The University of Cologne is hosting a “Planetary Health Diet” workshop on April 21, 2026, as part of its Summer of Sustainability. This initiative promotes evidence-based nutritional frameworks designed to simultaneously reduce chronic disease risk in humans and mitigate the environmental degradation of global food systems.
This movement is not merely about “eating green”; it is a clinical imperative. We are witnessing a symbiotic crisis where the degradation of our planetary ecosystem—soil depletion, biodiversity loss and climate instability—directly correlates with the rise of non-communicable diseases (NCDs). When we shift our dietary patterns, we aren’t just protecting the biosphere; we are altering the metabolic pathways that lead to systemic inflammation and cardiovascular collapse.
In Plain English: The Clinical Takeaway
- Eat More Plants: Focus on whole grains, legumes, nuts, and fruits to lower your risk of heart disease and diabetes.
- Eat Less Processed Meat: Reducing red and processed meats lowers systemic inflammation and protects your arteries.
- Planet-Health Link: Choosing sustainable foods reduces the pollution that causes respiratory and metabolic health issues in the general population.
The Metabolic Mechanism: How Planetary Health Diets Combat Chronic Inflammation
At the core of the Planetary Health Diet is the reduction of saturated fats and the increase of phytonutrients. From a clinical perspective, this targets the mechanism of action—the specific biochemical process—of systemic inflammation. High intake of processed meats triggers the release of pro-inflammatory cytokines, which can lead to atherosclerosis (the hardening of the arteries).
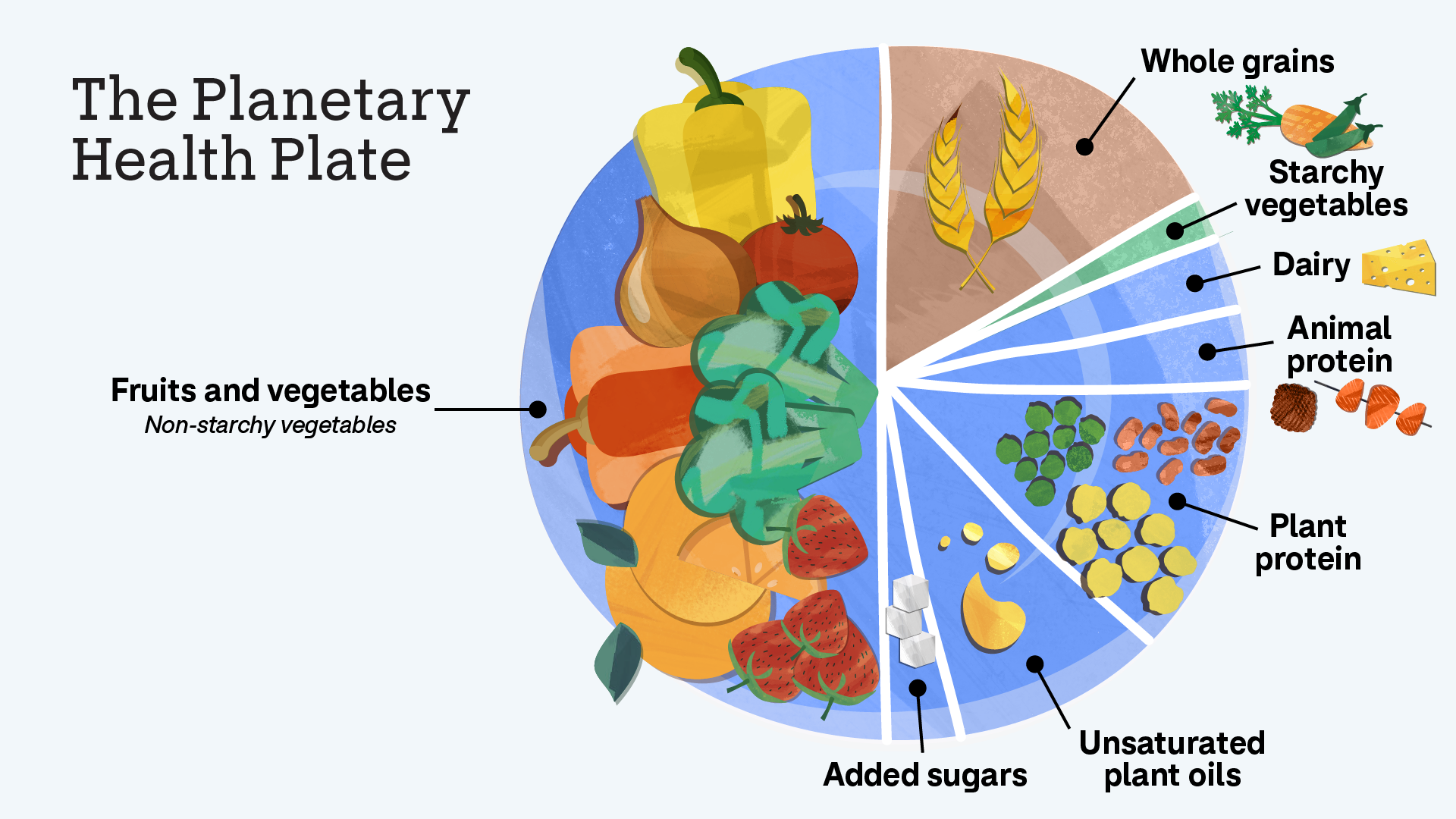
Conversely, a diet rich in legumes and whole grains increases the intake of soluble fiber. This fiber undergoes fermentation by the gut microbiota, producing short-chain fatty acids (SCFAs). These SCFAs act as signaling molecules that maintain the integrity of the intestinal barrier and modulate the immune response, effectively lowering the risk of Type 2 Diabetes and metabolic syndrome.
