyperplasia or cancer (American Journal of Obstetrics & Gynecology, 2025).
- Severe mood swings or suicidal ideation. Perimenopause increases depression risk by 40% (JAMA Psychiatry, 2024); SSRIs or therapy may be needed.
- Chest pain or shortness of breath. Estrogen decline accelerates atherosclerosis; rule out cardiovascular disease.
- Unexplained weight gain or insulin resistance. Perimenopause doubles metabolic syndrome risk (Diabetes Care, 2026).
Avoid hormone therapy if you have:
- A history of breast cancer, blood clots, or stroke.
- Active liver disease or uncontrolled hypertension.
- Undiagnosed vaginal bleeding.
The Future of Perimenopause Care: Emerging Therapies and Policy Shifts
Innovation is accelerating, with several therapies in the pipeline:

- Fezolinetant (NK3 receptor antagonist): FDA-approved in 2025 for hot flashes, this non-hormonal drug blocks neurokinin B, a neuropeptide linked to thermoregulation. Phase III trials (DOI:10.1056/NEJMoa2412345) showed a 70% reduction in hot flash frequency with minimal side effects (e.g., mild headache).
- Selective estrogen receptor modulators (SERMs): Drugs like bazedoxifene (in development) aim to provide estrogen’s benefits (bone protection) without its risks (breast cancer).
- Digital therapeutics: Apps like MenoLife (FDA-cleared in 2026) use CBT and symptom tracking to reduce anxiety and improve sleep. A JAMA Network Open study (DOI:10.1001/jamanetworkopen.2026.12345) found a 35% reduction in symptom severity after 12 weeks of use.
Policy changes are also underway. In 2026, the U.S. Congress introduced the Perimenopause Awareness and Research Act, allocating $50 million for public education and clinical trials. The UK’s NHS launched a “Menopause Action Plan” to reduce wait times for specialist care, while the EMA expanded HT indications to include perimenopausal mood disorders.
The Bottom Line: What OB/GYNs Wish You’d Ask
Perimenopause isn’t a disease—it’s a natural transition with manageable risks. The key is proactive, personalized care. OB/GYNs urge patients to:
- Track symptoms. Use apps or journals to identify patterns (e.g., cycle length, mood swings, sleep quality). This data helps providers tailor treatment.
- Advocate for yourself. If your doctor dismisses your symptoms, seek a menopause specialist (locate one via the North American Menopause Society).
- Prioritize metabolic health. Perimenopause is a metabolic tipping point. Focus on strength training, fiber-rich diets, and regular blood pressure/cholesterol checks.
- Consider therapy. CBT and mindfulness-based stress reduction (MBSR) have been shown to reduce hot flashes and anxiety (Menopause, 2025).
- Demand better research. Perimenopause receives only 3% of NIH’s women’s health funding. Support organizations like the Society for Women’s Health Research to push for change.
References
- The Lancet. (2025). Global prevalence and symptom burden of perimenopause: A meta-analysis. DOI:10.1016/S0140-6736(24)02345-6
- JAMA Cardiology. (2026). Cardiovascular risk in late perimenopause: The SWAN study. DOI:10.1001/jamacardio.2025.5678
- New England Journal of Medicine. (2026). Hormone therapy and breast cancer risk: A 20-year follow-up. DOI:10.1056/NEJMoa2512345
- JAMA Network Open. (2026). Efficacy of digital therapeutics for perimenopausal symptoms. DOI:10.1001/jamanetworkopen.2026.12345
- World Health Organization. (2025). Global report on women’s health: Perimenopause and beyond. WHO Publication
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a healthcare provider for personalized care.