To understand the scale of this impact, we must look at the EAT-Lancet Commission’s framework, which provides the scientific bedrock for the University of Cologne’s workshop. Their research emphasizes a “double-blind” reality: while individual patients may not see immediate changes, the longitudinal population data is undeniable.
“The planetary health diet is not a restrictive regime but a scientific blueprint for survival. By aligning human nutritional needs with planetary boundaries, One can prevent millions of premature deaths from malnutrition and obesity-related diseases.” — Dr. Walter Willett, Professor of Public Health and Nutrition at Harvard University.
Geo-Epidemiological Bridging: From Cologne to Global Healthcare Systems
While the University of Cologne’s initiative is rooted in the European context, the clinical implications are global. In Europe, the European Food Safety Authority (EFSA) and the European Medicines Agency (EMA) are increasingly recognizing the role of “Food as Medicine.” This shift is mirroring the NHS’s focus in the UK on social prescribing, where doctors prescribe dietary changes as a primary intervention for hypertension.
In the United States, the FDA and CDC have long advocated for the Dietary Guidelines for Americans, but the Planetary Health Diet goes further by integrating environmental metrics. The gap here is patient access. In “food deserts” within the US or underserved regions in the Global South, the ability to adhere to a plant-forward diet is hindered by socioeconomic barriers, not a lack of will. This creates a health disparity where the most vulnerable populations suffer the highest rates of diet-related NCDs.
The funding for these large-scale dietary frameworks, such as the EAT-Lancet Commission, is typically transparently sourced from philanthropic grants and academic institutions, ensuring that the recommendations are not skewed by the industrial meat or sugar lobbies. This independence is critical for maintaining the integrity of public health intelligence.
Comparative Clinical Impact: Plant-Forward vs. Standard Western Diets
To visualize the clinical shift, consider the following data comparing a standard Western diet (high in processed meats and refined sugars) against the Planetary Health Diet (PHD) parameters.
| Biomarker/Metric | Standard Western Diet | Planetary Health Diet (PHD) | Clinical Significance |
|---|---|---|---|
| LDL Cholesterol | Elevated (High Saturated Fat) | Reduced (High Fiber/Unsaturated Fat) | Lower risk of Myocardial Infarction |
| Glycemic Variability | High (Refined Carbohydrates) | Stable (Complex Carbohydrates) | Improved Insulin Sensitivity |
| C-Reactive Protein (CRP) | Higher (Pro-inflammatory) | Lower (Anti-inflammatory) | Reduced Systemic Inflammation |
| Carbon Footprint | High (Industrial Livestock) | Low (Plant-based proteins) | Reduced Environmental Stressors |
The Nutrient Gap: Avoiding Deficiency in a Plant-Centric Transition
As we pivot toward these diets, we must address the “Information Gap” regarding micronutrient bioavailability. A strict transition without clinical guidance can lead to deficiencies in Vitamin B12, Iron, and Omega-3 fatty acids. B12 is synthesized by bacteria and is virtually absent in plant foods; deficiency can lead to irreversible neurological damage and megaloblastic anemia.
the bioavailability—the proportion of a nutrient that is absorbed and utilized by the body—of non-heme iron (found in plants) is lower than heme iron (found in meat). Patients must be educated on “nutrient pairing,” such as consuming Vitamin C-rich foods alongside iron sources to enhance absorption through the reduction of ferric iron to ferrous iron in the gut.
Contraindications & When to Consult a Doctor
While the Planetary Health Diet is generally safe for the general population, it is not a universal prescription. Certain individuals must exercise caution:
- Chronic Kidney Disease (CKD): Patients with advanced CKD may need to limit potassium-rich foods (like certain legumes and fruits) to avoid hyperkalemia, which can cause cardiac arrhythmias.
- Severe Malnutrition/Anemia: Individuals with acute iron-deficiency anemia should consult a physician before eliminating animal proteins to ensure they can meet their iron requirements through supplementation or fortified foods.
- Gastrointestinal Disorders: Those with Crohn’s disease or IBS may locate the increase in high-fiber legumes triggers flare-ups. A gradual “step-up” approach to fiber is medically indicated.
If you experience unexplained fatigue, tingling in the extremities (potential B12 deficiency), or sudden digestive distress after transitioning your diet, seek a professional medical evaluation immediately.
The transition toward a Planetary Health Diet is not merely a lifestyle choice; it is a clinical necessity for the survival of both the patient and the planet. By integrating the rigor of peer-reviewed science with the urgency of environmental sustainability, we can move from a system of “sick-care” to a true system of health-care.

